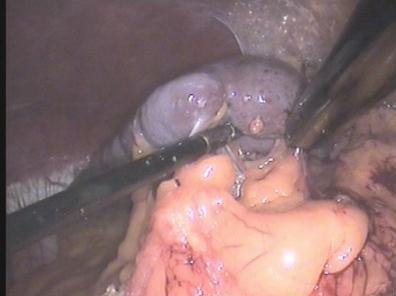
Introduction
The spleen, similar in structure to a large lymph node, acts as a blood filter. Current knowledge of its purpose includes the removal of old red blood cells and platelets, and the detection and fight against certain bacteria. It is also known to function as a site for the development of new red blood cells from their hematopoietic stem cell precursors, and particularly in situations in which the bone marrow, the normal site for this process, has been compromised by a disorder such as leukemia. The spleen is enlarged in a variety of conditions such as malaria, mononucleosis and most commonly in "cancers" of the lymphatics, such as lymphomas or leukemia.
It is removed under the following circumstances:
- When it becomes very large such that it becomes destructive to platelets/red cells
- For diagnosing certain lymphomas
- Certain cases of wandering spleen
- When platelets are destroyed in the spleen as a result of an auto-immune process (see also idiopathic thrombocytopenic purpura)
- When the spleen bleeds following physical trauma
- Following spontaneous rupture
- For long-term treatment of congenital erythropoietic porphyria (CEP) if severe hemolytic anemia develops
- The spread of gastric cancer to splenic tissue
- When using the splenic artery for kidney revascularisation in renovascular hypertension.
The spleen, originally called the "organum plenum mysterii" by Galen, has long been an important organ for surgeons. Traditionally, surgical removal of the spleen was done by an open approach using either an upper midline or left subcostal incision. With the advent of minimally invasive techniques, laparoscopic splenectomy has become a standard procedure for elective removal of the spleen for most indications. However, several technical challenges remain related to removing this fragile, well-vascularized organ that lie close to the stomach, colon, pancreas, and kidney.
Indications
Indications for laparoscopic splenectomy are the same for open splenectomy except when emergent splenectomy and exploratory laparotomy for traumatic injuries are needed. Laparoscopic splenectomy is indicated for various benign hematologic diseases, malignant hematologic diseases, secondary hypersplenism, and other anatomical disorders of the spleen.
- Laparoscopic splenectomy for malignant diseases of the spleen can be used for diagnostic or therapeutic reasons. Indications include myeloproliferative disorders, lymphoproliferative diseases, hairy cell leukemia, Hodgkin and non-Hodgkin lymphoma, malignant vascular tumors, malignant lymphomas, and lymphangiosarcomas.
- The most common benign hematologic disease treated with laparoscopic splenectomy is immune thrombocytopenia purpura, and it is recommended when medical therapy, including steroids and intravenous gammaglobulin, fail or long-term steroids are needed. Laparoscopic splenectomy can also be warranted in other benign conditions, including other types of thrombotic purpura, hereditary spherocytosis, major and intermediate thalassemia with secondary hypersplenism or severe anemia, sickle cell disease, and refractory autoimmune hemolytic anemia.
- Although the use of laparoscopic splenectomy in trauma has been reported, its role is limited because most hemodynamically stable patients with splenic injuries are successfully treated non-operatively, and unstable patients require emergent laparotomy for control of hemorrhage and to evaluate possible associated traumatic injuries.
Contraindications
Contraindications to laparoscopic splenectomy are similar to contraindications for all laparoscopic surgeries.
- Although reports on the safety of laparoscopic splenectomy in patients with cirrhosis and portal hypertension have been published, many consider this an absolute contraindication to laparoscopic splenectomy.
- Contraindications include the inability to tolerate general anesthesia, uncontrollable coagulopathy, and the need for laparotomy for associated procedures.
- Massive splenomegaly is a relative contraindication; however, the hand-assist technique may facilitate removal of large spleens in a minimally invasive fashion.
What are the side effects of Splenectomy?
Spleen-Removal Side Effects: Lung Collapse:
The spleen is situated within very close proximity to the lung around the left side of the abdomen. Lake Norman Surgical Associates of Pennsylvania explains that you have a chance of lung collapse after spleen removal surgery along with an increased likelihood of fluid inside the lungs and pneumonia. Lung collapse is treatable with physical and respiratory therapy. Chest infection and pneumonia are often treated in conjunction with antibiotic therapy.
Spleen-Removal Side Effects: Thrombocytosis:
Thrombocytosis is often a condition that typically occurs after spleen-removal surgery. In the book "Platelets in Thrombotic and Non-Thrombotic Disorders: Pathophysiology," author Paolo Gresele explains that the spleen holds approximately one-third in the blood platelets which can be in the human body. So, it isn't surprising that the removal of the spleen would prompt a boost in blood-platelet circulation during the entire body. However, the lab most current listings for some patients which have had their spleens removed show an elevated platelet level in excess of 1 / 2. The thrombocytosis condition can persist for upward of a fortnight, enhancing the patient's chance of life-threatening thrombus.
Spleen-Removal Unwanted side effects: Excessive Bleeding:
Blood loss is really a complication and major complication of spleen-removal surgery. An enlarged spleen that is overfilled with red blood cells poses a risk of rupture. If the rupture happens before surgery, the effect could be life-threatening. In these situations, an emergency splenectomy is warranted. But may the spleen can rupture during surgery, causing severe hemorrhage and hemorrhage. For that reason, laparoscopic surgery has taken the area of open spleen-removal surgery anytime you can. In the book "Complications in Surgery and Trauma," author Stephen M. Cohen explains that patients that undergo a spleen removal that is performed laparoscopically experience significantly less hemorrhage compared to those patients who undergo open splenectomies. Laparoscopic spleen removal also needs a shorter a hospital stay.






