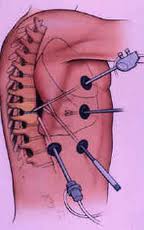
Video assisted thoracic surgery or thoracoscopic surgery is fast becoming a popular way of diagnostic and therapeutic reasons. Several diseases of the chest can now be diagnosed because of ease of look and biopsy. Also therapeutic procedures can be achieved using minimal access thereby giving the patient a significant advantage about the morbidity front. Thoracoscopy has been used for diseases from the pleura, lung, mediastinum, spine and heart.
INTRODUCTION
The enthusiasm for Minimal Access Surgery from the chest has been intermittent and in some way not as much as it promises to become. Just A century ago, surgery within the chest was regarded as unsafe and surgeons dreaded this surgery. Even though thoracoscopy has been a a part of thoracic surgical practice for several years, the advent of videoassisted methods offers greatly widened the signs and also the utilizes of the method. Where formerly thoracoscopy was performed primarily for diagnostic purposes, it now has thought a major role in the therapy of chest pathology as more anatomical areas have available.
For that treatment of many chest diseases, sufferers can occasionally face an extended and difficult recovery simply because standard “open” thoracic surgery is extremely invasive. In most cases, surgeons must create a long incision via chest muscles after which reduce or spread the patient’s ribs to achieve the diseased area. As a result, sufferers may spend up to and including week within the hospital and up to 4 to 6 weeks of recovery at home.
Now, a surgical method referred to as video clip assisted thoracic surgery is enabling surgeons to perform numerous popular thoracic procedures inside a non-invasive method. With respect to the kind of procedure, most patients don't need intensive care, can leave the hospital in 1 to 3 days and, oftentimes, are back to normal actions inside a week.
With controlled pneumothorax, the idea of thoracoscopy produced. Jacobeus put in the cystoscope in 1910 to initial visualize the pleural cavity. The technique was adopted for creating pneumothorax for TB also to diagnose and manage malignancies from the pleural space. Using the advent of anti tuberculous treatment and chemotherapy, these uses grew to become outdated and so did the use of thoracoscopy
In the 1990’s there is an abrupt increase in using thoracoscopy. This happened because of many reasons:
- Miniaturization of video gear
- Improvement inside quality of pictures and lightweight solutions
- Single lung anesthesia enhancements to permit uninterrupted examination of stomach.
- Development of staplers make it possible for biopsies and wedge resections.
- Innovative instruments
Ultimately, thoracoscope grew to become the main surgical treatment that received called as Video Assisted Thoracic Surgical treatment. Ten years has passed since the thoracoscopic surgical treatment counter-top revolution. Many thoracic operations have been attempted along with varying level of achievement. The passage of time may uncover what's feasible and what is good for this process.
In most VATS procedures, surgeons manage via 2 to 4 small openings between your ribs while watching the patient’s internal organs on a tv watch. Each opening is under 1 inch in size, whereas 6- to 10-inch incisions are not uncommon in receptive thoracic medical procedures.
How's VATS carried out?
All VATS procedures generally start the same way.Patients are placed under basic nesthesia and therefore are generally positioned on their own factors. Using a trocar, the surgeon gains access into the chest hole via a space between your ribs. An endoscope is inserted with the trocar, giving the surgeon a amplified view of the patient’s organs on a television monitor.
Indication generally accepted
- Analysis
- Lung biopsy in nonventilated patients
- Biopsy of pleural disease
- Biopsy associated with mediastinal masses
- Staging of lymph nodes within the aortopulmonary window
- Excision of indeterminate pulmonary nodules
Therapeutic
- Sclerosis from the pleural room with regard to malignant disease
- Excision of benign pleural lesions
- Excision of harmless lung tumors
- Sympathectomy regarding hyperhidrosis and upper-extremity
- pain syndromes
- Stapling of blebs
- Debridement for severe empyema
- Decortication for chronic empyema
Indications not generally accepted but commonly performed
Excision of mediastinal tumors
- Pericardial biopsy or fenestration
- Wedge excision of T1 cancer of the lung as definitive treatment in patients with poor ulmonary reserve
- Volume reduction for bullous lung disease
- Treating thoracic spine disease
Indications not generally accepted and not commonly performed
Video-assisted lobectomy
- Esophageal myotomy for achahasia
- Excision of esophageal leiomyoma
- Ligation of thoracic duct for chylothorax
- Staging lymph nodes in esophageal cancer
PLEURAL DISEASES
Failure to diagnose the reason for pleural ailment regardless of the use of standard evaluative techniques is a very common clinical trouble. Thoracoscopy has been utilized properly with this condition in Europe, but is sometimes utilized in North America. Closed pleural biopsy stays a good technique in a few patients with effusions, but VATS techniques which allow biopsy of specific regions of the parietal pleura under direct vision, have many advantages. The major indication for horacoscopy within the management of pleural disease remains pleural effusion of unclear origin, but other indications are becoming more frequent. Undiagnosed effusion is a very common reason to complete thoracoscopy with a decent diagnostic yield. Other indications include chest trauma with hemothorax/ hemopneumothorax, thickened pleura, persistent pain, suspected mesothelioma, empyema and pneumothorax. Thoracocentesis is the first procedure done in most cases has the capacity to give a route for thoracoscopy. It helps in deciding if a therapeutic process like pleurodesis, decortication may be needed. The most direct method to measure the potential room isby thoracocentesis, which helps to look for the ability from the owner to get into the pleural room under consideration. At some time this kind of review can be created via adjustments seen about the CT scan from the chest. Scalloping of the lung close to the pleura is a indicator of the more strong procedure that may not yield an area for that thoracocscope. Another signal of potential difficulty is really a zone of enhancement from the edge of the pleural fluid advising an organized fibrinous or fibrin remove on the lung that could prevent lung development.
The diagnostic/ therapeutic thoracoscopy can be achieved within nearby or basic anesthesia. Through basic anesthesia lung is collapsed both through a double lumen tube or by insufflation of carbon dioxide. During local anesthesia, lung is collapsed by a controlled pneumothorax.
One of the time honored indication of an nvasive procedure is empyema. On drainage of the empyema, the lung might not expand due to two reasons:
- Multiloculated empyema at the level of parietal pleura.
- Thickened granulation tissue within the visceral pleura.
In the first situation, a thoracoscopic ebridement if done early results in great results. In the second situation, a decortication is needed to get the lung to expand again. Previously, a patient with an empyema often required formal decortication through thoracotomy to permit lung reexpansion, especially if the pleural peel had become organized. With VATS techniques, thoracotomy is often avoided, specifically patients are treated early in the course of the empyema. We along with other groups feel that early thoracoscopic debridement is indicated in the febrile patient with a pleural effusion in whom complete drainage cannot be effected through tube thoracostomy. What is frequently present in these cases is thick, fibninous material that would not be probably be completely drained by a large-bore chest tube. For similar reasons, VATS techniques have proven useful in the management from the organizing posttraumatic hemothorax by which a number of chest tubes happen to be not able to completely drain the fibninous clot and debris. Once more, early referral, prior to organization from the hemothorax, would appear to be important in these circumstances. Also a biopsy can be taken simultaneously.
Troubles are uncommon with diagnostic thoracoscopy only. However, all the usual problems do occur from time to time, including bleeding, infection, nerve injury from a biopsy or from pressure on an intercostal nerve, post thoracotomy pain syndrome, pleural effusion, air leak, atelectasis and pneumonia. Each problem is addressed very much the same as any other thoracic procedure. Management of chronic pleural effusions remains under debate at the present time. Tetracycline, talc, bleomycin, abrasion, betadine, all have been tried. A combination of abrasion with talc seems to be supplying the highest success in malignant effusions. For benign effusions, talc isn't used the so long term safety factors are not established. Betadine is a good alternative in such instances. Recurrent pneumothorax is also a common indication for thoracoscopy. The best way of management is to adhere to the principles of stopping the environment leak by bleb resection and some kind of pleural procedure to produce pleurodesis. Mechanical abrasion is easily the most popular procedure. Pleural-based tumors may be sampled as well as resected using VATS. Benign pleural tumors, specifically solitary fibrous tumors as a result of the visceral pleural surface, are perfect lesions for thonacoscopic resection. Video thoracoscopy offers a choice within the treatment of malignant pleural effusions, particularly when the fluid is loculated. When tube thoracostomy results in incomplete drainage or when an effort at chemical pleurodesis via a chest tube fails, many would go to thoracoscopic pleurodesis. Loculations are visualized and debrided, and also the fluid is totally evacuated. Dry talc, which causes a significant inflammatory pleuritis and subsequent pleural symphysis, will be insufflated. Although no randomized, prospective trial continues to be completed comparing chest tube to thonacoscopic pleurodesis, one nonrandomized trial demonstrated a higher rate of successful pleurodesis with thonacoscopic insufflations of talc versus tetracycline or bleomycin introduced using a chest tube. Ninety-five percent of patients within the thoracoscopy team had successful pleurodesis, versus 47% within the tube thoracostomy team.
PARENCHYMAL DISEASE
Video-assisted techniques have made significant inroads in the diagnosis and treatment of panenchymal lung disease too. Previously, patients with a diffuse interstitial process often were treated empirically, without a specific diagnosis. Lung biopsy, which required a thoracotomy, had been restricted to individuals patients who either failed empiric therapy or have been desperately ill within the intensive care unit. In the patient having a chronic interstitial process who's not immunocompromised, obtaining a tissue diagnosis is often indicated, but it's these functional individuals in whom you have the greatest resistance to performing a process as morbid like a thoracotomy. Bronchoscopic transbronchial biopsy frequently fails to yield a specific diagnosis, particularly if vasculitis is really a consideration.
VATS wedge lung biopsy represents a significant advance. It provides the benefit of excellent visualization of and access to the entire lung, allowing biopsies of areas appearing abnormal and likely increasing diagnostic yield. Further, we and others feel it decreases postoperative pain and shortens hospital stay, although for this specific disease process, again, no data are yet offered by prospective, randomized trials to prove this theory.
The currently available data, however, are impressive. In a retrospective multiinstitutional study, Fenson at al.compared 47 patients undergoing thoracoscopic lung biopsy with 28 patients who had open wedge resection through limited thoracotomy. Adequate tissue for diagnosis was obtained for all patients in both groups. The hospital stay was significantly shorter within the group undergoing thoracoscopic biopsy, and much more complications occurred in the open group than in the thoracoscopic group. Video-assisted techniques have also affected the administration of spontaneous pneumothorax both in the young patient along with apical blebs as well as in the older patient with emphysema. The very first presentation of the spontaneous pneumothorax inside a youthful person is managed nonoperatively, as the likelihood of recurrence is around 30% .Operative treatment for a first-time pneumothorax classically has been restricted to people patients with persistent air leaks ,those whose occupations require them to experience extremes in atmospheric pressure, and those who live in isolated areas without use of health care. Otherwise, surgery is indicated following a first recurrence or the patient that has suffered bilateral pneumothoraces. Formerly, the operative management of spontaneous pneumothorax required whether thoracotomy with stapling of apical blebs and also at times a pleurectomy or, more recently, a transaxillary thoracotomy with excision of blebs and pleural abrasion or pleurectomy to create a pleural symphysis .Videothoracoscopic management of spontaneous pneumothorax offers a simple surgical alternative that's associated with minimal morbidity. The operation entails excising the apical blebs and developing a pleural symphysis-the same goals of the open procedures. The blebs are easily visualized with the thoracoscope and excised by several applying a specially designed endoscopic linear stapler that is both aerostatic and hemostatic .Even though a number of techniques are likely to provide successful pleurodesis, we would rather mechanically abrade the pleura having a gauze sponge. Talc is avoided in these young patients. Because the procedure performed is identical to that performed through open thoracotomy, you might expect similar recurrence rates, though used, recurrence rates following a VATS procedure have been slightly higher. In a randomized comparison of VATS as well as open up bullectomy with pleurectomy, WaIler at al. found that those patients with primary spontaneous pneumothorax undergoing VATS benefited from decreased postoperative pain, smaller hospital remain, and less pulmonary dysfunction. No patient either in the VATS or the thoracotomy groups suffered treatment failures. In our experience with 70 procedures in patients with spontaneous pneumothorax secondary to blebs, there's been one recurrence, and patients have remaining a healthcare facility on the 1st or 2nd postoperative working day.
The direction of bullous lung disease has also changed. The most established indication for operation in patients with bullous emphysema is the presence of a giant bulla considerably compressing adjacent lung parenchyma. This indication is readily recognizable on plain chest radiograph, although CT helps you to define the presence and extent of compressed lung tissue. The procedure itself requires excision of the bulla and stapling from the base to prevent air leak Surgeons have been loathe to perform this process via thoracotomy in these compromised patients due to fear that they may not survive the short-term results of the incision upon their already marginal pulmonary status. Videothoracoscopic techniques seem to obviate this concern considerably.
Brennen at al., inside a prospective, clinical trial of thonacoscopic ablation of pulmonary bullae having a laser, indicated that forced vital capacity, forced expiratory volume in 1 sec, maximum voluntary ventilation, residual volume, and airway resistance were all significantly improved through the process. These authors also demonstrated that quantitative radiographic research into the extent of bullous disease and the degree of associated emphysema during these patients may be used to determine postoperative pulmonary reaction. Giant bullae exist in only a small group of patients with bullous emphysema. It remains to appear whether there will be a job for VATS in volume reduction surgery in patients with diffuse bullous or nonbullous emphysema process of which impressive early results have been reported through a median sternotomy approach. Bronchopleural fistulae can often be sutured thoracoscopically.
PULMONARY NODULES
In several centers, VATS has changed the management from the patient with a solitary pulmonary nodule .By getting a trusted diagnosis to be made in a single,minimally morbid procedure, VATS has, for a lot of physicians, engendered a complete reassessment of the approach they decide to try this frequently encountered clinical problem. The question that must definitely be responded when given a solitary pulmonary nodule is merely, “Is it malignant?”
Although no criteria are absolute, a number of factors indicate a benign diagnosis .Lesions in nonsmokers younger than thirty are incredibly unlikely to be malignant. If the lesion has not changed in size over 2 years, it's also generally felt safe to think about the lesion benign. The importance of review of a prior chest radiograph, then, can't be overemphasized. Dense on central calcification about the chest radiograph is recognized as to be a trustworthy indicator that the lesion is benign. The current application of quantitative CT densitometry has obtained this idea a step further, but this method will identify as benign only 22-28% of these nodules without diagnostic calcification on a plain radiogram. Despite these noninvasive ways of attempting to decide the nature of a solitary pulmonary nodule, a large number of such lesions remain indeterminate and therefore require tissue acquired by one means on another to establish a diagnosis. Only 10-20% of patients with malignant solitary pulmonary nodules will have sputum positive for cancer . Furthermore, the preponderance of benign tissue fragments obtained from a nodule by among the two other available nonoperative diagnostic studies, bronchoscopy and transthoracic needle biopsy do not guarantee that the lesion is, in fact, benign. A particular benign diagnosis is created only 10% of times at bronchoscopy and between 12% and 67% of times by transthoracic needle biopsy. Because as many as 29% of patients with no diagnosis of malignancy on transthoracic needle biopsy are ultimately found to have carcinoma, just the appearance at specific benign medical diagnosis by cytology can, in our look at, avert a further treatment.
Thus, most “negative” final results from transthonacic needle biopsies are of no benefit to the individual and simply mandate a further diagnostic procedure, whereas an analysis of malignancy merely confirms that total excision should be completed. It should be noted that the risk of morbidity from trans-thoracic needle biopsy is considerable, using the rate of chest tube place for significant pneumothorax at approximately 5%. For these reasons, many groups currently do not perform transthoracic needle biopsy for that indeterminate pulmonary nodule except in the patient with multiple nodules who needs a tissue diagnosis, and in who the diagnosis is extremely probably be malignant, on within the patient by having an complete contraindication to operation. The practice used by these groups is complete removal ofthe lesion by VATS wedge resection. This really is done by serial firing of an endoscopic stapling gadget placed through among the usual incision sites , while the lesion is grasped with an instrument placed through another of the incisions. Once the lesion has been separated from surrounding lung, it's placed in an endoscopic bag and removed through one of the incisions .When the lesion is malignant on frozen section, lobectomy should be performed , which possibility is discussed in detail using the patient preoperatively. If the lesion is benign, the procedure is terminated and also the patient is spared a thoracotomy. Mack at al. looked closely in the role of VATS within the management from the indeterminate solitary pulmonary nodule.
They performed VATS excision on 242 patients like a primary diagnostic maneuver. A definitive diagnosis was obtained in most cases, and there was no mortality or major morbidity. Minor complications took place only3.6%. By 50 percent patients, the nodule could not be recognized and thoracotomy was needed. When a primary lung cancer was identified, as with 48% of patients, formal open thoracotomy and anatomic resection was completed. Thus, 127 patients were spared thoracotomy for any benign lesion. The average hospital stay for those undergoing thoracoscopy alone was 2.4 days. Santambnogio at mal. performed a randomized, controlled clinical trial evaluating VATS excision from the solitary pulmonary nodule and excision via muscle-sparing thoracotomy. Thediagnosis is made in 100% of both groups, however the VATS group had considerably less postoperative pain along with a much shorter period of stay. In a prospective, nonrandomized study of 138 patients, Landreneau at al. found those undergoing VATS versus limited lateral thoracotomy for wedge resection to profit from a lower complication rate, reduced pain, less shoulder dysfunction, and fewer early impairment in pulmonary function. Thus, VATS excision of pulmonary nodules can be performed having a high sensitivity and specificity, and a suitable level of morbidity, by surgical standards. But must you excise so many benign lesions? It's the uncertainty of the benign diagnosis generally that is definitely the most compelling argument for thoracoscopic excision of the majority of solitary pulmonary nodules. All queries are answered, and also the uncertainty is eliminated with one process.
Specific lesions aren't considered for thoracoscopic excision. For lesions more than 3 cm in size, the probability of malignancy is so high that even without the metastatic disease, thoracotomy ought to be the first process undertaken. Located lesions in close proximity to hilan structures are not ideal for thoracoscopic wedge excision and require thoracotomy and formal anatomic resection. It's these patients in whom almost all would agree that the make an effort to avoid thoracotomy by receiving a specific benign diagnosis by transthoracic needle aspiration is indicated.
For VATS wedge excision, CT aids greatly in localizing the nodule; we and others have found so that it is the only real localizing study required . Although localization by CT-guided wire-placement continues to be referred to with good achievement , we now have found that also lesions below the surface can be identified by palpation from the lung as it is moved towards a digit inserted through one of the chest incisions. Within our knowledge about 275 thoracoscopic excisions of pulmonary nodules, we now have failed to locate the nodule in only two cases, both very early in our experience. This discussion would be incomplete without some reference to the current management of a lesion excised thoracoscopically and located on frozen section to become malignant and consistent with a primary lung carcinoma. In the surgeon’s perspective, it is tempting, at times, to prevent at that time and think about the wedge excision to be adequate treatment, especially for a small lesion. Depending on current knowledge, however, wedge excision is not optimal therapy for a primarym lung cancer, a small T1 lesion, in a patient with sufficient pulmonary reserve to withstand a lobectomy. The Lung Cancer Study Group has addressed this question of limited resection versus lobectomy for T1 N0 lesions inside a prospective randomized trial. At Five years, the rate of local recurrence in individuals undergoing limited resection is increased, which rate has translated into a significant survival advantage in the group that underwent lobectomy. Wedge excision, therefore, is really a compromise that is suitable just for the patient who otherwise cannot tolerate a thoracotomy. Lobectomy may be performed utilizing a video assisted technique that requires a little utility incision but usually without the need for r ib spreading. Used, despite the technical feasibility from the method, there does not appear to be any decrease in postoperative pain or in the amount of days spent in the hospital. However, not good data are yet on this issue.
OTHER THORACOSCOPIC PROCEDURES
Videothoracoscopy has proven useful being an adjunct to more conventional procedures accustomed to stage lung cancer. Mediastinoscopy remains the gold standard for invasive staging of the mediastinum, but the posterior subcarinal lymph nodes and the nodes within the sub aortic window are not accessible by standard cervical mediastinoscopy
Videothoracoscopy offers use of the lymph nodes within the sub aortic window and the subcarinal space in those patients whose CTs show enlarged nodes in these regions only, and who may be spared thoracotomy and lobectomy if a tissue diagnosis of malignancy from these regions would render them unresectable. Primary lesions of the mediastinum are perfect for VATS management. All locations from the mediastinum are accessible, and whether sampling or excision may be the intent, video-assisted techniques save many patients from needing to undergo thoracotomy or median sternotomy. These techniques have been especially useful in patients in whom a lesion that would 't be treated surgically, for example lymphoma, is suspected. These lesions usually exist in the anterior mediastinum, and the question of thymoma versus lymphoma arises. If the lesion can't be reached by mediastinoscopy, thoracotomy or median sternotomy is no longer necessary to make a diagnosis of lymphoma.
Also performed are excision of mediastinal parathyroid adenomas and dorsal sympathectomy to treat upper-extremity pain syndromes, thoracolumbar sympathectomy to deal with intractable pancreatic pain, pericardial windows to deal with effusive disease, and ligation from the thoracic duct for chylothorax. Various procedures on the esophagus, including excision of the leiomyoma, and myotomy within the treating achalasia, are also performed. Each of these procedures continues to be reported within the literature with acceptable results.
In patients with nonthymomatous autoimmune myasthenia gravis thymectomy is recommended being an choice to increase the possibility of symptomatic improvement or remission. There is a consensus that all adults with generalized symptoms must have thymectomy, especially if they're younger than 55 years. In elderly patients, in children, plus pure ocular myasthenia, thymectomy has been shown to benefit you a minimum of in some series, even though surgical indications thus far remain controversial. These general selection criteria will also be applied to video-assisted thoracoscopic thymectomy that can be performed through right or left approaches.
For that operation, after double-lumen intubation, the patient is placed in a 45-degree off-center position and 4 flexible thoracoscopic trocars are inserted. The whole hemithorax is carefully explored with particular attention to aortic arch, subclavian artery, pericardium, and phrenic nerve. The dissection is begun inferiorly by incising the mediastinal pleura along the anterior border of the phrenic nerve .Due to the preoperative pneumomediastinum, the mediastinal adipose tissue is embedded with air and also the thymus has already been partially separated from the pericardium and in the sternum. Consequently, the dissection proceeds quicker and easily, mainly by blunt maneuvers, with the aid of two pledgets. All mediastinal tissue including fat is swept from the phrenic nerve and the left inferior horn is dissected off the underlying pericardium. Afterwards, the gland is dissected off the retrosternal area beginning just beneath the internal mammary pedicle and continuing rightwards before right mediastinal pleura is visualized. The best inferior horn is fully dissected up to the isthmus.
The low 1 / 2 of the gland is then retracted upward and the thymic veins, usually 2 or 3, are identified clipped and divided . Subsequently, the dissection proceeds cephalad, superior to the innominate vein, to the lower cervical region. The superior horns are progressively dissected free by blunt maneuvers with gentle traction applied downward about the thymus. In this manner, even long and thin upper horns could be dissected en bloc with the rest from the gland. The intact thymus is extracted inside a retrieval bag through the most anterior port and it is examined to ensure the whole gland has been removed Subsequently, all mediastinal fat that can be found in the pretracheal space, across the internal mammary pedicles, within the aorto-pulmonary window, as well as in the best or left pericardiophrenic angles that may contain ectopic thymic tissue is completely excised to complete a long thymectomy.
Relative contraindications for any left-sided VATS approach include patients having a history of pleurodesis within the left pleural cavity or those with severe cardiomegaly, in whom a right-sided approach is recommended.
ENDOSCOPIC THORACIC SYMPATHECTOMY
In 1954, an Austrian surgeon developed the strategy of Endoscopic Upper Thoracic Sympathectomy. Subsequent upgrades within the technology of optics and instrumentation through the Karl Storz Company led to the refinement of the ETS procedure by creating small devices that can visualize and clip the sympathetic nerves. The sympathectomy procedure has developed in the last 60 years. What began being an open chest operation is now being performed with small scopes and cameras. The sympathetic nerve trunks are no longer eliminated or destroyed, but instead are actually clamped. The brand new procedure is known as an Endoscopic Transthoracic Sympathetic Blockade with Metallic Clips. It's also known as an Endoscopic Transthoracic Sympathectomy with Metallic Clips. The terms ETB and ETS-C are interchangeable and mean the same. The therapeutic rationale within the treatment of hyperhidrosis is dependant on the interruption of transmission of sympathetic impulses from the reduced sympathetic ganglia through stellate ganglia towards the hands. Thoracoscopic T2-sympathectomy or sympathicotomy is considered the best treatment for hyperhidrosis.
ESOPHAGEAL SURGERY
Surgery for achalasia cardia by thoracoscopy has now already been completely replaced by the laparoscopic approach. Excision of leiomyoma is done for the most part centres where thoracoscopy is being done however no large series can be obtained. Surgeons have reported the use of minimally invasive processes to resection of the esophagus so that they can additional decrease the associated morbidity of esophagectomy. Many of these case research or small series have used video-assisted thoracoscopy to mobilize the thoracic esophagus in combination with a typical open laparotomy to accomplish the esophagectomy. Clear benefits of thoracoscopic esophageal mobilization more than thoracotomy or laparotomy only with transhiatal dissection weren't demonstrated in these studies. Esophageal mobilization throughout esophagectomy for cancer can be done thoracoscopically. The patient is intubated having a double lumen endotracheal tube for single lung ventilation and situated in the left lateral decubitus position. Four thoracoscopic ports are launched. Your camera port is positioned in the seventh intercostal space, midaxillary line. A 10 mm port is placed at the eighth or ninth intercostal space 2 cm posterior towards the posterior axillary line for that ultrasound coagulating shears. Two additional ports are put, one 5 mm posterior to the tip from the scapula and one 10 mm at the fourth intercostal space at the anterior axillary line for retraction and counter-traction throughout the esophageal dissection. The azygos vein is split following a twice tie.
The mediastinal pleura overlying the esophagus is divided and also the entire thoracic esophagus is exposed. First the inferior pulmonary ligament is divided to the level of the inferior pulmonary vein. The mediastinal pleura is divided anteriorly across the esophagus to the level of the azygos vein. While dissecting at the level of the subcarinal nodes, continuous attention is paid to prevent injuring the mainstem bronchi. The vagus nerve is typically divided cephalad towards the azygos vein. A tape is placed around the mid-esophagus to facilitate traction and exposure. Circumferential mobilization from the esophagus with all of surrounding lymph nodes and periesophageal tissue and fat is conducted from the diaphragmatic reflection to the thoracic inlet . A single 28 F chest tube is inserted with the camera port and the other port sites are closed with absorbable sutures.
SPINE SURGERY
Minimal-Access methods happen to be launched all through surgery, including orthopaedics and traumatology, exactly where, because the early 80s, arthroscopy has revolutionized the treatment of joint disorders. For a long time, the backbone didn't benefit from these types of innovations. This situation was changed when, in 1991, Obenchain done a laparoscopic L5-S1 discectomy, followed, in 1992, by Thomas Zdeblick’s L5-S1 fusion by laparoscopic keeping an interbody cage. In 1994, Rosenthal et al reported the first excision of the herniated thoracic disc by thoracoscopic surgery. At the same time, Le Huec and Husson performed the very first endoscopic retroperitoneal approach to the lumbar spine. Together, most of these three methods supply use of the thoracic and lumbar spine in the entirety.
Patient is usually make the lateral placement and knowledge of anatomy is very important when approaching the spine thoracoscopically. Initially, these endoscopic techniques gave limited access that helped easy treatments, since the new type of surgery was difficult and involved a learning curve. Working with their colleagues in general and thoracic surgery, and taking advantage of the instruments already developed in the some other subspecialties for minimally invasive surgery, allowed spinal surgeons speedily to evolve minimal-access approaches to their discipline.
Simultaneously, other surgeons were developing minimal-access surgery with endoscopic visualization. This video-assisted surgery proved an important stage, since it reduced how big the incisions and gave a better view of the surgical field, while still preserving the landmarks familiar to the surgeon from the times of available surgery. Video-assisted surgery is now establishing itself in a niche of its own, between conventional open surgery and fully endoscopic techniques. Treating symptomatic thoracic herniated discs utilizing a conventional approach is notoriously dangerous. The enlarged posterolateral approach described by Roy- Camille has been gradually superseded by an anterior approach. This anterior approach through a thoracotomy has proved to be superior. The endoscopic approach first described by Rosenthal makes this process less invasive, while optimizing visualization and, consequently, cord decompression.
The anterior discharge of stiff thoracic scoliotic deformities is yet another indication for an endoscopic approach. In conventional surgery via a thoracotomy, with elimination of a rib, disc excision at several levels soon becomes difficult, with curvatures > 90°, visualization is far from optimal. Thoracoscopy allows anterior releases to become extended over 7, 8, or 9 levels; switching the scope round the trocar sites will ensure that vision is always optimum. The instruments will be aligned with the disc to be tackled, and the endplates might be reamed under endoscopic vision. The segmental vessels can invariably be preserved, and the discharge of the rib head gives better mobilization of the spine as well as offering an interbody graft where this is required. The indications of the anterior release have yet to be definitively established. In principle, they must be the same as the indications of conventional surgery; however, the less invasive nature from the endoscopic technique should allow more patients to become selected to have an anterior release. Drainage of paraspinal abscess due to tuberculosis can potentially become a very common indication of thoracoscopy in India. Depending on the pathology and extent of disease, additional procedures to stabilize the spine may be required .
MEDICAL THORACOSCOPY
“Medical” thoracoscopy compared to “surgical” thoracoscopy has the advantage that it may be practiced under local anaesthesia or conscious sedation, in an endoscopy suite, using nondisposable rigid instruments. Hence, it's even less invasive and less expensive. The primary diagnostic and therapeutic indications for medical thoracoscopy are pleural effusions and pneumothorax. Due to its high diagnostic accuracy, approaching almost 100% in malignant and tuberculous pleural effusions, it ought to be used when pleural fluid analysis and needle biopsy are nondiagnostic. In addition, medical thoracoscopy provides staging for lung cancer and diffuse malignant mesothelioma. Talc poudrage, since the best conservative method for pleurodesis in 1998, may also be performed with medical thoracoscopy. It can also be effectively used in the early management of empyema. In spontaneous pneumothorax it allows staging, thereby facilitating treatment decisions, and likewise coagulation of eventual blebs and talc poudrage for efficient pleurodesis. Medical thoracoscopy is really a safe procedure which is easier still to understand than flexible bronchoscopy. Due to its high diagnostic and therapeutic efficiency, it ought to be utilized increasingly within the management of the above-mentioned pleuropulmonary illnesses.
COMPLICATIONS OF THORACOSCOPY
Inside a series that looked at the complications , the entire incidence was 10%, most abundant in prevalent complication being prolonged air leak. There have been five superficial wound infections and 5 patients who bled significantly plenty of to require either transfusion or reoperation, or both. In 4.1% patients, the proposed thoracoscopic procedure couldn't be completed as prepared, and a thoracotomy was necessary. The incidence of complications is unquestionably acceptable and other alike to that particular observed after thoracotomy, although overall hospital stay is shorter and patients appear to have less pain and go back to normal activity sooner. You might assume the incidence of complications to further reduce as surgeons acquire more knowledge about this significant modification and development of the old technique.
CONCLUSIONS
Videothoracoscopy is definitely a helpful tool for thoracic surgeons, greatly extending the utility of an old technique. Current video technology has made it simple for a surgeon and an assistant to work together, and developments in instrumentation, especially staplers, make methods that were previously impossible now commonplace. In many centers, VATS procedures have replaced a wide variety of similar procedures previously performed by thoracotomy. The entire approach to some clinical difficulties, for example, the solitary pulmonary nodule, has been called into question by the availability of VATS. Critical comparisons between VATS processes and corresponding open techniques are beginning to look in the literature, but more such studies are required before we will have definitive answers towards the many questions raised by these new procedures. In the present era of cost containment, cost issues may reign chief among these unresolved questions. Intuitively, the shorter period of stay afforded by VATS procedures and also the patients’ earlier return to work are likely to decrease the total cost to society, but total cost will be hard to measure. VATS has cleanly found a location in the modern practice of thoracic surgery and it is likely to play an ever-increasing role within the administration of diseases from the chest.
World Laparoscopy Hospital, Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555






