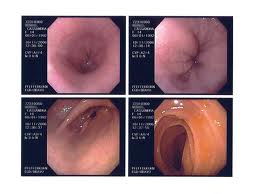
What is upper GI endoscopy?
Upper endoscopy lets patient's physician examine the lining of the upper a part of patient's gastrointestinal tract, which include the esophagus, stomach and duodenum. Your physician uses a thin, flexible tube called an endoscope, which has its lens and lightweight source, and will view the pictures on the video monitor. You might hear patient's doctor or other medical staff refer to upper endoscopy as upper GI endoscopy, esophagogastroduodenoscopy or pan endoscopy.
Why is upper GI endoscopy done?
Upper endoscopy helps patient's physician evaluate symptoms of persistent upper abdominal pain, nausea, vomiting or difficulty swallowing. It is the best test for locating the cause of bleeding from the upper gastrointestinal tract. It's also more accurate than X-ray films for detecting inflammation, ulcers and tumors from the esophagus, stomach and duodenum. Your doctor might use upper endoscopy to obtain a biopsy. A biopsy helps patient's doctor distinguish between benign and malignant tissues. Remember, biopsies are taken for a lot of reasons, as well as patient's doctor might order one even when he or she does not suspect cancer. For example, yourr doctor might use a biopsy to try for Helicobacter pylori, the bacterium that causes ulcers. Your doctor may also use upper endoscopy to execute a cytology test, where he or she will introduce a little brush to collect cells for analysis. Upper endoscopy can also be used to treat conditions from the upper gastrointestinal tract. Your doctor can pass instruments with the endoscope to directly treat many abnormalities - this makes patient little or no discomfort. For example, your doctor might stretch (dilate) a narrowed area, remove polyps or treat bleeding.
Can I take my current medications?
Most medications could be continued as usual, however, many medications can hinder the preparation or even the examination. Inform your doctor about medications patient’re taking, particularly aspirin products or antiplatelet agents, arthritis medications, anticoagulants, clopidogrel, and insulin or iron products. Also, be sure to mention any allergies patient have to medications.
What preparations are required?
A clear stomach allows for the best and safest examination, so patient must have nothing to eat or drink, including water, for about 6 hours before the examination. Your physician will explain when to start fasting as the timing can differ. Inform your doctor in advance about any medications patient take; patient might need to adjust your usual dose for the examination. Discuss any allergies to medications as well as health conditions, such as heart or lung disease.
What happens during upper endoscopy?
Your physician might begin by spraying your throat having a local anesthetic or giving a sedative to help patient relax. You'll then lie in your corner, and your doctor will pass the endoscope through the mouth area and into the esophagus, stomach and duodenum. The endoscope doesn't hinder your breathing, most sufferers consider the test only slightly uncomfortable, and several patients fall asleep throughout the procedure.
What goes on after upper endoscopy?
Your personal doctor will show patient the outcomes of the examination to patient, although patient'll likely need to wait for a outcomes of any biopsies performed. You'll be monitored until most of the effects of the medication normally wear off. Your throat may be a little sore, and patient might feel bloated because of the air introduced into your stomach during the test. You will be able to consume after patient leave unless your physician instructs patient otherwise. If patient were given sedatives throughout the procedure, someone must drive patient home and turn into along with patient. Even if patient feel alert following the procedure, your judgement and reflexes might be impaired throughout the day.
What are the possible complications of upper endoscopy?
Although complications after upper endoscopy are very uncommon, patient need to recognize early signs of possible complications. Note that bleeding may appear several days after the procedure. Contact your doctor immediately for those who have temperature following the test or if patient notice trouble swallowing or increasing throat, chest or abdominal pain, or bleeding, including black stools. Although complications may appear, they are rare when doctors who're specially trained and experienced on this procedure perform the exam. Bleeding can occur in a biopsy site or the place where a polyp was removed, but it's usually minimal and rarely requires follow-up. Perforation may need surgery but this can be a very uncommon complication. Some patients may have a reaction to the sedatives or complications from heart or lung disease. If patient have any concerns about a possible complication, it is always better to speak to your doctor immediately.






