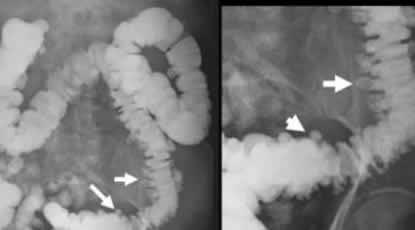
Diverticulosis
What's diverticulosis?
Diverticulosis is a symptom in which a patient will find small pouches or pockets within the wall or lining of any part of this enzymatic tract. Just one pouch is called a diverticulum. These pockets occur once the inner layer of the digestive system pushes through weak spots within the outer layer. The pouches associated with diverticulosis are generally located in the lower the main large intestine. Many people may have only several small pouches about the left side of the colon, while some might have participation in most of the colon.
What causes diverticulosis?
Because diverticulosis is uncommon in regions of the world where diets are high in fiber and rich in grains, vegetables and fruit, most physicians believe this problem is due in part to a diet low in fiber. A low-fiber diet leads to constipation, which increases pressure inside the digestive tract with straining during bowel movements. The combination of pressure and straining over many years likely leads to diverticulosis.
Who gets diverticulosis?
Diverticulosis affects half of all people over 60 years old and nearly everyone by the age of 80. As a person gets older, the pouches in the digestive system become more dominant. Diverticulosis is uncommon in people under 40 years of age. Additionally, it's rare in a few areas of the world, such as Asia and Africa.
What are the signs of diverticulosis?
Most people who've diverticulosis don’t know that they have the problem because it usually doesn't cause symptoms. It's possible that some people with diverticulosis encounter bloating, abdominal cramps or constipation due to trouble in stool passage with the involved area of the colon.
Are there complications from diverticulosis?
Diverticulosis may lead to several complications including inflammation, infection, bleeding or intestinal blockage. Fortunately, diverticulosis does not lead to cancer. Diverticulitis occurs when the pouches turn into infected or inflamed. This problem usually creates localized abdominal pain, tenderness to touch and fever. A person with diverticulitis may also experience nausea, vomiting, shaking, chills or constipation. Your doctor may order a CT scan to confirm an analysis of diverticulitis. Minor cases of infection are usually treated with oral antibiotics and do not require admission to the hospital. If left untreated, diverticulitis can lead to a collection of pus outside the colon wall or a generalized infection in the lining of the abdominal cavity, a condition known as peritonitis. Usually a CT scan is needed to diagnose an abscess, and treatment usually requires a hospital stay, antibiotics applied through a vein and possibly drainage from the abscess. Repeated attacks of diverticulitis may require surgery to get rid of the affected portion of the colon. Bleeding in the colon may occur from the diverticulum and it is called diverticular bleeding. This is actually the most common reason for major colonic bleeding in patients over 40 years old and it is usually noticed as passage of red or maroon blood through the rectum. Most diverticular bleeding stops on its own; however, if it doesn't, a colonoscopy may be required for evaluation. If bleeding is extreme or persists, a hospital stay is generally necessary to administer intravenous fluids or possibly blood transfusions. In addition, a colonoscopy may be necessary to determine the cause of bleeding and also to treat the bleeding. Occasionally, surgery or other procedures might be necessary to stop bleeding that cannot be stopped by other methods. Intestinal blockage may exist in the colon from repeated attacks of diverticulitis. In this instance, surgery might be essential to remove the involved part of the colon.
How's diagnosing of diverticulosis made?
Since most people don't have symptoms, diverticulosis is usually discovered incidentally during evaluation for another condition or throughout a screening exam for polyps. Gastroenterologists can directly visualize the diverticula in the colon during a procedure that uses a small camera attached to a lighted, bendable tube inserted through the rectum. One of these procedures is really a sigmoidoscopy, which uses a short tube to look at just the rectum minimizing part of the colon. A colonoscopy uses a longer tube to examine the whole colon. Diverticulosis can also be seen by other imaging tests, for instance, computed tomography (CT) scan or barium x-rays.
What is the treatment for diverticulosis?
Fortunately, most patients with diverticulosis don't have indications, and therefore don't need treatment. Once diverticula form, they don't vanish by themselves. When diverticulosis is accompanied by abdominal pain, bloating or constipation, patient’s Physician may suggest a high-fiber diet to make stools softer and easier to pass. Even though it is recommended that we consume 20 to 35 grams of fiber daily, many people only get about half that amount. The easiest way to improve fiber intake is to consume more fruits, vegetables or grains. Apples, pears, broccoli, carrots, squash, baked beans, kidney beans, and lima beans are several types of high-fiber foods. As an alternative, patient’s physician may recommend an additional fiber product such as psyllium, methylcellulose or polycarbophil. These products are available in various forms including pills, powders, and wafers. Additional fiber products help to bulk up and soften stool, making going number 2 simpler to pass. Patient’s physician may also prescribe medicines to assist relax spasms in the colon that create abdominal cramping or discomfort.






