Click Here to Use Our BMI Calculator
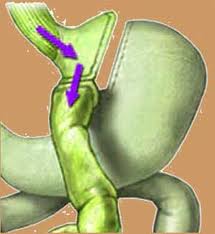
What is a Weight Loss Surgery?
Obesity has become more and more prevalent throughout the world and many men and women are considering bariatric surgery, also known as weight loss surgery, as a solution to their weight gain. Weight loss surgery may appear to be a simple answer to the obesity problems people have, but it is not something that can, or should, be entered into lightly. Not everyone will qualify for weight loss surgery. Patient should be at least 100 pounds overweight and Patient will have to undergo extensive tests, both physical and mental, in order to quality. Weight loss surgery was first discovered as a result of surgery on cancer and ulcer patients who had to have large parts of their stomachs or small intestines removed. It was noted that some of these patients lost weight after these surgeries. Over 40 years ago, doctors began performing these types of surgeries specifically for the purpose of weight loss. When we eat, our food travels down the approximately 20 feet of our small intestine, where most of the calories and nutrients from our food are absorbed. What isn't absorbed moves on to our large intestine and eventually gets eliminated.
The two forms of weight loss surgery are malabsorptive surgery, which restricts the absorption of nutrients that Patient's small intestine can absorb, and restrictive surgery, which reduces the size of Patient's stomach so Patient eat less. Some procedures do a combination of both types of surgery. Malabsorptive surgery changes where the small intestine connects to the stomach or shortens the length of the small intestine. This limits the amount of calories and nutrients that can be absorbed by the small intestine. Restrictive surgery changes the size of the stomach by banding part of it off or removing a section. Roux-en-Y gastric bypass surgery, also called gastroplasty, is a combination of both procedures. This procedure is very popular in America. Mainly popular in Europe, Biliopancreatic diversion (BPD) surgery, with or without a duodenal switch (BPD/DS), is a malabsorptive procedure. Another restrictive bariatric operation is the vertical sleeve gastrectory, which removes part of the stomach. By using one of the above methods of weight loss surgery, one will lose weight because the stomach will hold less, less calories and nutrients will be able to be absorbed, or a combination of both of these results.
Different Types of Weight Loss Surgeries Available and the One to Go For!
There are several different types of weight loss surgeries Patient can chose from. Gastric banding, which is a restrictive method; gastric bypass, which is a malabsorptive system; the Roux-en-Y Gastric Bypass, which is a combination of restrictive and malabsorptive procedures; the Biliopancreatic Diversion (BPD), or Scopinaro procedure, which is a "malabsorptive" operation, and can be performed alone or with a duodenal switch (DS); and Vertical Sleeve Gastrectomy, which is a restrictive bariatric operation. Gastric banding is a restrictive procedure, and the least intrusive of all the procedures. A silicone band encircles the upper part of the stomach leaving a small pocket above the band and the larger part of the stomach below. Between the two sections is a narrow channel for the food from the upper part to pass into the larger part. The upper part of the stomach only holds a small amount of food, thus a person feels satisfied with less. Also, the small channel slows down the passage of the food to the lower section, so the feeling of being full lasts longer. This procedure is performed by inserting long, slender instruments through 5 small slits in the skin and is called the laparoscope method. In a gastric bypass, a malabsorptive method, the available length of the small intestine is changed, either by being surgically reduced or by the stomach being reattached further down the small intestine. This reduces the amount of nutrients and calories that can be absorbed by the small intestine, thereby causing weight loss.
The most popular form of surgery in the United States is the Roux-en-Y gastric bypass system, also known as gastroplasty and is a combination of both malabsorptive and restrictive procedures. In the Roux-en-Y procedure, the stomach is reduced from being able to stretch to approximately 1000 ml to just 15-30 ml. Additionally, a significant length of the gastrointestinal tract is bypassed, reducing the amount of nutrients a person can absorb. Another malabsorptive procedure is the biliopancreatic diversion (BPD), also known as the Scopinaro procedure. The stomach in reduced, by having the left side of the stomach removed, so it can hold only about 2 to 3 cups of food. This reduced stomach is reattached after bypassing about 9 feet of the small intestine called the ileum. With the duodenal switch option chosen (DS), the lower part of the stomach is removed instead of the left side and the pylorus valve is not removed.
In Vertical Sleeve Gastrectomy, a restrictive method, 85 percent of the stomach is removed by dividing it vertically, leaving a thin banana shape that measures between 2-5 ounces. This procedure was originally for people who were morbidly obese or at a high risk due to health considerations, but today it is being performed more often for those who just want to lose weight. Many of these surgeries can be done with laparoscopy which uses long, slender instruments inserted through small incisions in the abdomen. If Patient feel that Patient are a candidate for weight loss surgery, Patient and Patient's physician can discuss which options are best for Patient's situation.
Gastric Bypass vs. Lap-Band Surgery
There are major differences between the two forms of weight loss surgery. Patient's doctor can help Patient decide which of the two, or if a combination of both, are better for Patient's situation. Here are some of the major differences: Gastric bypass surgery causes Patient to lose weight by malabsorption of the nutrients and calories Patient eat by reducing the size of Patient's stomach and bypassing a major portion of Patient's small intestine. Lap banding surgery causes Patient to lose weight because Patient's stomach is banded, divided into two sections, and the smaller, upper section can only hold a small amount of food. The narrow channel between the two sections of Patient's stomach also causes the food to pass slowly into the lower section, causing the feeling of fullness to last longer. The most common surgical method used for gastric bypass is major, open surgery, through an approximately 5" slit in the stomach. However, more and more doctors are gaining enough experience to now perform this procedure laparoscopally. A 3 - 5 day hospital stay is required. Lap banding surgery is performed laparoscopally using three to five 1/2"-2" slits and is the least invasive of the procedures. This surgery lasts about 1 hour and there is no cutting or reconnecting of the stomach or small intestine. An overnight stay in the hospital is usually all that is required and the patient can be released after 24 hours.
Gastric bypass surgery is not reversible but lap band surgery is reversible and adjustable as the situation warrants. The recovery period with gastric bypass surgery is a full six weeks. With lap band surgery, a person feels OK after two to three weeks and full recovery is obtained after six weeks. The weight loss result between the two procedures is approximately the same – 50-65% of the weight is lost during the first two years following the procedure. Because gastric bypass surgery restricts the nutrients and calories the body can absorb, it is very important to take supplements as prescribed by Patient's physician. Supplements after the lap band surgery aren't necessary, but are highly recommended. Gall stone formation can be a problem after a gastric bypass, but there is medication that can be prescribed to prevent this side effect. With lap band surgery it is very important to eat an adequate amount of protein, between 50-50 grams per day. Without adequate protein, hair loss, muscle cramps, fatigue and edema are some of the undesirable side effects that can occur. This is just a brief overview of the differences and similarities between the two methods of weight loss surgery. Other methods combine the two. Only Patient and Patient's doctor can decide which procedure, or combination of procedures, is right for Patient.
Laparoscopic Surgery for Weight Loss
Laparoscopic weight loss surgery is becoming more and more popular and is replacing open surgery as physicians become more experienced with the laparoscope procedure. During a laparoscope surgery, four to six incisions about 1/2" - 2" in length are cut in the abdomen. The surgeon passes a camera, a light and one surgical instrument, each about the diameter of a pencil, into the abdomen. After inflating the abdomen with carbon dioxide gas, so the surgeon can better see Patient's stomach and other internal structures, the surgery is performed. The NYU surgical weight loss program is now performing what they call "Single Incision Laparoscopic Surgeries", SILS, using a single slit through the belly button. The benefit of SILS is usually reduced scarring, better cosmetic results, faster recovery, and less pain. This latest advancement in weight loss surgery is the least invasive of all the surgeries and an important step forward for people needing weight loss surgery. The most common procedures performed for weight loss using the laparoscopic method are gastric bypass surgery, adjustable gastric band surgery, and sleeve gastrectomy, and a combination, such as the Roux-en-Y procedure.
In a gastric bypass procedure, part of the stomach is removed and reattached after bypassing a major portion of the small intestine. This results in less (malabsorption) of the calories and nutrients a person consumes, resulting in weight loss. For the gastric band surgery, a band is placed around the upper portion of the stomach limiting the amount of food someone can eat at one time. No nutrients or calories are lost. Roux-en-Y is a combination of gastric bypass and the band procedure where only a small part of the stomach, about the size of an egg, remains functional. The other portion is bypassed. Two-thirds of the stomach is removed during the sleeve gastrectomy procedure and a portion of the small intestine is bypassed. Some of the benefits of having Patient's procedure done laparoscopically are quick recovery with no complications; only 1 - 3 days in the hospital, and the ability to return to work after just two to four weeks. After Patient's surgery Patient will follow a strict eating regimen and for about one year, and Patient will need to make regular follow up visits to Patient's physician. If, after one or two years from Patient's surgery, Patient have a problem with folds of skin hanging around Patient's abdomen, Patient may want to consider abdominoplasty, a plastic surgery procedure
Do Patient Really Need to Go Under the Knife?
There are many factors to consider before Patient decide if weight loss surgery is right for Patient. To start with, Patient have to meet specific criteria in order to qualify for weight loss surgery. Some of the things Patient's doctor will consider are the following:
- Patient must be at least 100 pounds overweight. This can be reduced to 75 pounds if Patient have extreme weight related illnesses such as diabetes, serious sleep apnea, hypertension, or heart disease related to Patient's weight. This is because the risks of weight loss surgery are less than the risk of dying due to the illness.
- Patient's body mass index (BMI) should be 40 or greater. This puts a person in the morbidly obese category.
- Patient must have seriously tried to lose Patient's excess weight for at least five years or more, by a variety of methods, including diet and exercise.
- Patient must be totally committed, and motivated, to follow exactly the diet and exercise programs that go with the weight loss surgery Patient have.
Even if Patient meet the above guidelines, Patient's doctor may disqualify Patient from having the surgery. The characteristics that might cause Patient to be disqualified are:
- Severe psychiatric illnesses which are uncontrolled.
- Addiction to alcohol and/or drugs.
- If Patient have cancer and are not in remission.
- Most people over 65 can be disqualified, but this is not automatic.
- If Patient's expectations are unrealistic, Patient doctor may advise against Patient having weight loss surgery.
- If Patient are a woman and would like to become pregnant before a year after Patient's surgery.
Once Patient have decided to have weight loss surgery and Patient's doctor has approved, Patient will have many tests, including various lab test, an Upper Gastrointestinal test, an electrocardiogram, and psychiatric interviews and tests. Patient's doctor will want to be sure Patient understand precisely the diet, exercise, and medical rules Patient must follow for the rest of Patient's life. Having weight loss surgery is a big step. It would also benefit Patient to talk to other people who have had the surgery and look online for support groups and forums that discuss the surgery. Before Patient make the final decision, Patient must educate yourself on the different types of surgery and what will be required of Patient after Patient have the surgery. If Patient have a family, they must also understand the changes in Patient's life that will occur after the surgery.
Sleep Apnea Patients Beware!
Weight loss surgery has become safer and safer but there is still the risk that it could cause problems for people with a blood clot problem or sleep apnea. It is common for people who are obese or morbidly obese to have sleep apnea. Sleep apnea occurs when someone stops breathing while they are sleeping. A lot of fat around the neck contributes to sleep apnea and symptoms can be excess snoring and, during sleep, the upper airway collapses, sometimes several times a night. Sleep apnea then causes the sleeper to snort, gasping for breath. People prone to sleep apnea can also have higher incidents of hypertension, vascular changes, and a higher chance of heart disease. These are all factors that also lead to a higher surgical risk for weight loss surgery. Even taking these higher risks into consideration, some people with a high risk of death due to problems related to obesity are better off having the weight loss surgery than staying obese
Here are some recommendations to lower Patient's risks during and after weight loss surgery:
If Patient are at a higher risk, chose a lower-risk procedure such as gastric banding. The death rate for one recent study had a mortality rate of 2.1% for patients who had the open Roux-en-Y procedure; 0.2% for the laparoscopic Roux-en-Y procedure; and no deaths when the patients had the laparoscopic adjustable gastric banding procedure. If Patient can lose some weight before surgery and walk a little each day Patient will be at less risk. The more obese Patient are, the greater Patient's risk. The recommendation is to lose 10% of Patient's body weight before Patient's surgery and Patient will have a more speedy recovery. In order to lower the risk of blood clots, it is necessary to be able to walk around after Patient's surgery, so it is important to begin walking, even for five minutes each day, prior to Patient's surgery. Pay attention to the credentials of the staff and hospital where Patient will be having Patient's surgery. Not just the surgeons, but the non-physician health care providers, the anesthesiologist, the hospital's experience with weight loss surgery, and their equipment. The decision to have weight loss surgery is a very important and life-changing decision. Lower Patient's risk by educating yourself on all the steps Patient can take before Patient's surgery to ensure a successful outcome and a long, healthy life.
Things to do BEFORE Undergoing Weight Loss Surgery
Patient've made Patient's decision and Patient and Patient's physician agree that Patient are a candidate for weight loss surgery. Patient've found a surgeon and hospital Patient're comfortable with and Patient've undergone extensive tests, both physical and mental. Everything is OK.
What is next?
- Surround yourself with a strong support team. Read the website of the American Society of Bariatric Surgery. There Patient can educate yourself and Patient's support network about what will happen to Patient's body and the changes in Patient's lifestyle that will be necessary after Patient's surgery.
- Discuss Patient's decision openly with Patient's family and friends. Most will be supportive, but some may be concerned about Patient's safety and they need to have the benefits and risks explained to them so they understand. This is very important.
- Find a weight loss surgery support group or forum and get involved. Talk to other people who have had weight loss surgery. These people can be of great benefit to Patient after Patient's surgery. They know what Patient're going through.
- Realize that after Patient's weight loss surgery Patient will never be able to eat the same way Patient are eating now. This is very important to completely understand and agree with.
- If Patient doctor has given Patient any guidelines to follow before Patient's surgery, be sure to follow them to the letter. These are for Patient's benefit and to reduce the risks of any problems during and after the surgery.
- Stock Patient's kitchen with the things Patient will need for Patient's new way of eating. Get a list from Patient's health care provider and make sure Patient have everything Patient need ahead of time.
- Buy bags of ice to use in drinks and to sip on when Patient are thirsty but can't have a whole glass of water.
- Buy a food processor to prepare Patient's foods and a lot of small containers in which to freeze different dishes.
- Purchase any other equipment or items that will make Patient's post-op time easier. A seat for Patient's shower is nice as well as a comfortable robe to wear. One lady found sitting in her recliner, tilted back, helped her avoid any nausea.
Some common instructions to follow on the day of Patient's surgery:
- Don't eat or drink anything for the length of time specified by Patient's surgeon. If Patient have to take medications, take them with little sips of water.
- Relax. Patient've done all Patient could. Arrive at the hospital on time and begin Patient's new journey to health and slimness.
Things to do AFTER Undergoing Weight Loss Surgery
Patient've made it through Patient's surgery and are now back at home. Congratulate yourself on a long journey just completed and look forward to the lifetime journey Patient now face. One thing Patient will need is patience get used to Patient's new eating regime. Patient may get frustrated when Patient want to eat something that Patient can no longer eat. This is normal. Keep the phone numbers handy of Patient's support people and give one of them a call when Patient are having a rough time. Here are some general tips. They may differ from Patient's healthcare provider's guidelines, so make sure Patient follow the ones given to Patient:
- When Patient can eat solid food Patient must chew it well and eat slowly.
- Eat Patient's meal without drinking any liquids. They can make Patient feel nauseous or cause Patient to feel satisfied before Patient have eaten enough regular food.
- Don't eat sugary desserts.
- Avoid carbonated beverages. In some plans, Patient will never be able to drink carbonated beverages again.
- Stay away from alcohol.
- When Patient can return to work will be determined by the type of surgery Patient had. After a laparoscopic banding procedure Patient will probably be able to go to work and exercise after one to three weeks. If Patient have an open gastric bypass, Patient will need to allow yourself six weeks before Patient return to work.
- If Patient are planning to get pregnant, it's best to wait 16 to 24 months after Patient's surgery. This is for Patient's health as well as avoiding damage to Patient's unborn baby.
- If Patient have issues that need resolved after Patient's weight loss surgery, Patient can get therapy to help Patient get through this phase of Patient's recovery. Some people who had problems with emotional eating before their surgery have benefited greatly by getting therapy to help them understand their relationship with food and why they crave certain foods even when they are not hungry.
- Patient's weight loss surgery would eliminate Patient's hunger, but it won't eliminate Patient's emotional eating problems. It would be good to think about this seriously before Patient's surgery and make arrangements to get counseling after Patient have had Patient's surgery if it becomes a problem.
Conclusion
Weight loss surgery has improved the lives of many thousands of people, but it is not without its risks. Educating yourself on what weight loss surgery is all about is very important before Patient even consider such a step. Patient and Patient's doctor are the ones best able to decide if Patient are a good candidate for weight loss surgery. Patient's doctor can explain to Patient all the different types of options and help Patient decide which option is best for Patient. Weight loss surgery isn't something Patient can just jump into. It takes a long time from when Patient decide Patient would like to explore the possibilities of weight loss surgery to when Patient actually arrive at the hospital. Patient have a lot of time to change Patient's mind or explore other alternatives to weight loss surgery.