Introduction
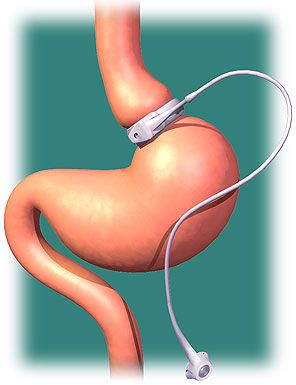
A laparoscopic adjustable gastric band, is an inflatable silicone device that is placed around the top portion of the stomach, via laparoscopic surgery, in order to treat obesity. Adjustable gastric band surgery is an example of bariatric surgery designed for obese patients with a body mass index (BMI) of 40 or greater or between 35–40 in cases of patients with certain comorbidities that are known to improve with weight loss, such as sleep apnea, diabetes, osteoarthritis, GERD, Hypertension (high blood pressure), or metabolic syndrome, among others.
Medically and surgically Obesity can be treated. Treatment is difficult for obesity by medically, because the amount of weight lost is small and patients tend to regain most of the weight. A 2010 prospective, randomized controlled trial in 50 adolescents demonstrated that a greater percentage of patients achieved a loss of 50% of excess weight with laparoscopic gastric banding than with lifestyle intervention. Operation that are designed to cause significant and long-lasting weight loss in patients who are severely obese are termed bariatric surgery. The term bariatric surgery is derived from the Greek words baros (weight) and iatreia (medical treatment). Laparoscopic lap band placement is one such surgery.
Causes of Obesity are a combination of genetics, environmental issues, and behavioral factors. Consumption of high-calorie foods, consumption of too much food, and a sedentary lifestyle all work together to create this condition. Obesity is associated with the development of diabetes mellitus, hypertension, dyslipidemia, arthritis, sleep apnea, cholelithiasis, cardiovascular disease, and cancer.
More than 100 million Americans (65% of the adult population) are overweight. After smoking Obesity is the second-leading cause of preventable death in the United States. Obesity-related diseases account for 400,000 premature deaths each year. Body mass index (BMI) describes relative weight for height and correlates significantly with an individual’s total body fat. BMI is based on height and weight and applies to adults of both sexes. BMI is calculated as follows: BMI equals weight in kg/height in m2 or weight in lb/height in square inches.
The placement of the band creates a small pouch, or stoma, at the top of the stomach. This pouch holds approximately ½ cup of food. The pouch fills with food quickly, and the band slows the passage of food from the pouch to the lower part of the stomach. As the upper part of the stomach registers as full, the message to the brain is that the entire stomach is full, and this sensation helps the person to be hungry less often, feel full more quickly and for a longer period of time, eat smaller portions, and lose weight over time
Indications
For selecting bariatric surgery candidates in 1991, the National Institutes of Health (NIH) provided a consensus statement. If the patient met one of the following criteria then they were considered candidates for surgery:
- Body mass index (BMI) >40
- BMI of 35-40 plus one of the following obesity-associated co-morbidities:
- Obesity-related cardiomyopathy
- Excess diabetes mellitus
- Excess sleep apnea
- Pickwickian syndrome
- Osteoarthritis interfering with lifestyle
To be candidates for bariatric surgery, patients should have attempted, without failure, to lose an appropriate amount of weight through supervised diet changes. With postoperative diet and exercise must be complying with by Patients.
Contraindications:
- An active major psychiatric disorder
- History of substance abuse
- End-stage organ disease (eg, cardiac, liver, pulmonary)






