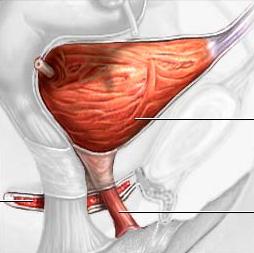
Needle bladder neck suspension
Definition
Needle bladder neck suspension, also called needle suspension, or paravaginal surgery, is conducted to aid the hypermobile, or moving urethra using sutures to add it to tissues since the pelvic floor. From the 3 popular surgical treatments for urethral lack of stability and it lead to urinary stress incontinence, needle bladder neck suspension may be the fastest and simplest to do. Its many variants, like the Raz, Stamey, customized Pereyra, or Gattes procedures, nevertheless its long-term answers are less impressive than other, more extensive, anti-incontinent surgeries.
Who performs the process and where could it be carried out?
Surgery is conducted with a urological surgeon that has a medical degree with advance learning urology as well as in surgery. Surgery is conducted inside a general hospital.
Demographics
Women go through bladder control problems two times as frequently men because of pregnancy, childbirth, menopause, and also the structure from the female urinary and gynecological systems. Anyone may become incontinent because of neurological injury, birth defects, cardiac conditions, multiple sclerosis and chronic problems in later life. Incontinence doesn't naturally go with old age but is assigned too many chronic problems that take place as age heightens. Incontinence is extremely related to obesity and insufficient exercise. As much as 15-30% of adults over 60 possess some type of bladder control problems. Stress incontinence is, undoubtedly, the commonest type of incontinence and it is the most typical kind of urinary control condition in younger and middle-age women.
Purpose
Half a century of surgical tries to treat incontinence, particularly in women, has led to three kinds of surgery associated with fundamentally three reasons for a specific kind of incontinence associated with muscle weakening from the urethra and also the "gate-keeping" sphincter muscles. Stress bladder control problems, the unmanageable leakage of urine when pressure is placed on the bladder during sneezing, coughing, laughing, or exercising, is extremely experienced by women too, and it is projected to influence 50% of elderly women in long-term care facilities. Not being able to hold urine has 2 causes. Patient has related to support for that urethra and bladder, referred to as genuine stress incontinence (GSI), and also the other relates to the shortcoming of sphincter muscles, or inbuilt sphincter deficiency (ISD), to maintain the opening from the bladder closed.
In GSI, weak muscles supporting the urethra ensure it is displaced and/or descend to the pelvic-floor fascia that will create cystoceles, or pockets. The aim of surgery for GSI would be to strengthen the sub-urethral fascia to avoid the urethra from being overly mobile during enhanced abdominal pressure. Another major supply of stress incontinence is a result of weakening from the internal muscles from the sphincter, because they affect closure from the bladder. During sex, known as the intrinsic sphincter muscles, control the frequent lowering and raising from the bladder whenever a decision is built to urinate. Lack of the intrinsic sphincter muscles causes the opening to stay open and therefore results in chronic incontinence. ISD is really a supply of serious stress incontinence and could be coupled with urethral hypermobility.
The process of surgery for stress incontinence would be to sufficiently assess the actual supply of incontinence, whether GSI or ISD, also to determine the probability of cystoceles that could need repair. Under good diagnostic circumstances, surgery for stress incontinence will start using a suprapubic procedure, or Burch procedure, to risk-free the hypermobile urethra and stabilize it inside a neutral position. Surgery for ISD uses what's known as the sling procedure, or "hammock" effect, that utilizes auxiliary tissue to undergird the urethra and supply contractive pressure towards the sphincter. Most stress incontinence surgeries fall under one of these simple two methods and their variants.
Needle neck bladder suspension, the 3rd most utilized process of stress incontinence, simply tries to add the urethra neck towards the posterior pelvic wall with the vagina or abdomen to be able to stabilize the urethra. It's, however, considered an undesirable choice compared to another two procedures due to the insufficient long-term efficacy and it is high incidence of urinary retention being an operative problem.
Questions a patient should ask a doctor:
- Are there other surgical treatments which are far better for my incontinence?
- Is surgery only option to coping with bladder control problems?
- Will doctor explain why this process is superior to what's known as the "sling procedure"?
- Will the patient get recommendation for any literature to read that explains surgical choices for incontinence?
Description
Needle bladder neck suspension surgery can be carried out as open abdominal or vaginal surgery, or laparoscopically, that allows for small incisions, video magnifying from the operative field, and accurate keeping sutures. Within general anesthetic, the individual is positioned ready on her behalf back with legs in stirrups allowing use of the suprapubic area. A Foley catheter is placed to the bladder. Outdoors procedure requires the passage of the needle in the suprapubic area towards the vagina with several sutures through looping. Cytoscopic monitoring prevents passage from the needle with the bladder or even the urethra. The laproscopic method enables visualization from the needle pass produced from the suprapubic area towards the vagina and also the looping technique. The vagina and also the surrounding areas are completely irrigated by having an antibiotic solution through the procedure. The individual is discharged exactly the same evening or even the next morning using the catheter in position. She's continued antibiotics and analyzed about the fourth next day of surgery using the elimination of the catheter. The follow-up evaluation includes wound inspection as well as an evaluation of left over urine. A pelvic examination is conducted to check on for bleeding or injury.
Diagnosis/Preparation
Stress bladder control problems may have a series of causes. It is necessary that patients consult with their doctors to eliminate medication-related, psychological, and/or behavioral causes of incontinence in addition to physical and neurological causes. This requires total health background, in addition to medication, clinical, neurological, and radiographic assessments. Once they are completed, urodynamic tests that assess the urethra, bladder, flow, urine retention, and leakage, are carried out and permit problems to look for the primary supply of the strain incontinence. Patients who're obese and/or participate in high-impact exercise aren't good candidates with this surgery. Patients with ISD might not be cured with this particular procedure, as it is primarily meant to treat the hypermobile urethra.
Morbidity and mortality rates
Urologic surgery has natural morbidity and mortality risks associated primarily to general surgery, with lung conditions, thrombus, infections and cardiac events taking place in a tiny percentage of surgeries, in addition to the kind of procedure. Additionally, the American Urological Association has figured needle suspension surgery includes a series of difficulties related straight to suturing within the suprapubic area. These difficulties :
- urethral injury, although rare, in a tiny percentage of cases
- a 5% incidence of bladder injury
- wound infections within 7% of cases, with higher rates the type with diabetes or obesity
- Nerve entrapment because of lateral keeping the sutures to the fascia at the rear of the suprapubic area
- bleeding, by having an incidence of 3-5%, primarily in the area below the pubic area
These operative difficulties, in conjunction with the procedure's high rate of described pain after surgery, and it is relatively high rate of urinary retention staying longer than a month, have led to needle neck suspension using a limited role within the management of stress bladder control problems.
Normal results
Despite adjustments to the needle suspension method, the long-term result of the process doesn't point out its lasting efficacy. Based on a current report through the AUA, research from the results of needle suspension found merely a 67% cure, or "dry rate," after 48 months, with postponed failures of sutures in an exceedingly large part of cases.






