INTRODUCTION
“No disease from the human body, belonging to the domain from the surgeon, demands in its treatment, a better mixture of precise, anatomical knowledge along with surgical skill compared to hernia in most its variations.” - Sir Astley Paston Cooper, 1804. A safe as well as successful results of any surgical treatment is actually conditional upon the actual obvious knowledge of this surgical structure from the relevant region. The particular laparoscopic view from the groin anatomy is quite different.
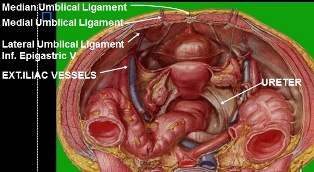
- The laparoscopic perspective is essentially a rear strategy view. Many surgeons are well experienced and also used to the anterior approach. Transforming to a laparoscopic approach requirements knowledge of the posterior technique.
- Certain structures that are obviously visible throughout the open approach (like the ilioinguinal neural, inguinal ligament, pubic tubercle and lacunar ligament) aren't as clearly visible with the laparoscope.
- Conversely structures that could require additional dissection during a open approach (for example Cooper’s ligament and the ilio-pubic tract) are clearly visible having a laparoscope.
- The laparoscopic observe is a ‘virtual view’ having a ‘2- dimensional’ handicap. You have the extra lack of tactile suggestions.
ANATOMY
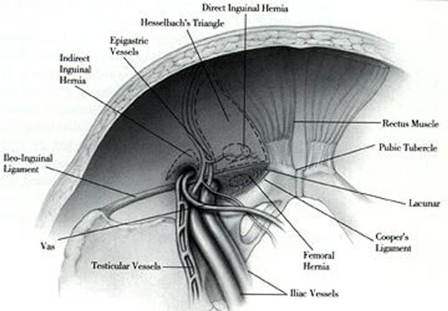
The particular groin has a unique practical amalgamated of musculo skeletal, visceral and neurovascular components, the group structures of which serves to maintain the dynamic physiological integrity of the region. Breakdown of the functional barrier brings about hernia. ‘Deep’ repair of inguinal hernia deals with the issue from the ‘point of origin’ rather than the ‘point of presentation’. This exercise has two important final results. Firstly, the ‘inlay/ posterior’ mesh placement provides a mechanical edge on the ‘onlay/ anterior’ mesh placement. Secondly covering the entire ‘Myopectineal orifice (of Fruchaud’) the ‘deep’ repair handles all the potential sites in danger
THE ‘MYOPECTINEAL ORIFICE OF FRUCHAUD’
In 1956, Henry Fruchaud espoused the theory that all groin (inguinofemoral) hernia originate in a single weak area called the Myopectineal orifice. This oval, funnellike, ‘potential’ orifice formed by the following structures, forms the ‘Myopectineal orifice of Fruchaud’.
- Superiorly Internal oblique and transverses abdominis muscles.
- Inferiorly Superior pubic ramus.
- Medially Rectus muscle sheath.
- Laterally Iliopsoas muscle.
Weakness through this area leads to inguinofemoral hernia. Proper exposure of the area is essential during a preperitoneal (posterior) repair!
- To avoid missing small hernia in addition to
- To achieve adequate fixation.
The orifice is divided through the Iliopubic tract and the inguinal ligament into an ‘inguinal’ defect and a ‘femoral defect’.
THE PERITONEAL LANDMARKS
Since the growth and development of the laparoscopic method for treating groin hernia an increased attention is being paid to ‘pure anatomy’ issues such as the infraumbilical fossae. These types of fossae havetwo important roles-
- The fossae delineate the websites of groin herniation.
- They are an essential landmark for orientation during hernia repairs.
The fossae are created by the presence of peritoneal folds, which radiate from the umbilicus or umbilical area.
Median Umbilical Ligament
This ligament ascends within the median plane in the apex of the bladder towards the umbilicus. It represents the obliterated allantoic duct and its lower part may be the site from the unusual urachal cyst.
Medial Umbilical Ligament
This ligament symbolizes the obliterated umbilical artery on both sides and can be traced down to the internal iliac artery.
Lateral Umbilical Ligament
It's the ridge of peritoneum, which is raised by the Inferior Epigastric artery and its companion two veins because they course around the medial border from the internal inguinal ring after which pass upwards into the posterior rectus sheath.
These ligaments delineate the next fossae
- Supravesical fossae: The infra-umbilical area between the median and medial umbilical structures. This is actually the site for that source of the supravesical hernia.
- Medial Umbilical fossae: The infra-umbilical area between the medial and lateral umbilical ligaments. This is the site for the ori- gin of the femoral and direct inguinal hernia.
- Lateral Umbilical fossae: The infra-umbilical area horizontal towards the lateral umbilical ligament. This is actually the site for the origins of the indirect inguinal hernia.
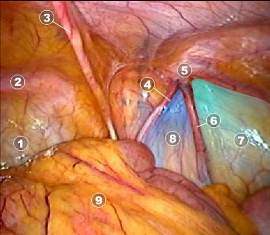
1= Bladder
2= Cooper Ligament
3= Medial Umbilical Ligament
4= Vas Defference
5= Deep Ring
6= Spermatic Vessels
7= Triangle of Pain
8= Triangle of Doom
THE THREE DANGEROUS AREA
Hesselbach’s (Inguinal) Triangle
Franz Caspar Hesselbach’s (1759-1816) original descriptions from the inguinal triangle were as follows:
- Superolateral boundary Inferior Epigastric vessels
- Medially Rectus sheath
- Medially Rectus muscle sheath.
- Inferiorly Cooper’s ligament (Inguinal
ligament in subsequent modification, to assist an ‘anterior’ approach surgeon.)
THE PREPERITONEAL SPACE
Understanding of the preperitoneal space and its extensions is vital to the laparoscopic surgeon. Value of the preperitoneal space is based on the truth that all posterior approaches for that repair of groin hernia have to traverse this area and work in it.
Embryology
The genesis of the preperitoneal space happens in concert with the global development of the abdominal walls.
Transversalis Fascia (of Gallaudet)
The current knowledge of the preperitoneal (properitoneal / extraperitoneal / pareito-peritoneal) space is tangled up intrinsically with the anatomy from the transversalis fascia in the infra-umbilical region. The present knowledge of the transversalis fascia envisages this fascia like a two layered (bilaminar) construction (confirmed through the laparoscope). Superiorly, both layers from the transversalis fascia are two distinct entities and inferiorly they insert onto the Cooper’s ligament. The anterior layer is adherent to the rectus abdominis muscle. The posterior layer is based on between your anterior coating and also the peritoneum. It divides that space into a anterior (vascular space) and a posterior (Space associated with Bogros). That old idea envisaged the transversalis fascia to be individual layered (unilaminar). The transversalis fascia is now not really believed to supply the kind of significant strength and integrity to the groin as earlier believed. Most importantly, it bridges the space between your transverses abdominis arch superiorly and also the inguinal ligament and the Cooper’s ligament inferiorly. The following crucial region is the “Achille’s heel” of the groin! It's right here which direct inguinal herniation happens. Condensations from the transversalis arch form three (3) named structures in this area.
Interfoveolar Ligament
This condensation of the transversalis fascia, whose fibresare oriented in a vertical direction compared to the rest of the fascia, forms the medial margin of the internal inguinal ring. It has no significant strength.
Iliopubic Tract
The Iliopubic tract is really a thickened lateral extension from the transversalis fascia, that runs from the superior pubic ramus to the iliopectineal arch and the anterior superior iliac spine. The iliopubic tract is distinct from the inguinal ligament, although intimately associated with the inguinal ligament with which it is often confused! It is anterior to the Cooper’s ligament and posterior to the inguinal ligament. The iliopubic tract separates the interior ring in the femoral canal. It's visualized as a fibrous (white) tract. It varies in constancy! In just 28% of (open) groin hernia repairs was it found to be above average in density and formed a very strong aponeurotic band. Its significance within the laparoscopic hernia repair is based on the fact that it forms the superior boundary for that ‘Triangle of Pain’, by which lie the nerves from the ilioinguinal region, which are in danger of injury/ entrapment if anchoring of the mesh is performed below the iliopubic tract! Therefore: Laterally, staples or tackers should not be placed below the level of the iliopubic
Iliopectineal Arch
This can be a thickened, tough, fascial structure since the iliac muscle arches in the anterior superior iliac spine inferiorly to the Iliopubic eminence. It gives origin to a portion of the internal oblique and transversus abdominis muscle as well as the inguinal ligament. It's an important structure as it is a vital supporting structure of the lateral groin!
Boundaries of the preperitoneal space
Anteriorly - Anterior layer of the transversalis fascia Posteriorly - The peritoneum.
Laparoscopic surgeon should are employed in the preperitoneal space ie. In the posterior space of Bogros to avoid unnecessary oozing.
Space of Bogros
This ‘preperitoneal space’ is split into two by the posterior lamina from the transversalis fascia. The posterior compartment continues to be now termed as the ‘Space of Bogros (proper)’, described by French anatomist Bogros in 1923. The anterior space has been referred to as the ‘Vascular Space’. In some places the posterior lamina is deficient, there the peritoneum adheres towards the anterior lamina. Medially it's continuous with the space of Retzius.
Prevesical space of Retzius
The preperitoneal space that lies deep to the supravesical fossa and also the medial umbilical fossa may be the Prevesical space of Retzius (described in 1858, by Swedish anatomist Retzius). This space contains loose connective tissue and fat. Dissection of the space during a laparoscopic hernia repair is mandatory to enable proper mesh overlap from the hernial defect to aid in proper mesh placement/ fixation. Important vascular structures on this space are:
- Normal and aberrant obturator vessels
- Accessory pudendal vessels (10%)
Contents (preperitoneal space)
The preperitoneal area is loaded with a variable amount of connective tissue, fat, vessels, nerves and various viscera. The contents are listed below.
VESSELS IN THE INGUINAL REGION
There are numerous blood vessels coursing the inguinal region and also the surgeon needs to be acquainted with these phones prevent iatrogenic injury and potentially devastating complications. Care has to be paid also to some minor vessels whose importance should not be underestimated. The following explanation provides the important information on the vessels in this area.
THE EXTERNAL ILIAC VESSELS
The particular exterior iliac artery and vein lie on the medial facet of the psoas muscle and also course deep to the Iliopubic tract to form the femoral vessels.
External Iliac Artery
This artery gives off two branches within its distal two cm:
- Laterally - It gives off the Deep Circumflex Iliac artery, which courses along the iliacus muscle, deep towards the Iliopubic tract, putting it in danger of injury during suturing or stapling. It then perforates the transverses abdominis muscle and ascends between your internal oblique and transversus muscles and supplies blood to both muscles. Here they complete an anastomotic circle by joining the iliolumbar and superior gluteal vessels.
- Medially - It emits the Inferior Epigastric artery. Near its takeoff the Inferior Epigastric artery emits two branche.
Cremasteric branch
This vessel penetrates the transversalis fascia and joins the spermatic cord.
Pubic branches
The anastomotic pubic branches course in a vertical fashion inferiorly, crossing the Cooper’s ligament and anastomosing with the obturator artery in the obturator foramen. The Inferior Epigastric artery also brings about anterior pubic artery, which associated with the Iliopubic vein crosses the superior pubic ramus. In 25-30% (some studies mention as high as 70-80%) of people, the anterior pubic branch is large and can replace the obturator artery (Obturator artery originating from the Hypogastric artery is missing). This large arterial branch (Aberrant obturator artery) can partially encircle the neck of a hernia sac and become injured in a femoral hernia repair. It might be also injured while exposing the Cooper’s ligament by freeing it of areolar-adipose connective tissue. Due to this possibility the whole anastomotic ring has previously been the - ‘Corona Mortis.” The Inferior Epigastric artery ascends to anastomose with branches from the Superior Epigastric artery.
External Iliac Vein
The vein is medial and posterior to the artery. This gets comparable tributaries. The actual Inferior Epigastric vein is paired, however, and joins the external iliac vein about 1cm proximal to the takeoff from the Inferior Epigastric artery and it is thus predisposed to injury. The Inferior Epigastric vessels cross over the Iliopubic tract in the medial facet of the interior ring and ascend across the posterior top of the rectus muscles, invested in a fold of peritoneum known as the lateral umbilical ligament.
Testicular Vessels
These vessels arise from the aorta just beneath the renal arteries at L2 level. These stick to the ureter caudally on its lateral border after which course along the lateral edge of the external iliac artery, cross the Iliopubic tract and join the spermatic cord in the lateral facet of the interior ring. Anastomoses between your testicular, differential and cremasteric arteries give you the testicle with rich collateral circulation. The pampiniform plexus drains into testicular veins. This testicular veins drain to the inferior cava about the right and also the renal vein about the left.
Deferential vessels
The deferential artery comes from the inferior vesicle artery, forming a microvascular network with the adventitia from the vas deferens. The deferential veins drain into the pampiniform plexus and vesical plexus.
Deep venous circulation from the preperitoneal space
The venous circle/ deep venous circulation of Bendavid is located at the subinguinal space of Bogros. It is a network of deep inferior epigastric, rectusial, suprapubic and retropubic veins. A familiarity with these relatively underestimated vessels is important for surgeons employed in the preperitoneal space! The reason being damage to these vessels is easy in most cases results in haematoma formation.
Iliopubic Vein
This vein courses deeply to the Iliopubic tract and accompanies the anterior pubic branch when this is present. It either empties straight into the Inferior Epigastric vein or joins the venous anastomotic pubic department to create a typical trunk which drains into the Inferior Epigastric vein.
Rectusial Vein (Bendavid)
This vein runs along or is embedded inside the lower lateral fibres of the rectus muscle. It forms (Bendavid) consistently a venous anastomotic ring by joining the Iliopubic vein above the pubic crest.
Retropubic Vein
This vein, a small collateral branch of the anastomotic pubic vein is commonly observed on the lower posterior facet of the pubic ramus, underneath the Cooper pectineal ligament.
NERVES IN THE INGUINAL REGION
The key nerves in the groin region are the ilioinguinal, genitofemoral, lateral femoral cutaneous nerve and the femoral nerve. These nerves arise from the lumbar plexus, innervate the abdominal musculature and supply sensation for that skin and parietal peritoneum. Entrapment causes severe pain, whereas transection leads to numbness. These nerves are variably visualized during laparoscopic hernia repair. Therefore, the surgeon must rely on understanding of their normal anatomy and a ‘sixth sense’ to avoid injury. They are doing exhibit significant variation within their course!
The following three (3) nerves are at risk for injury at laparoscopic hernia repair-
- Lateral Femoral Cutaneous Nerve
- Femoral Branch from the Genito-Femoral Nerve
- Intermediate Cutaneous Branch of the Anterior Branch of the Femoral Nerve
The next three (3) nerves are usually not in danger at laparoscopic hernia repair but could be injured if excessive pressure is applied during mesh fixation, compressing the muscles enough to permit the staples to reach the nerve. It is interesting to notice that conversely the below three nerves are in most risk in open hernia repairs.
- Ilioinguinal Nerve
- Iliohypogastric Nerve
- Genital Branch of Genito-femoral nerve
Communication between your Genito-femoral nerve and Ilioinguinal nerve is typical. This leads to overlap of sensory innervation, which can cause difficulties in diagnosing which nerve is involved in the complication.
LATERAL FEMORAL CUTANEOUS NERVE
This nerve is the most commonly injured nerve during laparoscopic hernia repair. Injury of this nerve may be normal with inexperienced surgeons performing laparoscopic hernia repair.
Course
It arises from L2-3, emerges in the lateral fringe of the psoas muscle, courses along the iliac fossa, lateral towards the iliac vessels. It passes below or with the inguinal ligament, where it lies free in a fibrous tunnel 1cm to the medial side of the anterior-superior iliac spine. Broin et al detailed its course in cadavers and found it was a mean distance of 6.6 cms from the Inferior Epigastric vessels and 5.6 cms in the Internal Inguinal ring as it passes below the Iliopubic Tract.
Section of sensory supply to the upper lateral thigh. Common Site of damage is to prevent nerve injury during, dissection and stapling ought to be over the Iliopubic Tract.
Post-Injury Pain
Injury results in pain and numbness within the higher lateral thigh and is called ‘Meralgia Paraesthetica’.
Sensory Changes
Injury results in pain and numbness within the upper lateral thigh and it is known as ‘Meralgia Paraesthetica’.
GENITOFEMORAL NERVE
The actual femoral department of the genito-femoral neural reaches risk of harm during laparoscopic hernia repair. Problems for the genital branch of the genito-femoral nerve occurs only if excessive pressure is applied during mesh fixation, compressing the muscles enough to permit the staples to reach the nerve. Injuries may also happen to the genital department of the genitor-femoral nerve through manouvres to reduce the sac of an indirect hernia.
Area of provide
Genital branch supplies the
- Cremaster
- Spermatic fascia and tunica vaginalis from the testis.
- In the feminine, this kind of branch ought to be preserved because it is sensory towards the labium majora.
- It is the efferent branch for the cremasteric reflex. Femoral department is the cutaneous department to
- The skin over the femoral triangle (Anteromedial thigh).
- It may be the afferent department for that cremasteric reflex.
Common site of entrapment is posterior abdominal wall, femoral or inguinal region.
- Post-injury pain
- Groin, scrotum and also upper thigh.
- Sensory changes
- Hyperalgesia.
- Point tenderness
- Internal inguinal ring.
- Along Inguinal canal.
Hip joint movement
- Hyperextension or external rotation of hip increases pain.
- Walking exacerbates this.
Motor signs
- Reduction of cremasteric reflex.
- Ejaculatory dysfunction.
FEMORAL NERVE
The intermediate cutaneous branch from the anterior branch from the femoral nerve is at danger during laparoscopic hernia repair. Injury to the femoral nerve has also been described in literature.
Course
The femoral nerve comes from L2-4, emerges from the lateral aspect of the psoas muscle and travels beneath the inguinal ligament, lateral towards the femoral artery (outside the femoral sheath), to split into sensory and motor branches.
Section of supply
Supplies the area round the medial and intermediate facets of top of the thigh. Motor supply is to the quadriceps.
Common site of damage
Posterior abdominal walls posterior towards the inguinal ligament.
Post-injury pain
Within the groin, anterior and medial thigh.
Sensory changes
- Hyperalgesia or dysthesia.
- Point tenderness
- Hip joint movement
- Minimal hip extension increases pain.
Motor signs
Quadriceps muscle weakness as well as atrophy and also loss of patellar reflex.
ILIOINGUINAL NERVE
Entrapment of the Ilioinguinal nerve is unusual during Laparoscopic hernia repair and only is entrapped / harmed if excessive pressure is utilized throughout mesh fixation, compressing the muscles enough to allow the staples to reach the nerve.
Course
This nerve has a smaller footprint than the Iliohypogastric nerve. It comes from L1. It courses retroperitoneally over the quadratus lumborum behind the kidney after which passes anterior to the upper the main iliacus muscle. It then pierces the transverses abdominis near the anterior end of the iliac crest. After that it pierces the interior oblique, moves with the inguinal canal in front of the spermatic cord as well as leaves through the superficial inguinal ring or even the surrounding external oblique aponeuorosis.
Section of supply
Supplies the
- Skin at the root of the penis.
- Anterior third from the scrotum (males).
- A little area of thigh below the inside end from the inguinal ligament.
- Labia majora (females).
- Motor supply to the abdominal musculature.
Common site of entrapment
Common site of entrapment/ injury is medial towards the anterior superior iliac spine. [Is only entrapped/ injured if excessive pressure is applied during mesh fixation, compressing the muscles enough to permit the staples to reach the nerve.]
Post-injury pain
Injury causes pain and burning (paraesthesia) within the lower abdomen (area mentioned in ‘Area of supply’.)
Sensory changes
Hypoalgesia or hyperalgesia.
Point tenderness
- Medial to anterior iliac spine.
- Anterior abdomen.
Hip joint movement
- Limitation of internal rotation.
- Extension of hip increases pain.
Motor Signs
Abdominal muscle weakness.
ILIOIGHYPOGASTRIC NERVE
Entrapment of the Ilioihypogastric nerve is unusual during Laparoscopic hernia repair and only is entrapped/injured if excessive pressure is applied during mesh fixation, compressing the muscles enough to permit the staples to achieve the nerve.
Course
It arises from T12 and L1. It emerges in the lateral edge of the psoas muscles and crosses before quadrates lumborum behind the low pole of the kidney. This perforates the transverses abdominis above this iliac crest and gives off a lateral cutaneous branch. The main nerve then pierces the interior oblique straight away above and in front from the anterior superior iliac spine. After that it runs deep to the external oblique, just better than the inguinal canal. After that it penetrates the external oblique muscles within 1-2 cms from the superomedial facet of the external ring.
Area of supply
- It supplies the skin within the suprapubic region with sensory fibres.
- The lateral cutaneous department materials the skin within the posterolateral gluteal region.
- It also provides the afferent and efferent path- ways for the abdominal reflex whereby stroking the skin within the suprapubic area produces contraction from the rectus abdominis musculature.
Common site of entrapment
Typical site of entrapment/ injury is medial towards the anterior excellent iliac spine. [Is just entrapped/ hurt if excessive pressure is utilized during mesh fixation, compressing the muscles sufficient to permit the staples to reach the nerve.]
Post-injury pain
- Injury causes pain and burning up (paraesthesia) in the exact same area.
- Sensory alterations
- Hypoalgesia or hyperalgesia.
Endoscopic Anatomy of Defects
Point tenderness
- Medial to anterior iliac spine.
- Suprapubic area.
Motor signs
Weakness from the lower abdominal wall
APPLIED ANATOMY
ANATOMICAL LANDMARKS
Anatomical attractions really are a surgeon’s guideposts. A procedure, where the actual surgeon can't locate the appropriate anatomical attractions, renders the procedure unsafe mand condemned to some poor outcome. In the following explanation, the surgical anatomy is referred to in the viewpoint of a surgeon carrying out a TAPP (Trans-Abdominal Pre-Peritoneal) groin hernia repair. However, all of the structures and entities described here are also visualized inside a TEP procedure. Thus, the incumbent surgeon is mandated by need, to know and understand the below described structures! Your reader is reminded that within the performance of the TEP (Total Extra Peritoneal) groin hernia repair,the first balloon dissection happens in just Bogros medially last but not least medio-inferiorly near the pubic symphisis. Thus all the below described structures (Phase I) will appear with no ‘initial’ benefit of the peritoneum covering them. Blunt dissection within the area of Bogros initially reveals areaolar / fattyareolar tissue with relatively minimal vascularity. The pubic symphisis is visualized like a white bony framework.
LANDMARKS FOR TRANSABDOMINAL PREPERITONEAL HERNIA REPAIR (TAPP)
PHASE - I
Inguinal Anatomy with the peritoneum intact
Using the introduction from the laparoscope into the abdomen, 5 (five) important landmarks will have to be identified within the infra-umbilical region!
- Inferior Epigastric vessels
- Medial Umbilical Ligament
- Spermatic vessels
- Vas Deferens
- Trapezoid of Disaster
- Inferior Epigastric vessels
The Inferior Epigastric artery is prominently visualized during laparoscopic preperitoneal dissection of groin hernia.
Implication
- It forms the lateral border of the Hasselbach’s triangle.
- Identifying these vessels differentiates between indirect and direct inguinal hernia.
- Bleeding from an ‘injured’ Inferior Epigastric artery can be quite brisk.
Identification
- A little calibre vessel, it arises proximal towards the inguinal ligament from the external iliac artery, ascends in a medial path on the anterior stomach walls towards the lateral border of the ipsilateral rectus muscle, running between your two lamellae of the transversalis fascia.
Visualisation - The artery is most prominent near to its origin in the external iliac artery at the medial margin from the internal ring. Fat may obscure these vessels in obese patients.
- Medial umbilical ligament (Obliterated Umbilical Artery)
Implication
- Can be mistaken with the inferior epigastric artery!
- DO NOT dissect medial to it throughout a TAPP procedure! Medial dissection to the medial umbilical ligament would put the urinary bladder in danger to injury.
Identification
- It courses from the Internal iliac artery since it's last branch for the umbilicus.
- It becomes apparent midway between the internal ring and Cooper’s ligament.
Visualisation
- It is made apparent by its mesentery.
- It could be differentiated in the inferior epigastric artery by its course toward the umbilical trocar, whereas the inferior epigastric vessels are targeted at the lateral border of the rectus.
- Spermatic vessels
Implication
- Forms the lateral border of the ‘triangle of doom’ and the medial border of the ‘triangle of pain’.
Identification
- The testicular artery and vein descend caudally in the retroperitoneum and go into the internal ring on its posterior aspect from a craniad direction.
- They travel directly over or slightly lateral towards the external iliac artery and vein and therefore are accompanied by the vas deferens before entering the ring.
Visualisation
- Easily visualized as they are covered only by peritoneum.
- Vas deferens
Implication
- Forms the medial border of the ‘triangle of doom’ and ‘quadrangle of disaster’.
Identification
- From the interior ring, it may be tracked medially since it figure within the pelvic brim to vanish behind the bladder.
- It joins the testicular vessels before entering the internal ring from a substandard and medial direction.
Visualisation
- Easily visualized as it is covered only by peritoneum.
- ‘Trapezoid of Disaster’ (Labeled by Seid)
Implication
Lying beneath the peritoneum and transversalis fascia (within this triangle) would be the external iliac artery and vein and may be damaged with serious consequences! No dissection should happen in this region! No staples should be placed in this area!
Identification
It is formed through the meeting from the vas deferens and the testicular vessels at the internal ring, which forms the apex of the triangle.
Visualisation
- Easily identifi ed and visualized since the vas deferens and the testicular vessels are covered only by peritoneum.
- ‘Triangle of pain’
Implication
- It explains the area where the femoral department from the genitofemoral nerve, the horizontal femoral cutaneous neural and femoral nerve lie.
- If a operating specialist uses staples, he must stay away from it in this region!
Identification
- It is bound inferomedially through the gonadal vessels and superolaterally through the iliopubic tract.
Visualisation - The ‘triangle’ is easily distinguished as it’s borders are acknowledged easily. (The iliopubic tract is more readily recognized after the peritoneal flaps are elevated.)
PHASE - II
Inguinal anatomy with the peritoneum incised
After the peritoneum is dissected apart, 4 (four) further structures have to be identified. They are:
- Internal Inguinal/ Spermatic ring
- Iliopubic tract
- Cooper’s ligament
- Femoral Canal
- Internal Inguinal / Spermatic ring
Implication
- Denotes the website of origin of an indirect inguinal hernia.
Identification
- The most dependable indicator from the internal ring is the junction of the testicular vessels and also the spermatic cord.
- The inferior border is bound through the iliopubic tract.
Visualisation
- The appearance of the ring varies depending on the hernia defect.
- Sometimes the ring is created prominent by the pneumoperitoneum.
- Iliopubic tract
This Iliopubic system is thickened lateral extension from the transversalis fascia, which runs in the exceptional pubic ramus to the iliopectineal arch and the anterior exceptional iliac spine.
Implication
- The iliopubic tract divides the internal ring from the femoral canal.
- The iliopubic tract is distinct from the inguinalligament, although intimately linked to the inguinal ligament along with that it is often puzzled!
- Laterally, staples/ tacks should not be positioned below the level of the iliopubic tract!
Identification
- It originates laterally from the iliopectineal fascia and the anterosuperior iliac spine and inserts to the superior pubic ramus lateral and superior to the Cooper’s ligament.
- It is anterior to the Cooper’s ligament and posterior towards the inguinal ligament.
Visualisation
- It is visualized as a fibrous (white) tract.
- Cooper’s ligament
This ligament is really a condensation from the transversalis fascia and also periosteum located lateral towards the pubic symphisis. It's a number of millimeters thick, densely adherent towards the pubic ramus and joins the Iliopubic tract and lacunar ligaments at their medial insertions.
Implication
- This ligament is used to anchor the mesh initially.
Identification
- It takes a curvilinear course medial and inferior to the insertion of the iliopubic tract to create the prominence from the pelvic brim anteriorly.
- The Cooper’s ligament can readily be palpated like a thick, strong fibrous band and is shiny when freed from surrounding fat and soft tissue.
- It is visualized as a fibrous (white) curvilinear structure.
Visualisation
- The Cooper’s ligament is instantly visible when adipose tissue doesn't pay for it.
- Otherwise, visualisation needs so that it is freed of surrounding adipose tissue.
Mobilising adipose tissue around the Cooper’s ligament can injure an aberrant obturator artery, that might course over it. Problems for this vessel leads to distressing bleeding. This unfortunate morbidity has led to the naming of this vessel as - ‘Crown of Death’/ ‘Corona Mortis’.
CORONA MORTIS The pubic branch from the Inferior Epigastric artery courses in a vertical style inferiorly, crossing the Cooper’s ligament and anastomosing using the obturator artery. In 25-30% of people (is often as high as 70-80%), the pubic branch is big and can replace the obturator artery. This large arterial branch (Aberrant obturator artery) can partially encircle the neck of a hernia sac and be injured in a femoral hernia repair. It might also be injured while exposing the Cooper’s ligament by clearing it of areolar-adipose ligament. Due to this chance an enlarged pubic branch from the Inferior Epigastric artery has previously been known as the - ‘Corona Mortis’. The danger of damage in this region is much more important for obturator veins.
6. Femoral canal
Implication
- It denotes the possibility site of origin of the femoral hernia.
Identification
- The canal lies posterior to the iliopubic tract. The anterior border is formed by the inguinal ligament, the medial border through the lacunar ligament, the posterior border through the pectineal ligament and also the lateral border through the femoral vein.
Visualisation
- It is a potential space (in the absence of a femoral hernia).
TECHNICAL ISSUES
Issues Relating to Exposure
- Any hernia over the iliopubic tract is definitely an inguinal hernia and something below is a femoral hernia.
- The inferior epigastric artery should be accurately differentiated from the obliterated umbilical artery to assist distinguish immediate through indirect inguinal hernia.
- The dissection ought to reveal the following structures-
- Cooper’s ligament
- Iliopubic tract
- Testicular vessels
- Internal ring
- Spermatic cord
- Musculo-aponeurotic transverses abdominis arch.
The preperitoneal tissue should be completely elevated across the peritoneum to achieve the right plane (Space of Bogros). Dissection outside this kind of space leads to bleeding
Issues Associated with Dissection
- Dissection in the Trapezoid of Disaster’ should be avoided
- While dissecting around Cooper’s ligament, take care to avoid problems for the divisions from the obtu- rator vein.
Issues Associated with Fixation of Mesh
- Staples or sutures should not be placed lateral to the cord or below the iliopubic tract (Trapezoid of Disaster) to avoid injury to the branches from the genitofemoral nerve and also the lateral femoral cutaneous nerve.
- Staples shouldn't be placed lateral towards the inter- nal ring within the endopelvic fascia to avoid injury to the ilioinguinal nerve.
- Cooper’s ligament should be properly uncovered as the initial fixation is conducted to this structure.






