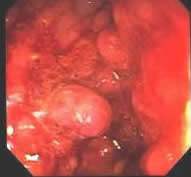
What is colonoscopy?
Colonoscopy lets a patient’s physician examine the liner of your large intestine for irregularities by inserting a thin flexible tube, as thick as like finger, into his/her anus and slowly advancing it into the rectum and colon. This instrument, called a colonoscope, has its own lens and lightweight source also it allows your physician to view pictures on the video monitor.
Exactly why is colonoscopy recommended?
Colonoscopy may be recommended like a screening test for colorectal cancer. It's been estimated that increased consciousness and screening would save a minimum of 30,000 lives every year. Colonoscopy can also be recommended by patient’s doctor to judge for symptoms for example bleeding and chronic diarrhea.
What preparations are needed?
A patient’s doctor will tell him/her what dietary restrictions to follow and what cleaning routine to use. In general, the preparation consists of restricting your diet to pay off liquids the day before and ingesting whether large amount of a unique cleansing solution or special oral laxatives. The colon must be completely clean for the procedure to be accurate and comprehensive, so be sure to follow your doctor’s instructions carefully.
Can a patient take current medications?
Most medications could be continued as usual, however, many medications can interfere with the preparation or the evaluation. Tell your doctor about medications you’re taking, particularly aspirin items, arthritis medications, anticoagulants, clopidogrel, insulin or iron items. Also, make sure to talk about allergies you have to medications.
What happens throughout colonoscopy?
Colonoscopy is well-tolerated and rarely causes much pain. You may feel stress, bloating or cramping pains throughout the procedure. Typically, your doctor provides you with a sedative or painkiller to help you relax and better withstand any distress. You will lie on your side or back while your physician slowly advances a colonoscope alongside your large intestine to look at the lining. Physician will examine the liner just as before because he or she slowly withdraws the colonoscope. The process itself typically takes under 45 minutes, although you should plan on two to three hours for waiting, preparation and recuperation. In some instances, the doctor cannot pass the colonoscope car colon to where it meets the little intestine. Physician will counsel a patient whether any additional testing is essential.
In case your doctor thinks a place needs further assessment, she or he might pass a musical instrument through the colonoscope to acquire a biopsy (a small sample from the colon lining) to be analyzed. Biopsies are utilized to determine many problems, and your physician will frequently have a biopsy even when he or she doesn’t suspect cancer. If colonoscopy is being performed to recognize sites of bleeding, your doctor might control the bleeding with the colonoscope by injecting medications or by cauterization or by utilization of small clips. Your physician might also find polyps in the course of colonoscopy, and he or she'll most likely take them off throughout the examination. These methods don’t generally result in any pain.
What exactly are polyps and why are they eliminated?
Polyps are abnormal growths within the colon lining which are usually benign. They vary in dimensions from the tiny dot to many inches. Your doctor can’t always tell a benign polyp from a malignant polyp by its outer look, so he or she will often remove polyps for analysis. Because cancer begins in polyps, removing them is a vital way of preventing colorectal cancer.
How are polyps removed?
Your doctor may damage tiny polyps by fulguration (burning) or by taking away them wire loops called snares or with biopsy instruments. Physician uses a technique known as “snare polypectomy” to get rid of larger polyps. Your doctor will pass a wire loop through the colonoscope and remove the polyp from the intestinal wall utilizing an electrical current. You need to feel pain free during them polypectomy.
What goes on following a colonoscopy?
You'll be monitored until most of the effects of the sedatives normally wear off. You might have some cramping pains or bloating because of the air released into the colon throughout the examination. This will vanish quickly when you pass gas. Your physician will show you the outcomes of the examination for you, although you’ll probably have to wait for the outcomes of any biopsies performed. If you have been given sedatives throughout the procedure, someone must drive you home and turn into with you. Even if you feel alert following the procedure, your common sense and reflexes could be impaired throughout your day. You should be able to eat after the evaluation, but your doctor might minimize your diet and activities, especially after polypectomy. Your doctor will counsel you about this.
hat are the possible difficulties of colonoscopy?
Colonoscopy and polypectomy are generally safe when performed by physicians who have been specially trained and therefore are experienced during these procedures. One possible complication is a perforation, or tear, with the bowel wall that could require surgery. Bleeding might occur at the site of biopsy or polypectomy, but it’s usually minor. Bleeding can stop by itself or perhaps be controlled through the colonoscope; it rarely requires follow-up treatment. Some patients might have a reaction to the sedatives or problems from heart or lung disease. Although difficulties after colonoscopy are uncommon, it’s vital that you recognize early signs of possible complications. Speak to your doctor if you see severe abdominal pain, fever and chills, or rectal bleeding. Observe that bleeding may appear several days after the procedure.






