Obesity and Sleeve Gastrectomy
Obesity has become a major health problem in the last few decades. Obesity is the most prevalent chronic disease of the 21st century. The World Health Organization (WHO) has identified obesity as one of the five leading health risks in developed countries. WHO has reported that over a billion people are overweight and that 300 million are clinically obese, with a projection of 3 million deaths annually worldwide. In the United States, 65 percent of adult Americans are overweight and 31 percent are clinically obese. Fourteen percent of American children and adolescents are obese. Bariatric surgery is now considered the only valid therapeutic option for morbidly obese patients but can be associated with significant risk, especially in patients affected by life-threatening comorbidities. Morbid obesity [defined as a body mass index (BMI) more than 40 kg/m2] affects 4.7 percent of Americans and these numbers are rapidly rising. For these patients, surgery represents the most effective treatment. However, failure is a frequent issue, and the selection of correct surgery is paramount to success.
A sleeve gastrectomy is a restrictive form of weight loss surgery in which approximately 85 percent of the stomach is removed leaving a cylindrical or sleeve-shaped stomach with a capacity ranging from about 60 to 150 cc. The stomach is reduced to about 15 percent of its original size, by surgical removal of a large portion of the stomach along the greater curvature. The open edges are then attached together with the help of a stapler to form a sleeve or tube with a banana shape. The procedure permanently reduces the size of the stomach. The procedure is performed either open or laparoscopically and is not reversible.
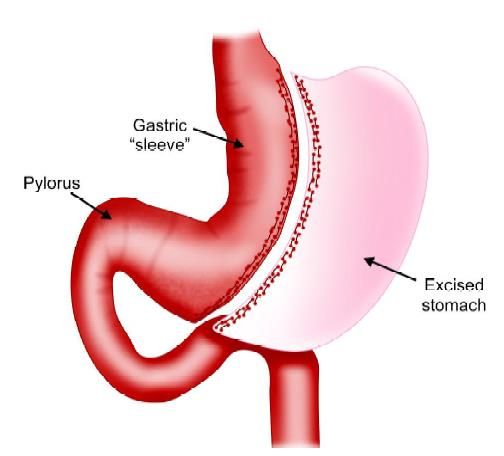
Sleeve gastrectomy
Ghrelin hormone
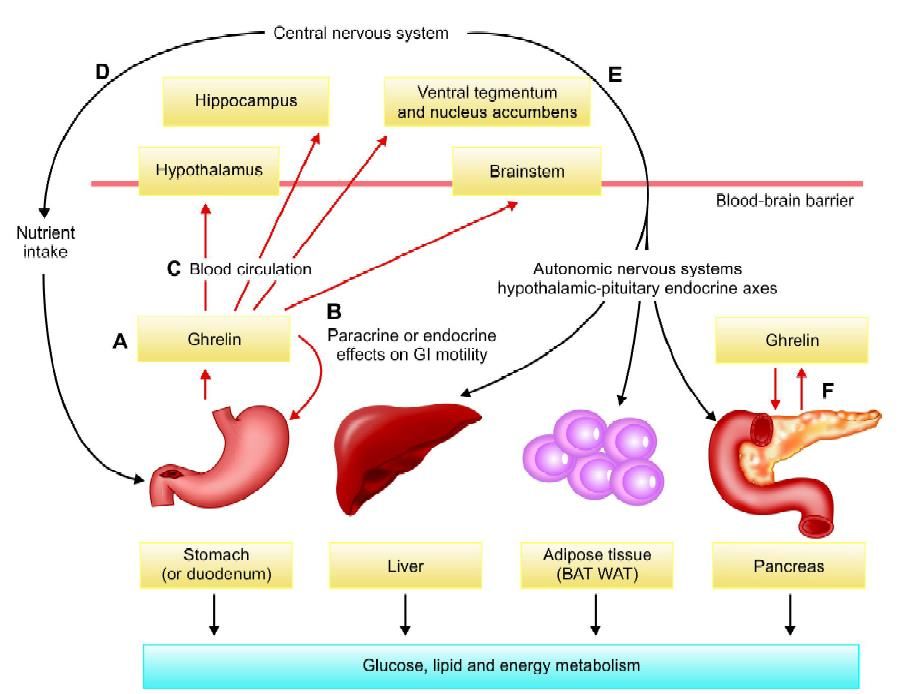
Role of ghrelin in glucose and lipid metabolism
Laparoscopic sleeve gastrectomy is a relatively new option originally published by Marceau et al. Unlike many other forms of bariatric surgery, the outlet valve and the nerves to the stomach remain intact and, while the stomach is drastically reduced in size, its function is preserved. Again, other forms of surgery such as the Roux-en-Y gastric bypass, the sleeve gastrectomy is not reversible.
Because the new stomach continues to function normally there are far fewer restrictions on the foods which patients can consume after surgery, although the quantity of food eaten will be considerably reduced. This is seen by many patients as being one of the great advantages of the sleeve gastrectomy, as is the fact that the removal of the majority of the stomach also results in the virtual elimination of hormone (Ghrelin) produced within the stomach which stimulate hunger.
Ghrelin Hormone
Ghrelin got its name from the word “ghre” from the Proto- Indo-European language, meaning to grow. Scientists did not go purposefully looking for a substance that stimulated appetite. Indeed the discovery of ghrelin occurred when scientists were investigating drugs that stimulated the release of growth hormone from the anterior pituitary gland. They came across some drugs that, rather than acting on the growth hormone-releasing hormone receptor, were acting on an unknown receptor located in the hypothalamus and pituitary, these drugs were called growth hormone secretagogues. It was concluded that the body had a second pathway for the induction of growth hormone secretion.
Ghrelin was identified as being the natural legend for these receptors causing secretion of growth hormone in 1999 by the Japanese scientist Masayasu Kojima (see key references). During Kojima's investigations, they found that although ghrelin's receptors were in the brain, ghrelin was surprisingly identified in the human stomach and circulating in the blood leading to the conclusion that it was released from the stomach where it then traveled in the blood and acted on the brain.
Ghrelin is a hormone produced mainly by P/D1 cells lining the fundus of the human stomach and epsilon cells of the pancreas that stimulates hunger. Ghrelin levels increase before meals and decrease after meals. It is considered as the counterpart of the hormone leptin, produced by adipose tissue, which induces satiation when present at higher levels. In some bariatric procedures, the level of ghrelin is reduced in patients, thus causing satiation before it would normally occur. Ghrelin is also produced in the hypothalamic arcuate nucleus, where it stimulates the secretion of growth hormone from the anterior pituitary gland. Receptors for ghrelin are expressed by neurons in the arcuate nucleus and the ventromedial hypothalamus. Once the high amount of ghrelin is secreted the patient feels intense hunger. Apart from hunger, ghrelin plays a significant role in neurotrophy, particularly in the hippocampus, and is essential for cognitive adaptation to changing environments and the process of learning.
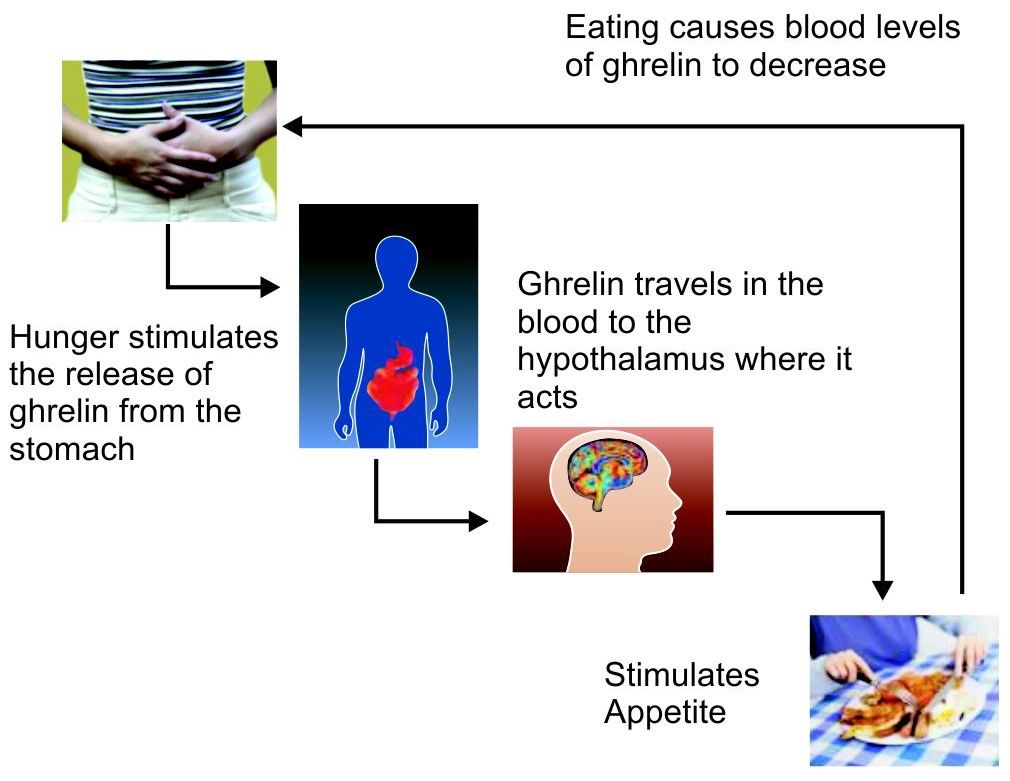
Mode of action of ghrelin
Ghrelin has emerged as the first circulating hunger hormone. Ghrelin and synthetic ghrelin mimetic increase food intake and increase fat mass by an action exerted at the level of the hypothalamus. They activate cells in the arcuate nucleus that include the orexigenic neuropeptide Y (NPY) neurons. Ghrelin-responsiveness of these neurons is both leptin- and insulin-sensitive. Ghrelin also activates the mesolimbic cholinergic-dopaminergic reward link, a circuit that communicates the hedonic and reinforcing aspects of natural rewards, such as food, as well as of addictive drugs, such as ethanol.
Ghrelin levels in the plasma of obese individuals are lower than those in leaner individuals. Recently, Scripps research scientists have developed an anti-obesity vaccine, which is directed against the hormone ghrelin. The vaccine uses the immune system, specifically antibodies, to bind to selected targets, directing the body's own immune response against them. This prevents ghrelin from reaching the central nervous system, thus producing the desired reduction in weight gain.
Obesity is the result of multifactorial changes involving both genetic and environmental factors. The physiopathology of obesity from the point of view of intake regulation has led to numerous experimental studies aimed at identifying new forms of regulation. These new forms of regulation are not only found in the secretion of ghrelin from the gastrointestinal system but also in the adipose tissue (via the metabolism of leptin and insulin) and the central nervous system to finally produce the relevant orexigenic or anorexigenic effect.
Obesity has become a major health problem in the last few decades. Obesity is the most prevalent chronic disease of the 21st century. The World Health Organization (WHO) has identified obesity as one of the five leading health risks in developed countries. WHO has reported that over a billion people are overweight and that 300 million are clinically obese, with a projection of 3 million deaths annually worldwide. In the United States, 65 percent of adult Americans are overweight and 31 percent are clinically obese. Fourteen percent of American children and adolescents are obese. Bariatric surgery is now considered the only valid therapeutic option for morbidly obese patients but can be associated with significant risk, especially in patients affected by life-threatening comorbidities. Morbid obesity [defined as a body mass index (BMI) more than 40 kg/m2] affects 4.7 percent of Americans and these numbers are rapidly rising. For these patients, surgery represents the most effective treatment. However, failure is a frequent issue, and the selection of correct surgery is paramount to success.
A sleeve gastrectomy is a restrictive form of weight loss surgery in which approximately 85 percent of the stomach is removed leaving a cylindrical or sleeve-shaped stomach with a capacity ranging from about 60 to 150 cc. The stomach is reduced to about 15 percent of its original size, by surgical removal of a large portion of the stomach along the greater curvature. The open edges are then attached together with the help of a stapler to form a sleeve or tube with a banana shape. The procedure permanently reduces the size of the stomach. The procedure is performed either open or laparoscopically and is not reversible.

Sleeve gastrectomy

Ghrelin hormone

Role of ghrelin in glucose and lipid metabolism
Laparoscopic sleeve gastrectomy is a relatively new option originally published by Marceau et al. Unlike many other forms of bariatric surgery, the outlet valve and the nerves to the stomach remain intact and, while the stomach is drastically reduced in size, its function is preserved. Again, other forms of surgery such as the Roux-en-Y gastric bypass, the sleeve gastrectomy is not reversible.
Because the new stomach continues to function normally there are far fewer restrictions on the foods which patients can consume after surgery, although the quantity of food eaten will be considerably reduced. This is seen by many patients as being one of the great advantages of the sleeve gastrectomy, as is the fact that the removal of the majority of the stomach also results in the virtual elimination of hormone (Ghrelin) produced within the stomach which stimulate hunger.
Ghrelin Hormone
Ghrelin got its name from the word “ghre” from the Proto- Indo-European language, meaning to grow. Scientists did not go purposefully looking for a substance that stimulated appetite. Indeed the discovery of ghrelin occurred when scientists were investigating drugs that stimulated the release of growth hormone from the anterior pituitary gland. They came across some drugs that, rather than acting on the growth hormone-releasing hormone receptor, were acting on an unknown receptor located in the hypothalamus and pituitary, these drugs were called growth hormone secretagogues. It was concluded that the body had a second pathway for the induction of growth hormone secretion.
Ghrelin was identified as being the natural legend for these receptors causing secretion of growth hormone in 1999 by the Japanese scientist Masayasu Kojima (see key references). During Kojima's investigations, they found that although ghrelin's receptors were in the brain, ghrelin was surprisingly identified in the human stomach and circulating in the blood leading to the conclusion that it was released from the stomach where it then traveled in the blood and acted on the brain.
Ghrelin is a hormone produced mainly by P/D1 cells lining the fundus of the human stomach and epsilon cells of the pancreas that stimulates hunger. Ghrelin levels increase before meals and decrease after meals. It is considered as the counterpart of the hormone leptin, produced by adipose tissue, which induces satiation when present at higher levels. In some bariatric procedures, the level of ghrelin is reduced in patients, thus causing satiation before it would normally occur. Ghrelin is also produced in the hypothalamic arcuate nucleus, where it stimulates the secretion of growth hormone from the anterior pituitary gland. Receptors for ghrelin are expressed by neurons in the arcuate nucleus and the ventromedial hypothalamus. Once the high amount of ghrelin is secreted the patient feels intense hunger. Apart from hunger, ghrelin plays a significant role in neurotrophy, particularly in the hippocampus, and is essential for cognitive adaptation to changing environments and the process of learning.

Mode of action of ghrelin
Ghrelin has emerged as the first circulating hunger hormone. Ghrelin and synthetic ghrelin mimetic increase food intake and increase fat mass by an action exerted at the level of the hypothalamus. They activate cells in the arcuate nucleus that include the orexigenic neuropeptide Y (NPY) neurons. Ghrelin-responsiveness of these neurons is both leptin- and insulin-sensitive. Ghrelin also activates the mesolimbic cholinergic-dopaminergic reward link, a circuit that communicates the hedonic and reinforcing aspects of natural rewards, such as food, as well as of addictive drugs, such as ethanol.
Ghrelin levels in the plasma of obese individuals are lower than those in leaner individuals. Recently, Scripps research scientists have developed an anti-obesity vaccine, which is directed against the hormone ghrelin. The vaccine uses the immune system, specifically antibodies, to bind to selected targets, directing the body's own immune response against them. This prevents ghrelin from reaching the central nervous system, thus producing the desired reduction in weight gain.
Obesity is the result of multifactorial changes involving both genetic and environmental factors. The physiopathology of obesity from the point of view of intake regulation has led to numerous experimental studies aimed at identifying new forms of regulation. These new forms of regulation are not only found in the secretion of ghrelin from the gastrointestinal system but also in the adipose tissue (via the metabolism of leptin and insulin) and the central nervous system to finally produce the relevant orexigenic or anorexigenic effect.






