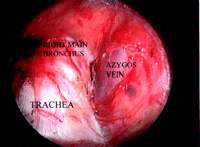
Mediastinoscopy
Definition
Mediastinoscopy is really a surgical procedure which allows physicians to view regions of the mediastinum, the cavity behind the sternum that lies between the lungs. The organs within the mediastinum include the heart and it is vessels, the lymph nodes, trachea, esophagus, and thymus. Mediastinoscopy is most commonly used to identify or stage cancer. It is also ordered to identify infection, and also to confirm diagnosis of certain conditions and diseases from the respiratory organs. The process requires insertion of the endotracheal tube, followed by a small incision in the chest. A mediastinoscope is inserted with the incision. The purpose of these devices is to allow the physician to directly see the organs within the mediastinum, and to collect tissue samples for laboratory study.
Purpose
Mediastinoscopy is often the diagnostic method of choice for detecting lymphoma, including Hodgkin's disease. The diagnosis of sarcoidosis and the staging of lung cancer can also be attained through mediastinoscopy. Lung cancer staging involves a resolution of the amount or progression from the cancer into stages. These stages help patient’s physician study cancer and supply consistent cancer treatments. Additionally they supply some guidance regarding prognosis. If lung cancer has spread beyond the lungs will probably revealed by the lymph nodes in the mediastinum. Mediastinoscopy allows patient’s physician to observe and draw out a sample from the nodes for more study. Involvement of these lymph nodes indicates diagnosing and stage of lung cancer.
Mediastinoscopy can also be ordered to ensure an analysis which was not clearly confirmed by other methods, for example certain radiographic and laboratory studies. Mediastinoscopy may aid in some surgical biopsies of nodes or cancerous tissue within the mediastinum. In fact, a doctor may immediately execute a surgical treatment if a malignant tumor is confirmed while the patient is undergoing mediastinoscopy. In these instances, the diagnostic exam and surgical procedure are combined into one operation.
Demographics
Nearly all pulmonary nodules are diagnosed via mediastinoscopy.
Description
Mediastinoscopy is usually carried out in a hospital under general anesthesia. Prior to the general anesthesia is administered, local anesthesia is applied to the throat while an endotracheal tube is placed. Once the patient is under general anesthesia, a little incision is created, usually just beneath the neck or at the notch at the top of the sternum. The doctor may clear a path and have the person's lymph nodes first to evaluate any abnormalities within the nodes. The scope is a narrow, hollow tube with an attached light that allows the doctor to see within the area. Next, problems insert the mediastinoscope with the incision. The doctor can put equipment through the hollow tube to help perform biopsies. A tissue sample in the lymph nodes or a mass can be taken off and sent for study under a microscope, or to a laboratory for more testing. In some instances, tissue sample analysis that shows malignancy will suggest the requirement for immediate surgery while the person has already been prepared and under anesthesia. In some cases, the physician will complete the visual study and tissue removal, and stitch the little incision closed. The individual will remain within the surgical recovery area before effects of anesthesia have lessened and it is safe to leave the region. The entire procedure should require about an hour, not counting preparation and recovery time. Mediastinoscopy is really a safe, systematic, and cost-effective diagnostic device with less risk than some other procedures.
Diagnosis/Preparation
Because mediastinoscopy is really a surgical treatment, it should only be performed when the advantages of the exam's findings over-shadow the risks of surgery and anesthesia. Individuals who previously had mediastinoscopy shouldn't receive it again when there is scarring from the first exam. Other medical conditions, for example impaired cerebral circulation, obstruction or distortion of the upper airway, or thoracic aortic aneurysm could also prevent mediastinoscopy. Certain structures in a person's anatomy that may be compacted through the mediastinoscope may complicate these pre-existing health conditions.
Patients are asked to sign a consent form after reviewing the risks of mediastinoscopy and known risks and reactions to anesthesia. The physician will normally instruct the patient to fast from midnight before the test until following the procedure is finished. A physician could also suggest a sedative the night prior to the exam and again prior to the procedure. Often a local anesthetic is going to be applied to the throat to avoid irritation during keeping the endotracheal tube.
Risks
Difficulties from the actual mediastinoscopy procedure are relatively rare. The following difficulties have been presented in decreasing order of frequency:
- hemorrhage
- pneumothorax (air within the pleural space)
- recurrent laryngeal nerve injury, causing hoarseness
- infection
- tumor implantation within the wound
- phrenic nerve injury
- esophageal injury
- chylothorax
- air embolism
- transient hemiparesis
The usual risks associated with general anesthesia also affect this procedure.
Morbidity and mortality rates
Abnormal findings might point to cancer of the lung, tuberculosis, the spread of disease in one part of the body to a different, sarcoidosis (a disease that triggers nodules, usually affecting the lungs), lymphoma (abnormalities within the lymph tissues), and Hodgkin's disease. Complications of mediastinoscopy include bleeding, pain, and post-procedure infection. They are relatively uncommon. Mortality is extremely rare.
Normal results
Within the most of procedures done to identify cancer, an ordinary result indicates the presence of small, smooth lymph nodes, and no abnormal tissue, growths, or signs of infection. Regarding lung cancer staging, answers are associated with the severity and progression from the cancer.
Aftercare
Following mediastinoscopy, patients will be carefully monitored and watched for changes in vital signs, or the signs of problems in the procedure or anesthesia. The patient might have an aching throat in the endotracheal tube, experience temporary heart problems, and also have soreness or tenderness at the incision site.
Important Questions a patient should ask the Doctor while going for Mediastinoscopy.
- Why is this test required?
- Is the test dangerous?
- How long will the exam take?
- What type of anesthesia will be used?
- What test preparation is needed?
- When will the outcomes be available?
- What may be the Physician’s complications rate?
- How many mediastinoscopy procedures have got the doctor performed?
Alternatives
A less invasive way is ultrasound. However, it's not as specific as mediastinoscopy, and the information obtained is not as beneficial in making a diagnosis. Although still performed, there's a decline within the utilization of mediastinoscopy as a result of advancements in computed tomography (CT), magnetic resonance imaging (MRI), and ultrasonography techniques. In addition, improved fine-needle aspiration outcomes of and core-needle biopsy (using a needle to acquire a small tissue sample) investigations, along with new approaches to thoracoscopy offers additional options in examining masses within the mediastinum. Mediastinoscopy are usually necessary when other methods cannot be used or when they provide uncertain results.
Who performs and where the procedure is performed?
A mediastinoscopy procedure is usually performed by a thoracic or general surgeon inside a hospital setting.






