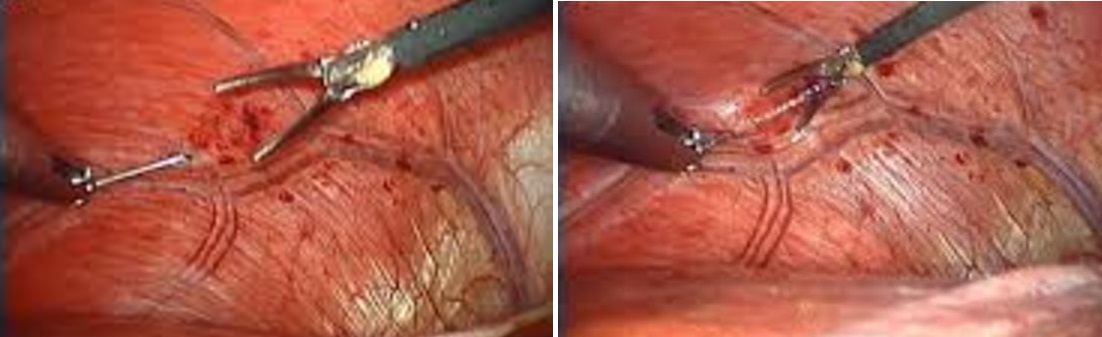
This laparoscopic newly evolved technique of electrical stimulation is utilized to treat morbid obesity, gastroparesis, and diaphragmatic paralysis.
Diaphragm Pacing: As these technologies carry on and evolve and alter the treatment of many different pathophysiologic processes, the typical surgeon needs to understand the technical elements of these products and their potential complications. The diaphragm pacing stimulation (DPS) system was built to exchange or delay the need for patients requiring long-term positive pressure mechanical ventilation via tracheostomies.
The first clinical indications for phrenic nerve or diaphragm pacing have been cervical spinal-cord injuries and congenital central hypoventilation syndromes (CCHS or Ondine curse). To the DPS device to be effective, the phrenic nerve must have the ability to provide conduction pathways to the muscle. Therefore, the low motor neurons inside the spinal cord along with the phrenic nerve needs to be intact. In case a phrenic nerve is completely severed or injured, the diaphragm should not be paced. The DPS procedure, which takes about 1.5 hours, is described in four phases: exposure and routing, implantation and mapping.
The exposure is made up of the setup for the typical four-port laparoscopy to visualize the diaphragm. Because these patients will not be paralyzed, the usage of preemptive local anesthetics from the skin and abdominal muscles on the planned trocar sites really helps to decrease abdominal muscle spasms. The original port is placed in the midline supraumbilical in order that adequate visualization in the diaphragm can be acquired; this can be a 5- or 10-mm port according to the laparoscope choice. The epigastric port is utilized for your diaphragm implant instrument. An additional grounding patch is placed on the sufferer and connected to the clinical station.
Gastric Pacing: Gastroparesis, considered delayed gastric emptying in the absence of mechanical obstruction, affects greater than 1.5 million Americans with approximately 100,000 struggling with a serious form. Causes for gastroparesis include idiopathic, diabetic, and post-foregut surgery. Patients present with nausea, vomiting, abdominal pain, bloating, early satiety, malnutrition, and weight-loss.
Treatment solutions for gastroparesis are limited and include medical therapy, operative therapy, and nutritional support. Even with a multidisciplinary approach, treatment is often challenging and medical therapy may only offer temporary or partial relief. In cases of severe disorder, nutritional support and a lot more aggressive medical therapy can be indicated. Invasive interventions are reserved for patients with severe disease, including nutritional deficiencies, refractory symptoms despite medical therapy, and frequent visits or hospitalizations.
Various ways of GES have been studied with all the most widely applied method being utilized the top-frequency short-pulse low-energy method. A number of studies show that it shortpulse GES demonstrates significant antiemetic effect but only modest improvement in gastric emptying. However, symptom improvement is not going to rely soly on improved gastric emptying, and the standard of living improvement with GES has been significant. It has been demonstrated in both a randomized, double-blind, placebo-controlled study as well as in a crossover study. In a publication by Forster, GES patients showed improvements in bmi, hemoglobin A1C levels, quality of life, and variety of hospital admissions. GES may be easily performed laparoscopically which is a comparatively safe treatment selection for patients with refractory gastroparesis that contributes to improvement in gastrointestinal and excellence of life symptoms and a decrease in drug therapy.
Standard laparoscopic access is conducted far from any previous or present feeding If necessary, an adhesiolysis, tubes and could be performed to determine the anterior gastric wall. All previous gastrostomies needs to be taken down, preferably having a stapler to diminish the opportunity of contamination. The liver is retracted cranially along with the stomach is marked 10- cm proximal to the pylorus about the greater curvature. The conducting end from the electrode is linked to a monofilament, which happens to be in turn attached to some straight needle. This needle is pushed tangentially throughout the muscular wall. The electrodes are secured towards the serosa in the stomach using silk sutures proximally as well as a plastic disc with two clips in the monofilament suture distally. Clips may also be used within the monofilament to keep the disk in position. A second electrode is implanted 1-cm parallel towards the first, electrode and secured to the gastric wall within a similar fashion. Excess wire must be wrapped around the neurostimulator, as well as the connector pins and leads should have bodily fluids Before they are connected, wiped off. The etched identification side should face outward and from muscle tissue to reduce the potential of skeletal muscle stimulation, which might be perceived by the individual as twitching or burning.
The external programmer device sets the gastric stimulator in the standard configuration and the electrode impedance and gastric wall conductance is tested to confirm correct placement of electrodes.
Complication: The categories of patients undergoing DPS implantation are in an inherent risk for problems because of the comorbidities with their disease process. ALS patients possess a terminal disease; the goal is usually to increase their quality of life by delaying their need for tracheostomy ventilation. Capnothorax, which occurs from intraabdominal air tracking towards the chest cavity in the needle being put into the thin diaphragm of such patients. This takes place approximately 50% of the time and could be managed by watchful waiting since the carbon dioxide is absorbed readily or easily aspirated by way of a thoracentesis catheter.
A general 3% wound infection rate is likely due to simultaneous gastrostomy tube placement. The laparoscopic implantation in the GES, historically was done in an open fashion, has not any significant reported rates of conversion to a laparotomy. The major postoperative complication as with all implantable foreign body is infection. This most commonly involves infection from the hardware, but case reports have described electrode erosion in the stomach, electrode dislodgment, electrode malposition, abdominal pain, and small bowel volvulus around the electrodes.
Conclusion: An elementary FES unit involves stimulating electrodes, an anode, a pulse generator, along with a programmer. The sorts of electrodes which can be implanted are variable. There are electrodes which are only employed to map or assess nerve function, electrodes that are placed near muscle motor points, or electrodes that happen to be placed in contact with nerves. Electrodes which are placed in contact with nerves are numerous times called cuff electrodes. Electrodes use a non-insulated area to transfer the electrical impulse on the target. The connecting lead between the exposed electrode as well as the pulse generator must have a minimal resistance and also be insulated, flexible, and capable of transferring current. According to where electrode needs to be placed, a proper implant instrument has to be used, such as the one employed for diaphragm pacing. All electrical systems need an anode, or ground electrode, that may be the If implanted, pulse generator. The pulse generator is amongst the key areas of functional electrical stimulation, commonly referred to in surgery since the “pacemaker” or “stimulator.” This has got the battery to store the charge as well as the hardware and software that allow it to be programmable to offer the stimulus with some other rates, amplitude and frequency and pulse width. if the pulse generator is implanted it is known as an IPG (implanted pulse generator). All pulse generators offer an external programmer that will permit the clinician to gauge the machine and program the stimulation parameters the patients will receive.






