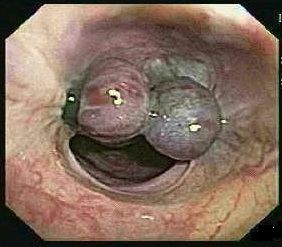
Introduction:
Cirrhosis, high pressure in the veins that take blood from the intestines to the liver triggers several disorders. Variceal bleeding is the bleeding from larged veins that is varices in the digestive tract, is an enormously acute disorder of portal hypertension. For people who have sophisticated cirrhosis and varices, specifically in the esophagus, the threat of variceal bleeding is extremely high. Just After varices have bled at one occassion, there is an acute dander of bleeding consistently. The possibility of bleeding consistently is top-notch immediately after the first bleed ceases. After it the possibility of bleeding again slightly falls down over the subsequent multitude weeks. If varices are not cured, bleeding can proceed to death. Endoscopic therapy is the process most frequently applied to cure acute variceal bleeding. It may be applied to protect from chronic series of variceal bleeding as well that are usual.
The two kinds of endoscopic therapy are:
- Endoscopic variceal banding that is mainly known as ligation.
- Endoscopic sclerotherapy.
Endoscopic therapy is frequently applied together with medicines like beta-blockers and vasoconstrictors.
Endoscopic variceal banding or ligation:
During variceal banding, a doctor make uses an endoscope in the course of variceal banding, to set up a flexible ring which seems just like a rubber band closed to a larged vein. Banding the vein in this way will discontinue blood circulation by the vein. It may be hard to utilize this method although the person is seriously bleeding, because the device applied to position the bands hardly seen by the doctor's vision. Variceal banding has been indicated to be as valuable as sclerotherapy in curing series of bleeding. And it has less health concerns.
Variceal banding is frequently applied for many times to manage the varices and protect from bleeding. For instance, banding might be recurrent every 2 to 4 weeks for 3 to 4 sessions. Your doctor will observe the varices every 3 to 12 months just after that for the rest of your life.
Endoscopic sclerotherapy:
Sclerosant is a chemical may be administered intramuscularly directly in the course of endoscopic sclerotherapy into an larged vein or into the wall of the esophagus opposite to the enlarged veins. The constituents triggers inflammatory events of the inside lining of the vein, that over time triggers the vein to blockade and blemish. When the vein is blockade, blood cannot circulate by it.
Endoscopic sclerotherapy may be valuable for ceasing acute flow of blood triggered by esophageal varices. Sclerotherapy is still performed in case of emergency, but it is not as famous as it was in the early era. More than before, doctors are utilizing variceal banding to cure and protect from esophageal variceal bleeding. Even if sclerotherapy is carried out at first, variceal banding is frequently performed subsequently to minimize the risk of future bleeding. Both procedures work. But variceal banding has less minimum risks of creating problems as compare to sclerotherapy.
Complications of endoscopic therapy:
The complications of variceal bleeding are due to either the bleeding itself or the methods applied to manage bleeding Problems related endoscopic sclerotherapy are unusual and complications of variceal banding are also considerably less common. If complications do produce, they may include:
- Infection.
- Demolish of the wall of the esophagus that is esophageal perforation.
- Accumulation in the esophagus that is esophageal ulcers.
- Tapering of the esophagus that is esophageal stricture.
- Aspiration pneumonia.
- vascular collapse
- hypotension,
- encephalopathy,
- aspiration,
- Subacute bacterial peritonitis.
All of these complications may necessitate admission to the ICU. However, the most common reasons for ICU admission are hypotension, aspiration and airway protection, and encephalopathy. Hepatic encephalopathy is a neuropsychiatric syndrome characterized by personality change and a depressed conscious level. It has a number of precipitants such as infection, dehydration, constipation, and gastrointestinal bleeding. The clinical spectrum of encephalopathy ranges from inappropriate behaviour and lethargy, to a comatose patient at risk of aspiration, requiring ICU admission and endotracheal intubation. Treatment involves the correction of precipitating factors, rehydration, antibiotics, and lactulose. Lactulose inhibits intestinal ammonia production and is commonly used at a dose of 20 ml three times daily.
Conclusion:
Variceal eradication by endoscopic procedures is valuable, with band ligation being the safe procedure. Sclerotherapy may be carried out when band ligation is not technically possibly done, whereas it is less efficient in decreasing the complications of re-bleeding. Endoscopic band ligation was initially performed as secondary prophylaxis when patients had bled, despite being on beta-blockers, or when beta-blockers were not tolerated or contraindicated. However, recent data suggest that combination therapy of band ligation and beta-blockers reduces the rate of variceal re-bleeding compared with either therapy alone.
World Laparoscopy Hospital
Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555






