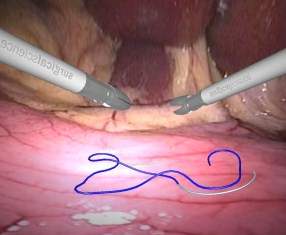
Endo suturing and Tissue Approximation in Laparoscopic Surgery
Endoscopic surgery is speedily being a well-known option to traditional procedures for variety of diseases and many of these procedures may need the employment of Laparoscopic suturing. Laparoscopic ligation and suturing can be used for approximation of tissues and it is also an effective way of delivering hemostasis. The adaptation of tissue and suturing for hemostasis and reformation of anatomic components has been considered probably the most demanding of endoscopic technical skills. Endoscopic procedures are performed by taking a look at a 2 dimensional TV screen with as many as 6 times magnification, eliminating depth perception and the tactile feeling of the tissues; this involves significant hand - eye coordination. The state-of-the-art endoscopic procedures demand the laparoscopic surgeon to master suturing. Each and every surgeon performing laparoscopic procedures ought to be extensively acquainted with basic principles of knotting and suturing.
KNOTS IN SURGICAL PRACTICE
In context with laparoscopic surgery the knots are categorized as
- Intracorporeal Knots
- Extracorporeal Knots
Intracorporeal Knots
These are tied within your body cavities utilizing needle holders. The various knots used in Endoscopic practice are:
- The square knot (Reef knot). It is a safe knot for securing small arteries and includes two opposite half knots.
- The ligature knot. It is safer compared to reef knot and employs an initial double knot then a single half knot
- The double knot. It consists of two double half knots.
- The Mayo knot. It includes two identical half knots forming a granny knot followed by a third and opposite half knot which looks the completed knot.
- The surgeons knot. It consists of a double half knot followed by two single half knots. The favored internal knot for interrupted suturing in Endoscopic surgical practice will be an surgical knot or a square knot.
IDEAL STITCH
An ideal stitch is a which supports the tissue edges as well as correct tension and resists reverse slippage.
- The three procedures in knotting
- Tying the knot (configuration)
- Working or drawing the knot (shaping)
- Snuggling or locking the knot (securing)
All of the three stages are essential along with a knot is secure only if it is tied correctly, drawn (shaped) to adapt to the anatomy of the knot and locked tightly. As Clifford Ashely wrote ‘a knot is never nearly right; it is either exactly right or is hopelessly wrong’.
The perfect characteristics of the surgical knot are:
- It ought to be safe
It ought to be quick also it should simple to tie
Triadic relationship of port sites. In suturing placed in Endoscopic surgery it is advisable to always maintain some relationship between your both sides. The telescope and suturing port sites form a triad with the optical port within the center, and suturing ports on each side.
Wrapping processes for knotting: There's two basic techniques of wrapping most commonly practiced by Endoscopic surgeons.
- Overwrap method
- Underwrap method
Essentials in intracorporeal knot tying:
A period of ligature materials for trying a knot (just like a rope) can be considered as consisting of three sections
- the end
- the bight
- the standing part
The essentials that ought to be followed while intracorporeal knotting are listed below:
- Good magnification
- Economy of motion
- Directional hold principle
- Avoidance of instrument crossing
- Correct knot - tying choreography
- Execution of the knots near to the tissue surfaces
- Closed instrument jaws except during grasping
- Awareness of dominant versus assisting instruments throughout the knotting process
- Correct wrapping techniques
- Knots con?gured and tied near to the tail
Extracorporeal Knots
External or extracorporeal slip knots are used in endoscopic surgery for:
- Ligature of vessels and tubular structures in continuity
- Transfixation of huge vascular pedicles
- Interrupted suturing with external knots
In all these situations, the knot is tied and drawn outside the body after which ‘slipped down’ with a knot pusher towards the intended target after which stiffened by traction on the standing up part against the knot pusher.
Extracorporeal versus Intracorporeal knots:
More often than not during endoscopic surgery, intracorporeal knotting utilizing instrument - tied knots is preferred to extracorporeal tying. However in the next situations extracorporeal knotting is recommended:
- Ligature in continuity of large vessels
- Suturing in regions of limited access where the performing space is restricted
- In the approximation of edges of defects where the force necessitates approximating the edges is substantial
Rules governing external slip knotting
The following rules should be followed for safe ligature for slip knots in endoscopic surgery are:
- Type of the thread must be 1.5 m and also the guage ought to be 2/0 or greater.
- The type of slip knot selected depends upon the ligature material being used. Certain slip knots provide suf?cient holding strength with catgut but not along with other materials.
- For any ligature material, the holding force (resistance to reverse slipping) of any surgical slip knot varies directly using its caliber. Thus the holding strength of a 1/0 slip knot is roughly twice those of the 2/0 equivalent.
- Stiff hydrophobic mono?lament material ought to be avoided since it exerts a lesser frictional hold and has a larger tendency to spill than braided.
Extracorporeal knots utilized in endoscopic surgical practice
- Tayside knot
- Roeder knot Click here to learn Roeders Knot
- Melzer knot Click here to learn Melzers Knot
- square knot
- Mishra Knot Click here to learn Mishra Knot
SUTURE MATERIAL
In endoscopic surgical practice there is a large variation in choice of suture materials amongst individual surgeons. The overall preferences which exist in today’s practice are listed below:
A) Absorbable sutures
- Catgut- Poor gliding ability
- Vicryl- Good maneuverability
- PDS- Excellent gliding ability, no need to follow during intracorporeal anastomosis
B) Non-absorbable sutures
- Silk- it's braided and thus more traumatizing
- Prolene- Mono?lament but has memory so makes it very tedious to use
- Ethibond- Mono?lament with less memory and better maneuverability than problem
Needles
Surgical needles are penetrating devices which are designed to pass sutures through tissues with minimum trauma. Objective of surgical needles
- To give a secure grip for that needle driver.
- To penetrate the object to become sewn and create a channel for that thread to go in.
- To provide a strategies by which thread can be trailed
Needle used in Laparoscopic / Endoscopic surgical practice
Straight needle
The advantages of using straight needle in endoscopic surgery are:
- Easy to introduce even through the smallest port direction of the needle tip is not altered by the needle
- Wivel within the jaws of needle holder
- The positioning of the straight needle involves movement in the 2-D plane
Curved needle
Tendency to swivel require more experience. Most often we make use of a 25mm and a half circle needle for endosuturing.
Endoski needle
This combined needle was developed specifically for laparoscopic use within order to combine the positive attributes of the curved needle in terms of needle passage through tissues with the ease of handling of straight needles. The dynamic suturing component is basically a tapered ½ circle. This is then a passive straight shaft (body) that is 1.5 times the length of the curved section.
Laparoscopic considerations: The followings considerations ought to be considered while endosuturing:
- Prevention of needle loss
- Secure grasping
- Ease of tissue penetration
When placing stitch, either for tissue plane or cut edge re-approximation, the inclusion or exclusion of particular tissue layers (Figure 2.6) plays an important role in the recovery process and restoration of normal physiology.
The entire process of acquiring the correct suture depth in endoscopic surgery is technically challenging and involves four variables:
- visualization
- eye-hand coordination
- the role from the assisting instrument in suturing
- judgment and tactile feedback
- Introduction and retrieval of the suture to the operative ?eld: For transfer back and forth from the operative ?eld, the suture is grasped through the assisting grasped through the assisting grasper some 2-3cm behind the needle. The needle should only be organised during suturing, otherwise it can be dangerous.
- Loading the needle within the needle driver: There's two processes for loading the needle. The option depends upon the precise conditions and also the proximity or otherwise of a smooth serosal surface:
- The deposit - pick-up technique
- The dangling pirouette technique
If adjustment of the needle is needed, this can be done in 3 ways:
- maintaining a light grip about the needle and pulling the thread taut so that angle from the needle is modified
- maintaining an easy grip and brushing the end from the needle gently from the close by tissues forward for backward within the 3 o’ clock direction
- reducing the grip from the needle and gently hooking it on super?cial ?bres of the serosal layer in an avascular area A popular but ineficient technique involves while using supporting the assisting instrument to reposition the angle from the needle.
Needle driving Principles
- Angle of approach and direction of the force: The end of the needle must approach tissue at right angles regardless of the configuration of the needle. The direction from the power apply with the needle driver should be perpendicular to the cut surface or tissue edge.
- Needle detection: Needle detection occurs when the needle is not pushed directly opposite to the plane of tissue resistance and the extent of de?ection is directly of the power in the perpendicular interface with the resistance provided by the tissue.
- Counter pressure in needle driving: The correct using counter pressure or counter traction expedites suturing.
- Technique of needle driving: The needle driver may be the dominant handed instrument and the assistant grasper is grasped.
- Needle positioning: A slowly driven needle passage results in a smoother and much more successful passage. The needle is driven having a delicate grip and also the direction from the pushing force is maintained directly against tissue resistance.
- Entrance bite: for that entrance bite, the needle tip should be ready that's perpendicular, or nearly so, towards the tissue surface. The motive force will be supinated rotating the needle clockwise, thereby pushing it down with the tissues and then forward and upwards penetrating appropriate tissue layers.
- Extracting the needle: two methods are usually used one, once the needle tip is grasped by the assisting instrument, when only the tip from the needle is shown. Second whenever a half circle needle is used, it's just extracted after extensive rotation and not along the horizontal plane.
- Exit bite: the needle ought to be pulled from the tissue surface only for ten or twenty yards enough make it possible for the maneuverability required for reloading needle within the driver.
Advancing the thread
Pulling on the needle is restricted towards the initial extraction of the suture, thereafter the needle is dropped and also the thread is pulled apart by grasping it using either the assisting instrument or using the active needle driver. The two handed pull entails the sequential use of the assisting grasper and active needle holder and is probably the most ef?cient method but requires experience and coordination.
Knot tying
The most important component for endosuturing is a needle holder. The need for ideal kind of laparoscopic suturing instruments to facilitate ?uent choreographed two handed movements essential for effective tissue approximation resulted in the introduction of Coaxial handles. A coaxial stem-to-handle relationship allows for the higher maneuverability and rotation essential for laparoscopic suturing. This straight line relationship reduces the complexity of movement coordination which makes it more ergonomic. A cylindrically shaped handle design permits a smooth 360 degrees rotation from the instrument. Another important feature which makes it possible for internal half knotting in areas of complicated access is for the finish of 1 of the needle drivers to be coaxially curved. The Szabo-Berci Needle driver sets and the Cuschieri needle sets utilizes this function.
STAPLERS IN LAPAROSCOPIC SUGERY
- Indications
- Gastrectomy.
- Gastric Bypass.
- Resection anastomosis.
- Splenectomy.
- Bilio-pancreatic diversion.
Requirements of Laparoscopic Surgery
- Maximum reach and versatility.
- Staple line security.
- Hemostasis.
- Thick tissue penetration.
- Precise staple formation
Kinds of Staplers used in laparoscopic Surgery There are two types of staplers utilized in laparoscopic surgery
- Linear staplers.
- Circular staplers.
Staplers in laparoscopic Surgery
Autosuture Endo GIA universal
- Can be used upto 25 times.
- Same gun may be used for all staple heights and cartridge sizes.
- XL size for obese patients
Options that come with Tyco Gun and Cartridge
- 2 triple staggered rows.
- Straight and articulating cartridges available.
- New knife for every application.
- Sizes : 2.0/2.5/3.5/4.8.
Ethicon Stapling Gun
- Can be fired upto 8 times.
- Different gun to be used for different length of cartridge.
- It could be a straight or an articulating stapler.
- The XL size should be use for obese patients
Echelon The innovation that resulted is a multiple-squeeze method for the cutting and stapling, which required careful focus on user feedback to really make it intuitive. Other improvements include increases in ef?ciency, intuitiveness and overall surgeon satisfaction.
Gold Cartridge
Has 6 rows of staples.
- Tissue penetration of compressible staple is 1.8mm.
- Used mainly on gastric tissue.
Recommendations for use in laparoscopic surgery
Grey - mesentery.
White - small gut.
Blue / Gold - stomach (except pylorus).
Green - pylorus / redo surgery.
Precautions
Avoid excessive use of gun.
- No excess tissue.
- Right cartridge.
- Under run when in doubt.
- Good vascularity.
Characteristics
- Single use
- Head tilt / straight head
- Double staple row
- Circular knife blade
Indications Gastrojejunostomy Colo-Rectal surgery
- Curved stapler very useful
- Preferred sizes 21mm and 25mm
- Safe and ensures optimum size stoma
Precautions
- When using stapling devices ensure you understand their assembly and performance.
- Careful preparation and meticulous setup from the anastomotic site is really as essential when stapling as when suturing.
- These instruments aren't intended for use wherever surgical stapling is contraindicated.
- Ensure that you choose the correct sized instrument for that task expected..






