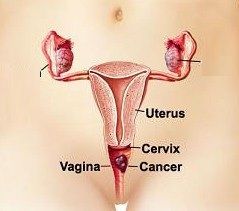
What's vaginal cancer?
Vaginal cancer is really a disease by which malignant (cancer) cells form in the vagina. Vaginal cancer is not common. When found in initial phases, it may get cured. There's two main kinds of vaginal cancer:
- Squamous cell carcinoma: Cancer that forms in squamous cells, the thin, flat cells lining the vagina. Squamous cell vaginal cancer spreads slowly in most cases stays close to the vagina, but may spread to the lungs andliver. This is the most typical kind of vaginal cancer. It's found usually in females aged 60 or older.
- Adenocarcinoma: Cancer that begins in glandular (secretory) cells. Glandular cells in the lining of the vagina make and release fluids such as mucus. Adenocarcinoma is much more likely than squamous cell cancer to spread to the lungs and lymph nodes. It is found most often in females aged 30 or much younger.
What are causes and risk factors for vaginal cancer?
Age and exposure to the drug DES (diethylstilbestrol) before birth affect a woman's risk of developing vaginal cancer. Anything that increases your risk of having a disease is called a risk factor. Risk factors for vaginal cancer range from the following:
- Being aged 60 or older.
- Being exposed to DES while in the mother's womb. In the 1950s, the drug DES was given to some women that are pregnant to prevent miscarriage (premature birth of the fetus that cannot survive). Women who were subjected to DES before birth come with an increased risk of developing vaginal cancer. Some of these women develop a rare type of cancer called clear cell adenocarcinoma.
- Having human papilloma virus (HPV) infection.
- Using a history of abnormal cells within the cervix or cervical cancer.
What are symptoms and signs of vaginal cancer?
Possible signs of vaginal cancer include pain or abnormal vaginal bleeding. Vaginal cancer often does not cause early symptoms and may be found during a routine Pap test. When symptoms occur they might be caused by vaginal cancer or by other conditions. A doctor should be consulted if the following problems occur:
- Bleeding or discharge not associated with menstrual periods.
- Pain during sexual intercourse.
- Pain within the pelvic area.
- A lump within the vagina.
What tests are utilized to diagnose vaginal cancer?
Tests that examine the vagina and other organs within the pelvis are used to detect (find) and diagnose vaginal cancer. The next tests and procedures may be used:
- Physical exam and history: An exam from the body to check on general signs of health, including checking for signs and symptoms of disease, such as lumps or anything else that seems unusual. A history of the patient's health habits and past illnesses and treatments will also be taken.
- Pelvic exam: An exam from the vagina, cervix, uterus, fallopian tubes, ovaries, and rectum. A doctor or nurse inserts a couple of lubricated, gloved fingers of one hand into the vagina and places the other give the low abdomen to feel the size, shape, and position of the uterus and ovaries. A speculum can also be inserted to the vagina and the doctor or nurse looks at the vagina and cervix for signs of disease. A Pap test or Pap smear of the cervix is usually done. A doctor or nurse also inserts a lubricated, gloved finger into the rectum to feel for lumps or abnormal areas.
- Pap smear: A process to collect cells from the surface of the cervix and vagina. A bit of cotton, a brush, or perhaps a small wooden stick is used to carefully scrape cells from the cervix and vagina. The cells are viewed within microscope to discover when they are abnormal. This procedure can also be called a Pap test.
- Biopsy: Removing cells or tissues from the vagina and cervix so they can be viewed under a microscope by a pathologist to check on for signs and symptoms of cancer. If a Pap smear shows abnormal cells in the vagina, a biopsy may be done throughout a colposcopy.
- Colposcopy: A process in which a colposcope (a lighted, magnifying instrument) can be used to determine the vagina and cervix for abnormal areas. Tissue samples may be taken using a curette (spoon-shaped instrument) and checked within microscope for signs of disease.
What is the prognosis for vaginal cancer?
Certain factors affect prognosis (possibility of recovery) and treatments. The prognosis (possibility of recovery) depends on the next:
- The stage of the cancer (be it within the vagina only or has spread to other areas).
- The size of the tumor.
- The grade of tumor cells (how different they are from normal cells).
- Where the cancer is at the vagina.
- Whether you will find symptoms.
- The patient's age and general health.
- Whether the cancer has just been diagnosed or has recurred (come back).
Treatment options rely on the next:
- Happens, size, and location of the cancer.
- Whether the tumor cells are squamous cell or adenocarcinoma.
- If the patient includes a uterus or has had a hysterectomy.
- If the patient has had past radiation treatment towards the pelvis.
How's staging determined for vaginal cancer?
After vaginal cancer has been diagnosed, tests are done to discover if cancer cells have spread within the vagina in order to other parts from the body. The procedure accustomed to find out if cancer has spread inside the vagina in order to other parts from the body is called staging. The information gathered in the staging process determines happens from the disease. You should be aware of stage in order to plan treatment. The following procedures can be utilized within the staging process:
- Biopsy: A biopsy may be done to determine whether cancer has spread towards the cervix. An example of tissue is cut from the cervix and viewed within microscope. A biopsy that removes only a small amount of tissue is usually done in the doctor's office. A woman may need to go to a hospital for any cone biopsy (elimination of a bigger, cone-shaped piece of tissue from the cervix and cervical canal). A biopsy of the vulva may also be done to find out if cancer has spread there.
- Chest x-ray: An x-ray of the organs and bones within the chest. An x-ray is a type of energy beam that can go through the body and onto film, creating a picture of areas within the body.
- Cystoscopy: A procedure to look inside the bladder and urethra to check for abnormal areas. A cystoscope is inserted through the urethra into the bladder. A cystoscope is really a thin, tube-like instrument having a light along with a lens for viewing. It might in addition have a tool to remove tissue samples, that are checked under a microscope for signs and symptoms of cancer.
- Ureteroscopy: A process to appear inside the ureters to check for abnormal areas. A ureteroscope is inserted through the bladder and into the ureters. A ureteroscope is really a thin, tube-like instrument having a light and a lens for viewing. It may in addition have a tool to remove tissue to become checked under a microscope for signs of disease. A ureteroscopy and cystoscopy may be done throughout the same procedure.
- Proctoscopy: A procedure to appear inside the rectum to check for abnormal areas. A proctoscope is inserted through the rectum. A proctoscope is really a thin, tube-like instrument having a light and a lens for viewing. It may also have a tool to remove tissue to become checked under a microscope for signs of disease.
- CT scan (CAT scan): A procedure which makes a series of detailed pictures of areas within the body, taken from different angles. The images are made with a computer associated with an x-ray machine. A dye may be injected into a vein or swallowed to assist the organs or tissues appear more clearly. This procedure can also be called computed tomography, computerized tomography, or computerized axial tomography.
- MRI (magnetic resonance imaging): A procedure that utilizes a magnet, radio waves, along with a computer to create a series of detailed pictures of areas inside the body. This procedure can also be called nuclear magnetic resonance imaging (NMRI).
- Lymphangiogram: A process used to x-ray the lymph system. A dye is injected to the lymph vessels in the feet. The dye travels upward with the lymph nodes and lymph vessels and x-rays are come to see if you will find any blockages. This test helps find out whether cancer has spread towards the lymph nodes.
The following stages are used for vaginal cancer:
Stage 0 (carcinoma in situ)
In stage 0, squamous cell cancer can be found in tissue lining the inside of the vagina. Stage 0 cancer is also called carcinoma in situ.
Stage I
In stage I, cancer is located only within the vagina.
Stage II
In stage II, cancer has spread from the vagina towards the tissue around the vagina.
Stage III
In stage III, cancer has spread from the vagina towards the lymph nodes in the pelvis or groin, or to the pelvis, or both.
Stage IV
Stage IV is divided into stage IVA and stage IVB:
- Stage IVA: Cancer might have spread to lymph nodes in the pelvis or groin and it has spread to 1 or both of the next areas:
- The lining of the bladder or rectum.
- Beyond the pelvis.
- Stage IVB: Cancer has spread to areas of the body that aren't near the vagina, such as the lungs. Cancer may also have spread to the lymph nodes.
Recurrent vaginal cancer
Recurrent vaginal cancer is cancer that has recurred (come back) once it has been treated. Cancer may come during the vagina or in other areas of the body.
What is the treatment for vaginal cancer?
Various kinds of treatments are available for patients with vaginal cancer. Some remedies are standard (the currently used treatment), plus some are now being tested in clinical trials. Before starting treatment, patients may want to consider getting involved in a clinical trial. Cure medical trial is really a research study designed to help to improve current treatments or obtain home elevators new treatments for patients with cancer. When clinical trials show that the new treatment is better than the standard treatment, the brand new treatment may become the standard treatment.
Clinical trials are taking devote many parts of the country. Information about ongoing clinical trials is available from the NCI Web site. Choosing the most appropriate cancer treatment methods are a decision that ideally requires the patient, family, and healthcare team.
Three kinds of standard treatment are utilized:
Surgery
Surgery is easily the most common treatment of vaginal cancer. The next surgical procedures can be utilized:
- Laser surgery: A surgical treatment that uses a laser beam (a narrow beam of intense light) like a knife to create bloodless cuts in tissue in order to remove a surface lesion such as a tumor.
- Wide local excision: A surgical treatment that removes cancer and some of the healthy tissue around it.
- Vaginectomy: Surgery to get rid of all or the main vagina.
- Total hysterectomy: Surgery to remove the uterus, including the cervix. When the uterus and cervix are taken out with the vagina, the operation is known as vaginal hysterectomy. If the uterus and cervix are taken out via a large incision (cut) in the abdomen, the operation is called a total abdominal hysterectomy. When the uterus and cervix are removed via a small incision in the abdomen using a laparoscope, the operation is known as total laparoscopic hysterectomy.
- Lymphadenectomy: A surgical procedure by which lymph nodes are removed and checked under a microscope for signs and symptoms of cancer. This procedure can also be called lymph node dissection. When the cancer is incorporated in the upper vagina, the pelvic lymph nodes might be removed. When the cancer is in the lower vagina, lymph nodes within the groin might be removed.
- Pelvic exenteration: Surgery to remove the lower colon, rectum, and bladder. In females, the cervix, vagina, ovaries, and nearby lymph nodes are also removed. Artificial openings (stoma) are made for urine and stool to flow from the body right into a collection bag.
Skin grafting may follow surgery, to correct or reconstruct the vagina. Skin grafting is a surgical procedure by which skin is moved from one part of the body to a different. A piece of healthy skin is obtained from part of your body that's usually hidden, like the buttock or thigh, and accustomed to repair or rebuild the region given surgery.
Whether or not the doctor removes all of the cancer that can be seen at the time of the surgery, some patients might be given radiation therapy after surgery to kill any cancer cells that are left. Treatment given following the surgery, to increase the likelihood of a cure, is called adjuvant therapy.
Radiation therapy
Radiation therapy is a cancer treatment that utilizes high-energy x-rays or other forms of radiation to kill cancer cells or have them from growing. There's two types of radiotherapy. External radiotherapy runs on the machine away from body to send radiation toward the cancer. Internal radiotherapy runs on the radioactive substance sealed in needles, seeds, wires, or catheters which are placed directly into or close to the cancer. How a radiation therapy is given depends on the kind and stage from the cancer being treated.
Chemotherapy
Chemotherapy is really a cancer treatment that uses drugs to prevent the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can affect cancer cells through the body (systemic chemotherapy). When chemotherapy is positioned directly into the spinal column, an organ, or a body cavity like the abdomen, the drugs mainly affect cancer cells in those areas (regional chemotherapy). How a chemotherapy is offered depends upon the kind and stage of the cancer receiving treatment.
Topical chemotherapy for squamous cell vaginal cancer might be applied to the vagina in a cream or lotion.
New kinds of treatment are now being tested in clinical trials. These include the following:
Radiosensitizers
Radiosensitizers are drugs that make tumor cells more responsive to radiation therapy. Combining radiotherapy with radiosensitizers may kill more tumor cells.
This summary section refers to specific treatments under study in clinical trials, but it might not mention every new treatment being studied. Information about ongoing clinical trials can be obtained from the NCI Site.
Treatments by stage
Stage 0 Vaginal Cancer (carcinoma in situ)
Treatment of vaginal squamous cell carcinoma in situ may include the following:
- Wide local excision, with or without a skin graft.
- Partial or total vaginectomy, with or with no skin graft.
- Topical chemotherapy.
- Laser surgery.
- Internal radiation therapy.
Stage I Vaginal Cancer
Treating stage I squamous cell vaginal cancer may include the following:
- Internal radiation therapy, with or without external radiation therapy to lymph nodes or large tumors.
- Wide local excision or vaginectomy with vaginal reconstruction. Radiation therapy might be given after the surgery.
- Vaginectomy and lymphadenectomy, with or without vaginal reconstruction. Radiation therapy might be given after the surgery.
Treating stage I vaginal adenocarcinoma can sometimes include the following:
- Vaginectomy, hysterectomy, and lymphadenectomy. This can be followed by vaginal reconstruction and/or radiotherapy.
- Internal radiotherapy, with or without external radiation therapy to lymph nodes.
- A mix of therapies that could include wide local excision with or without lymphadenectomy and internal radiation therapy.
Stage II Vaginal Cancer
Treatment of stage II vaginal cancer is identical for squamous cell cancer and adenocarcinoma. Treatment may include the next:
- Both internal and external radiotherapy towards the vagina, with or without external radiation therapy to lymph nodes.
- Vaginectomy or pelvic exenteration, with or without radiation therapy.
Stage III Vaginal Cancer
Treatment of stage III vaginal cancer is the same for squamous cell cancer and adenocarcinoma. Treatment may include both internal and external radiation therapy, with or without surgery.
Stage IVA Vaginal Cancer
Treating stage IVA vaginal cancer is identical for squamous cell cancer and adenocarcinoma. Treatment can sometimes include both internal and external radiotherapy, with or without surgery.
Stage IVB Vaginal Cancer
Treatment of stage IVB vaginal cancer is identical for squamous cell cancer and adenocarcinoma. Treatment can sometimes include the next:
- Radiotherapy as palliative therapy, to relieve symptoms and improve the standard of living. Chemotherapy can also be given.
- A clinical trial of chemotherapy and/or radiosensitizers.
This summary section refers to specific treatments under study in clinical trials, however it may not mention every new treatment being studied. Details about ongoing clinical trials can be obtained in the NCI Site.
Treatment options for recurrent vaginal cancer
Treating recurrent vaginal cancer may include the next:
- Pelvic exenteration.
- Radiotherapy.
- A medical trial of the new treatment.
Information about ongoing clinical trials can be obtained in the NCI Web site.






