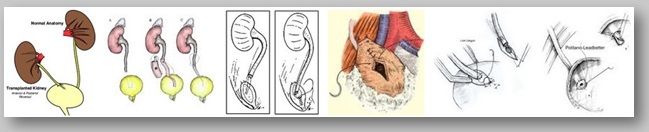
Introduction
Ureteroneocystostomy (UNC) or Laparoscopic ureteral reimplantation refers to reimplantation of the ureter into the bladder. In the adult population, ureteroneocystostomy is primarily acclimated for disease or trauma involving the lower third allocation of the ureter that after-effects in obstruction or fistula. In children, ureteroneocystostomy it is frequently acclimated for surgical analysis of vesicoureteral reflux (VUR).
Laparoscopic ureteral reimplantation:
The events of ureteral injuries have been on the rise. Regretfully, the moost of this increase can be attributed to the development of ureteroscopic techniques and complex pelvic laparoscopy. Although some shorter ureteral strictures can be managed via an endoscopic approach, success rates suffer when longer strictures are treated. Thus, these strictures are traditionally managed with open laparotomy, which is usually associated with a significant hospital stay and convalescence. Several investigators have described laparoscopic ureteral reimplantation as a minimally invasive alternative to the open approach with comparable short-term success rates.
Technique and outcomes:
There has been an explanation of initial series of 6 patients who underwent laparoscopic ureteral reimplantation (LUR). This minimally invasive technique allows for treatment of long strictures of the distal ureter, without the need for complex reconstructive maneuvers.
Operative Technique of Ureteroneocystostomy:
Following induction of anesthesia and the administration of intravenous prophylactic antibiotics, the patient is positioned in the modified lateral position. It is important that the genitalia are prepared into the operative field in case cystoscopy is required to aide in ureteral stent placement. An infraumbilical incision is made, and the Veress needle is used to establish pneumoperitoneum. A 10-mm blunt tip optical trocar is then inserted under direct visualization through the umbilicus and used as the camera port. Subsequently, a second 12-mm trocar is placed two-thirds the distance between the umbilicus and anterior superior iliac spine. A 12-mm trocar is used to allow for easy passage of an SH-needle for intracorporeal suturing. Finally, a 5-mm trocar is placed midway between the umbilicus and pubic symphysis.
Once trocars are within the abdomen, the colon is mobilized medially along the line of Toldt. The ureter is identified cephalad to the bifurcation of the iliac vessels, away from the point of obstruction. Ureterolysis is then carried out in a caudal direction taking care not to devascularize the ureter. If the length of the stricture extends more proximally, the ureter can be mobilized cephalad to the lower pole of the kidney. Once the ureter becomes entrapped in scar tissue, the ureter is transected, taking care to excise any nonviable tissue. The healthy ureter is then sharply spatulated posteriorly.
The bladder is filled with 200 mL of normal saline, and the overlying peritoneum is divided between the obliterated umbilical ligaments. This allows entrance into the space of Retzius, and the bladder can then subsequently be further mobilized by dividing anterolateral attachments. When performing a bladder dome advancement technique, no further mobilization is typically necessary. When performing a psoas hitch for longer strictures, the contralateral bladder pedicle may need to be divided before suturing the bladder to the ipsilateral psoas tendon. The ipsilateral anterior bladder wall is then opened transversely (2 cm to 3 cm) one-third the distance from the dome to the bladder neck. A temporary holding suture placed through the bladder caudal to the cystotomy can be brought through the anterior abdominal wall to make the subsequent anastomosis easier to perform. The middle portion of the posterior flap is then sewn to the apex of the spatulated ureter. Suturing the anastomosis is performed with a continuous 4–0 polyglactin suture with a double-armed, knotted suture as described for laparoscopic pyeloplasty by Eichel and associates. Once the posterior anastomosis is completed, a ureteral stent is passed proximally over a guidewire that is placed via the inferior trocar. When the wire cannot be directed into the proximal ureter secondary to a poor angle, it may be passed transurethrally with a flexible cystoscope or percutaneously through a large-bore angiocatheter. With the ureteral stent in place, the anterior anastomosis is completed, and the remaining bladder is closed in a longitudinal HeinekeMikulicz fashion. For a psoas hitch procedure, interrupted polydioxanone sutures are used to approximate the bladder dome to the psoas tendon to allow a tension-free vesicoureteral anastomosis. Finally, the anastomosis is checked by instilling 300 mL of saline into the bladder, and any additional interrupted sutures are placed as necessary.
A Jackson Pratt drain is placed through the lateral 12-mm trocar site, placed on bulb suction, and removed on the second postoperative day as long as drain fluid analysis is not consistent with urine. The Foley catheter is removed 7 days to 10 days after cystography reveals no evidence of extravasation, and the ureteral stent is subsequently removed at 4 weeks to 6 weeks. Diuretic renal scintigraphy or cystography is performed at 3 months and further radiographic follow-up is done at 6 months and 1 year with repeat renal scintigraphy, sonography, or intravenous pyelography.
Contraindications of Laparoscopic Ureteroneocystostomy:
Contraindications for this procedure are the same as those for an open ureteroneocystostomy. Importantly, a widely patent tension-free anastomosis is critical to success. If the stricture is too long or located more proximally, then the bladder may need to be mobilized cephalad with either a psoas hitch or Boari flap. Although technically more complex, these procedures can also be performed laparoscopically. The obvious limitation of this study is its retrospective nature, small number of patients, and limited follow-up.
Acute postoperative complications:
Acute postoperative complications of ureteroneocystostomy may include the following:
- Extravasation of urine
- Ureteral obstruction
- Hematuria
- Infection
- Bladder spasms
Long-term complications:
Long-term complications of ureteroneocystostomy may include the following:
- Persistent reflux
- Contralateral reflux
- Ureteral obstruction
- Urinary fistula
Conclusion:
Distal ureteral injuries are on the rise secondary to complex pelvic laparoscopy and ureteroscopy. The short-term results of LUR are encouraging with excellent success rates and minimal morbidity. Longer follow-up will be necessary to ultimately determine whether LUR will be the approach of choice for distal ureteral strictures.
World Laparoscopy Hospital, Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555






