Laparoscopic Endometriomas Surgery
Ovarian endometriosis causes the adhesions between the ovarian surface and the broad ligament. As the ovary enlarges, endometriomas form. Sometimes surface endometrial implants penetrate more deeply into the cyst wall, making excision more difficult. The degree of endometrial invasion of the cyst wall forms the basis for differentiating between these two subtypes and is characterized by the progressive difficulty in removing the cyst wall.
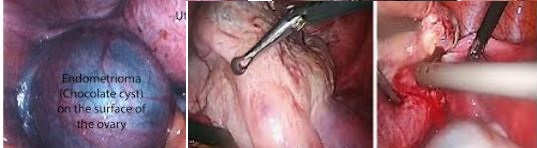
Ovarian Endometrioma
The least invasive and the technically simplest approach to endometriomas involve laparoscopic fenestration and removal of “chocolate” fluid without cystectomy or ablation of the cyst wall. However, fenestration and irrigation are associated with a 50 percent recurrence rate compared to 8 percent in the group with the capsule removed. Postoperatively, either danazol 800 mg/d or a GnRH analog is used for 6 to 8 weeks. Large hematomas are associated with periovarian adhesions attaching them to the pelvic sidewall and the back of the uterus and tend to rupture during separation. After mobilizing the ovary, the contents of the cyst are removed with the suction-irrigator probe and the cavity is irrigated.
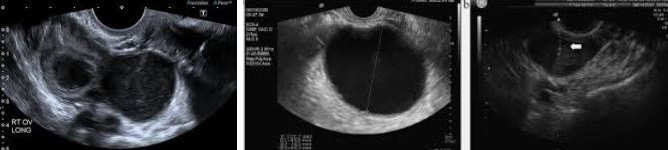
Ovarian Endometrioma
The inside of the cyst is evaluated and the portion of the ovarian cortex involved with endometriosis is removed. Using the grasping forceps and the suction-irrigator probe, the cyst wall is grasped and separated from the ovarian stroma by traction and counter traction. Small blood vessels from the ovarian bed and bleeding from the ovarian hilum can be controlled with bipolar electrocoagulation. The remaining ovarian tissue is approximated with low-power laser or electrosurgery to avoid adhesions. Low-power, continuous laser or bipolar coagulation applied to the inside wall of the redundant ovarian capsule causes it to invert, but excessive coagulation of the adjacent ovarian stroma must be avoided. Sutures, if needed, are placed inside the capsule and 4-0 polydioxanone sutures used. Fewer sutures result in fewer adhesions.
The ability to diagnose and treat endometriosis at earlier stages may prevent its progression and invasion, reducing its adverse impact on health, quality of life, and fertility potential.
Ovarian endometriosis causes the adhesions between the ovarian surface and the broad ligament. As the ovary enlarges, endometriomas form. Sometimes surface endometrial implants penetrate more deeply into the cyst wall, making excision more difficult. The degree of endometrial invasion of the cyst wall forms the basis for differentiating between these two subtypes and is characterized by the progressive difficulty in removing the cyst wall.

Ovarian Endometrioma
The least invasive and the technically simplest approach to endometriomas involve laparoscopic fenestration and removal of “chocolate” fluid without cystectomy or ablation of the cyst wall. However, fenestration and irrigation are associated with a 50 percent recurrence rate compared to 8 percent in the group with the capsule removed. Postoperatively, either danazol 800 mg/d or a GnRH analog is used for 6 to 8 weeks. Large hematomas are associated with periovarian adhesions attaching them to the pelvic sidewall and the back of the uterus and tend to rupture during separation. After mobilizing the ovary, the contents of the cyst are removed with the suction-irrigator probe and the cavity is irrigated.

Ovarian Endometrioma
The inside of the cyst is evaluated and the portion of the ovarian cortex involved with endometriosis is removed. Using the grasping forceps and the suction-irrigator probe, the cyst wall is grasped and separated from the ovarian stroma by traction and counter traction. Small blood vessels from the ovarian bed and bleeding from the ovarian hilum can be controlled with bipolar electrocoagulation. The remaining ovarian tissue is approximated with low-power laser or electrosurgery to avoid adhesions. Low-power, continuous laser or bipolar coagulation applied to the inside wall of the redundant ovarian capsule causes it to invert, but excessive coagulation of the adjacent ovarian stroma must be avoided. Sutures, if needed, are placed inside the capsule and 4-0 polydioxanone sutures used. Fewer sutures result in fewer adhesions.
The ability to diagnose and treat endometriosis at earlier stages may prevent its progression and invasion, reducing its adverse impact on health, quality of life, and fertility potential.






