Introduction:
Thoracoscopy is a process in which a small tube is fixed to a camera and introduced into the chest opening by means of tiny incisions in the skin layer through intercostal space. Because telescope is introdeuced in thorax so it is considered as thoracosopy. It is a Minimal Access Surgical procedure relating to interior observation, biopsy, and/or resection of disorder or masses within the pleural cavity and thoracic cavity. Thoracoscopy may be done together with under standard anesthesia or under slumber with local anesthetic. Thoracoscopic surgery is less invasive than open surgery, and requires much smaller incisions.
Pleurodesis:
Pleurodesis is a medical procedure in which pleural space is annihilated artificially that requires the attachment of two pleura. The pleural cavity is considered to be an impending gap between the visceral and parietal pleura of the lungs. The space between the two pleura is thin and known as pleural cavity, containing a small quantity of pleural fluid. Pleurodesis is done to protect against outbreaks of pneumothorax or regular pleural effusion. It can be performed chemically or surgically. It is normally evaded with cystic fibrosis patients if possible, as lung transplantation turns out to be much more challenging after this procedure.
Thoracoscopic Pleurodesis:
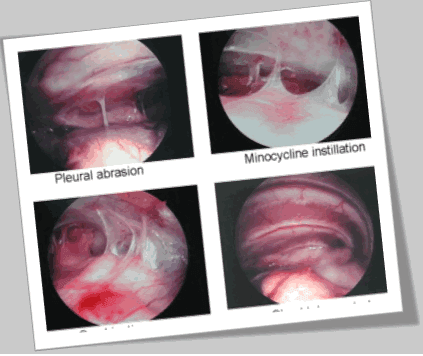
Thoracotomy or thoracoscopy is considered to be performed against the plueurodesis surgery. In this thoracoscopy, parietal pleura is mechanically irritating, most frequently with the rough pad. Meanwhile, the pleurodesis stability can be obtained via surgical eradication of parietal pleura as it is an effective method.
However, tunneled pleural catheters (TPCs) may be positioned in an outpatient place and frequent outcome in auto-pleurodesis through which compact vaccum bottles are being utilized to abandon pleural fluid. Regular venting maintains the pleura together consequently, in external or physical upheaval through the catheter that slightly triggers the pleura to scrape jointly. This process, however the minimally invasive and minimal cost solution requires normally 30 days to obtain pleurodesis and is consequently the slightest signifies the obtaining pleurodesis between different modalities.
All pleural fluid must be withdrawn just before pleurodesis is performed. This is accomplished by instilling a chest tube by means of skin and within the pleural space - thoracostomy. Instillation of the chest tube is performed in the hospital. The patient is conscience throughout the surgery. The dermis is sanitized and a injection of common pain killer is applied into the deeper layers of skin and subcutaneous tissue. A tiny slit is developed within the epidermis and a tube is inserted into the pleural space. Fluid is taken out and the tube is permanently in place eventually the entire pleural fluid is worn-out, that normally consumes two to five days. Subsequently, the patient may either stay in the hospital or be enabled to get back home with guidelines on how to concern for the tube. A chest x ray may be carried out to verify that all the fluid has been worn-out.
Pleurodesis is accomplished by means of arranging one of any number of chemicals such as sclerosing agents or sclerosants within the pleural space. The sclerosant agitates the pleurae which rewards in inflammation that is pleuritis and triggers the pleurae to adhere jointly. The patient is administered a narcotic pain reducer and lidocaine, a general pain killer, is incorporated to the sclerosant. A multitude of various chemicals are utilized as sclerosing agents. There is no one sclerosant which is highly impactful or less risky than the others. Frequently used sclerosants and their resulting success ratios are:
- Talc: 90% to 96%
- Nitrogen mustard: 52%
- Doxycycline: 90%
- Bleomycin: 84%
- Quinacrine: 70% to 90%
The tube is enclosed just after the sclerosant has been keep through the chest tube. The patient may be soliciting to adjust position every 15 minutes for a two-hour time period. This was believed to be necessary to achieve an even distribution of sclerosant in the pleural space. Then, the chest tube is reopened and the sclerosant is absorbed out of the pleural space. The tube continues to be in place for many days to let entire fluid to extract. The chest tube is removed Once drainage slows down, and the wound fringes sutured once again.
Risks and complications of pleurodesis:
Risks and complications are associated with the pleurodesis are not common containing certain infections, bleeding, acute respiratory distress syndrome, pneumothorax, and respiratory tract disorders. Moreover, fever and pain are also associated with the complications of pleurodesis, particularly for every sclerosant. These sclerosants can cause certain complications such as.
Talc and doxycycline - cause fever and pain.
- Quinacrine - cause low blood pressure, fever, and hallucination.
- Bleomycin - cause fever, pain, and nausea
Conclusion:
It may be concluded as thoracoscopic pleurodesis is the most efficient way to cure malignant pleural effusion. Successful pleurodesis protect against the repetition of pleural effusion which relieves indications thereby making better quality of life.
World Laparoscopy Hospital, Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555






