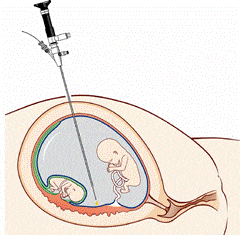
Fetoscopy
Definition
Fetoscopy is definitely an endoscopic procedure during pregnancy to permit use of the fetus, the amniotic cavity, the umbilical cord, and also the fetal side from the placenta. A little (3-4 mm) incision is created in the abdomen, as well as an endoscope is inserted through the abdominal wall and uterus into the amniotic cavity. Fetoscopy allows medical interventions such as a biopsy or perhaps a laser occlusion of abnormal arteries. Fetoscopy is really a process that employs a guitar known as a fetoscope to judge or treat the fetus while pregnant.
Purpose
There are two various kinds of fetoscopy: endoscopic and external.
Endoscopic fetoscopy
The second kind of fetoscope is really a fiber-optic endoscope. It's placed to the uterus either transabdominally or transcervically to visualise the fetus, to acquire fetal tissue samples, in order to perform fetal surgery. Certain birth problems are challenging through the labor and delivery process, while some may develop quickly after birth to cause substantial disability or death. Fetal surgical methods making use of the endoscopic fetoscope offer early intervention to be able to treat such problems before they become severe. A few of the fetal irregularities which may be treated by endoscopic fetoscopy are:
- Twin/twin transfusion syndrome (TTTS). In certain twin pregnancies, both fetuses will share a placenta. TTTS happens in approximately 15% of those twins when blood volume between patient’s fetuses is unequal, causing unusually low blood volume within the donor twin and unusually high volume within the recipient twin. There's normally a large difference in dimensions between patient’s twins. Around 70-80% of fetuses struggling with TTTS will die without intervention.
- Congenital diaphragmatic hernia (CDH). In infants with CDH, the diaphragm which is sometimes called the thin muscle that isolates the chest area in the abdomen doesn't create properly. The abdominal organs may go into the chest cavity via a hole and cause pulmonary hyperplasia. CDH happens in about one inch every 2,000 births.
- Acardiac twin. This problem also happens in monochorionic pregnancies, but one twin builds up usually as the other evolves with no heart. The acardiac twin receives its circulation in the normal twin, whose heart must now continue to work harder to supply blood through both fetuses. About 50-75% of acardiac twins will die consequently. An acardiac twin happens in 1% of monochorionic pregnancies and something from 35,000 overall pregnancies.
- Urinary tract obstruction. The urethra can become blocked in utero or neglect to create normally. At these times, urine can support to the kidneys and damage tissue or make the bladder being made bigger. The quantity of amniotic fluid also reduces because fetal urine is its key component. Pulmonary hypoplasia generally results since the lungs depend on amniotic fluid within their advancement.
External fetoscopy
Another fetoscope looks like a stethoscope, however with a headpiece. It's utilized externally about the mother's abdomen to auscultate the fetal heart tones after about 18 week’s gestation. Additionally, it enables a birth attendant to watch the fetus from time to time and be sure how the baby is tolerating labor with no mother needing to be mounted on a continuing fetal monitor.
Description
The external fetoscope can be used to hear fetal heart tones for rate and rhythm. The earpieces and also the headpiece permit auscultation via both air and bone conduction. External fetoscopy is relatively cheap, noninvasive, and doesn't need electricity. It is not easy, however, to obviously hear the fetal heart tones just before 18 to twenty weeks gestation. Doppler ultrasound can identify fetal heart tones around weeks 10 to 12. Endoscopic fetoscopy runs on the thin (1 mm) fiber-optic scope. Designed within the 1970s, the endoscope was originally introduced transabdominally to visualise the fetus for gross irregularities diagnosed by ultrasound in order to acquire tissue and liquid blood samples. It had been carried out after about 18 week’s gestation. Despite practitioner expertise, associated fetal loss was 3%-7%. Throughout the 1980s, ultra-sound-guided needle sampling of cord blood swapped out fetoscopy when examples of fetal blood were needed.
As laparoscopic and microsurgical methods have grown to be more prevalent and also the instrumentation is becoming heightened technologically, fetoscopy has enhanced for fetal diagnostic and therapeutic purposes. Fetal surgery carried out with an open maternal abdomen includes a greater risk of such problems as infection, premature rupture of membranes, preterm labor, or fetal death. If surgery is conducted via fetoscopy, which takes a really small transabdominal incision, the potential risks less difficult smaller? Methods have sophisticated enough to permit some fetoscopy to become performed within the first trimester through the mother's cervix. The word "obstetrical endoscopy" can be utilized for surgery about the placenta, umbilical cord, or about the fetal membranes. The word "endoscopic fetal surgery" can be used for such a task since the repair of the fetal congenital diaphragmatic hernia or blocked bladder.
Demographics
External fetoscopy enables to figure out the fetal heartbeat in a woman having a practical pregnancy, although specific situations may compromise its quality just like a noisy environment, an obese mother, or hydramnios. No demographic data can be found regarding patients going through operative fetoscopy, as it is a comparatively new procedure being carried out of them.
Who performs the process and where could it be conducted?
Health-care professionals who could use the external fetoscope incorporate a nurse practitioner, nurse midwife, and obstetrician. External fetoscopy might be carried out in a setting using the pregnant woman lying supine or perhaps in a semi-sitting position. Endoscopic fetoscopy takes a higher level of skill and experience by fetal doctors and it is carried out inside a hospital setting. Throughout the procedures, a radiology technician may carry out an ultrasound, along with a laboratory technician might be involved with blood sampling. Nurses will take part in both outpatient and inpatient procedures.
Diagnosis/Preparation
Using external fetoscopy needs use of the maternal abdomen, using the mother lying supine or perhaps in a semi-seated position. Afterwards, mom has the capacity to wake up and resume an ordinary activity level. Preparation for endoscopic fetoscopy is determined by the extent from the procedure, and be it carried out transcervically or transabdominally. Receiving a small fetal tissue sample is really a smaller process in comparison to fetal surgery. Additional factors include outpatient versus inpatient stay and anesthesia (both maternal and fetal). For many procedures medication might be given to temporarily decrease fetal movement to reduce the chance of fetal injury. Maternal anesthesia might be local, regional, or general.
Questions a patient should ask a doctor:
- Why is fetoscopy suggested with such case?
- What options to fetoscopy are available to a patient?
- For endoscopic fetoscopy, what's going to function as the results when there is no medical intervention?
- For endoscopic fetoscopy, will the process be practiced with an outpatient basis? Which kind of anesthesia is going to be used?
Risks
The only real potential problem with external fetoscopy may be the chance of missing an abnormal heartbeat or rhythm. Its effectiveness and accuracy rely on the ability of the practitioner. Endoscopic fetoscopy has got the possibility of causing infection within the fetus and/or mother; premature rupture from the amniotic membranes; premature labor; and fetal death. When endoscopic fetal surgery is performed rather than open-uterus tential risks towards the mother and fetus are reduced. The potential risks are since the incision is considerably smaller, with less potential loss of blood, decreased uterine irritability, and reduced risk of early miscarriage.
Normal results
The standard fetal heartbeat is 120 to 160 beats each minute, whatever the method employed for auscultation. Some variability of fetal heartbeat is anticipated, since the heartbeat increases with fetal activity and slows with fetal rest. Results anticipated using endoscopic fetoscopy will be different with respect to the process undertaken. The goal is perfect for the most benefit using the least risk or problem to both mother and fetus.
Morbidity and mortality rates
There isn't any morbidity or mortality related to external fetoscopy. Regarding endoscopic fetoscopy, the chance of fetal loss is projected to become between 3% and 5%. The process is therefore generally recommended just for the greater serious cases of fetal disorders which may be treated while pregnant.
Aftercare
External fetoscopy doesn't need aftercare. The concern following fetal endoscopic use is determined by the extent from the procedure and also the kind of anesthesia used. When the procedure is performed with an outpatient basis, mom and fetus is going to be supervised for any time period just before discharge. More substantial surgery will need inpatient hospital postoperative care.
Alternatives
Physician may pay attention to the fetal heartbeat using a hand-held Doppler device, which makes use of ultrasound to boost the heartbeat. A continuing electronic fetal monitor could also be used to trace the fetal heartbeat and maternal uterine contractions. It's held from the mother's abdomen by way of elastic straps. Open fetal surgery is definitely an option to internal fetoscopy. It's employed for conditions that can't be treated endoscopically. An incision is created with the abdomen and also the uterus is partly taken off patient’s body. Amniotic fluid is drained in the uterus and saved in a warmer for replacement after completing the surgery. An incision is created within the uterus is known as hysterotomy. To be able to minimize bleeding from the uterus, a device known as a uterine stapler can be used to create an incision while at the same time placing staples round the perimeter from the incision to avoid bleeding. Surgery will be performed about the fetus with the opening within the uterus to find the abnormality and take away or do the repair. There’s the upper chance of infection, premature labor, and seepage of amniotic fluid with open fetal surgery than there's with fetoscopy.






