Dr. Rehana Raja; Prof. Dr. R. K. Mishra
Projected to be submitted towards completion of Diploma in Minimal Access Surgery, World Laparoscopy Hospital, Gurugram, NCR Delhi, India.
Abstract:
T.P.Wright originally introduced the concept of a learning curve in aircraft manufacturing in 19361. He described a basic theory for costing the repetitive production of airplane assemblies. The term was introduced to medicine in the 1980s after the advent of minimal access surgery. It also caught the attention of the public and the legal profession when a surgeon told a public enquiry in Britain that a high death rate was inevitable while surgeons were on a learning curve.2 Recently it has been labeled as a dangerous curve3with a morbidity, mortality and unproven outcomes. Yet there is no standardization of what the term means. In an endeavor to help laparoscopic surgeons towards evidence based practices this commentary will define and describe the learning curve, its drawing followed by a discussion of the factors affecting it, statistical evaluation, effect on randomized controlled trials and clinical implications for both practice and training, the limitations and pitfalls, ethical dilemmas and some thoughts to pave the way ahead.
DEFINITION AND DESCRIPTION
For the Wright learning curve, the underlying hypothesis is that the direct man-hours necessary to complete a unit of production will decrease by a constant percentage each time the production quantity is doubled. In manufacturing, the learning curve applies to the time and cost of production. Can a surgeons learning curve be described on similar lines ? A simple definition would be : the time taken and / or the number of procedures an average surgeon needs to be able to perform a procedure independently with a reasonable outcome1 But then who is an average surgeon ? Another definition may be that a learning curve is a graphic representation of the relationship between experience with a new procedure or technique and an outcome variable such as operation time, complication rate, hospital stay or mortality4. A learning curve may also be operationally defined as an improvement in performance over time. Although learning theorists often disagree about what learning is, they agree that whatever the process is, its affects are clearly cumulative and may therefore be plotted as a curve. By cumulative it is meant that somehow the effects of experience carry over to aid later performance. This property is fundamental to the construction of learning curves. The improvement tends to be most rapid at first and then tails off. Hence there are three main features of a learning curve. First, the initial or starting point defines where the performance of an individual surgeon begins. Secondly, the rate of learning measures how quickly the surgeon will reach a certain level of performance and thirdly the asymptote or expert level measures where the surgeons performance stabilizes5. This has implications for the laparoscopic surgeon - it suggests that practice always help improve performance but the most dramatic improvement happens first. Also with sufficient practice surgeons can achieve comparable levels of performance.
THE DRAWING OF LEARNING CURVES
There are a variety of methods of constructing learning curves. They all assume that successive exposures in a learning series may be plotted on the x-axis, response characteristics on y-axis and the data points distributed in the xy plane may be legitimately connected by a curve. This is the Cartesian Method6 More recently the Cumulative Sum Method has been applied for the construction of these curves for basic skills in Anesthetic procedures - the method consists of relatively simple calculations that can be easily performed on an electronic spreadsheet. Statistical inferences can be made from observed successes and failures. The method also provides both numerical and graphical representation of the learning process.7
The multimode learning curve is useful because several factors can be put into one graph8. The earlier used method of the performance analysis with its on the spot appraisals at certain time intervals has been replaced by continuous assessment. For continuous data like operation time the Moving average method is useful9.
FACTORS AFFECTING LEARNING CURVES
A complex hierarchy of factors are involved here5. At the bottom ( Fig.1 ) factors like guidelines, protocols and standards for clinical governance agreed upon by the medical fraternity are vital. Next the Institutional policies and cost effectiveness are contributory. Needless to say the surgical team, the case mix and public awareness are relevant. The final level in the hierarchy that can influence individual learning is the characteristics of the surgeon such as attitude, capacity for acquiring new skills and previous experience10.
Amongst the latter that is the characteristics of the surgeon the learning curve may depend on the manual dexterity of the individual surgeon and the background knowledge of surgical anatomy. The type of training the surgeon has received is also important11 as training on inanimate trainers and animal tissue has been shown to facilitate the process of learning. The slope of the curve depends on the nature of the procedure and frequency of procedures performed in specific time period. Many studies suggest that complication rates are inversely proportional to the volume of the surgical workload12. However rapidity of learning is not significantly related to the surgeons age, size of practice or hospital setting13. Another important factor that affects the learning curve is the supporting surgical team. A recent observational study 14 to investigate the incidence of technical equipment problems during laparoscopic procedures reported that in 87% of procedures one or more incidents with technical equipment or instruments occurred. Hence improvement and standardization of equipment combined with incorporation of check lists to be used before surgery has been recommended.
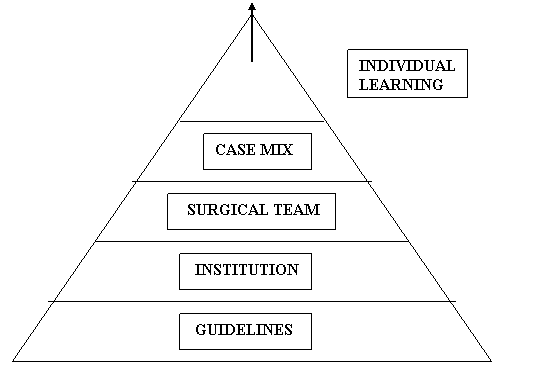
Fig-1. Hierarchy of factors affecting learning curve
STATISTICAL EVALUATION OF LEARNING CURVES
Various statistical methods have been reported in the assessment of the learning curve 15. Commonly data are split into arbitrary groups and the means compared by chi-squared test or ANOVA. Some studies had data displayed graphically with no statiscal analysis. Others used univariate analysis of experience versus outcome. Some studies used multivariate analysis techniques such as logistic regression and multiple regression to adjust for confounding factors. A systematic review 16 concluded that the statistical methods used for assessing learning curves have been crude and the reporting of studies poor. Recognizing that better methods may be developed in other non clinical fields where learning curves are present ( psychology and manufacturing ) a systematic search was made of the non clinical literature 17 to identify novel statistical methods for modeling learning curves. A number of techniques were identified including generalized estimating equations and multilevel models. The main recommendation was that given the hierarchical nature of the learning curve data and the need to adjust for covariant, hierarchical statiscal models should be used.
EFFECT OF LEARNING CURVE ON RANDOMIZED CONTROLLED TRIALS
The learning curve can cause difficulties in the interpretation of RCTs by distorting comparisons. The usual approaches to designing trials of new surgical techniques has been either to provide intensive training and supervision or require participating surgeons to perform a fixed number of procedures prior to participation in a trial. Surgeons have been reluctant to randomize until they are proficient in a technique but then once convinced of its worth argue that it is too late to randomize. However the best way to address the problem is to have a statistical description of the learning curve effect within a trial and various methods can then be used example Bayesian hierarchical model 5.
IMPLICATIONS FOR PRACTICE AND TRAINING
In the current era of evidence based medicine enthusiasm for laparoscopic surgey is rapidly gaining momentum. There is an immense amount of literature showing advantages of minimal access surgery and acceptance by the public. The learning curve for many procedures has been documented 18,19,20. As far as training is concerned, the introduction of laparoscopic techniques in surgery led to many unnecessary complications. This led to the development of skills laboratories involving use of box trainers with either innate or animal tissues but lacks objective assessment of skill acquisition 21. Virtual reality simulators have the ability to teach psychomotor skills. However it is a training tool and needs to be thoughtfully introduced into the surgical training curriculum 22. A recent prospective randomized controlled trial 23 showed that virtual simulator combined with inanimate box training leads to better laparoscopic skill acquisition. An interesting finding reported is that in skills training every task should be repeated atleast 30 to 35 times for maximum benefit 24. The distribution of training over several days has also been shown to be superior to training in one day 25. Other factors enhancing training are fellowship programmer 26, or playing video games 27. One can also obtain feedback for improvement of training programme In one such study the deficiency factors 28 identified were lack of knowledge, lack of synchronized movement of the non dominant hand and easy physical fatigue. Incorporation of intensive, well planned invitro training into the curriculum were made and the programmed reassessed.
WHAT ARE THE LIMITATIONS OR PITFALLS ?
"Steep" learning curves are usually used to describe procedures that are difficult to learn - however this is a misnomer as it implies that large gains in proficiency are achieved over a small number of cases. Instead the curve for a procedure that requires a lot of cases to reach proficiency should be described as "flattened" 29.
As long as no valid scoring system concerning the complexity of a surgical intervention exists, the learning curve cannot be used as benchmarks to compare different surgeons or clinics as legitimate instruments to rank surgeons or different hospitals..
Limitations of long learning curves, facilities for training, mistakes of pioneers, surgical techniques not being described in books are some of the limitations described 30.
There are other limitations due to the nature of laparoscopic surgery like the lack of 3D vision and of tactile sensations 31, difficult hand eye co-ordination and long instruments.
ETHICAL DILEMMAS
Many dilemmas exist 32 and many questions will always be with us - who bears the burden of the learning curve ? Are the patients aware of the risks ? Many reports validate the impression that a patient operated upon during the learning curve takes greater risks and incurs more adverse circumstances than the patient operated upon later. The issue of how informed the informed consent should be needs to be addressed. Is the integrity and conscience of a surgeon measurable? Should the forces of marketing be curtailed or regulated?
THE WAY FORWARD
Laparoscopic surgery is here to stay and success in it is determined by how quickly and effectively we learn. However certain measures may be taken to lessen some of the adverse effects of the learning curve and others to help laparoscopic surgeons ease into the specialist. Setting up 32 of minimal standards and credentialing is a must. Current guidelines in many countries are vague and general. The evidence for training is well documented. The message for individual surgeons is to identify their deficiencies, and chart a way forward for their personal graph of progress. Evaluation and monitoring in a systematic scientific manner will benefit the surgeon with a satisfactory learning curve that will ensure that patient welfare is not compromised.
REFERENCES:
- K. Subramonian, Muir G. The learning curve in surgery : what is it, how do we measure it and can we influence it ? BJU International 2004; 93 (9) 1173 - 1174
- Clare Dyer. Bristol case surgeon claimed to have been on "learning curve" BMJ 1999;319:1456
- Leon Morgenstenn , Warning ! Dangerous curve head: the Learning Curve Surgical Innovation , 2005; 101-103
- Michel LA. Epistelogy of evidence-based medicine. Surg Endosc 2007:21:2 pg146
- Cook JA, Ramsay CR, Fayers P. Statistical evaluation of learning curve effect in surgical trials. Clinical Trials 2004;1:421-427
- Learning as a cumulative function. ht://trincoll.edu/depts./ecopsyc/shaw/curves access on 22.4.07
- Getulio Rodriques de Oliveira Filho. The construction of learning curves for basic skills in anaesthetic procedures : an application for the Cumulative Sum Method: Anaesth Analg 2002; 95:411-6
- Buchmann P. Dincler S. Learning curve calculation and value in laparoscopic surgery Ther Umsch 2005;62(2):69-75
- Dincler S, Koller MT, Steurer J, Bachmann LM, Christen D, Buchmann P. Multidimensional analysis of learning curves in laparoscopic sigmoid resection: eight year results. Dis colon Rectum 2003;46(10):1371-8
- Cushieri A. Whither minimal access surgery: Tribulations and Expectations Am J.Surg 1995: 169:9-19.
- Traxer O, Gettmann MT Wapper CA et al . the impact of intense laparoscopic skills training on the operation performance of urology residents J, Urol 2003: 166: 1658-61.
- Hu Jc Gold KF, Pashos CL, Mehtass, Litwin MS, Role of surgeon volume in radical prostajtectomy outcomes. J clin Oncol 2003: 21: 401-5
- Gibbs VC Auerbach AD Learning curves for new procedures. Htpp://www.ahrq.gov/clinic/ptsafety/chap19.htm accessed on 24.4.07.
- Verdaasdonk EGG, Stassen LPS, Elst Mvander, Karsten TM, Dankelman J. Problems with technical equipment during laparoscopic surgery. Surg Endosc 2007;21:275-279
- Ramsay CR, Grant AM, Wallace SA, Garthwaite PH, Monk AF, Russell IT.Assessment of the learning curve in health technologies. A systemic review. Int J Technol Assess Health Care 2000;16:1095-108
- Ramsay CR, Grant AM, Wallace SA, Garthwaite PH, Monk AF, Russell IT. Statistical assessment of the learning curves of health technologies. Health Technol Assess 2001; 5:1-79
- Ramsay CR, Grant AM, Wallace SA, Garthwaite PH, Monk AF, Russell IT.Lessons from the non clinical literature. Int J Technol Assess Health Care 2002, 18:1-10
- Agachan F, Joo JS, Sher M, Weiss EG, Nogueras JJ, Wexner SD. Laparoscopic colorectal surgery. Do we get faster ? Surg Endosc 1997 11(4):331-5
- Schlachta CM, Mamazza J, Seshadri PA Cadeddu M, Gregoire R, Poulin EC. Defining a learning curve for laparoscopic colorectal resection. Dis Colon Rectum 2001 44(2):217-22
- Perino A, Cucinella G, Venezia R, Castelli A, Cittadini E. Total Laparoscopic hysterectomy versus total abdominal hysterectomy: an assessment of the learning curve in a prospective randomized study. Human Rep 1999 14:12 2996-2999
- Aggarwal R, Moorthy K, Darzi A. Laparoscopic skills training and assessment. BJS 2004 91:2 pg 1549-1558
- Gallager AG, Ritter EM et al. Virtual reality simulation for the operating room : proficiency based training as a paradigm shift in surgical skills training. Annals of Surgery 2005 241(2) :364-372
- Mada AK, Frantzides CT, Prospective randomized controlled trial of laparoscopic trainers for basic laparoscopic skills acquisition. Surg Endosc 2007 21:2 pg 209-13
- Scott DJ, Young WN, Tesfay ST,et al Laparoscopic skills training. Am J Surg 2001 Aug 182(2):137-42
- Verdaasdonk EGG, Stassen LPS et al. Influence of different training schedules on the learning of psychomotor skills for endoscopic surgery. Surg Endosc: 2007 21: 214-219
- Oliack D, Owens M, Schmidt HJ. Impact of fellowship training on the learning curve for laparoscopic gastric bypass. Obes Surg 2004 14(2) : 197-200
- Rosser JC et al. The impact of video games on training surgeons in the 21st century. Arch Surg 2007; 142:181-186
- Gupta R. Feedback from operative performance to improve training programme of Laparoscopic Radical Prostectomy. J of endourology 2004 18:9 pg 836-839
- Guillonneau BD. The learning curve as a measure of experience. Nature Clinical Practice Urology 2005: 2:309
- Canis M, Mage G, Wattiez A, Pouly JL, Bruhat MA The ovarian endometrioma; Why is it so poorly managed ? Human Repr: 2003 18;1 pp5-9
- Agha R, Muir G. Does Laparoscopic surgery spell the end of open surgery ? J R Soc. Med 2003; 96:544-546
- Iservon KV, Chiasson PM, The ethics of applying new medical technologies 2000, Semin Laparosc Surg 9(4): 222-229.






