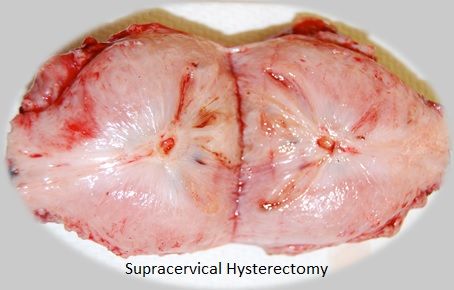
Inroduction:
Hysterectomy is one of the most common surgical procedures performed all over World. It is done for a variety of reasons including fibroids, which are benign tumors of the uterus, uncontrolled menstrual bleeding, and pelvic pain, as well as other indications. Hysterectomies are performed in a number of different ways. The traditional abdominal hysterectomy is done through either a small “bikini” type incision through the lower abdomen or occasionally an incision that’s made from the bellybutton down to the pubic bone in the middle. When a hysterectomy is performed in this manner the patient does experience significant discomfort from the incision itself and the general recuperation time is approximately six weeks. A smaller number of hysterectomies in the United States are done through the vagina. In a vaginal hysterectomy, the uterus is removed through the vagina starting with the cervix and then disconnecting the rest of the uterus after which the uterus is removed through the vagina. This surgery is generally better tolerated than the abdominal type and patients have approximately a four-week recovery with less pain.
Gynecological complications can significantly reduce the quality of life for some women. Often, with complications involving pain and abnormal bleeding, women find even activities of daily living can become quite challenging.
With abnormal bleeding, many women are opting to undergo a procedure known as laparoscopic supracervical hysterectomy. As a procedure that does not require an extensive invasive surgical process, many women are finding abnormal bleeding and associated gynecological complications are well controlled and resolved with this procedure.
While many women opt for total hysterectomy, removing the cervix, the use of supracervical hysterectomy is becoming increasingly more common as it was prior to the 1950s. The difference, today, is the method by which the hysterectomy can be performed, supracervically, without imposing extensive invasive surgery upon a woman.
The advantages of a laparoscopic supracervical hysterectomy (LSH) over an abdominal hysterectomy:
The advantages of a laparoscopic supracervical hysterectomy are:
- Smaller incisions (one centimeter in size) which allows for a quicker postoperative recovery with less postoperative pain.
- Shorter hospital stay (e.g. overnight stay) and patients go home the next day. The patient can return back to normal activities in usually 14-21 days.
- Preservation of the cervix (which does not disrupt the support of the pelvis tissue and the vaginal cavity). As a result, there is preservation of sexual function.
- Fewer surgical complications (e.g. less blood loss, decreased risk of infection, and decreased postoperative adhesion formation).
- For women who choose to undergo the laparoscopic supracervical hysterectomy find they recover much quicker, experience few urinary complications, improve their overall sex drive and libido and are given the option to retain the cervix which is crucial to managing future cervical screenings for cancer.
The greatest argument for not proceeding with the laparoscopic supracervical hysterectomy lies in the retention of the cervix itself. While some physician would argue the cervix should remain in place to ensure cervical screening for cancer can be performed, others argue the very presence of the cervix may place a woman at risk for cervical cancer. This is a gynecological debate that continues and must be weighed through your surgeon's advice and expertise. Most physicians, however, state the presence of the cervix does not pose a great risk but, instead, simply allow for screening to be done more efficiently. In terms of cost, there are few differences associated with the costs of surgery and recovery when comparing the types of hysterectomy procedures. Therefore, cost is generally not considered a factor.
For most women, the choice to proceed with a laparoscopic supracervical hysterectomy is often based on the speed by which recovery can be expected. With a more expedient recovery, many women find they can resume normal living activities and often return to work much sooner than other, more invasive hysterectomy procedures. When considering your options, therefore, it is important to consider not only timing but also the impact and need for cervical screenings of the future as these may determine which hysterectomy procedure you choose.
The advantages of a LSH (in comparison to a TLH) are:
A total laparoscopic hysterectomy (TLH) removes both the uterus and the cervix. In comparison, a laparoscopic supracervical hysterectomy removes only the body of the uterus and leaves the cervix in place. This is a woman’s personal choice. One can either elect to leave the cervix or remove the cervix at the time of the hysterectomy.
- Leaving the cervix intact maintains normal anatomical support of the pelvis. The ligaments (e.g. uterosacral ligaments) that support the cervix and the vagina are not disrupted. As a result, there is less chance of urinary incontinence and vaginal vault prolapse (the top of the vagina falling down).
- Leaving the cervix intact helps preserve sexual function. No incision is made into the vaginal canal so there is no disruption of the nerve and blood supply to the vaginal cavity. This allows one to return to normal intimacy sooner. However, more recent research shows that there is no difference in sexual function between a supracervical hysterectomy and a total hysterectomy.
- Leaving the cervix intact allows for a quicker postoperative recovery in comparison to the total laparoscopic hysterectomy (TLH). The operating room time is shorter and the time under general anesthesia is less because there is a little less cutting of tissue.
The disadvantages of a laparoscopic supracervical hysterectomy (LSH) over an abdominal hysterectomy:
- There are some drawbacks to leaving the cervix, even if it's healthy. One is the possibility of adhesions leading to chronic pelvic pain. There could also be cervical bleeding or postoperative infection of the cervical stump due to infection from the cervical canal.3 Any of these circumstances could lead to morbidity or an additional procedure to remove the cervical stump.
- A very common argument for a woman to keep her cervix focuses on the possibility of diminished sexual pleasure if it were to be removed. There's no convincing evidence either to support or refute this claim. Studies in the United States and Denmark reported no difference between preoperative and posthysterectomy sexual response, regardless of whether the cervix had been removed or not. A recent study in Atlanta, Georgia exhibited the same results, as did a 2-year follow-up of hysterectomy patients in Tucson, Arizona.
- However, in another study of 100 women in Barcelona, Spain, in which half underwent TLH and the other half the supracervical procedure, the results differed. The women in the group who didn't have their cervices removed had significantly better clinical outcomes, and stated they felt less castrated than the women who received TLH.
- A woman's personal feelings, cultural background, and self-image must be considered when deciding whether to remove the cervix. No data can predict an individual's emotional reaction postoperatively, especially if she has already formed a firm opinion of what will happen. The surgeon is obligated to explain the benefits and risks of leaving or removing the cervix, including the potential for additional future surgery. Agreement can be reached when all of the above factors are reviewed.
Limitations to the laparoscopic supracervical hysterectomy:
Although most hysterectomies can be performed laparoscopically, there are some limitations. For instance, if the size of the uterus is greater than 22 weeks in size, the fundus (the top) of the uterus reaches above the level of the umbilicus (belly button). When the laparoscopic camera is placed through the umbilicus to visualize the pelvis and the uterus, the visualization is poor and the laparoscopic access is challenging. As a result, it would significantly increase the risk of the surgical procedure. As a result, it would be recommended a total abdominal hysterectomy rather than a laparoscopic hysterectomy simply based on patient surgical safety.
Conclusion:
The laparoscopic supracervical hysterectomy allows you to return to your normal activities sooner and also provides a higher degree patient satisfaction. But you must meet the proper indications for this procedure. The indications include: (a) Your physician has recommend a total abdominal hysterectomy and you are looking for a more minimally invasive option (b) Large fibroid uterus (c) Heavy menstrual cycles and failed medical management (e.g. failed birth control pills / progesterone) (d) Dysfunctional uterine bleeding (e) Adenomyosis (f) Failed endometrial ablation (e.g. Novasure, Thermachoice, etc)






