Introduction:
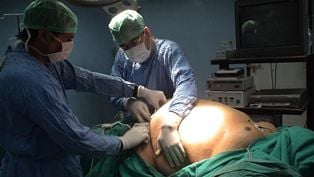
Mycobacterial infections due to atypical mycobacteria at the laparoscopic port site are a common menace encountered in patients undergoing laparoscopic surgery. Atypical mycobacterial colonies often exist in tap water, natural waters and soil and so can easily contaminate solutions and disinfectants used in hospital settings. These infections have been a source of significant morbidity for patients recovering from laparoscopic surgeries.
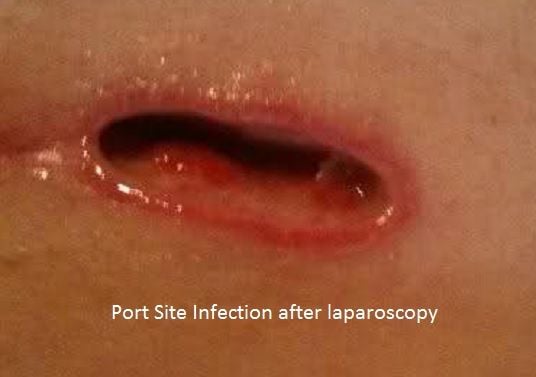
Port Site Wound infections in laparoscopy can be of two types:
- The first type occurs immediately within 1 week of laparoscopic surgery due to gram negative or positive bacteria derived from infection acquired during surgery from the infected gall bladder or from the skin or the surgical procedure itself and can be treated by common antibiotics and local wound dressing.
- The second type is caused by atypical mycobacteria which includes the group of mycobacterial species that is not part of the M. tuberculosis complex having an incubation period of 3 to 4 weeks which do not respond to common antibiotics
Infections with atypical mycobacteria have been primarily reported after laparoscopic procedures. This is because, unlike open surgery, the instruments used for laparoscopic surgery have a layer of insulation that restricts the use of the autoclave in the sterilization process as the high temperatures involved destroy the insulation on them. The standard sterilization procedure has been a 20 minute exposure to 2.0 2.5% glutaraldehyde. At the current exposure time, these solutions act only as disinfectants and not sterilants thus allowing bacterial endospores to survive.
Also, when proper mechanical cleaning of the instruments is not done, blood and charred tissue deposits are left in the joints of the instruments during laparoscopic surgery. These Contaminated instruments deposit the endospores on to the subcutaneous tissue during the surgery which then germinate following which clinical symptoms appear after an incubation period of 3 to 4 weeks.
Prevention
- Disposable laparoscopic instruments is the best solution for prevention of infection and is used in western countries.
- The use of advanced sterilization systems like STERRAD, which utilises gas plasma technology to kill spores at low temperatures, or using ethylene oxide gas for sterilization of insulated laparoscopic instruments. One can also keep instruments for 24 hours in a formalin gas chamber.
Treatment:
These microorganisms show limited response to first line anti-tuberculosis drugs. the standard treatment consist of combinations of second line anti-tubercular drugs including macrolides such as clarithromycin, quinolones like ciprofloxacin, tetracyclines like doxycycline, and aminoglycosides like amikacin.
The standard treatment starts after manifestation of clinical symptoms which consists of a 28 day regimen of oral clarithromycin and ciprofloxacin or amikacin. However, local administration of aminoglycosides has been shown to be highly efficacious in the treatment of particularly stubborn nodules and sinuses that persist after completion of oral therapy
Conclusion:
Port Site Wound infection in laparoscopy is a problem faced by laparoscopic surgeons in developing countries which is preventable through proper sterilization of instruments and early clinical diagnosis and treatment.
For more information:
World Laparoscopy Hospital, Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555
Email: contact@laparoscopyhospital.com






