Introduction
Prostate cancer is one of the most common newly diagnosed cancer in men. Although the incidence rates and mortality rates associated with prostate cancer have shown an overall declining trend, widespread screening and early diagnosis makes the management of clinically localized prostate cancer an ongoing challenge. After the popularization of the technique of anatomic nerve-sparing radical prostatectomy, open radical prostate surgery became a more desirable treatment for organ-confined prostate cancer.
The laparoscopic approach gained new attention when two French groups published their experience with laparoscopic radical prostatectomy in 1999 and 2000. They reported modifications to the original technique, resulting in operative times that ranged from 4-5 hours and a mean blood loss of 402 ml. Even in the hands of these skilled laparoscopists, nerve-sparing dissection and construction of the urethravesical anastomosis were demanding. With advances in medical technology, improved optics, and the widespread use of new laparoscopic instrumentation such as ultrasonic cutting and coagulating devices (e.g., Harmonic scalpel; Ethicon Endo-Surgery, Inc; Cincinnati, Ohio), laparoscopic radical prostatectomy began to gain acceptance and was performed increasingly in several high-volume centers worldwide. However, the technical demands of laparoscopic radical prostatectomy prevented its widespread use by the average urologist and thus limited penetration.
The next significant advancement in the surgical treatment of localized prostate cancer was the development of robotic surgical technology. Initially developed by the United States Department of Defense for use in military battlefield applications, robotic technology was adapted for civilian use through the entrepreneurial efforts of two rival corporations, Intuitive Surgical, Inc, and Computer Motion, Inc. These companies simultaneously developed robotic interfaces for use in human surgical applications. Computer Motion, Inc. introduced the Zeus Surgical System at approximately the same time that Intuitive Surgical, Inc, developed its da Vinci Surgical System.
Surgical Techniques
The basic technique for performing minimally invasive radical prostatectomy is the same regardless of the technology used. Candidates for this approach include patients in whom the diagnosis and staging support organ-confined prostate cancer and in whom the appropriate metastatic workup results are negative. The goal of minimally invasive radical prostatectomy is to laparoscopically resect the prostate and its capsule, along with the seminal vesicles. The procedure can be performed extraperitoneally or, more commonly, trans-peritoneally. The two most reported techniques for performing minimally invasive radical prostatectomy are robotic (robotic radical prostatectomy) and laparoscopic (laparoscopic radical prostatectomy).
Laparoscopic radical prostatectomy
The laparoscopic approach involves 2-dimensional monitors and conventional laparoscopic instruments (5 or 10 mm) with a 10-mm 0° and/or 30° telescope. The camera may be operated by a one-armed camera holder or by an assistant. The use of a single voice-operated robotic arm has also been described as an adjunct to the laparoscopic approach. A camera-holding device provides stability and prevents camera shake that can result from holding it by hand (i.e., by an assistant).
Robotic radical prostatectomy
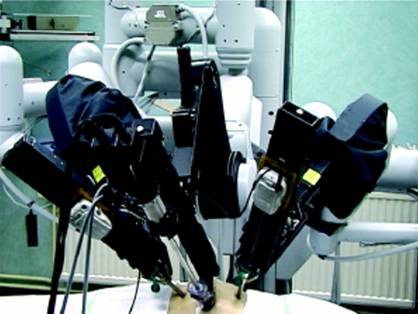
Currently, the only available integrated robotic surgical system is the da Vinci Surgical System (Intuitive Surgical, Inc; Sunnyvale, California). This computer-aided system has a basic master-slave design. A second generation of this system is currently available (da Vinci S HD System). The basic design is as follows:
- Surgeon console: This is the user interface of the robot for the surgeon. It consists of the following:
- Display system: The system is a 3-dimensional stereoscopic display for the console surgeon and is generally available for view in 2-dimensional form by assistants and observers.
- Master arms: These are the controls the surgeon uses for making surgical movements. Movements of the master arms translate to real-time movements of the instrument tips and may be scaled for fine movements. The master arms also provide basic force feedback to the surgeon but are limited in their ability to discriminate complex hepatic feedback. Camera movements are controlled with a clutch mechanism. In the 4-arm systems, the surgeon can toggle between instruments.
- Control panel: The control panel is used to adjust the surgeon console display and control options. The control panel allows toggling between 2- and 3-dimensional display, adjusting various levels of scaling, and choosing the camera perspectives (0° vs. 30° lens).
- Central processing unit: This is the computer that controls the system and integrates and translates robot control inputs from the surgeon.
- Robotic arms: Two or 3 arms are provided for mounting surgical instruments and one camera arm is provided for camera manipulation. The robotic arms are mounted on a surgical cart that is sterilely draped and moved into position over the patient. The arms are then mounted to 8-mm trocars placed through the patient's abdominal wall. The surgeon console is connected to the surgical cart via cables. Although the surgeon console and the surgical cart are typically in close proximity in the operating room, a longer interface has the potential to be used for long-distance surgery or telementoring.
Surgical Approaches
Patient Preparation and Positioning for Minimally Invasive Radical Prostatectomy
Once the patient is confirmed as an appropriate candidate for a complex laparoscopic procedure, to minimize complications and to facilitate operative success he must undergo an appropriate preoperative preparation. The primary routine consists of an extended office visit with the patient to explain the risks, benefits, and potential alternatives of the procedure.
The priorities of the procedure are also emphasized, including patient safety, preservation of the oncologic integrity of the surgical procedure, and an attempt at performing the procedure laparoscopically. The risk of conversion to an open procedure is explained thoroughly in the framework of this group of priorities. Specifically, if the patient’s safety or the oncologic integrity of the operation is jeopardized, the attending surgeon may decide to convert the procedure to the open surgical technique.
The preoperative and pre-anesthesia screening to determine suitability for a complex laparoscopic procedure is identical to that performed prior to open surgery. The authors generally perform a preoperative bowel preparation, including both antibiotic and mechanical bowel cleansing. This not only reduces bowel distention and adds visualization but also reduces the potential for infection due to the spillage of bowel contents in the uncommon event of a bowel perforation. On the day of surgery, a preoperative enema is performed, sequential compression stockings are placed, and a large-bore intravenous line is begun with preoperative antibiotics that cover both genitourinary and skin flora.
Regardless of the technique used, the patient is placed in the supine position with his head down. This head-down position allows for gravity to facilitate the natural retraction of the pelvic tissues. If the procedure is to be performed trans-peritoneally, a periumbilical incision is made to provide access for the initial laparoscopic port. A Veress needle or Hasson-type trocar is used to establish pneumoperitoneum and to facilitate the laparoscopic survey of the abdomen. The Veress needle is an ideal access device when the patient has no history of abdominal surgery. In patients who have undergone previous abdominal surgery, particularly involving infra-umbilical incisions, the Hassan trocar is ideal for direct visualization and confirmation of entrance into the peritoneal cavity.
Carbon dioxide is then insufflated into the abdomen to achieve pneumoperitoneum. If a Veress needle was used for initial access, it is replaced by a 12-mm radially dilating laparoscopic trocar. The 3-dimensional robotic laparoscope is then inserted through the infra-umbilical trocar site, and a laparoscopic survey of the abdomen and pelvis is performed. If the procedure is to be performed extra-peritoneally, the first steps for access consist of a small incision and development of the extra-peritoneal space.
Robotic Trans-peritoneal Approach
In this technique, the dissection proceeds in an ante grade manner and releases the prostate from the bladder neck early in the procedure, allowing the prostate to be manipulated with traction to aid in visualization for nerve sparing. The seminal vesicles and all subsequent dissection proceed in the direction of telescope vision (i.e., ante grade), facilitating visualization.
The patient is placed in the supine position, secured to the table, and placed in steep Trendelenburg position (45°). The legs can be placed in stirrups or positioned apart. The robot is then brought between the patient’s feet.
The total number of ports and port configurations depends on several factors. Three-armed robots have a total of 6 ports in an inverted V-shaped configuration. The Veress needle is used to establish the pneumoperitoneum, and a 12-mm port is placed just to the left of the umbilicus (camera port). A 30° upward-looking lens is then used to place the remaining ports; two 8-mm ports are placed as mirror images of each other, 10-12 cm from the camera port and 2 fingerbreadths below it. The ideal port position is approximately 15 cm above the pubic symphysis to afford the instrument adequate length of excursion.
Two ports are placed in the right lower quadrant—(1) a lateral 10-mm port just above the right anterior superior iliac spine for retraction and passage of sutures and (2) a medial 5-mm port for suction and irrigation midway and slightly inferior to the umbilicus and right robotic port. Finally, a 5-mm left lateral port is placed as a mirror image of its right-sided counterpart. Initially, this procedure called for two bedside assistants, but the evolution and application of the fourth robotic arm eliminated the need for one of the assistants, in turn obviating the need for the most lateral left 5-mm port.
The port placement of a da Vinci system with a 4-arm configuration is similar except the assistant is usually relegated to the left side and two right lateral ports are 8-mm robotic trocars. The assistant can then use either one or two of the ports on the left side. At least one 10-mm trocar is necessary for suture passage. The authors use a single 10-mm trocar with the port placed about 2 fingerbreadths above the umbilicus on the left. Although this trocar position necessitates the use of an extended-length (bariatric) suction irrigator, the more cephalad positioning of the trocar discourages movement conflicts with the left robotic arms. Careful trocar positioning is more important with the first-generation 3-arm and 4-arm systems. The newer da Vinci S was designed to have a smaller profile for camera and instrument arm movement, thereby making precise trocar placement less vital. The robot is then docked, and the robotic instrument ports and the camera port are fixed to the arms of the robot. This portion of the procedure is initially time-consuming but becomes much shorter with experience. A stepwise approach to robotic transperitoneal prostatectomy is discussed below. Instruments used include a bipolar cautery on the left robotic arm (left hand) and a monopolar cautery scissors or hook/spatula on the right robotic arm (right hand). If a fourth robotic arm is used, large grasping forceps (Cadiere or Prograsp) are also used.
Early posterior dissection – Exposure of seminal vesicles and development of a plane between the prostate and rectum
Some surgeons use a posterior approach for dissection of the seminal vesicles and identification of the plane between the prostate and rectum. This step is performed using a 0° lens. The bowel is pulled superiorly and the rectum identified. The peritoneal reflection is incised in the midline, and blunt dissection is used to identify the ampulla of the vas and the seminal vesicles. Care should be taken to stay in the midline, as the insertion of the ureters in the trigone of the bladder occurs laterally. The vasa can then be dissected and divided bilaterally. The peritoneal reflection is divided slightly more laterally; the seminal vesicles are then encountered. The seminal vesicles are then freed inferiorly and laterally and the vessels at the tip are divided bilaterally. By retracting the vasa and the seminal vesicles superiorly, the plane between the posterior prostate and the rectum can be easily developed under direct visualization.
This plane is carried caudally to the prostatic apex. Care is taken to avoid lateral dissection because of the proximity to the neurovascular bundles. After this plane is well developed, attention is again turned to the development of the extra-peritoneal space. Some surgeons do not routinely use the posterior approach initially and instead dissect the seminal vesicles with anterior traction after separating the bladder neck from the prostate.
Development of the extra-peritoneal space
This step is performed using a 30° upward-looking lens. A transverse peritoneal incision is made extending from the left to the right medial umbilical ligament and extended in an inverted U-shaped manner to the level of the vasa on either side. The vasa can also be divided at this point to aid in bladder mobility. The extra-peritoneal space is developed after the medial and median umbilical ligaments are transected, allowing the bladder, prostate, and bowel to drop posterior and the remainder of the operation to be performed extra-peritoneally. Some authors fill the bladder to help identify the planes of dissection and to aid in dropping the bladder posteriorly.
Lymph node dissection: A 0° lens is used for optimum visualization, and 1:3 scaling is used for lymphadenectomy. Lymphadenectomy is performed at the surgeon’s discretion if the preoperative serum prostate-specific antigen (PSA) value exceeds 10 ng/mL, the biopsy Gleason score is greater than 6, or more than 50% of the biopsy cores are positive for cancer. The anatomic boundaries of the limited bilateral pelvic nodes dissection include the iliac artery superiorly, the obturator nerve inferiorly, the iliac bifurcation cranially, and the obturator fossa caudally. The nodal package is sent for frozen-section analysis only if the nodes appear grossly enlarged.
Exposure of prostatic apex and endopelvic fascia: The 0° lens with 1:3 scaling is used for this part of the dissection. This endopelvic fascia is incised after the prostate is retracted medially with the da Vinci cautery scissors or hook. The fascia is incised from the urethra distally to the prostatovesical junction proximally. Blunt dissection allows sweeping of the levator muscle from the lateral surface of the prostate. Dissection is carried distally until the urethra, with the surrounding puboperinealis muscle, is exposed.
Retro apical dissection and release of the neurovascular bundle
The plane behind the prostate-urethral junction is developed using a combination of blunt and sharp dissection. This dissection helps enormously to precisely identify the posterior apical margin of the prostate at the time of detachment of the specimen.
Bladder neck trans-section
The assistant provides vertical traction on the prostatic suture, and the anterior wall of the bladder is incised until the Foley catheter is observed. The assistant then retracts the catheter to provide counter traction as the posterior bladder wall is cut. Sparing of the bladder neck is possible but uncommon. The bladder neck incision is elliptical so that the posterior lip is slightly longer than the anterior lip. This maneuver aids in visualization of the posterior suture line during anastomosis. Using the da Vinci bipolar forceps, the surgeon grasps the cut end of the posterior bladder neck in the midline and gradually dissects it away from the prostate. The anterior layer of Denonvilliers aponeurosis (fascia) is then exposed and incised, exposing the vasa and seminal vesicles.
If the seminal vesicles were previously released, the plane is easily entered. However, if the surgeon did not elect to use an initial posterior approach, at this point, the left assistant retracts the posterior lip of the prostate anteriorly while the fourth robotic arm depresses the bladder posteriorly to provide a clear operative field for dissection of the seminal vesicles and vas deferens. The vasa are transected, and the seminal vesicles are skeletonized, avoiding damage to the neurovascular bundles.
Once the seminal vesicles are freed, the left assistant retracts the seminal vesicles anteriorly. At this point, the posterior layer of Denonvilliers aponeurosis can be observed between the two lateral prostatic pedicles. This fascia is incised close to the prostate, and a plane between the prostate anteriorly and the rectum posteriorly is developed. The plane of dissection leaves the most posterior layer(s) of Denonvilliers aponeurosis on the rectum. This dissection is carried down to the apex of the prostate.
Control of the lateral pedicles and the veil of Aphrodite (preservation of the neurovascular bundles)
The lateral pedicles at the prostate vesical junction are controlled using Hem-o-lock clips and/or bipolar coagulation. The clips are applied close to the prostate, and the pedicle is divided between them. Once the dissection enters the plane between the prostatic fascia medially and the levator fascia laterally, electro-cautery is avoided and the anterior nerve-sparing dissection proceeds using sharp cutting with scissors and blunt dissection using the grasper. This dissection proceeds distally to the puboprostatic ligaments.
Incision of the dorsal venous complex and urethra
This is the final step of the dissection. Using a 0° lens with 1:3 scaling, the dorsal venous complex is incised tangentially to the prostate to avoid capsular incision. A plane between the urethra and dorsal venous complex is gently developed to expose the anterior urethral wall. The Foley catheter is reinserted and used to identify the anterior surface of the urethra at the urethroprostatic junction. The anterior wall of the urethra is transected with the scissors a few millimeters distal to the apex of the prostate. The posterior wall of the urethra and the rectourethralis muscle are cut under direct vision. The freed specimen is then examined for adequacy of resection margins and is placed in a specimen-retrieval bag.
Urethrovesical anastomosis
Urethrovesical anastomosis is performed using a hybrid tied suture, which consists of two 3-0 Monocryl sutures (one dyed and the other undyed) tied to each other to form a double-ended suture on RB-1 needles, each 6 inches long. Some authors advocate the use of a similarly constructed Vicryl suture, although this suture may prove to be more difficult to tighten prior to ligation.
The initial throw is placed outside in the bladder at the 5-o'clock position, and the dyed suture is pulled through so that the knot lies securely on the outside wall of the bladder posteriorly. The dyed suture is then used as a running stitch to suture the posterior bladder wall to the urethra. The dominant hand is used for the urethral pass, and the non dominant hand is used for the vesical pass. Approximately 5-6 throws are made posteriorly, with the assistant placing slight tension on the suture, if necessary. At the corner, the surgeon reverses the suture within the bladder lumen and passes the suture outside-in on the urethra.
The post suture ends at the 11-o'clock position and is held on traction by the left assistant to prevent loosening of the stitch. The undyed suture is then used to perform the anterior part of the urethravesical anastomosis extending from the 5-o'clock position to the 12-o'clock position. The two sutures are then tied to each other to complete the anastomosis. The bladder is irrigated with 200 ml of saline to look for any leaks. Any leaks are reinforced with sutures. A new 20F indwelling Foley catheter is placed, and the balloon is filled with 30 ml. The specimen is retrieved and ports closed.
Robotic Extra-peritoneal Approach
The patient is placed supine in a 15° Trendelenburg position. A 3-cm horizontal incision is made 1 fingerbreadth below the umbilicus, and the pre-peritoneal space is entered. A blunt port Hasson canula is placed, and the preperitoneum is insufflated to 18 mm Hg. The space of Retzius is developed by blunt dissection using a conventional laparoscope until the pubic symphysis is reached. A 5-mm port is then placed in the midline 2 fingerbreadths above the symphysis to further develop the retro-pubic space. The right and left extra-peritoneal robotic instrument ports are placed 4 cm below the camera port at the pararectal line. Two additional assistant ports are placed on the right side, the first at the level of the umbilicus above the right robotic instrument port and the second to the right and in line with the right robotic instrument port. The procedure essentially follows the same steps of the robotic prostatectomy described above, but the dissection is entirely extraperitoneal.
Laparoscopic Trans peritoneal Approach
The patient is placed supine with the arms at the sides and the legs spread apart and in an extreme Trendelenburg position. One surgeon and one assistant perform the operation, with a right-handed surgeon standing on the left side of the patient. The Montsouris group uses the AESOP voice-controlled robot to hold the telescope.
Five ports are placed in a diamond configuration, (1) a 10-mm telescope port at the umbilicus, (2) a 10-mm port at the McBurney point, (3) a 5-mm port at the midpoint between the umbilicus and the pubis symphysis in the midline, (4) a 5-mm port at the midpoint between the left anterior superior iliac spine and the umbilicus, and (5) the final 5-mm port at the right pararectal line at the level of the umbilicus. The abdomen is initially inspected, and a pelvic lymphadenectomy is performed, if required.
The procedure is begun with incision of the peritoneal fold between the rectum and bladder and the dissection of the seminal vesicles posteriorly. The seminal vesicles are retracted anteriorly, and the Denonvilliers aponeurosis is incised. The dissection is carried distally to the level of the rectourethral muscle, separating the prostate anteriorly from the rectum posteriorly. Attention is then directed anteriorly, and the peritoneum is incised to enter the space of Retzius, thereby causing the bladder to fall posteriorly. The endopelvic fascia is incised, and the levator muscle is pushed laterally to free the prostate gland. This is followed by ligation of the dorsal vein. The next step is incision of the bladder neck.
Finally, the lateral pedicles are dissected, and the urethra is transected to free the prostate gland with the seminal vesicles. The final step of the surgery is construction of the urethrovesical anastomosis. The Montsouris group performs the anastomosis with interrupted 3-0 re-absorbable sutures on a five-eighths needle. A total of 8 sutures are placed. Finally, a drain is placed and the ports closed.
The advantages of the transperitoneal approach include familiarity with anatomy, adequate space for dissection, and the presence of several reference points to aid the surgeon in orientation. Maximum mobility of the bladder is achieved in this approach, which helps provide a tension-free urethravesical anastomosis.
Disadvantages of the transperitoneal approach include communication of the anastomotic site to the peritoneal cavity with the potential for peritoneal urine leak and ascites. The transperitoneal approach also increases the risk of bowel injury, ileus, and adhesions.
Laparoscopic Extraperitoneal Approach
The patient preparation, position, and draping are similar to the transperitoneal technique except that a steep Trendelenburg position is unnecessary.
A 1-cm infra-umbilical incision is made and carried down to the pre-peritoneal space, which is bluntly dissected, and a Hasson canula is placed in this space. The extraperitoneal space is then developed by either blunt dissection using additional trocars or by using a visual balloon-dilating trocar or Gaur balloon dilator. Once the space is developed, the steps of the surgery mimic those of the transperitoneal approach except that the seminal vesicles and vas are dissected after the bladder neck is transected.
Theoretical advantages of this approach include its feasibility in patients who have undergone extensive abdominal surgeries and its minimal associated risk of bowel injury. The peritoneum acts as a self-retractor for the intestines, thus obviating the need for steep Trendelenburg positioning. Reports of simultaneous inguinal hernia repairs using prosthetic mesh have been published. The most significant limitation of this approach is the lack of adequate space for dissection and suturing. Also, because the peritoneal and urachal attachments of the bladder are not divided, tension at the urethravesical anastomosis is a concern. As a result, the extraperitoneal approach should be performed only by experienced laparoscopic surgeons.
Advantages and Disadvantages of Robotics versus Laparoscopy
For performing radical prostatectomy the robotic techniques have several advantages over laparoscopic techniques.
- Because the display system of the da Vinci projects the image in the direction of the surgeon's hands, the optically correct hand-eye coordination is restored. This is more difficult with laparoscopy, in which the camera is sometimes offset to the plane of dissection.
- The 11-mm telescope in the da Vinci system is a combination of two 5-mm optical channels (one for the right and one for the left eye), which have 2 separate 3-chip–charged coupling devices in the camera head. The 2 images are displayed to provide 3-dimensional stereoscopic vision to the surgeon, providing depth perception lacking in laparoscopy. The conventional laparoscopic technique does not provide a 3-dimensional depth of view.
- The movements of the robotic system are intuitive (i.e., a movement of the master control to the right causes the instrument to move to the right), as opposed to the counterintuitive movements in laparoscopy with fulcrum movement effects (i.e., movement of the laparoscopic instrument to the right by the surgeon causes the tip of the instrument to move to the left inside the patient's body).
- The robotic systems provide increased precision by filtering hand tremors, providing magnification (10X or 15X), and providing scaling for the surgeon's movements (a 1:3 scaling means that a 3-in movement of the master is translated into a 1-in movement of the instrument tip).
- The robotic instruments have articulated tips, which permit 7° of freedom in movements (i.e., they mimic human wrist movements, including rotation), which is unlike laparoscopy, with which only 4° of freedom are permitted.
Robotic techniques also have disadvantages.
- The current-generation robot is still bulky and tends to limit the working space of the assistant(s).
- The availability of instrumentation for the robotic systems is presently limited, although development of new instruments is ongoing.
- Economically, the robotic system is viable only for centers with a high volume of cases or multidisciplinary robotic use. The system cost exceeds $1.2 million, and the annual maintenance costs range from $100,000-$150,000.
Comparative Studies
Relatively few studies have directly compared robotic or laparoscopic radical prostatectomy with open radical retro-pubic prostatectomy. Even fewer studies have compared pure laparoscopic prostatectomy with robotic prostatectomy. Because of the inherent difficulty with performing a prospective randomized trial for minimally invasive prostatectomy, most studies are designed as case-matched control studies.
Conclusions
Most of the major leaps in the evolution of minimally invasive surgical treatments for prostate cancer have been driven by the efforts of only a few pioneering groups. These groups are to be commended for their hard work and commitment to improving these complex procedures. Although laparoscopic radical prostatectomy still requires considerable technical skill, robotic technology has bridged the gap for open surgeons to perform these complex procedures.
The literature supports improved operative and perioperative parameters with minimally invasive techniques, including decreased blood loss, shorter hospital stay, and decreased time of catheterization. In the available studies, both laparoscopic and robotic prostatectomy seems to improve functional parameters, namely potency and continence, compared with open prostatectomy. Unfortunately, these studies are usually reported by high-volume single-center experiences and are criticized for their reproducibility across multiple centers and levels of surgeon experience. Reported oncologic outcomes for laparoscopic and robotic prostatectomy are comparable with those of open series, although long-term oncologic data are currently limited.
As the penetration of robotics increases, urologists are challenged to adapt to the rapid changes in this procedural technology. This raises challenges both for established urologists and for urology training programs. Little has been done to establish firm parameters in terms of case volume and operative learning curve, and most large centers are in a constant state of procedural evolution intended to improve clinical outcomes. Finally, the definitive prospective, randomized clinical trial comparing laparoscopic or robotic prostatectomy to open radical prostatectomy would be very difficult to perform given the reported benefits from the minimally invasive procedures. The highest level of achievable data will likely be a well-performed meta-analysis of the literature intended to confirm the consistency of data between clinical centers and individual surgeons.






