Video of PPH Stapler. To download video right click here and save target
Hemorrhoids (PILES)
What are hemorrhoids?
Stapled anopexy/haemorrhoidectomy (SH) was introduced in 1993 and first described by Longo in 1998. A hemorrhoids can be described as masses or clumps ("cushions") of tissue within the anal canal that contain blood vessels and the surrounding, supporting tissue made up of muscle and elastic fibers. The anal canal is the last four centimeters through which stool passes as it goes from the rectum to the outside world. The anus is the opening of the anal canal to the outside world. Although most people think hemorrhoids are abnormal, they are present in everyone. It is only when the hemorrhoidal cushions enlarge that hemorrhoids can cause problems and be considered abnormal or a disease.
Prevalence of hemorrhoids
Although hemorrhoids occur in everyone, they become large and cause problems in only 4% of the general population. Hemorrhoids that cause problems are found equally in men and women, and their prevalence peaks between 45 and 65 years of age.
What is stapled hemorrhoidectomy?
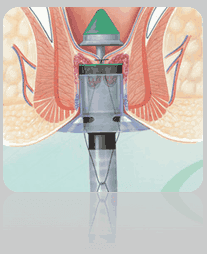
It is relatively new surgical technique for treating hemorrhoids, and it has rapidly become one of the treatment of choice for third-degree hemorrhoids. Stapled hemorrhoidectomy is a misnomer since the surgery does not remove the hemorrhoids but, rather, the abnormally lax and expanded hemorrhoidal supporting tissue that has allowed the hemorrhoids to prolapse downward. Once the blood supply of hemorrhoidal tissue is cut off it is cured and the prolapsed mucosa will be pulled up.
For stapled hemorrhoidectomy, a circular, hollow tube is inserted into the anal canal. Through this tube, a suture a long thread is introduced, actually woven, circumferentially within the anal canal above the internal hemorrhoids just like a purse string. The ends of the suture are brought out of the anus through the hollow tube called as anoscope. The stapler which is made by ethicon company is a disposable instrument with a circular stapling device at the end. This is also called as PPH stapler. PPH stands for procedure for prolapse and hemorrhoid.
Stapler is placed through the first hollow tube and the ends of the suture are pulled. Pulling the suture pulls the expanded hemorrhoidal supporting tissue as purse string into the jaws of the stapler. The hemorrhoidal cushions are pulled back up into their normal position within the anal canal. The stapler then is fired. When it fires, the stapler cuts off the circumferential ring of expanded hemorrhoidal tissue trapped within the stapler and at the same time staples together the upper and lower edges of the cut tissue. After firing the staple it should be kept pressed for one minute to stop capillary bleeding.
Stapled hemorrhoidectomy, although it can be used to treat second degree hemorrhoids, usually is reserved for higher grades of hemorrhoids - third and fourth degree. If in addition to internal hemorrhoids there are small external hemorrhoids that are causing a problem, the external hemorrhoids may become less problematic after the stapled hemorrhoidectomy. Another alternative is to do a stapled hemorrhoidectomy and a simple excision of the external hemorrhoids. If the external hemorrhoids are large, a standard surgical hemorrhoidectomy may need to be done to remove both the internal and external hemorrhoids.
During stapled hemorrhoidectomy, the arterial blood vessels that travel within the expanded hemorrhoidal tissue and feed the hemorrhoidal vessels are cut, thereby reducing the blood flow to the hemorrhoidal vessels and reducing the size of the hemorrhoids. During the healing of the cut tissues around the staples, scar tissue forms, and this scar tissue anchors the hemorrhoidal cushions in their normal position higher in the anal canal. The staples are needed only until the tissue heals. They then fall off and pass in the stool unnoticed after several weeks. Stapled hemorrhoidectomy is designed primarily to treat internal hemorrhoids, but if external hemorrhoids are present, they may be reduced as well.
Stapled hemorrhoidectomy is faster than traditional hemorrhoidectomy, taking approximately 30 minutes to perform the surgery in experienced hand. It is associated with much less pain than traditional hemorrhoidectomy and patients usually return earlier to work. Patients often sense a fullness or pressure within the rectum as if they need to defecate, but this usually resolves within several days. The risks of stapled hemorrhoidectomy include bleeding if the purse string suture is properly not made, infection, anal fissuring tearing of the lining of the anal canal, narrowing or stricture of the anal or rectal wall due to scarring, persistence of internal or external hemorrhoids, and, rarely, trauma to the rectal wall.
Stapled hemorrhoidectomy may be used in cases of second and third degree of hemorrhoid to treat patients who have both internal and external hemorrhoids; however, it also is an option to combine a stapled hemorrhoidectomy to treat the internal hemorrhoids and a simple resection of the external hemorrhoids.
Complications after stapled hemorrhoidectomy?
Interestingly, in one study done for stapler hemorrhoidectomy, 65% of complications occurred after the surgeon had done 25 or more cases, suggesting that the learning curve phenomenon does not apply. Septic complications in this study, and others, have been very rare. Bacteraemia after haemorrhoidectomy is more common with stapled hemorrhoidectomy rather than after conventional hemorrhoidectomy, but this does not seem to have clinical relevance.
Conclusion:
Stapled hemorrhoidectomy is at least as good as conventional haemorrhoidectomy and is less painful. Some have been skeptical about this surgery. But if it is performed by skilled minimal access surgery the SH is less painful, it was not associated with an earlier return to work than CH, and it failed to deal with external haemorrhoids.
Hemorrhoids at a Glance
- Internal hemorrhoids are clumps of tissue within the anal canal that contain blood vessels, muscle, and elastic fibers. External hemorrhoids are enlarged blood vessels surrounding the anus.
- Internal hemorrhoids cause problems when they enlarge. The cause of the enlargement is not known.
- Complications of internal hemorrhoids include bleeding, anal itchiness, prolapse, incarceration, and gangrene. Pain is not common.
- The primary complication of external hemorrhoids is pain due to blood clotting in the hemorrhoidal blood vessels.
- When dealing with hemorrhoids, it is important to exclude other diseases of the anus and rectum that may cause similar symptoms such as polyps, cancer, and diseases of the skin.
- Treatment of hemorrhoids includes over-the-counter topical medications, sclerotherapy, rubber band ligation, heat coagulation, cryotherapy, anal dilation, Doppler ligation, sphincterotomy, and surgical hemorrhoidectomy.
- The newest treatment for hemorrhoids is stapled hemorrhoidectomy.






