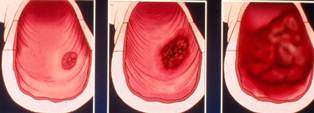
Polyps and their Treatment
What does Colon Polyp mean?
Polyps are benign growths relating to the lining from the bowel. They can occur in various locations in the gastrointestinal tract but they are most common within the colon. They differ in size from less than a quarter of an inch to several inches in diameter. They look like small bumps growing from the lining of the bowel and protruding to the lumen. They sometimes grow on the “stalk” and appear like mushrooms. Some polyps may also be flat. Many patients have several polyps scattered in different parts of the colon. Some polyps can contain small regions of cancer, even though great majority of polyps do not.
What Are The Different Types of Polyps?
There are two frequent types: hyperplastic polyp and adenoma. The hyperplastic polyp isn't in danger of cancer. The adenoma, however, is thought to be the precursor for almost all colon cancers, although most adenomas never become cancers. Histology is the best way to distinguish between hyperplastic and adenomatous polyps. Although it’s impossible to tell which adenomatous polyps will become cancers, larger polyps may become cancers and some of the largest ones can already contain small areas of cancer. Because patient’s physician can't be certain of the tissue type through the polyp’s appearance, physicians generally recommend removing all polyps found throughout a colonoscopy.
What Causes Colon Polyps? How Common Are They?
Polyps are extremely common in adults, who've a heightened chance of acquiring them, especially as we grow older. While quite exceptional in 20-year-olds, it’s projected how the average 60-year-old without unique risk elements for polyps includes a 25 % possibility of having a polyp. Some specialists believe a high-fat, low-fiber diet could be a predisposition to polyp development. There might be a genetic risk to build up polyps as well.
What Are Known Risks for Developing Polyps?
The biggest risk factor for building polyps has been over the age of 50. A household history of colon polyps or colon cancer increases the risk of polyps. Also, patients having a personal history of polyps or colon cancer are at risk of developing new polyps. In addition, there are some rare polyp or cancer syndromes that run in families and boost the risk of polyps happening at younger ages.
What Are the Risks of Polyp Removal?
Polyp removal in the course of colonoscopy is really a routine outpatient procedure. Possible complications, that are unusual, include bleeding from the polypectomy site and perforation from the colon. Bleeding in the polypectomy site could be immediate or postponed for several days; persistent bleeding can more often than not be stopped by treatment during colonoscopy. Perforations rarely happen and could require surgery to correct.
How Are Polyps Discovered?
Most polyps result in no symptoms. Bigger ones can cause blood in the stools, but even they are usually asymptomatic. Therefore, the best way to detect polyps is by screening people with no symptoms. Other screening techniques are available: testing stool specimens for traces of blood, performing sigmoidoscopy to look to the lower third of the colon, or using a radiology test such as a barium enema or CT colonography. If a person of those tests finds or suspects polyps, patient’s physician will normally suggest colonoscopy to remove them. Because colonoscopy is the most accurate method to detect polyps, many specialists now recommend colonoscopy like a screening method so that any polyps discovered or suspected can be removed throughout the same procedure.
How Are Polyps Eradicated?
Most polyps discovered during colonoscopy could be completely removed during the procedure. Various removal techniques can be found; most include removing them with a wire loop biopsy forceps and/or burning the polyp base with an electric energy. This is known as polyp resection. Because the bowel’s lining isn’t responsive to reducing or burning, polyp resection doesn’t result in uneasiness. To determine the tissue type and also to detect any cancer resected polyps are then analyzed under a microscope with a pathologist. If a large or unusual looking polyp is taken away or left for possible surgical management, the endoscopist may mark the site by inserting small amounts of sterile India ink or carbon black into the bowel wall. This is known as endoscopic tattooing.
How Often Does A Patient Need Colonoscopy if She/he Has Polyps Removed?
Patient’s physician will make a decision whenever his/her next colonoscopy is essential. The timing depends upon a number of factors, such as the number and size polyps removed, the polyps’ tissue type and the quality of the colon cleaning for the previous procedure. The caliber of cleansing affects patient’s physician’s capability to see the surface of the colon. When the polyps were small and the whole colon was well seen during patient’s colonoscopy, physicians usually recommend a repeat colonoscopy in three to five years. In case patient’s repeat colonoscopy doesn’t display any suggestion of polyps, he/she will possibly not want another procedure for an additional 5 years. However, when the polyps were big and flat, patient’s physician might advocate a period of only months before a repeat colonoscopy to declare total polyp removal. Patient’s doctor will talk about those options with him or her.






