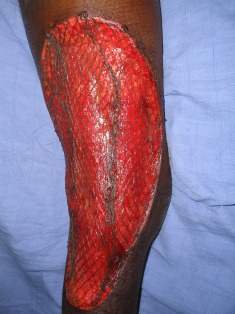
Skin grafting
Definition: Skin grafting is really a surgical treatment by which skin or perhaps a skin alternative is positioned on the burn or non-healing wound.
Purpose: An epidermis graft can be used to completely replace ruined or missing skin in order to give a temporary wound covering. This covering is essential since the skin safeguards against fluid loss, helps with temperature regulation, helping stop disease-causing bacteria or viruses from entering a patient’s body. Skin that's ruined thoroughly by burns or non-healing wounds can give up for well-being of the patient.
Description: Skin of a person undoubtedly the largest organ of the body. It's also referred to as integument or integumentary system since it covers the whole outside the body. Patient’s skin includes two primary layers: the outer layer, or epidermis, which depends on and it is revitalized through the thicker dermis. Both of these layers are around 0.04-0.08 in (1-2 mm) thick. The skin includes an outer layer of dead cells called keratinocytes, which offer a difficult protective coating, and many layers of quickly dividing cells underneath the keratinocytes. The dermis offers the arteries, nerves, sweat glands, follicles of hair, and sebaceous glands. The dermis is made up mainly of ligament that is largely comprised of a protein called collagen. Collagen provides the skin its versatility and offers structural support. The fibroblasts which make collagen would be the main kind of cell within the dermis.
Skin differs thick around patient’s body; it's thickest about the palms and soles from the feet, and thinnest about the eyelids. Generally, guys have thicker skin than women, and adults have thicker skin than children. After age 50, however, skin of every individual starts to grow thinner again since it seems to lose its variable fibers plus some of their fluid content.
Injuries given skin grafts: Skin grafting may also be done included in elective cosmetic surgery methods; nevertheless it’s most considerable one which is within the treating burns. For first or second-degree burns, skin grafting is usually not necessary, because these burns generally heal with little if any scarring. With third-degree burns, however, patient’s skin is demolished to its full depth, along with damage completed to underlying tissues. Individuals who suffer third-degree burns often need skin grafting.
Wounds for example third-degree burns should be covered as soon as possible to avoid infection or lack of fluid. Wounds which are left to heal by them can contract, often leading to serious scarring; when the wound is big enough, the scar can in fact prevent mobility of limbs. Non-healing wounds, for example diabetic ulcers, venous ulcers, or pressure sores, may be treatable with skin grafts to avoid infection and further progression from the wounded area.
Skin types grafts: The word "graft" alone generally describes either an allograft or an autograft. An autograft is a kind of graft that utilizes skin from another part of the patient's own body when there is enough undamaged skin available, and when the individual is good enough to endure the extra surgery needed. An allograft uses skin from another individual, Donor skin from cadavers is frozen, stored, and readily available for use as allografts. Skin obtained from a pet is known as xenograft since it develops from a nonhuman species (often a pig). Allografts and xenografts provide temporary covering since they're rejected through the patient's defense mechanisms within 7 days. They have to then get replaced by having an autograft.
FULL-THICKNESS GRAFTS. Full-thickness skin grafts might be essential for worse burn injuries. These grafts include both layers of your skin. Full-thickness autografts tend to be more complex than partial-thickness grafts, and still provide better contour, natural color, and less contraction in the grafted site. A flap of skin with fundamental muscle and circulation is transplanted towards the area to become grafted. This process can be used when tissue loss is considerable, for example after open fractures from the lower leg, with substantial skin loss and main infection. The rear and also the abdomen are typical donor sites for full-thickness grafts. The primary drawback to full-thickness skin grafts would be that the wound in the donor site is larger as well as more careful management needed. Often, a split-thickness graft can be used to pay for the donor site.
An amalgamated skin graft may also be used, which includes mixtures of skin and fat, skin and cartilage, or dermis and fat. Composite grafts are utilized in patients whose injuries need three-dimensional renovation. For instance, a wedge of ear containing skin and cartilage may be used to restore the nose. A full-thickness graft is taken away in the donor site having a scalpel rather than dermatome. Following the doctor has cut round the edges from the pattern accustomed to figure out how big the graft, she or he lifts your skin having a special hook and trims off any fat. The graft will be positioned on the wound and guaranteed in position with absorbable sutures.
SPLIT-THICKNESS GRAFTS. The most crucial a part of any skin graft process is appropriate preparation from the wound. Skin grafts won't survive on tissue having a restricted circulation (cartilage or tendons) or tissue that's been ruined by radiation treatment. The patient's wound should be free from any dead tissue, foreign matter, or bacterial infections. Following the patient continues to be anesthetized, the doctor works on the wound by rinsing it with saline solution or perhaps a diluted antiseptic (Betadine) and gets rid of any dead tissue by débridement. Additionally, the doctor stops the blood circulation to the wound by making use of pressure, tying off arteries, or applying drugs (epinephrine) that triggers the arteries to constrict.
Following preparation from the wound, the cosmetic surgeon then harvests the tissue for grafting. A split-thickness skin graft requires the epidermis along with a little from the fundamental dermis; the donor site generally heals within several days. The doctor first marks the outline from the wound about the skin from the donor site, enlarging it by 3-5% to permit for tissue shrinkage. The doctor runs on the dermatome (a unique device for cutting thin slices of tissue) to get rid of a split-thickness graft in the donor site. The wound ought not to be too deep if your split-thickness graft will probably be effective, because the arteries which will nurture the grafted tissue must range from dermis from the wound itself. The graft is generally obtained from a place that's in most cases hidden by clothes, like the buttock or inner thigh, and spread about the bare area to become covered. Gentle pressure from the well-padded dressing will be utilized, or perhaps a few small sutures accustomed to contain the graft in position. A sterile non adherent dressing will be put on the raw donor area for about 3 to 5 days to safeguard it from infection.
Demographics: Although patient is worried inside a fire and want an epidermis graft, the populace groups having a greater risk of fire-related injuries and deaths include:
- persons residing in rural areas
- children four years of age and younger
- persons residing in manufactured homes (trailers) or substandard housing
- adults 65 or older
Morbidity and mortality rates: The typical size a burn injury inside a patient admitted to some burn center is around 14% from the total body area. Smaller burns covering 10% from the total body area or less take into account 54% of burn center admissions, while greater burns covering 60% or even more take into account 4% of admissions. About 6% of patients admitted to lose centers don't survive, mostly due to having sustained serious inhalation injuries inside a fire. Treatment for extreme burns has enhanced dramatically previously Two decades. Today, patients can survive with burns covering as much as about 90% from the body, whilst they often face permanent bodily impairment.
Risks: The potential risks of skin grafting include those inherent in a surgical treatment which involves anesthesia. Included in this are reactions towards the medicines, difficulty in breathing, bleeding, and infection. Additionally, the potential risks of the allograft process include transmission of the infectious disease in the donor. The tissue for grafting and also the recipient site should be as sterile as you possibly can to avoid later infection that may lead to failure from the graft. Failure of the graft might results from insufficient preparation from the wound, poor blood circulation towards the injured area, swelling, or infection. The most typical reason behind graft failure may be the formation of the hematoma, or assortment of blood within the wounded tissues.
Normal results: An epidermis graft usually supplies substantial improvement within the company's wound site, and could avoid the serious problems related to burns or non-healing wounds. Normally, new arteries begin growing in the donor area to the transplanted skin within 36 hours. From time to time, skin grafts don't succeed or don't heal well. In these instances, repeat grafting is essential. Although skin graft should be protected from trauma or major stretching for 2 to 3 weeks following split-thickness skin grafting, healing from surgery is generally rapid. A dressing might be essential for up to fourteen days, with respect to the location from the graft. Any exercise or activity that extends the graft or puts it in danger of trauma ought to be avoided for 3 to 4 weeks. A 1 to 2-week hospital stay is frequently needed in cases of full-thickness grafts, since the recovery period is longer.
Aftercare: When a skin graft continues to be set up, it has to be taken care of carefully despite its healed. Patients who've grafts on the legs should stay in bed for seven to 10 days using their legs elevated. For many months, the individual should offer the graft by having an Ace bandage or Jobst stocking. Grafts on the areas from the body ought to be similarly supported after healing to diminish the quantity of contracture. Grafted skin doesn't contain sweat or sebaceous glands, and really should be moisturized daily for 2 to 3 months with mineral oil or another bland oil to avoid drying and cracking.
Aftercare of patients with significant burns usually includes psychological or psychiatric counseling in addition to wound care and physical rehabilitation, especially if the patient's face continues to be damaged. The serious pain and lengthy amount of recovery involved with burn treatment in many cases are associated with anxiety and depression. When the patient's burns took place combat, a transportation disaster, terrorist attack, or other fire involving many people, they're at high-risk of developing post-traumatic stress disorder (PTSD). Doctors treating the survivors of the nightclub fire in Rhode Island in February 2003 gave them anti-anxiety medicines inside a couple of days from the tragedy to be able to slow up the risk of PTSD.
Questions a patient should ask a doctor: Skin grafts in many cases are carried out right after any sort of accident or fire, and therefore preparation might not be possible. When the patient has got the opportunity, however, she or he may ask a doctor the next questions:
- How long will recovery take?
- What will the injured area seem like after grafting?
- Will a patient be delivered to a hospital having a special burn unit?
- How long a patient going to need to remain in a healthcare facility?
- When a patient going to have the ability to continue normal activities?
- Can the doctor explain the entire process of skin grafting experience to the patient?
Alternatives: There's been great progress within the growth and development of artificial skin substitution products recently. Although nothing works along with the patient's own skin, artificial products are essential because of the restriction of accessible skin for allografting in seriously burned patients. In contrast to allographs and xenographs, artificial skin substitutions aren't rejected through the patient's body and also really encourage the generation of recent tissue. Artificial skin generally includes a synthetic epidermis along with a collagen-based dermis. The artificial dermis includes fibers arranged inside a lattice that behave as a template for that development of recent tissue. Fibroblasts, arteries, nerve fibers, and lymph vessels from surrounding healthy tissue come to be the collagen lattice, which ultimately dissolves because these cells and structures develop a new dermis. The synthetic epidermis, which provides a temporary hurdle in this process, is finally substituted for a split-thickness autograft or by having an epidermis cultured within the laboratory in the patient's own epithelial cells.
Several artificial products are for sale to burns or non-healing wounds, including Integra®, Dermal Regeneration Template® (from Integra Life Sciences Technology), Apligraft® (Novartis), Transcyte® (Advance Tissue Science), and Dermagraft®. Scientific study has also acquired promising results growing or cultivating the patient's own skin cells within the laboratory. These cultured skin substitutes slow up the requirement for autografts and may slow up the difficulties of burn injuries. Laboratory cultivation of skin cells may enhance the prognosis for drastically burned patients with third-degree burns over 50% of the body. The recovery of those patients continues to be impeded through the reduced accessibility to uninjured skin using their own bodies for grafting. Skin substitutes could also decrease treatment costs and also the period of hospital stays. Additionally, other studies have demonstrated the potential of using stem cells collected from bone marrow or blood to be used in growing skin grafts.
Patients with less serious burns are often treated inside a doctor's office or perhaps a hospital emergency room. Patients with the following conditions, however, are often used in hospitals with specific burn units: third-degree burns; partial-thickness burns over 10% of the total body area; electrical or chemical burns; smoke inhalation injuries; or preexisting medical disorders that may mess with management, increase recovery, or impact mortality. Additionally, burned children in hospitals without qualified personnel ought to be admitted to some hospital having a burn unit. A surgical team that is experts in burn treatment and skin grafts will perform the required methods. They can sometimes include neurosurgeons, ophthalmologists, oral doctors, thoracic surgeons, psychiatrists, and trauma specialists in addition to cosmetic surgeons and dermatologists.






