Esophageal resection
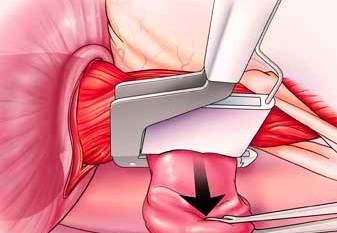
Esophageal resection
Definition
An esophageal resection may be the surgery from the esophagus, nearby lymph nodes, and occasionally of the stomach. The esophagus is really a hollow muscular tube that passes with the chest in the mouth towards the stomach-a "food pipe" that bears food and liquids towards the stomach for digestion and nutrition. Elimination of the esophagus needs reconnecting the residual the main esophagus towards the stomach to permit swallowing and also the ongoing passage of food. The main stomach or intestine enables to get this to connection. A number of surgical methods and approaches are utilized, based on just how much or which the main esophagus must be taken out; whether the main stomach is going to be taken out; the patient's overall condition; and also the doctor's preference.
There are two basic esophageal resection surgeries. Esophagectomy may be the surgery from the esophagus or perhaps a cancerous part of the esophagus and nearby lymph nodes. Esophagogastrectomy may be the surgery from the lower esophagus and also the upper part of the stomach that links towards the esophagus, carried out when cancer has been discovered both in organs. Lymph nodes within the area will also be taken out. An esophageal resection might be performed in conjunction with pre- and postoperative radiation and chemotherapy also known as chemoradiation.
Purpose
An esophagectomy is frequently carried out to deal with early-stage cancer from the esophagus prior to the cancer has spread towards the stomach or other organs. Esophagectomy is a treatment for esophageal dysplasia, which is a precancerous condition from the cells within the lining from the esophagus. Lymph nodes are removed to become tested for that existence of cancer cells, which will help to find out when the cancer is spreading. Esophagectomy can also be suggested when irreversible ruin has taken place due to traumatic problems for the esophagus; swallowing of caustic (cell damaging) agents; chronic inflammation; and complicated motility disorders that hinder the passage of food towards the stomach.
An esophagogastrectomy is conducted when cancer from the esophagus can be spreading to nearby lymph nodes and also to the stomach, producing new tumors. When cancer invades other tissues in this manner, it is stated to become metastatic. The aim of esophagogastrectomy would be to relieve difficult or painful swallowing in patients with sophisticated esophageal cancer, and also to prevent or slow multiplication of metastases to more faraway organs like the liver or even the brain.
Demographics
The candidates for esophageal resection parallel those at high-risk for esophageal cancer. Esophageal cancer is located among middle-aged and older adults, using the average age at diagnosis between 55 and 60. Esophageal cancer and esophageal dysplasia appear much more often in males compared to women. One sort of esophageal cancer occurs more often in African Americans; another type adenocarcinoma is much more common in Caucasian males. Caucasian and Hispanic men having a good reputation for gastroesophageal reflux disease (GERD) will also be at greater risk, because GERD can cause alterations in cells from the esophagus that could result in cancer. Higher risks will also be related to smoking (45%), excessive drinking (20%), and lung disorders (23%).
Who performs the process and where could it be carried out?
Esophageal resection surgeries are carried out inside a hospital or clinic operating room with a general doctor or perhaps a thoracic surgeon.
Description
Even though esophageal cancer isn't as common as breast and colon cancer, its rate of occurrence is increasing. This rise is regarded as associated with a rise in gastroesophageal reflux disease, or GERD. The esophagus includes a muscular opening, or sphincter, in the entrance towards the stomach, which often keeps acid from moving upward. In individuals with GERD, the esophageal sphincter enables partially digested food and excess gastric acid to flow back to the esophagus. This occurrence is called regurgitation. Regurgitation continuously exposes the liner from the esophagus to considerable amounts of acid, causing repetitive harm to cells from the esophageal lining. The end result is Barrett's esophagus, an ailment where the normal cells called squamous cells from the esophageal lining are changed through the glandular kind of cells that usually line the stomach. Glandular cells tend to be more resistance against acid ruin but simultaneously, they are able to more readily become cancer cells. Studies at New York's Memorial Sloan-Kettering Hospital show that only 30% of individuals identified as having Barrett's esophagus will later be identified as having cancer; another 70% won't develop dysplasia, the precancerous condition. Effective treatment of acid reflux disease is regarded as an issue within the low incidence of cancer in individuals with Barrett's esophagus. Other forms of cancer also occurs within the esophagus, including melanoma, sarcoma, and lymphoma.
The danger components for esophageal cancer consist of:
- Abuse of alcohol.
- Use of tobacco. The greatest risk for esophageal cancer may be the mixture of smoking and heavy alcohol use.
- Barrett's esophagus due to long-term acid reflux disorder.
- Esophageal webs. They are bands of irregular tissue within the esophagus making it hard to swallow.
- Accidental swallowing for cleaning liquids or other caustic substances in early childhood.
- A rare passed down disease called tylosis, by which excess layers of skin grow about the hands and also the soles from the feet. Individuals with this problem are almost sure to grow esophageal cancer.
- A low-fiber diet; that's, dieting that's lower in vegetables and fruit, and whole grain products that maintain their outer bran layer. Other dietary risk components contain such vitamin and mineral deficiencies, as lower levels of zinc and riboflavin.
- Achalasia. Achalasia is definitely an impaired functioning from the sphincter muscle between patient’s esophagus and also the stomach.
Cancer from the esophagus begins within the inner layers from the tissue that lines the passage way and develops outward. Cancer from the top layer from the esophageal lining is known as squamous cell carcinoma; it may take place anywhere across the esophagus, but seems usually in the centre and upper portions. It may spread extensively inside the esophagus, demanding the surgery of huge areas of the esophagus. Adenocarcinoma may be the kind of cancer that develops within the lower end from the esophagus close to the stomach. Both kinds of cancer may produce in individuals with Barrett's esophagus. As much as 83% of patients going through esophagectomy have been shown have adenocarcinoma. This improvement might be associated with such alterations in risk factors as reduced smoking and alcohol use in addition to increased reflux disease. People at high-risk for esophageal cancer ought to be analyzed and tested regularly for alterations in cell types.
Esophageal cancer is classified in 6 stages based on laboratory study of tissue cells in the esophagus, nearby lymph nodes, and stomach. The 6 stages are:
- Stage 0. This is actually the earliest stage of esophageal cancer, by which cancer cells can be found only within the innermost lining from the esophagus.
- Stage I. Cancer has spread much deeper layers of cells but hasn't spread into nearby lymph nodes or organs.
- Stage IIA. Cancer has occupied the muscular layer from the esophageal walls, sometimes so far as the outer wall.
- Stage IIB. Cancer has invaded the lymph nodes close to the esophagus and it has most likely spread into much deeper layers of tissue.
- Stage III. Cancer exists within the tissues or lymph nodes close to the esophagus, particularly in the trachea or stomach.
- Stage IV. Cancer has spread to additional distant organs, like the liver or brain.
Unfortunately, the signs of esophageal cancer generally don't appear before disease has advanced beyond the first stages and it is already metastatic. Without early diagnostic screening, patients may wait to see a physician only if there's little chance of cure. The signs of esophageal cancer can sometimes include problems swallowing or painful swallowing; unexplained weight reduction; hiccups; pressure or burning within the chest; hoarseness; lung disorders; or pneumonia.
The choice to carry out an esophageal resection is going to be made when staging tests have proved the existence of cancer and it is stage. Two-thirds of people that undergo endoscopy, a detailed study of the interior lining from the esophagus, and biopsies will currently have cancer, which could progress rapidly. Many will be given surgery yet others with medical therapy, with respect to the stage from the cancer, the patient's overall health status, and also the level of risk. Taking out the esophagus or even the affected portion is easily the most common treatment for esophageal cancer; it may cure the condition when the cancer is incorporated in the initial phases and also the patient is good enough to endure the stressful surgery. Esophagectomy is going to be recommended if early-stage cancer or perhaps a precancerous condition continues to be proved through extensive diagnostic testing and staging. Esophagectomy isn't a choice when the cancer has spread towards the stomach. In this instance an esophagogastrectomy will often be practiced to get rid of the cancerous the main esophagus and also the upper the main stomach.
Esophagectomy
An esophagectomy requires about Six hours doing. The individual will be presented general anesthesia, keeping her or him unconscious and free from pain during surgery. One of many approaches or incisional strategies is going to be used, chosen through the doctor to achieve sufficient use of top of the abdomen and take away the esophagus or even the tumor and also the nearby lymph nodes. The 4 common incisional approaches are: transthoracic, that involves a chest incision; Ivor-Lewis, a side entry with the fifth rib; three-hole esophagectomy, which uses small incisions within the chest and abdomen to support using devices; and trans-hiatal, that involves a mid-abdominal incision. The approach chosen depends upon the extent from the cancer, the position of the tumor or blockage, and also the overall condition from the patient.
Inside a minimum-access laparoscopic and thoracoscopic treatment, the doctor makes a number of small incisions about the chest and abdomen by which they might insert thin telescopic devices with light sources. The abdomen is going to be inflated with gas to expand the abdominal cavity and provide the doctor a much better view of the procedure. First, the camera-tipped laparoscope is going to be inserted through one small incision, permitting pictures from the organs within the abdominal area to become displayed on the video monitor within the operating room. When the surgeon will make use of a part of the stomach to change the resected esophagus, she or he will first identify the fundus, or upper part of the stomach. The fundus is going to be manipulated, stapled off, and taken out laparoscopically, to become sutured in position (gastroplasty) as an alternative esophagus. Next, the physician will pass thorascopic devices to the chest through another incision. The esophagus or cancerous part of the esophagus is going to be visualized, manipulated, cut and taken away. Lymph nodes in the region may also be removed. Then patient’s doctor will either pull-up some from the stomach and connect it towards the remaining part of the esophagus called anastomosis, or make use of a bit of the stomach or intestine, generally the colon, to rebuild the esophagus. Either procedure allows the individual to swallow and pass food and liquid towards the stomach after recovery. As outlined above, other approaches enable to access the affected part of the esophagus.
There are many variations of the esophagectomy, including:
- Vagal-sparing esophagectomy. This process maintains the branches from the vagus nerve supplying the stomach, with only minimal change from the size the stomach and also the nerves that control acid generation and digestive functions.
- Laparoscopic esophagectomy. This can be a less invasive technique carried out through several small incisions about the chest and abdomen using the camera-tipped laparoscope along with a video monitor to steer elimination of the esophagus or tumor together with nearby lymph glands.
- Standard open esophagectomy. This method needs larger incisions to become produced in the chest area called thoracotomy as well as in the abdomen so the doctor can dissect the esophagus or cancerous portion and take away it combined with the nearby lymph nodes. The esophagus may then be reconnected towards the stomach utilizing a part of either the stomach or even the colon.
Esophagogastrectomy
An esophagogastrectomy can also be major surgery carried out using the patient under general anesthesia. The doctor will pick the incisional approach which allows the perfect access for resecting the lower part of the esophagus and also the upper part of the stomach. The doctor's decision is determined by the extent from the cancer, the quantity of the esophagus that must definitely be removed, and also the patient's all around health status. An esophagogastrectomy can be carried out being an open procedure through large incisions, or like a laparoscopic process through small incisions. Inside a minimum-access laparoscopic procedure, a number of small incisions are created within the patient's abdomen. A laparoscope is going to be placed through one small incision, allowing images from the abdominal organs to become displayed on the video monitor. As with an esophagectomy, gas enables you to inflate the abdominal cavity for better viewing and space for that surgeon to move. The cancerous upper part of the stomach will first be stapled off and resected. The cancerous part of the esophagus will be slashed and taken off together with nearby lymph nodes. Finally, some from the stomach is going to be pulled upward and attached to the remaining part of the esophagus; or, if the majority of the esophagus continues to be removed, a bit of the colon is going to be accustomed to construct a brand new esophagus. Sometimes the physician must make an incision within the neck to be able to access and resect top of the part of the esophagus, then making an anastomosis between patients esophagus along with a part of the stomach.
Questions a patient should ask a doctor:
- What would be the risks involved with having one of these surgery?
- Will this surgery cure patient’s cancer? Does it let a patient live longer?
- How will the surgery be practiced? Just how long does it take?
- Why will a patient need this surgery?
- What would be the chances how the cancer is?
- What are patient’s options basically do not have the surgery?
- How quickly a patient is going to recover?
- How often perhaps a doctor has performed this process? How frequently could it be performed on this hospital?
- How much discomfort can one expect for the short term? In the long run?
- What type of care should a patient have at doctor’s supervision subsequently?
Preparation/Diagnosis
Preparation
The individual is going to be accepted towards the hospital at the time from the operation or even the previous day, and patient will have to come to a pre-operative nursing unit. The doctor and anesthesiologist will go to the patient to explain the resection process and answer any queries how the patient might have. The conventional preoperative blood and urine tests are going to be carried out. An intravenous line (IV) is going to be introduced within the patient's vein for that administration of fluids and pain medicines during and following the surgery. Sedatives might be given prior to the patient who is about to come to the operating room.
Diagnosis
Diagnosing of esophageal cancer starts with a careful background and overview of symptoms, and requires a variety of diagnostic assessments. An esophagoscopy might be performed within the doctor's office, allowing a doctor to look at the interior from the esophagus having a lighted telescopic tube. A barium swallow is yet another common screening test, carried out within the radiology (x-ray) department from the hospital or perhaps in a personal radiology office. Inside a barium swallow, the individual drinks a tiny bit of radiopaque barium which will highlight any raised areas about the wall from the esophagus when chest x-rays are taken. The x-ray studies will disclose irregular patches which may be early cancer or larger abnormal areas that could narrow the esophagus and may represent a far more advanced stage of cancer. If either of those conditions exists, the doctors may wish to read the proper diagnosis of esophageal cancer; figure out how far it's invaded the walls from the esophagus; and whether or not this has spread to close by lymph nodes or organs. This staging process is important to be able to figure out the very best treatment for that patient. One staging way is a diagnostic process called endoscopic ultrasound. A doctor will thread an endoscope, which is a tiny lighted tube having a small ultrasound probe at its tip, to the patient's mouth and into the esophagus. This process allows the interior from the esophagus to become viewed on the monitor to exhibit what lengths a tumor has occupied the walls from the esophagus. Simultaneously, a doctor is capable of doing biopsies of esophageal tissue by cutting and taking away small pieces for microscopic study of cells for cancer staging. Staging tests could also include computed tomography (CT scans); thorascopic and laparoscopic assessments from the chest and abdomen; and positron emission tomography (PET).
Risks
Among the primary risks related to esophageal resection surgeries is leakage to begin from the anastomosis, the place where a new feeding tube was sutured towards the remaining esophagus. As much as 9% of patients happen to be reported to build up leaks, most happening whenever a part of the stomach as opposed to the colon was adopted to create the brand new portion of the esophagus.
Other risks include:
- narrowing from the remaining esophagus, which might cause swallowing problems
- adverse reactions to anesthesia
- formation of thrombus that may go one's heart, lungs, or brain
- increased acid reflux disease and heartburn due to problems for or elimination of the esophageal sphincter
- nerve injury, which could cause faulty emptying from the stomach
- infection
- breathing complications and pneumonia
Normal results
Esophageal resection, particularly esophagectomy, could be curative if cancer hasn't spread beyond the esophagus. About 75% of patient going through esophagectomy is going to be found to possess metastatic ailment that has spread with other organs. Esophagectomy will decrease symptoms in many patients, specifically swallowing difficulties that will enhance the patient's nutritional status too. Patients whose esophagectomy is preceded and then a mix of chemotherapy and radiation remedies have longer periods of survival. The normal consequence of an esophagogastrectomy is palliation that is the pain relief of symptoms with no cure. Because esophagogastrecomy is definitely carried out when metastases have been found elsewhere in patient’s body, the process may reduce pain and difficulty in swallowing, and could delay multiplication of the cancer towards the liver and brain. Cure from the disease, however, isn't an expectation. Patients having less invasive laparoscopic and thorascopic resection methods are experiencing less pain and fewer problems than patients going through open procedures.
Morbidity and mortality rates
Because 75% of esophagectomy patients and 100% of esophagogastrectomy patients may have metastatic disease, morbidity and mortality rates for these methods are high. Thirty-day mortality for esophagectomy ranges from 6-12%; it's 10% or more for esophagogastrectomy. Patient’s survival of early-stage cancer after esophagectomy runs from 17 to 34 months if surgery alone may be the treatment. The mortality rate for early-stage cancer patients having esophagectomy alone is greater than when surgery is coupled with pre- and post-operative chemoradiation. The three-year survival rate for early-stage cancer affected individuals who obtained pre- and post-esophagectomy chemoradiation is all about 63%. Better staging methods, more cautious choice of patients, and much better surgical techniques will also be thought to be accountable for the rise in postoperative survival rates. Recurrence of cancer in esophagectomy patients can actually cover 43%. A greater percentage of patients going through esophageal resections survive beyond the 30-day postoperative period in hospitals in which the doctors carry out these methods regularly.
Aftercare
Soon after surgery the individual is going to be sent to a recovery area in which the pulse, body's temperature, and heart, lung, and kidney function is going to be monitored. Hours later, the individual is going to be used in a concentrated care area. Surgical wound dressings are going to be clean and dry. Pain medicine will be presented when needed. A chest tube introduced during surgery is going to be checked for drainage and removed once the drainage stops. A nasogastric tube, also positioned during surgery, is going to be accustomed to drain stomach secretions. Nurses will check it frequently and rinse it. It is going to be removed through the doctor. Before patient has the capacity to swallow soft foods, she or he is going to be fed intravenously or via a feeding tube which was put into the little intestine during surgery. Patient is going to be asked to cough and also to breathe deeply after surgery to completely expand the lungs and assist in preventing infection and collapse from the lungs. Walking and movement may also be asked to promote a quicker recovery.
About 10-14 days following the surgery, the individual will be presented another barium swallow so the doctor can look at the esophagus for just about any regions of leaking fluid. If they are not seen, the nasogastric tube can be taken off. The individual may then start to sip clear liquids, followed slowly by small quantities of soft foods. Patients receiving treatment for esophageal cancer can start chemotherapy, radiotherapy, or both, before or right after discharge in the hospital. Patients typically stay in a healthcare facility so long as fourteen days after surgery if no problems have taken place. Once the patient goes home, any remaining bandages should be clean and dry. Frequent walking and light exercise are invited. Because laparoscopic and thorascopic surgery is less invasive and makes use of only small incisions, there's less trauma towards the body, and activity could be resumed faster compared to open procedures that need larger incisions. The individual should report any chills or fever, persistent pain, or incision drainage towards the surgeon. The patient's diet will usually be limited for some time to soft foods and small portions; an ordinary diet could be resumed within per month, however with smaller amounts. Patients are advised to not drive when they are still taking prescribed narcotic pain medicines. Daily care and assistance in patient’s own home is suggested throughout the recuperation period. Regular health care and periodic diagnostic testing, for example endoscopic ultrasound, is important to watch the health of the esophagus and also to identify recurrence from the cancer or even the growth and development of new tumors.
Alternatives
Individuals with Barrett's esophagus may be treatable with treatments and dietary changes to lessen acid reflux disorder. These nonsurgical approaches work in relieving heartburn, calming inflamed tissues, and avoiding further cell changes. Fundoplication, or anti-reflux surgery, can improve the barrier to acid regurgitation once the lower esophageal sphincter doesn't work properly, curing GERD and lowering the exposure from the esophagus to excessive levels of acid. Photodynamic therapy (PDT) may be the injection of the cytotoxic drug along with laser light treatments, delivering advantages similar to more set up treatments. Endoscopic laser light treatments that deliver short, powerful lasers towards the tumor with an endoscope can increase swallowing difficulties; however, multiple remedies are needed and also the benefits are neither long-lasting nor proven to prevent cancer.






