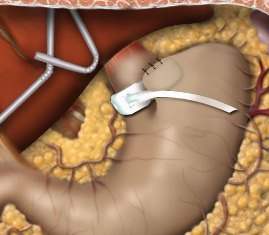
Laparoscopic Adjustable Gastric Banding for Morbid Obesity
Obesity was identified as a disease thirty years ago when, the WHO listed obesity like a disease symptom in its International Classification of Diseases in 1979. The prevalence of obesity, and particularly of morbid obesity, is increasing worldwide and it is today being a significant health risk. Indeed, obesity rates have now reached really dangerous levels in the western emisphere, with over 25 per cent from the population obesity in US and 15 percent in Europe. An identical pattern of increasing examples of overweight problems have been demonstrated within the pediatric population. Overweight children and adolescents have a higher risk of becoming obese adults.
Prevalence of obesity in India is up to 50% in women and 32.2% in men in the upper strata of the society2. In Delhi alone the prevalence of obesity stands at 33.4% in women and 21.3% in men. Co-morbidities commonly associated with obesity include diabetes, cardiovascular and respiratory disease, dyslipidemia, degenerative joint disease, stress incontinence, and various types of cancers amongst others. They are all accountable for a lower life expectancy as well as an impaired standard of living. Obesity bias and discrimination starts in the earliest social contacts, in preschool children and progresses through childhood and adolescence into adulthood. This prejudice may contribute to depression, eating disorders, and body image disturbance. The practical social implications of morbid obesity are manifold e.g. inability to ambulate, limited options in clothing, stress incontinence, and difficulty with personal hygiene. A direct consequence of the social bias is an economic disadvantage with decreased educational, job and promotion opportunities. There's also a direct relationship between increasing BMI and relative risk of dying prematurely. The Framingham data1 says for each pound gained between ages 30 to 42 years, there was a 1% increased mortality within 26 years, as well as for each pound gained thereafter, there is 2% increased mortality. In the morbidly obese population, the typical life expectancy is reduced by 9 years in females and 14 years in men.
BMI
Obesity generally is dependent upon calculating bmi (BMI), which measures weight for height and is stated in numbers. BMI is calculated by the weight in kilograms divided by height in meter square Obesity was further classified within the 1998 NIH Clinical Guidelines about the Identification, Evaluation, and Treatment of Overweight and Obesity in grown-ups 4 into:
MANAGEMENT OF MORBID OBESITY
Obesity demands long-term management. The goal of treatment is weight loss to enhance or eliminate related health problems, or even the risk for them, to not attain an ideal weight. Conservative therapy invariably does not achieve weight loss, or sustain the weight loss in morbidly obese patients. The patients gain back the lost weight very quickly. Therefore, surgery has been increasingly considered as the preferred option for these patients. Surgical treatment of morbid obesity has been established as being safe and effective. It is the best therapy available for the dangerously obese population. It markedly lowers body weight, reverses or ameliorates the myriads of obesity related co-morbidities and improves the quality of life. Since introduction of laparoscopic techniques in seo, the number of patients being referred for surgery continues to be on the rise.
Indications for surgery
Surgical therapy should be thought about for those who:
- Have an appearance mass index (BMI) equal to or more than 40 kg/ m2 Or
- Possessa BMI add up to or greater than 35 kg/ m2 with significant co- morbidities. And
- Prior dietary attempts at weight control happen to be ineffective.
High-risk co-morbid conditions that can justify surgery at a BMI to 35 kg/ m2 include diabetes type 2, life-threatening cardiopulmonary problems, obesity-induced physical problems interfering with an ordinary lifestyle, and body size problems precluding or severely interfering with employment, family functions, and ambulation.
Surgical options
The surgical options available for treating morbid obesity are:
- Restrictive:
- Vertical Banded Gastroplasty (VBG)
- Laparoscopic Adjustable Gastric Banding (LAGB)
Within the adjustable gastric band, the amount of restriction can be adjusted whilst in the vertical banded gastroplasty it remains fixed. The popularity of VBG has been decreasing because of the poor longterm weight loss and complications.
- Restrictive and Malabsorptive:
Roux en Y gastric bypass having a standard limb, long-limb or a very long-limb is really a procedure which has been used for the longest time with known long term results. The gastric bypass causes gastric restriction but additionally depends on varying amounts of intestinal malabsorption as an additional weight loss mechanism
- Malabsorptive:
Biliopancreatic diversion alone or with duodenal switch. Certain surgeons perform one operation exclusively; other surgeons offer the full-range of operations. It comes with an ever-increasing effort to complement a specific patient to a particular operation. To this end, several selection approaches or algorithms happen to be suggested, although randomized trials that test these algorithms haven't been conducted. Increasingly, hormonal changes are being named an important mechanism of post surgical weight loss; recent reports have demonstrated that gastric bypass results in altered release of hunger-causing hormones, such as ghrelin.
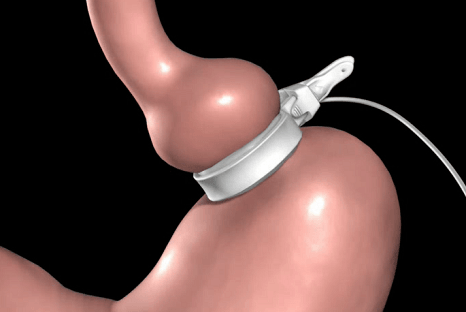
LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING
Patient Evaluation and Preparation
Operations should only be performed inside the setting of the obesity treatment program committed to maintaining long-term follow up for evaluation of outcomes. Careful preoperative evaluation and patient preparation are critical to success. Patients should have a clear understanding of expected benefits, risks, and long-term consequences of medical procedures. Surgeons have to know how you can diagnose and manage complications specific to bariatric surgery. Patients require lifelong follow-up with nutritional counseling and biochemical surveillance.
Surgeons also must understand the requirements of severely obese patients in terms of facilities, supplies, equipment and staff necessary to meet these needs, and should make sure that the specialized staff and/or multidisciplinary referral system is available for treating these patients. This multi-disciplinary approach includes medical management of co-morbidities, dietary instruction, exercise training, specialized nursing care and psychological assistance as needed with an individual basis. A practitioner familiar with relevant bariatric operations should direct post-operative management of the co-morbidities.
Contra-indiations for that procedure include:
- Mentally Retarded - not able to understand the guidelines of eating and use and for that reason not able to fulfill their part from the partnership
- Malignant hyperphagia - Prader Willi syndrome
- Portal hypertension
Pre-Operative Care:
A bariatric surgery patient needs to be well-informed, motivated, prepared to participate in the long term care, change dietary patterns, and embrace a revised lifestyle. The patient is best evaluated, and subsequently looked after with a team approach relating to the surgeon, a dedicated dietician, a nurse practitioner, and other specialists when needed.
And a preoperative history, physical, and laboratory evaluation, a preoperative discussion or teaching seminar providing you with information on postoperative recovery, dietary changes, activity, and clinical outcomes, by the dietician, the bariatric nurse, and also the bariatric surgeon, is crucial. Availability of a support group is recommended, as is distribution of literature describing procedures, postoperative diets, exercise etc. Accessibility to a complete spectrum of expert consultants is mandatory. Anti-thrombotic measures need to be in place. Graduated compression stockings may be placed on, eventually prior to surgery. Low molecular weight heparin shall have to be administered 24 to 48 hours just before surgery.
Anesthetic considerations:
Expert anesthesiology support, knowledgeable within the specific problems of the bariatric patient, is essential. The anesthesiology support includes an awareness of patient positioning, blood volume and cardiac output changes, airway maintenance, and drug pharmacokinetics in the morbidly obese. It is advisable to have preoperative, intraoperative, and postoperative written protocols. Airway access and intubations in obese patients are difficult. Blood pressure level monitoring takes a larger sized cuff. Venous access and maintenance requires expertise. Intra-operative pneumatic compression stockings need to be placed on both the lower limbs just before positioning from the patient is performed.
Surgical Technique
Patient position and Port Placements
The patient is place in a modified Lloyd Davies’ Position with the hands outstretched, along with a steep change Trendelenberg position around are usually necesary. An overall total of Five to six ports are utilized. There is significant variation within the placement of port placement between surgeons who otherwise do the operation within an almost identical fashion and who, at completing the operation, have the band in a similar position. A abdomen is inflated to 15 mm Hg by introducing a Veress needle, Alternatively visual access is gained with a 12-mm Excel port utilizing a 0° laparoscope. The peritoneal cavity is inspected and all subsequent ports are put under vision. This left subcostal (midclavicular) port shall be subsequently substituted for a 15 mm port for the introduction of the band into the peritoneal cavity.
A 10 mm trocar is introduced under guidance from the telescope at a hands’ width distance from the tip from the xiphoid process towards the umbilicus along with a thumbs spread left of the midline. This will be your camera port. Another 10 mm trocar is inserted within the right subcostal region for liver retractor. Two additional working 5-mm trocars are then placed; one out of the anterior axillary line about the left side for fundal retraction through the assistant and the other within the epigastrium for the left hand dissection from the surgeon and the articulating dissector to make a retgrogastric tunnel for that passage of the band.
Operative Technique
Belachew described the original technique for LAGB placement. Numerous modifications and variations have subsequently been proposed. The LAGB is created specifically for laparoscopic placement. Obviously, it may be placed by open technique also when occasionally this is needed, usually due to the presence of large, fragile liver or copious levels of intra abdominal fat. The degree of visibility, and therefore accuracy of placement and fixation are much greater with laparoscopic placement. Furthermore, you will find fewer peri-operative complications. The operation requires good laparoscopic skills and prior knowledge about advanced laparoscopic surgery.
The Pars Flaccida pathway for placing the band
The pars flaccida path has now become the recommended approach by most surgeons. This method has the benefits of easy dissection and reduce in the incidence of prolapse of the posterior wall from the stomach through the band which was a major flaw from the used perigastric technique. The dissection on the lesser curvature from the stomach includes the neurovascular bundle of the lesser omentum. The pars flaccida path requires minimal tissue dissection and therefore little probability of encountering bleeding. It is usually quick and safe. It is definitely defined, easily taught and places the band within the optimal alignment across the very top from the stomach. It almost never traverses the lesser sac and doesn't require posterior fixation. When the surgeon wishes to keep open selecting later conversion to gastric bypass, this method doesn't compromise subsequent dissection.
A potential disadvantage to the pars flaccida path is the chance of early postoperative obstruction to swallowing due to excess tissue within the band. The amount of fat included with the banded upper stomach is a lot more variable compared to the perigastric approach. With too much fat present, transit of fluid over the band is going to be excessively delayed or stopped in the early days postoperatively. Particular attention must be given to using the calibration tube and also the dissection of the lesser omental and perigastric fat to ensure the band is not too tight.
- Step one. Division of phreno-gastric ligament: By retracting the left liver lobe upward pulling downward on the gastric fundus by having an atraumatic grasper, a triangular area is exposed above the gastric fundus where the 3 sides in clockwise sequence are the diaphragm, the gastrosplenic ligament, and the esophagus. The phenro-gastric ligament in the heart of the triangle is divided utilizing a monopolar hook, thereby releasing the fundus in the diaphragm and exposing the angle of His, the left crus of the diaphragm and also the retrogastric pad of fat.
- Step 2. Exposure of the right crus: After freeing the gastric fundus, the dissection is now use the lesser omentum. A window is made within the lesser omentum with the hook at an avascular site. Continuing the division of the lesser omentum upwards, the right crus from the diaphragm is exposed by detaching the pars flacida. The anaesthetist is now requested introducing the gastric calibration tube and decompress the stomach. The balloon is stuffed with 15 ml of saline and the tube is withdrawn till a resistance is felt from the gastro-oesophageal junction. The retrogastric tunnel should be made in the center of the balloon for creating a small pouch. This point is noted, the balloon is deflated and also the tube is withdrawn to the oesophagus. The peritoneum just medial to the lower part of the right crus is incised in the point meant for placement of this guitar rock band using diathermy. The Goldfinger is introduced through this opening, curving its tip into the retrogastric fat tissue next to the left margin from the crus and directing it toward the exposed angle of His. The end of the goldfinger comes out left of the gastric fundus through the opening produced in the phrenogastric ligament.
At this time, the sterile SAGB is unwrapped on the back table, and sterile normal saline injected into its tubing with a 5 ml syringe, that is subsequently withdrawn till all of the air bubbles are removed. This process must be repeated a few times to make sure there isn't any air within the balloon. The connecting tube is clamped having a rubbershod mounted curved hemostat. A knot is tied on the tubing distal to the clamp to keep the vaccum. The Swedish band has a pre-tied Ethibond loop at its tip. The fully deflated balloon will be grasped with this loop with a 5mm grasper and it is introduced into the peritoneal cavity with the 15 mm left sub costal port. - Retro-gastric transit of the band: The pneumoperitoneum is reestablished. The ethibond loop in the tip of the band is snugged to the slit about the tip of the Goldfinger. The Goldfinger is gently pulled through its retro-gastric extraperitoneal path. The shoulder of the band sometimes appears coming out from behind the stomach, in the lesser curve. The balloon side from the band should face the stomach The tip of the band is eased out with the opening pulling this guitar rock band in position.
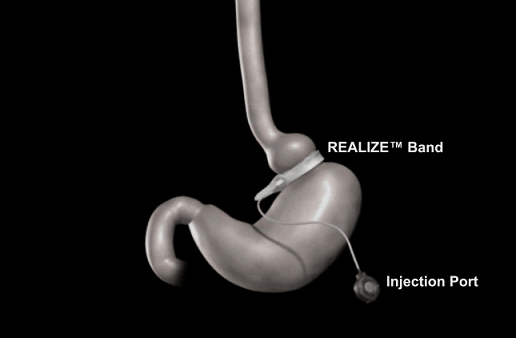
- 4. Gastric Band Tightening: Following the band continues to be placed in the retrograstric tunnel, the anesthetist is again requested to push the gastric calibration tube into the stomach, inflate the balloon and pull it back till the balloon comes to the GE junction. The band-end tags are locked forming the pouch above the band. The buckle is glided onto the lesser curvature from the stomach and also the band can be seen secured at 450 in the lesser curve towards the fundus of the stomach. Interrupted anterior gasro-gastric sutures are taken with 2-0 Ethibond to pay for the band anteriorly, starting near to the greater curve. Two or three gastro-gastric sutures are required to cover the band. The buckle from the band at the lesser curve must do not be engrossed in gastrogastric sutures, because this may initiate gastric erosion through the and. The connecting tube is then exteriorized through the subxiphoid port.
The particular siting from the band at the top of the stomach is the most critical facet of the process. If it is too low, it causes problems. If the band is simply too high, it doesn't work correctly and could cause achalasia like symptoms. One must keep in mind that the LAGB is a gastric band, no esophageal band. The most crucial mechanism of their action is as simple as inducing a sense of satiety. Even when patients haven't eaten, they do not feel hungry. Patients can miss a meal or eat late and not have the perpetual concentrate on food they have had for a long time. This effect allows eating three or less meals daily. Once they do eat, the 2nd mechanism of action comes into play, specifically, a sense of rapidly achieved fullness. The sense of satiety is probably mediated by the vagal afferent receptors within the apex of the gastric cardia. The band needs to overlay this area to generate this response. The particular posterior facet of this guitar rock band is almost certainly around the distal esophagus since it runs along the type of the left crus. The anterior aspect therefore needs to be set within the upper stomach to offer the satiety-inducing effect. There must be correct keeping the gastrogastric sutures as a part of the anterior fixation.
The particular calibration tube has two important functions; defining the road of the esophago-gastric junction and enabling a check that the band isn't too tight after closure. Additionally, it can be helpful as an aspiration tube to empty the stomach of gas at the commencement from the operation. After closure from the band along with the calibration tube in position, you should make sure that this guitar rock band can rotate freely and that a grasper could be handed underneath the band without difficulty. If not, much more fat ought to be removed from the anterior top of the stomach. - Keeping Injecting Port (IP): The access port should be positioned on the anterior rectus sheath just below the sternum. A 5 cm transverse incision is created and the rectus sheath is exposed by dividing the fat. A pouch is made for the placement of the port. Prolene sutures are passed through the holes in the ports after which through the rectus sheath and held in artery forceps. The connecting tube is mounted on the port and locked in position. The IP will be squeezed to the presternal space with its flat bottom facing the sternum and pushed into position. The prolene sutures are tied to anchor the main harbour towards the rectus sheath. The 10mm and 15 mm port sheaths have to be closed with vicryl suture using wound closure needle. Following complete reversal of pneumo peritoneum and careful removal of all ports, the skin is sutured with subcuticular sutures. A Mobilization from the patient begins immediately, i.e. a couple of hours after surgery. Oral intake begins in the evening following the surgery and quickly increased to 1000 ml on the second day, 1500 about the 3rd day and two liters thereafter. The individual is normally discharged the day following the procedure Outpatient adjustment from the band under fluoroscopy is then employed for experienceing this optimal tightness.
Complications
- Perioperative: Probably the most appealing individual feature of the LAGB is actually its safety. It's proved to be one of the most secure with surgical treatments, being 7 - 10 times safer compared to Roux-en- Y gastric bypass in terms of mortality with an over-all perioperative problem rate of 1 - 2%. The ASERNIP-S systemic review of the published literature identified an occurrence of perioperative problems of 2.6%, to be in contrast to 29.9% for Vertical Banded Gastroplasty and 23.4% for RYGB23. Surgical mortality for laparoscopic adjustable gastric banding when performed by experienced surgeons is about 0.1%. Operative morbidity is all about 5%.
- Late complications: Late complications have been regular but they are proving to become avoidable with enhanced technique. Prolapse of the stomach with the band might occur. The particular clinical options that come with prolapse are those of obstruction in the higher abdomen. There's heartburn, reflux of fluid to the mouth and also airway, vomiting after eating, coughing as well as choking spells along with wheezing. A limited barium swallow is the greatest investigation to define the issue. Uncommonly, the prolapse becomes large along with tense, leading to upper abdominal pain, tenderness and also the need for emergent exploration to rule out gastric necrosis. Prolapse of the posterior wall of the stomach through the band, the central problem from the perigastric approach, is managed by laparoscopic elimination of the band and site of the new band along the pars flaccida pathway. This process has been proven as safe and effective since it allows the patients to continue on with their progressive weight reduction. Adherence to the correct technique of pars flaccida pathway has virtually eliminated posterior prolapse.
Anterior prolapse happens equally within the pars flaccid along with perigastric approaches and indicates some failure of anterior fixation. When the prolapsed segment isn't excessively edematous or hypertrophied, it can generally be managed by mobilization, reduction of the prolapsed and refixation. On occassions, removal and replacement is required.
Erosion from the band into the abdomen is reported in 3.2% of subjects but with the newer higher quantity low stress bands, this issue should be controlled to some large extent. Erosion occurs when the band is stuffed too rapidly or if the anterior wrap of gastric wall covers part of, or even the entire buckle of the band. Avoidance of sutures in this region has resulted in virtual disappearance of the problem.
Post Operative Outcomes
Weight reduction
Research of weight loss in bariatric surgery will generally convey the outcome within the terms of proportion of excess fat lost, as change in body mass index or as absolute weight loss in kilograms or pounds. The load loss occurs more slowly than is generally seen after gastric bypass or bilio-pancreatic diversion. After the initial placement, there is a gentle, progressive weight reduction controlled by steady increments of saline added to the machine. Once a new stable point regarding weight has been reached, the weight loss could be maintained and also the recidivism of gastric bypass avoided by further small additions involving saline. The maximum weight loss is reported to occur in 3 or 4 years, instead of one or two years. Current data indicate that when the most weight reduction is achieved, the weight remains stable up to a minimum of 6 years. These functions reflect the advantage of adjustability.
Improvement in Co-morbidities:
There is no more powerful treatment in health care compared to weight loss in the obese. Numerous diseases are enhanced or solved completely and also the risk associated with illness is considerably reduced.
- Diabetes type 2 and insulin resistance: Diabetes type 2 is the paradigm of an obesity associated condition. Generally it exists due to the obesity and will disappear along with weight reduction. Remission of diabetes was predicted by a greater weight reduction and a smaller history of diabetes (p<0.001). Improvement in diabetes was related to increased insulin sensitivity and improved beta cell function. In association with weight loss there were also substantial improvements in the fasting triglyceride and HDL-cholesterol levels, hypertension, sleep, depression, appearance evaluation and medical quality of life. Four factors were found to significantly predict remission: greater percentage of excess fat lost at 1-year, a diagnosis of diabetes at its early stage, better preoperative beta-cell function and lower pre-operative fasting plasma glucose level. The last two factors were not significant after controlling for the time with a diagnosis of diabetes. The two remaining factors had significant independent effects, with the percentage of EWL being positively associated with remission, and length of time with a diagnosis of diabetes being negatively associated with remission.
These types of studies help to make numerous important points. First, weight loss is strongly beneficial for the kind 2 diabetic. Secondly, the more weight lost, the better the end result. Third, earlier treatment in the newly diagnosed obese diabetic is important. A better resolution of diabetic issues is accomplished when weight reduction takes place just before pancreatic experiment with cell perform is reduced. Fourth, weight reduction is associated with measurable improvements of insulin resistance as well as pancreatic beta cell function, thereby reversing both key pathogenic features of type 2 diabetes. Weight loss also offers an excellent and durable effect on the fasting plama glucose and also serum levels of insulin within the non-diabetics having a marked decrease in the blood sugar, HbA1c and plasma insulin on the 5-year period. - Hypertension: Hypertension is another ailment that is strongly but not totally powered by weight problems. The prevalence of hypertension in our overall patient team was 33%. The city norm27 for age and sex matched controls is 14.6%, confirming the increased risk of the disease in association with severe obesity.
- Dyslipidemia: Dyslipidemia is an important comorbidity of obesity associated with a high incidence of coronary as well as vascular events. The alterations in dyslipidemia in 515 severely obese patients have been studied before and up to four years after Lap-Band® placement Favorable changes in fasting triglycerides (TG), HDL-cholesterol (HDL-C) and total cholesterol (TC): HDL-C ratio were seen at 1-year and there were more improvements in HDL-C and TC: HDL-C ratio in the second year. All improvements were maintained out to 4 years when body mass index and weight were stable. Male gender, central obesity, elevated fasting glucose and insulin resistance were found to be related to less favorable lipid levels. TC and LDL-cholesterol did not correlate with measures of body shape or glucose metabolism. Dyslipidemia of obesity is related to weight distribution, insulin sensitivity and impaired glucose tolerance. Improvement with weight reduction is related to the fall in fasting glucose, improvement in insulin sensitivity and extent of weight lost. Improvement in dyslipidemia is sustained with long-term weight loss.
- Asthma: The prevalence of asthma in obesity and also the results of weight loss on asthma were studied in a group of patients undergoing Lap-Band placement. A consecutive sample of 32 asthmatic patients were followed clinically through a typical questionnaire for at least 12 months after surgery and any change in asthma was recorded. The prevalence of doctor-diagnosed asthma was 24.6% (73 of 296 consecutive patients). The 32 patients who were followed had a mean body weight of 125.2 kg (BMI = 45.7 kg/m2) prior to operation and a weight of 89.3 kg (BMI = 32.9 kg/m2) at follow-up. All 32 patients had a major clinical improvement in their asthma and the asthma severity score was reduced. There were significant improvements in all aspects of asthma, including severity, daily impact, medications, hospitalization, sleep and exercise. During the year preceding LAGB/ SAGB placement, 9 of these 32 patients had one or more admissions to hospital for acute asthma. No admissions were required during the 12 months follow-up. Mechanisms other than direct weight loss appear to play a part in this improvement, such as prevention of gastro-esophageal reflux.
- Gastroesophageal Reflux Disease: Gastro-esophageal reflux is a common problem with an estimated prevalence in the community of around 20%, of whom approximately 7% require daily medication. Obesity is regarded as an important contributing factor to the pathophysiology of gastro esophageal reflux, with prevalence between 37% and 72% in obese patients. Resolution or improvement was reported to have occurred soon after surgery and before substantial weight loss. These results contrast sharply with those of Ovrebow and Westling where gastric banding was implicated as a cause of gastroesophageal reflux. It is possible that the presence of prolapse of the stomach through the band in their patients could account for the disparate results. Prolapse creates a mechanically disadvantageous situation in which each additional bolus of food further distorts the path of emptying across the band and obstruction supervenes. Patients often present with symptoms of heartburn as an early feature of prolapse. This heartburn is probably generated by the stasis of food in the lower esophagus and not associated with acid. It does not generally respond to acid inhibition. Excessive tightening of the band also can lead to heartburn and reflux. This problem is easily corrected by establishing a more appropriate adjustment level.
- Sleep-disordered breathing: Sleep disordered breathing (SDB), particularly in the form of obstructive sleep apnea (OSA) occurs in approximately 4% of men and 2% of women in the general population. Obesity, especially upper body obesity, is considered a major risk factor for OSA and clinical assessments and sleep studies indicate a prevalence of OSA in morbid obesity (i.e. BMI > 40) to be 42-48% in men and 8-38% in women. The sleep quality score changed markedly. Prior to surgery, 29% had poor quality sleep and 28% had top quality sleep. These scores changed to 2% and 76% respectively at twelve months after operation.
- Depression: The twenty-one term Beck Depression Inventory has been utilized like a way of measuring the characteristic attitudes and symptoms of depressive illness in severely obese subjects presenting for Lap-Band placement. The BDI has been utilized for over 40 years as a way of measuring the characteristic attitudes and symptoms of depression. It has been validated and utilized in different ethnic groups, in subjects with co-existent medical conditions and in obese subjects. Fall in BDI score correlated with improvement to look at evaluation. This study indicated that severely obese subjects, especially young women with a poor body image, are in high risk of depression. There is sustained improvement with weight loss. These bits of information offer the hypothesis that depression is really a significant comorbidity of severe obesity.
- Alternation in Quality of life: Severe overweight problems have a major impact on patients physical, mental, psychosocial and economic health. In the perspective of many patients, the improvement in standard of living could well be the most crucial outcome to become achieved from a weight reducing procedure. The preoperative scores were all markedly lower than the community normal values for all eight domains and all had lower scores compared to those in the community with severe medical conditions. All scores improved significantly after SAGB/LAGB and remained much like community normal values to 4 years after operation. Of the both mental and physical component summary scores, the preoperative impairment was greatest in the physical component summary score and improved probably the most with weight reduction.
FUTURE CHALLENGES
Although the existing data show the procedure of adjustable gastric banding safe, effective and gentle, still remains to become established whether it will make a direct effect about the current epidemic of obesity. There are three challenges that must definitely be overcome to achieve this. Firstly, we want enough surgeons with good laparoscopic skills. The workload is immense and optimal results will not occur with suboptimal technique. Second, we must have in place something for good patient support and care to undertake the assessments and advice before operation and, most of all, to provide the ongoing care, with adjustments and support, permanently after operation. Third, we must still measure and also to learn. The perfect techniques for SAGB/LAGB and patient care after placements continue to be evolving. The sooner we are able to identify these and incorporate them into our clinical practice, the greater the SAGB/LAGB is going to be broadly accepted and also the more the benefits of weight reduction will be achieved over the community.






