Light cable and light source and Future of laparoscopy
The Interface of a standard light source:
Manual or automatic intensity control circuit:
Troubleshooting of Laparoscopic Light Source:
Key Words:
Light cable, Light Source, Laparoscopy, Fibre Optic Cables, Gel cables, Halogen lamp, Xenon lamp, Metal halide lamp.
Introduction:
Light is essential for performing most of the modus operandi of life. Thanks to Edison who discovered electric bulb. The Minimal access surgery depends on the artificial light available in closed body cavity, and before the discovery of light source and light cable; mirrors were used to reflect the light onto the subject where the direct light access was not possible. In 1867 Bruck, a Dentist from Breslau, made a platinum wire loop which he heated with electric current, and used that as a light source for purpose of surgery. Endoscopy was performed, by using tungsten light bulbs inside the body cavity before 1954. These bulbs were emitting low frequency red color of light. The bulb was so hot that there was always a risk of injury to bowel.
Fibre Optic Cables:
In 1954 a major breakthrough in technology occurred in the development of fibre optic cables. The principle of fibre optic cable was based on the total internal reflection of light. Light can be conducted along a curved glass rod due to multiple total internal reflections at the walls of the rod. Light would enter at one end of the fibre and emerge at the other end after numerous internal reflections with virtually all of its strength.
Now a day there is two types of light cable available in market.
- Fiber Optic cable
- Liquid crystal Gel cable
Optic cables
These cables are made up of a bundle of optical fibres glass thread swaged at both ends. The fibre size used is usually between 10 to 25 mm in diameter. They have a very high quality of optical transmission, but are fragile. In fact, progressively as they are used, some optical fibres break. The loss of optical fibres may be seen when one end of the cable is viewed in daylight. The broken fibres are seen as black spots.
Gel cables
These cables are made up of a sheath that is filled with a clear optical gel. (Liquid crystal). Theoretically they are capable of transmitting 30% more light than optic fibres. Swaged at both ends by quartz. Due to more light and better color temperature transmission this cable is recommended in those circumstances where documentation (movie, photography or TV) is performed. They pose three problems:
- The quartz swaging at the ends is extremely fragile, especially when the cable is hot. The slightest shock, on a bench for example, can cause the quartz end to crack and thus cause a loss in the transmission of the light;
- These cables transmit more heat than optical fibre cables.
- These cables are made more rigid by a metal sheath, which makes them more difficult to maintain and to store.
In conclusion, even though the choice is a difficult one, we use optical fibre cables, which are as fragile as the gel cables but their flexibility makes them much easier to maintain.
Attachment of Light Source:
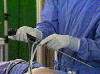
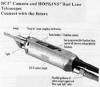
Conventional attachment. DIC Attachment
Conventional attachment has at right angle connection for light source and camera. Now a day some new attachment for light cable is available known as DIC Interface. The benefit of this is that it maintains upright orientation regardless of angle of viewing, using auto Rotation system. It also provides single handed control of the entire endoscope camera system.
Maintenance of light cable:
- Handle them carefully,
- Avoid twisting them
- After the operation has been completed, the cable should preferably be disconnected from the endoscope and then connected to the light source. In fact, most of the sources currently available have a plug for holding the cable until it cools down.
- The intensity of light source is so high that there is chance of retinal damage if the light will
- The end of the end crystal of cable should be periodically cleaned with a cotton swab moistened with alcohol.
- The outer
- Fiber optic cable should never be placed on or under drapes, or next to the patient, if it is connected to an illuminated light source. The heat generated from the intensity of light may cause burns to the patient or ignite the drapes.
The light source:
One of the advantages of the laparoscopy is that of obtaining a virtually micro-surgical view compared to that obtained by laparotomy. Whereas in fact at present, this view has become opto-electronic. Quality of the image obtained very much depends on the quantity of light available at each step of optical and electronic system.
A typical light source is consist of
- A lamp
- A heat filter
- A condensing lens and
- Manual or automatic intensity control circuit.
Lamp:
Lamp or bulb is the most important part of the light source. The Quality of light depends on the lamp used. Several Modern types of light sources are currently available on the market. These light sources mainly differ on the type of bulb used. Four types of lamp are used more recently.
- Quartz halogen.
- Incandescent bulbs.
- Xenon &
- Metal halide vapor arc lamp.
Halogen bulbs
Halogen bulbs provide a highly efficient, almost crisp white light source with excellent color rendering. Electrodes in halogen lamps are made of tungsten; this is the only metal with a sufficiently high melting temperature and sufficient vapor pressure at elevated temperatures. They use a halogen gas that allows bulbs to burn more intensely without sacrificing life. Halogen bulbs are low voltage and have an average life of 2,000 hours. Colour temperature of Halogen lamp is (5000-5600 K). These lamps are cheap and can be used for laparoscopic surgery if low budget setup is required.
Xenon lamps
Xenon lamps consist of a spherical or ellipsoidal envelope made of quartz glass, which can withstand high thermal loads and high internal pressure. For ultimate image quality, only the highest-grade clear fused silica quartz is used. It is typically doped, although not visible to the human eye, to absorb harmful UV radiation generated during operation. The colour temperature of Xenon lamp is 6000-6400 K. The operating pressures are tens of atmospheres at times, with surface temperatures exceeding 600 degrees C.
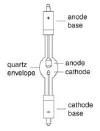
The smaller, pointed electrode is called the cathode, which supplies the current to the lamp and facilitates the emission of electrons. To supply a sufficient amount of electrons, the cathode material is doped with thorium. The optimum operating temperature of the cathode tip is approximately 2000 degrees C. To obtain this precise operating temperature, the cathode tip is pointed and in many cases has a groove on the pointed tip to act as a heat choke. This heat choke causes the tip to run at a higher temperature. This configuration of the cathode tip allows for a very high concentration of light from the cathode tip and a very stable arc. The anode, the larger electrode, receives electrons emitted by the cathode. Once the electrons penetrate the anode face, the resulting energy is converted to heat, most of which radiates away. The large, cylindrical shape of the anode helps to keep the temperature low by radiating the heat from the anode surface.
Metal halide vapor arc lamp.
In metal halide lamp the mix of compounds (comprising mostly salts of rare earths and halides as well as the Mercury which provides the conduction path) is carefully chosen to produce an output which approximates to 'white' light as perceived by the human eye. There are two type of Metal halide lamp generally used:
Iron Iodide Lamp: Iron Iodide is a broad emitter and enhances the spectral output of the lamp in the 380nm region.
Gallium Iodide Lamp: Gallium Iodide has the effect of introducing spectral lines at 403nm and 417nm of the electromagnetic spectrum.
The intensity of the light delivered by any lamp is also depend on the power supply of the source. However, increasing the power poses a real problem as concerns the heat created. At present, the improvements made to the cameras means that it is possible to return to reasonable power levels, of the order of 250 Watts. 400 W units are, however, preferable in order to guarantee sufficient illumination of the abdomen even when bleeding causes strong light absorption.
The most frequently used two main types of lamps are halogen and xenon. This difference may be remarked in the colors obtained, the xenon having a slightly bluish tint. The light emitted by xenon lamp is more natural compared to halogen lamp. However, most of the cameras at present analyze and compensate these variations by means of automatic equalization of whites (2100 K to 10000 K), which allows the same image to be obtained with both light sources. A proper white balancing before start of the operation is a very good practice for obtaining a natural color. The white light is composed of the equal proportion of Red, Blue and Green Colour and at the time of white balancing the camera sets its digital coding for these primary colors to equal proportion assuming that the target is white. And if at the time of white balancing the telescope is not seeing a perfectly white object then the setup of the camera will be very bad and the color perception will be very poor.
The newer light source of Xenon, now a day used is defined as a cool light but practically it is not completely heat free and it should be cared for ignition hazard.
Heat Filter:
For 100 % of energy consumed, a normal light source (a light bulb) uses approximately 2 % in light and 98 % in heat. This heat is mainly due to the infrared spectrum of light and due to obstruction in the pathway of light. If Infrared will travel through the light cable than the cable will become intolerable hot. A heat filter is introduced to filter this infrared to travel in fibre optic cable. A cool light source lowers this ratio by creating more light, but does not reduce the heat produced to zero. This implies a significant dissipation of heat, which increases as the power rating increases. The sources are protected against transmitting too much heat at present. The heat is essentially dissipated in transport, along the cable, in the connection with the endoscope and along the endoscope.
Some accidents have been reported due to burning caused by the heat of the optics system. It is therefore important to test the equipment, particularly if assemblies of different brands are used.
A condensing lens:
The purpose of condensing lens is to converge the light emitted by lamp to the area of light cable input. In most of the light source it is used for increasing the light intensity per square cm of area.
The Interface of a standard light source:
It is essential to know about all the switch and function of the light source. All essential details of the equipment and all the action required on the part can be found on the operating manual of the product.
Some common functions on almost every light source are as follows:
- Power switch
- Intensity display in %
- Display for control range
- Pilot lamp "Video" when Video is received
- Keys to adjust control range (Automatic video mode)
- Pilot lamp "Video" when no video signal is received
- Key to adjust light intensity (Manual mode)
- Light Exit
- Dummy Socket for plugging light source when not in use.
- Air Vent
- Power fuse holder
- Power cord connector
- Jack for potential equalization cable
- Video Signal Output
- Video Signal Input
Every light source is fitted with an extra lamp for emergency purpose, but even though the surgeon or their staff should know the technique of changing of bulb and few extra bulb should always be ready for emergency replacement.

Internal view of the light source:
- Lamp holder
- Lamp
- Connecting cord of Lamp
- Lamp locking clip.
Technique of changing bulb:>

Slide the lamp locking clip with any screw driver after disconnecting the cord of the lamp.
Gently lift out the lamp and replace it with new lamp and then connect the cord of the lamp to the appropriate socket. The caution should be there not to touch the lamp immediately after use because they may be very hot to cause burn.
Manual or automatic intensity control circuit:
Manual adjustment, which allows the light source to be adjusted to a power level defined by the surgeon. When video cameras are used, close-up viewing is hampered when there is too much light, whereas more distant views may be too dark. To counter this problem, the luminosity of most of the current light sources is adjustable.
Automatic adjustment: The advance light source system is based on the automatic intensity adjustment technology. The video camera transforms the signal into an electronic signal. This electronic signal is coded in order to be transported. The coding dissociates the luminance and chrominance of the image. The luminance is the quantity of light of the signal (black and white) that dictates the quality of the final image. When there is too much light for the image, (when the endoscope is near to the tissue) the luminance signal of the oscilloscope increases. On the other hand, when the luminosity is low, (distant view or red surroundings), the luminance is low and the electronic signal much weaker. A good quality luminance signal is calibrated to 1 milli volt. Overexposed images make the electronic signal pass above one millivolt, whereas underexposed images make the signal drop below one millivolt. Light sources equipped with adjustment analyze the luminance. If the signal is significantly higher than 1 millivolt, they lower the power and bring the signal back within the standards. Inversely, if the signal is too weak, they increase their intensity.
These systems are extremely valuable, permitting work to be performed at different distances from the target in good viewing conditions. However, the cameras currently available are often equipped with a regulation system, which are capable of automatic gain control in poor light condition and the purchase of a light source with adjustment associated with a camera equipped with an adjustment system is a double purchase that is unnecessary.
Troubleshooting of Laparoscopic Light Source:
Iinadequate lighting:
| Probable cause | Remedy |
|---|---|
| Loose connection at source or scope | Adjust connector |
| Light is on "manual-minimum" | Go to "automatic" |
| Bulb is burned out | Replace bulb |
| Fiber optics are damaged | Replace light cable |
| Automatic iris adjusting to bright | Dim room lights |
| reflection from instrument | Re-position instruments, or switch to "manual" |
A laparoscopic surgeon should be technically well acknowledged of the principle of the instrument they are using, and should not always depend upon their technical team should an emergency arrive. The purchase of a costly instrument is not only answer for achieving a good task, perceptive to handle them is equally important.
Future of Minimal Access Surgery.
Remote possibilities
04/04/2002 -- In the future remote handling technology will overcome the manipulative restriction in the current instruments. There is no doubt 20 years from now some surgeons will be operating exclusively via a computer interface controlling a master-slave manipulator. If computer-controlled machinery can mimic the awareness, adaptability and knowledge of a human surgeon, such a takeover in the operating theatre is actually realistic. In the operating room of the future, physicians will use tiny high-tech tools to travel inside the body with dexterity and precision beyond imagining. The future is now But the future of any new technology depends upon how well the training is.
Although the potential of robotic surgery is just beginning but, progress may come quickly. Laparoscopic gallbladder surgery was first done 1987, but it became standard within five years. Just think about a surgeon ! He picks up this black box and waves it over your body, and you're fixed. How's that going to happen? One day a surgeon may use robotic devices to enter the body through its own orifices. They could carry medical instruments inside the body, where they would be manipulated by simple computer commands.
Minimal Access Surgeon






