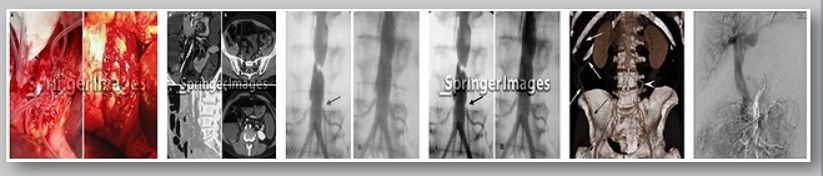
Introduction
Mesenteric thrombosis considers to a blood clot that occludes the mesenteric vein, which is situated in the tissue that adjoins the intestine to the back of the abdominal wall. People who have undergone former abdominal surgery and individuals who suffer from hyper-coagulable states are at high risk for mesenteric thrombosis. Other predisposing factors containing inflammation, such as pancreatitis; portal hypertension; enlargement of the spleen (splenomegaly); disease; decompression; paroxysmal nocturnal hemoglobinuria;malignancy; blunt abdominal trauma; and visceral infection. However, in half the cases, no underlying cause is found. Mesenteric thrombosis is a rare but often lethal form of intestinal ischemia. Mesenteric thrombosis makes up 5% to 15% of all cases of acute mesenteric ischemia.
Laproscopic management of thrombosis of the inferior mesenteric artery:
Surgical treatment incorporates exploratory laparotomy, followed by recognition of the involved artery and bowel. Due to thrombosis develops at the base of the vessel, the whole small bowel and proximal large bowel appears ischemic. In contradistinction, embolization of the SMA results in the proximal jejunum being spared, reflecting the more distal occlusion. Remove dead bowel and attempt reanastomosis. Open the affected artery and perform an endarterectomy. Bypass techniques may also be performed using prosthetic grafts. If a patient is found to have perforated bowel on laparotomy, use an autogenous saphenous vein graft because of the decreased risk of graft infection. Endovascular therapies have been described for chronic mesenteric ischemia, and some authors have tried thromboaspiration. The criterion standard remains operative exploration to allow assessment of bowel viability.
Patients with acute ischemia should have immediate repletion of fluids and correction of any acid/base abnormalities; they should then undergo surgery without delay. All patients should receive broad-spectrum antibiotic therapy prior to the start of the operation. Type and cross 4 units of packed red blood cells prior to surgery.
Intraoperative management of thrombosis of the inferior mesenteric artery:
Assess the viability of the bowel during direct observation. Look for peristalsis and observe the color of the bowel. Intraoperative Doppler ultrasonography of the bowel can provide valuable information on the patency of the vessels. One gram of intravenous fluorescein followed by bowel examination under Wood lamp illumination can delineate poorly perfused bowel. Treat mesenteric thrombosis by revascularization or endarterectomy. If not already started, begin anticoagulation therapy with intravenous heparin. Following reconstitution of arterial flow, the viability of the bowel is reassessed. Reassessment is based on clinical findings, including the color of the bowel and the presence or absence of palpable pulses.
Postoperative management of thrombosis of the inferior mesenteric artery:
Postoperative care should include close monitoring of blood pressure and hemoglobin level to evaluate for sepsis or hemorrhage. Patients should continue to have postoperative heparin anticoagulation therapy in order to reduce thrombotic events, and papaverine may be administered to reduce vasospasm. Perform a 12-lead electrocardiogram to evaluate for myocardial dysfunction. Patients can be expected to have a postoperative ileus due to bowel reperfusion.
Complications:
Because of the high incidence of atherosclerosis in patients with mesenteric ischemia, it is not surprising that one of the most common postoperative complications involves MI. Prevention of postoperative MI involves preoperatively identifying correctable coronary artery disease. During the perioperative period, use a Swan-Ganz catheter to monitor fluid and cardiac function. Finally, when cross-clamping the supraceliac aorta, the anesthesiologist can ensure myocardial protection and after load reduction to maximize cardiac output. Acute renal failure in the immediate postoperative period can be prevented by keeping the patient well hydrated and administering mannitol before the aorta is cross-clamped. Other possible complications include bleeding, infection, bowel infarction, prolonged ileus, and graft infection.
Results:
Unfortunately, the outcome of patients suffering from acute thrombosis is not as good as that of patients with chronic ischemia. The average mortality rate of patients with acute thrombosis is 75-80%. For those patients who do survive, the risk of rethrombosis is high, and lifestyle may be hindered by a lifetime of total parenteral nutrition.
World Laparoscopy Hospital, Cyber City, DLF Phase II, Gurugram, NCR Delhi, 122 002, India
PHONES:
For Training: +919811416838
For Treatment: +919811912768
For General Enquiry: +91(0)124 - 2351555





