Department of Anesthesiology, Medical city, Iraq, Baghdad
BACKGROUND: nausea and vomiting are frequent after general anesthesia ,the most important causes of morbidity after anesthesia and surgery are postoperative nausea and vomiting.
METHODS: A comparatives analysis of published articles was done to determine the relative efficacy and safety of ondansetron, droperidol, ,metoclopramide, dexamethasone,and Intravenous crystalloid fluid For the prevention of postoperative nausea and vomiting. I performed a literature search of English references using both the MEDLINE database and a manual search. Double-blinded, randomized, controlled trials comparing the effect of these agents in redaction or prevention of postoperative nausea and vomiting.
RESULTS: A total of 60studies were identified, of which 6were excluded for methodological concerns. For each comparison of drugs, Ondansetron ( P < 0.001) ,droperidol ( P < 0.001) were more effective than metoclopramide in preventing vomiting. We conclude that ondansetron and droperidol are more effective than metoclopramide in reducing postoperative nausea and vomiting. the incidence of vomiting was reduced in the I.V administration of crystalloid 30mg/kg in healthy adults ( P=0.001)and for dexamethsone is( P < 0.03.).
Conclusion: In summary, both ondansetron and droperidol were more effective than metoclopramide, I.V crystalloid fluid and dexamethoson in preventing postoperative vomiting.
Keywords: laparoscopy postoperative nausea and vomiting ,droperdol, metoclopramide, Ondansetron,IV crystalloid.
Introduction:
Postoperative nausea and vomiting (PONV) remains one of the most common postoperative complications and is experienced by up to 70% of patients. Hofer and colleagues{!}. It is a limiting factor in the early discharge of ambulatory surgery patients and is a leading cause of unanticipated hospital admission {2,3}. There is still controversy concerning the best approach to managing postoperative nausea and vomiting (PONV){4}.PONV can lead to increased recovery room time, expanded nursing care, and potential hospital admission—all factors that may increase total health care costs. Patients report that avoidance of PONV is of greater concern than avoidance of postoperative pain {5}. the optimal approach to PONV management remains unclear to many clinicians. Guidelines for prevention and treatment of PONV based on data from systematic reviews of randomized trials have been published {6,7}. Patients incur a fluid deficit by mandatory preoperative fasting. Guided i.v. fluid therapy improves outcomes in major surgery{8,9} It has been suggested that relative hypovolaemia may be a factor in such adverse outcomes after surgery and that preoperative administration of i.v. fluids reduces their incidence{10}.
Gan and colleagues showed an earlier return to bowel function, decreased length of hospital stay and a reduction in PONV by using oesophageal Doppler with goal-directed therapy aimed at maintaining stroke volume{11}. While they studied a major surgery group with expected blood loss in excess of 500 ml, their work supports our hypothesis that reduced bowel mucosal perfusion may be a factor in PONV. I, therefore performed a meta-analysis of published, randomized, controlled trials of prophylactic antiemetic therapy to determine the relative efficacy and safety of ondansetron, metoclopramide, droperidol,i.v crystalloid fluid and dexamethsone for preventing PONV.
Methods:
An initial list of published studies was obtained by searching the MEDLINE database from (1996 to 2007) using the terms (MeSH as well as text search) "prevention," "postoperative complications," "nausea and vomiting" separately for "ondansetron," "droperidol," "metoclopramide,dexamethasone,and I.V crystalloid fluid." The list was expanded by a manual search of table of contents in English anesthesiology journals and reference lists from all articles, review articles, correspondence, and abstracts related to PONV. Only English-language references were included .
Articles that met the following criteria were included in the meta-analysis
- the study was a double-blinded, randomized, controlled trial;
- patients underwent general anesthesia for laparoscopy;
- vomiting, nausea, or the use of rescue antiemetic therapy were identified as outcomes;
- antiemetic therapy was administered prophylactically, not just in the treatment of PONV;
- at least two drugs (metoclopramide 10mg, droperidol 20 micrgram, , ondansetron 2mg ,dexamethasne 2 mg I.V crystalloid fluid 10ml /kg and 30 ml/kg ) were compared.
The meta-analyses were designed to determine the relative efficacy of ondansetron, droperidol, , metoclopramide, dexamethasone and I.V crystalloid fluid compared with each other in reducing the odds of PONV. Separate meta-analyses were performed for the different drug combinations. All patients from the included studies were categorized as having postoperative vomiting or nausea or using rescue antiemetic medication under each two-drug comparison. In some studies, counts were calculated from percentages identified in tables or figures. Studies with different drug doses within the therapeutic range. In the study where the patients received crystalloid fluid (J.J. magner) {12} divided the patient to tow groupe the CSL-10 group (n=70) received compound sodium lactate (CSL) 10 ml kg–1; the CSL-30 group (n=70) received CSL 30 ml kg–1. CSL contains sodium 131 mmol litre–1, potassium 5 mmol litre–1, calcium 2 mmol litre–1, chloride 111 mmol litre–1 and lactate 29 mmol litre–1. To maintain patient and investigator blinding, i.v. fluid administration was initiated in the preoperative area.
Result:
The details of the articles involving a total of 676 patients included in the meta-analyses. The meta-analysis comparing the efficacy of ondansetron versus metoclopramide included 175 patients (table 1,2){12}. .droperidol versus metoclopramide analysis included (table2){13} The ondansetron versus droperidol (table3){14}and the deference between them in 1st day (figer 1)
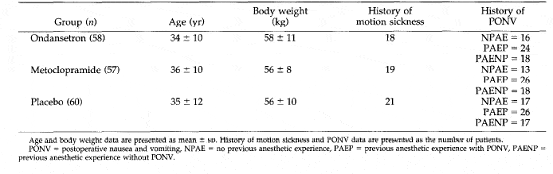
Table 1: demographicand clinical characterstic of patient population(N=175)

Table 2: Coddes ratio(95% confidance interval of one hour efficacy of antiematic regimen in 175 patients
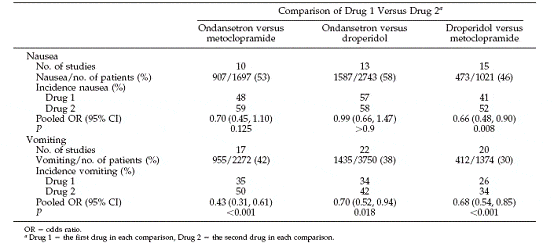
Table 3: post operative nausea and vomiting
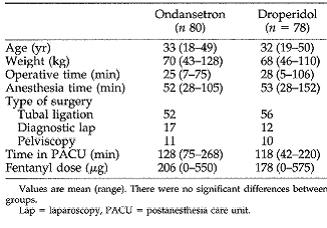
tbli 4:subject characteristics
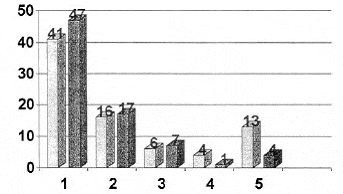
Table 5 : disterbution for nousea and vomiting post operatively in 1st 24 H
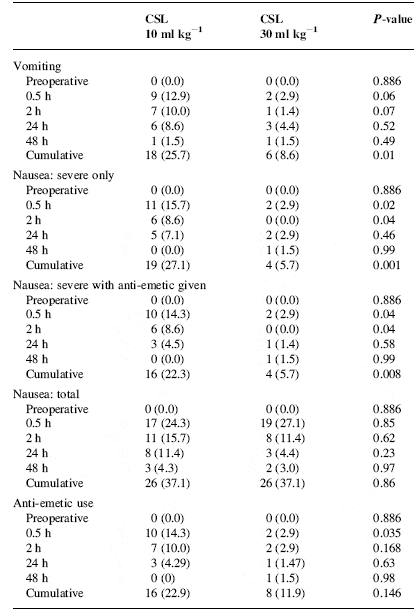
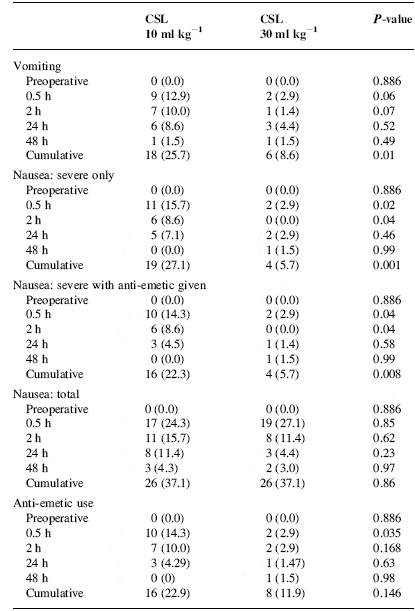
light bars=ondesteron ,dark bars= droperidol ,p=0.115 for the comparisons in the study for the patient receiving crystalloid floiud. In the first 48 h after anaesthesia, the incidence of vomiting was lower in the CSL-30 group than in the CSL-10 group (8.6% vs 25.7%, P=0.01). Anti-emetic use was less in the CSL-30 group at 0.5 h (2.9% vs 14.3%, P=0.04). The incidence of severe nausea was significantly reduced in the treatment group at awakening (2.9% vs 15.7%, P=0.02), 2 h (0.0% vs 8.6%, P=0.04) and cumulatively (5.7% vs 27.1%, P=0.001). (12)
This prospective, randomized, double-blind clinical investigation has shown a beneficial effect of rapid infusion of 30 ml kg–1 compared with 10 ml kg–1 of crystalloid solution in reducing the incidence of PONV after gynaecological laparoscopy in ASA 1 female patients. However, there were no significant differences in the subjective symptoms of dizziness, thirst or opioid consumption at any time. Sore throat was transiently increased in the CSL-30 group on emergence from anaesthesia(table 4).
Table(4): postoperative nausseaand vomiting .cumulative refers to namber of patient affected or treated,not namber of episoides CSL=compound sodium lactate.
The result for dexamethasone in comparesom with metaclopramice as in table 5,6 {15} Patients in group I reported a lower incidence of PONV and requested less rescue antiemetics than those in group III during the first four postoperative hours (P <0.01). Patients in group I reported a lower incidence of PONV than those in groups II (P <0.05) and III (P <0.01) during the 24-hr postoperative period. Groups II and III did not differ from each other in the incidence of PONV and the proportion of patients who requested rescue antiemetics.
Table 5: Patients' characteristics
| Dexamethasone (Group I) | Metoclopramide (Group II) | Saline (Group III) | |
|---|---|---|---|
| No. | 39 | 38 | 38 |
| Age (yr) | 32 (27–35) | 34 (31–36) | 35 (30–37) |
| Weight (kg) | 54 (42–72) | 56 (46–75) | 56 (45–76) |
| Height (cm) | 158 (145–172) | 157 (138–170) | 156 (139–173) |
| Interval since last menstrual period | |||
| 0–8 | 12 | 11 | 11 |
| 9–16 | 7 | 9 | 10 |
| 16–28 | 11 | 12 | 9 |
| >28 | 9 | 6 | 8 |
| Duration of anesthesia (min) | |||
| 65 (45–78) | 68 (49–78) | 64 (51–76) | |
| Duration of surgery (min) | 41 (32–63) | 45 (38–65) | 42 (38–64) |
| Values given as numbers or median (range). | |||
Table 6: Incidence of nausea and vomiting after laparoscopic tubal ligation
| Dexamethasone (Group I) | Metoclopramide (Group II) | Saline (Group III) | |
|---|---|---|---|
| No. | 39 | 38 | 38 |
| In the PACU (0-4 hr postoperatively) | |||
| - Nausea | 6 (15) | 8 (21) | 12 (32) |
| - Vomiting | 3 (8) | 6 (16) | 10 (26) |
| - Total | 9 (23) | 14 (37) | 22 (58) |
| - Rescue antiemetic | 4 (10) | 10 (26) | 16 (42) |
| After discharge (4-24 hr postoperatively) | |||
| - Nausea | 4 (10) | 6 (15) | 8 (21) |
| - Vomiting | 1 (3) | 4 (11) | 3 (8) |
| - Total | 5 (13) | 10 (26) | 11 (29) |
| From 0-24 hr postoperatively | |||
| - Nausea | 8 (21) | 12 (32) | 13 (34) |
| - Vomiting | 3 (8) | 8 (21) | 11 (29) |
| - Total | 11 (28)* | 20 (53) | 24 (63) |
| Successful protection | 28 (72)* | 18 (47) | 14 (37) |
| Values are numbers of patients (%). PACU=postanesthetic care unit. Successful protection was defined as no nausea, no vomiting and no antiemetic medication.*P <0.05 when compared with group II; P <0.01 when compared with group III using 3 x 2 2 test followed by 2 x 2 2 test. | |||
From the result we con see that the Prophylactic iv dexamethasone 5 mg significantly reduces the incidence of PONV in women undergoing ambulatory laparoscopic tubal ligation. At this dose, dexamethasone is more effective than metoclopramide 10 mg or placebo{16}.
Discussion:
The clinical benefits of routine antiemetic prophylaxis for high-risk surgical patients have been well documented in the anesthesia literature {4,20,21,22,23,24,25}. These benefits were not limited to cost savings for treatment of emetic episodes but also included improved patient satisfaction compared with simply treating esTableshed symptoms {22,23}). Although multimodal antiemetic regimens involving up to three antiemetic drugs are justified in patients at high risk of developing PONV {20}, the possibility of adverse drug interactions increases as a function of the number of drugs administered. In this meta-analysis, i demonstrated that the prophylactic administration of ondansetron and droperidol was more effective than that of metoclopramide, dexamethasone and intravenous crystalloid in preventing postoperative nausea and vomiting.the droperidol is less cost than ondasetron and the intravenous crystalloid have same effect in decreasing the postoperative nausea and vomiting so we cane use droperdol and crystalloid for prophylactic antiematic effect . the results were sometimes variable, and most studies individually lacked the power to detect differences in efficacy among the different drugs. In such settings, the use of a meta-analysis has been advocated to provide greater power to detect differences among the drugs and to obtain a more precise estimate of effect size {17,18}. The results of the meta-analyses in the present study are strengthened by the remarkable consistency of the large number of individual studies for most drug comparisons. A meta-analysis merits more confidence when the individual ORs for each study are predominately on the same side of the no difference line, an OR of 1.0 ({19}). This consistency of results occurred with both the ondansetron versus metoclopramide and the droperidol versus ondansetron analyses. This meta-analysis suggests that the usual clinical doses of either ondansetron or droperidol, rather than metoclopramide, dexamethsone, and I.V crystalloid fluid should be administered for the greatest antiemetic efficacy. Droperidol and ondansetron were similarly effective in preventing PONV in adults.
Conclusion:
All method's were associated with low incidences of postoperative nausea and vomiting .I conclude that ondansetron, droperidol, were more effective than the anther in laparoscopy .Equivalents effectiveness for ondansetron, droperidol,and significant cost saving may be obtained by using droperidol prophylactic ally for laparoscopic surgery.
References:
- Hofer CK, Zollinger A, Büchi S, et al. Patient well-being after general anaesthesia: a prospective, randomized, controlled multi-centre trial comparing intravenous and inhalation anaesthesia. Br J Anaesth 2003; 91: 631–6 (Abstract/freefull text)
- Gold BS, Kitz DS, Lecky JH, Neuhaus JM. Unanticipated admission to the hospital following ambulatory surgery. JAMA 1989; 262: 3008–10 abstract
- Fortier J, Chung F, Su J. Unanticipated admission after ambulatory surgery: a prospective study. Can J Anaesth 1998; 45: 612–9(Abstract/freefull text)
- White PF, Watcha MF. Postoperative nausea and vomiting: prophylaxis versus treatment [editorial]. Anesth Analg 1999;89:1337–9
- Macario A, Weinger M, Carney S, Kim A. Which clinical anesthesia outcomes are important to avoid? Anesth Analg 1999; 89: 652–8. (Abstract/freefull text)
- Tramèr MR. A rational approach to the control of postoperative nausea and vomiting: evidence from systemic reviews. I. Efficacy and harm of antiemetic interventions, and methodological issues. Acta Anaesthesiol Scand 2001; 45: 4–13 (ISI.midline)
- Yogendran S, Asokumar B, Cheng DC, Chung F. A prospective randomized double-blinded study of the effect of intravenous fluid therapy on adverse outcomes on outpatient surgery. Anesth Analg 1995; 80: 682–6 abstract
- Wilson J, Woods I, Fawcett J, et al. Reducing the risk of major elective surgery: randomised controlled trial of preoperative optimisation of oxygen delivery. BMJ 1999; 318: 1099–103(Abstract/freefull text)
- Mythen MG, Webb AR. Perioperative plasma volume expansion reduces the incidence of gut mucosal hypoperfusion during cardiac surgery. Arch Surg 1995; 130: 423–9 abstract
- Yogendran S, Asokumar B, Cheng DC, Chung F. A prospective randomized double-blinded study of the effect of intravenous fluid therapy on adverse outcomes on outpatient surgery. Anesth Analg 1995; 80: 682–6
- Gan TJ, Soppitt A, Maroof M, et al. Goal-directed intraoperative fluid administration reduces length of hospital stay after major surgery. Anesthesiology 2002; 97: 820–medline
- J.J.magner effect of intravenas crystalloid fliud on post operative nausea and vomiting British Journal of Anaesthesia 2004 93(3):381-385; doi:10.1093/bja/aeh219 free abstract
- Karen B. DominoComparative Efficacy and Safety of Ondansetron, Droperidol, and Metoclopramide for Preventing Postoperative Nausea and Vomiting: A Meta-Analysis. Anesth Analg 1999;88:1370
- MS Sniadach and MS Alberts A comparison of the prophylactic antiemetic effect of ondansetron and droperidol on patients undergoing gynecologic laparoscopy Anesth. Analg. 1997 85: 797-800.
- jeng: dexamethasone: laparoscopy: 48: 973: Jul 2001 Nov 2001: Jul 2001: Nov 2001:
- Capperelli JC, Ioannidis JPA, Schmid CH, et al. Large trials vs. meta-analysis of smaller trials. JAMA 1996;276:1332–8(abstract))
- Bailar JC III. The practice of meta-analysis. J Clin Epidemiol 1995;48:149–57 Medline
- LeLorier J, Grégoire G, Benhaddad A, et al. Discrepancies between meta-analyses and subsequent large randomized, controlled trials. N Engl J Med 1997;337:536–42(Abstract/freefull text)
- Scuderi PE, James RL, Harris L, Mims GR. Multimodal antiemetic management prevents early postoperative vomiting after outpatient laparoscopy. Anesth Analg 2000;91:1408–14(Abstract/freefull text)
- Tang J, Chen X, White PF, et al. Antiemetic prophylaxis for office-based surgery: are the 5-HT3 receptor antagonists beneficial? Anesthesiology 2003;98:293–8(ISI.midline)
- Tang J, Wang B, White PF, et al. The effect of timing of ondansetron administration on its efficacy, cost-effectiveness, and cost-benefit as a prophylactic antiemetic in the ambulatory setting. Anesth Analg 1998;86:274–82.absract
- Sadhasivam S, Saxena A, Kathirvel S, et al. The safety and efficacy of prophylactic ondansetron in patients undergoing modified radical mastectomy. Anesth Analg 1999;89:1340–45(Abstract/freefull text)
- .Gupta A, Wu CL, Elkassabany N, et al. Does the routine prophylactic use of antiemetics affect the incidence of postdischarge nausea and vomiting following ambulatory surgery? Anesthesiology 2003;99:488–95(ISI.midline)
- Apfel CC, Korttila K, Abdalla M, et al. A factorial trial of six interventions for the prevention of postoperative nausea and vomiting. N Engl J Med 2004;350:2441–51(Abstract/freefull text)






