Dr. Maria Anna Sabelli
Consultant Gynecologist
Milano Italy P.O. Box 20154
Milano Milano
20154 Italy
Project submitted towards completion of Diploma in Minimal Access Surgery, World Laparoscopy Hospital, India 110018
Abstract:
Purpose: The aim of this study is to review qualified literature to compare the laparoscopic (MAS) with the abdominal (TAS) approach for treatment of patients with endometrial carcinoma
Methods: We search for all clinical trial, comparative prospective and retrospective studies, and cohort studies throw Cochrane Central Register of controlled trial, Medline, EMBASE, NCI.
Results: Were found five Randomized Clinical trial LAVH or TLH versus Abdominal Hysterectomy and nine comparative reliable studies. We proceeded to analyze these study to compare MAS versus TAS first surgery to manage endometrial cancer Overall Survival (OS), Disease free survival (DFS), recurrence, surgery and post surgery complication, Concordance of results between RCT and Comparative studies give value at: OS and DFS independent variables from the access technique but size sample is not sufficient in both, comparative and RCT, to definitively accreditatethis purpose. Intraoperative complications and Postoperative more frequent significantly in TAS.
Conclusion: LAVH and TAH seem to be save in endometrial cancer I to III FIGO stage patients with less side effect but more evidence needs about OS, DFS and recurrences by site. Vaginal recurrence and urologic complications need more attention. Lack of consensus agreement about surgery techniques for extrafascial total hysterectomy in MAS often not permit comparability of the studies. Doubts persist about vault and pelvic and port side recurrence in MAS technique.
Keywords: endometrial cancer, endometrial neoplasm, Laparoscopic assisted vaginal hysterectomy, Trans Abdominal Hysterectomy, Total Laparoscopic Hysterectomy.
Backgraund
Traditionally staging endometrial cancer (1) is performed through a laparotomy (TAS) but growing instruments and skills for Minimal Access Surgery (MAS) increased over in the World performing, in the clinical practice, surgery and staging endometrial cancer laparoscopically. Some studies suggest that the laparoscopic approach results in a reduction in postoperative morbidity also in overweight and elderly women (2) (3), in comparable intraoperative complications and perhaps similar Overall Survival and Desease free Survival (4), (5), (6). The effectiveness of the new surgical technical approach for staging endometrial cancer Laparoscopy assisted vaginal hysterectomy (LAVH) and Total Laparoscopic Hysterectomy (TLH) with attention to the main outcome it is not yet established. The risk of port site metastases and the risk of vaginal recurrence are not established. All studies found less hospital stay, operative time longer in MAS, similar possibility to execute a correct staging for I and II stage with more linphonodes in MAS. The aim of this study is to review qualified literature to compare overall survival (OS), Disease free survival (DFS), surgery and post surgery complication, in open versus MA surgery to manage endometrial cancer.
Material and Methods:
We search for clinical trial and comparative studies for all stages endometrial cancer in woman managed with surgery as first step therapy throw Cochrane Central Register of controlled trial, Medline, EMBASE, NCI.
Type of surgery: LAVH and TLH and TAH
End point for searching: DFS, OS, Recurrences, Complication intraoperative (Blood loss, urinary tract injury, bowel injury, vessel injury) and postoperative (Infection, DVT, hematoma).
We searched with :
- Endometrial cancer
- Endometrial neoplasm
- Endometrial carcinoma
- Laparoscopic Assisted Vaginal Hysterectomy
- Total Laparoscopic Hysterectomy
- LAVH
- TLH
- Controlled clinical trial
- Randomized controlled trial
- Clinical trial And mesh the terms
We looked at type of study design, size of study and duration of follow up. And chose to extend the search also to comparative clinical study because the size of RCT was really too small and too short in follow up to evaluate OS, DFS, Recurrence.
This is not a systematic review and no statistic analyses have been performed. A systematic review will be performed by Cochrane Collaborative Oncology Group (18). Data abstraction was directly by full test of the publications in the Journals.
Results
We found five RCT that are shown in the figure 1. All compare LAVH or TLH with TAH. We consider together LAVH and TLH (MAS) because the majority of the studies compare LAVH with TAH and very few TLH (20) (21) (13). We found 3 publications from Tozzi and Malur (6) (8) (9) and there is some doubt about the independence of the cases reported. . It would be possible that one RCT was reported on going. The total number of randomized patients is 429 but only 261 if the three publications by Tozzi and Malur are not independent. We would have had ask them about.
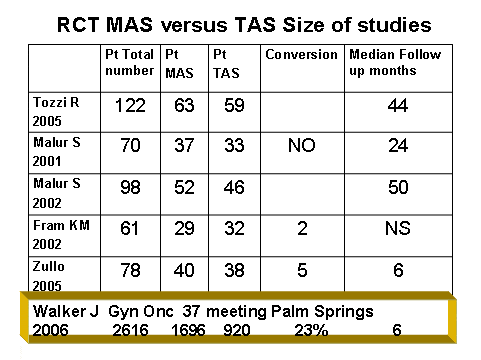
Figure 1
The median follow up in Tozzi and Malur is sufficient to exclude 80% recidive but this is not true for Fram and Tozzi because the time of follow up is less of 1 year. All trials admitted woman with diagnosis of endometrial carcinoma without selection of histological type. The trial from GOG J Walker with a sample size adequate had been closed in 2006 but we are attending for results. From preliminary report we can see that the rate of convertions is higher ( 23%) than that of RCT (12) Tozzi (6) and Malur (8) (9) admitted stage I to III, Fram (10) and Zullo (11) admitted woman with estimated I stage endometrial cancer. Tozzi and Malur perfomed LAVH also with coagulation of uterine artery during laparoscopy time at the origin from internal iliac artery without transaction. Fram catch the artery during vaginal time. Zullo refer to LAVH previous description. Not all studies reported if and which kind of uterine manipulator was used in LAVH performed. Malur (8) performed “abdominal hysterectomy extrafascially”. The convertion rate to open surgery is not always given. In figure 2 is shown the sizes of the comparative studies. Total number of patients was 1532 and all authors declare the comparability of the groups but Wang (19) and Obermair (20) for bias of distribution of stage in the two groups. The conversion rate results range between 2% and 46 % and the median follow up period is longer (than RCT until now) between 23 and 53 months.
Fram and Zullo don’t give information about the surgical way for cutting uterine artery.
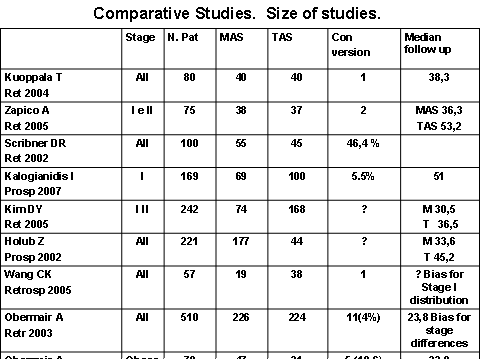
Obermair A Retr 2005 | Obese | 78 | 47 | 31 | 5 (10,6) | 23,8 |
Figure2
Recurrences, OS and DFS from RCT and comparative are in figure 3 and 4
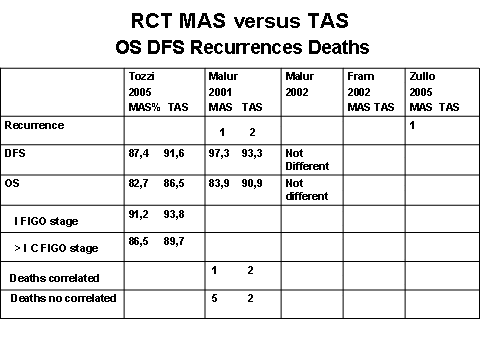
Figure 3
RCT found no significant differences in OS, DFS. This conclusion is the same in the nine studies comparative with a longer time of median follow up. (Fig 4) Recurrences is not so different in the groups if we exclude Obemair and Kalogianidis that declare bias for Stage I different distribution and found more recurrences in the MAS group.
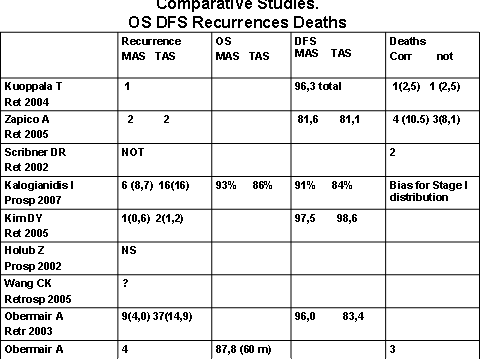
Figure 4
Obermaier (21) found a better DFS in TAS than in MAS for the bias. The size of RTC studies permits quite good evaluation of some complications like blood loss intraoperative and overall complication postoperative but not rare complications like injury and DVT or deaths surgery correlate (Fig 5).
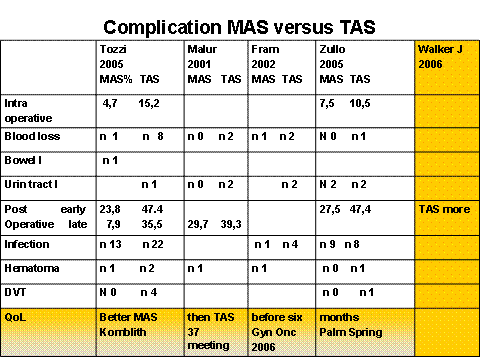
Figure 5
From the comparative studies there is confirm that postoperative complication are reduced by MAS. (Fig 6) Reduction is significant for the infection complications. The rate of intraoperative complications is less in MAS in the RCT studies but not in comparative studies where not significant differences were found. The blood loss is significantly less in MAS than in TAS but postoperative transfusions was no so different.
Comparative Studies. Complications
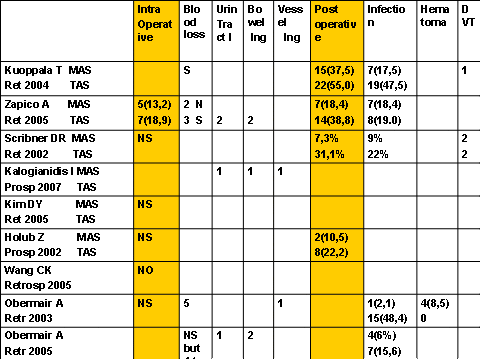
Figure 6
Conclusion
It seems safe to perform MAS for staging endometrial cancer. We must expect more conversions than we thought, also in I and II stage cancer. We have only few observations about recurrences. It seems that MAS approach doesn’t’ change the rate of port side recurrences and abdominal recurrences. We need more confirms that cells are not spread in the abdominal cavity by CO2 insufflation. More follow up time and the Walker GOG trial results we hope will give us more certainties., Postoperative complications are less in MAS and for the intraoperative complications we can hope that increasing skills will give more advantage to the MAS technique. More consensus about extrafascial hysterectomy needs. This can influence recurrences. The laparoscopic way to perform LAVH is described ( Childers M 1993, 1992 and McCartney 1995) but division of the uterine vessels sometime is performed during the laparoscopy time, sometime during vaginal approach The actual tendency to prefer to perform LTH open new problems about uterine manipulator save for the integrity of endometrial line after surgery. Tube manipulator has been proposed by Obemair. RCT proposed by Janda (24) 2006 that compare TLH with TAH is the replay to respond questions MAS versus TAS in a really similar way to perform staging endometrial cancer quality surgery.
Bibiography
- Revised FIGO staging for gynaecological cancer. Shepherd JH .Br J Obstet Gynaecol. 1989 Aug;96(8):889-92
- Scribner DR Jr, Walker JL, Johnson GA, McMeekin SD, Gold MA, Mannel RS. Surgical management of early-stage endometrial cancer in the elderly: is laparoscopy feasible? Gynecol Oncol. 2001 Dec;83(3):563-8.
- Eltabbakh GH, Shamonki MI, Moody JM, Garafano LL. Hysterectomy for obese women with endometrial cancer: laparoscopy or laparotomy? Gynecol Oncol. 2000 Sep;78(3 Pt 1):329-35
- Eltabbakh GH. Analysis of survival after laparoscopy in women with endometrial carcinoma. Cancer. 2002 Nov 1;95(9):1894-901.
- Obermair A, Manolitsas TP, Leung Y, Hammond IG, McCartney AJ. Total laparoscopic hysterectomy for endometrial cancer: patterns of recurrence and survival. Gynecol Oncol. 2004 Mar;92(3):789-93
- Tozzi R Malur S, Koehler C, Schneider A. Laparoscopy versus laparotomy in endometrial cancer: first analysis of survival of a randomized prospective study. J Minim Invasive Gynecol. 2005 Mar-Apr;12(2):130-6.
- Tozzi R, Malur S, Koehler C, Schneider A. Analysis of morbidity in patients with endometrial cancer: is there a commitment to offer laparoscopy? Gynecol Oncol. 2005 Apr;97(1):4-9
- Malur S Possover M, Michels W, Schneider A. Laparoscopic-assisted vaginal versus abdominal surgery in patients with endometrial cancer--a prospective randomized trial. Gynecol Oncol. 2001 Feb;80(2):239-44
- Malur S, SteinmetzI, PossoverM, SchnederA Laparoskopisch Assistertie vaginale versus Abdominale operationstechnik bei patietinnen mit Endometriumkarzinom. Eine prospektiv Randomisierte Stadie.Geburshilfe und Frauenheilkunde 2002 62, 5: 446-451
- FramK M Laparoscopically assisted vaginal hysterectomy versus abdominal hysterectomy in stage I endometrial cancer. Int J Gynecol Cancer. 2002 Jan-Feb;12(1):57-61
- Zullo F, Palomba S, Russo T, Falbo A, Costantino M, Tolino A, Zupi E, Tagliaferri P, Venuta S.A prospective randomized comparison between laparoscopic and laparotomic approaches in women with early stage endometrial cancer: a focus on the quality of life. Am J Obstet Gynecol. 2005 Oct;193(4):1344-52
- Hope JM Advancing Women,s Cancer care Conference Report from 37th Annual Meeting of the Society of Gynec Oncol, Palm Springs, Calif USA March 22-26, 2006
- Kuoppala T, Tomás E, Heinonen PK. Clinical outcome and complications of laparoscopic surgery compared with traditional surgery in women with endometrial cancer. Arch Gynecol Obstet. 2004 Jul;270(1):25-30. Epub 2003 May 1.
- Zapico A, Fuentes P, Grassa A, Arnanz F, Otazua J, Cortes-Prieto J. Laparoscopic-assisted vaginal hysterectomy versus abdominal hysterectomy in stages I and II endometrial cancer. Operating data, follow up and survival. Gynecol Oncol. 2005 Aug;98(2):222-7
- Scribner DR Jr, Walker JL, Johnson GA, McMeekin SD, Gold MA, Mannel RS. Surgical management of early-stage endometrial cancer in the elderly: is laparoscopy feasible? Gynecol Oncol. 2001 Dec;83(3):563-8
- Kim DY, Kim MK, Kim JH, Suh DS, Kim YM, Kim YT, Mok JE, Nam JH. Laparoscopic-assisted vaginal hysterectomy versus abdominal hysterectomy in patients with stage I and II endometrial cancer Int J Gynecol Cancer. 2005 Sep-Oct;15(5):932-7.
- Holub Z, Jabor A, Bartos P, Eim J, Urbánek S, Pivovarniková R. Laparoscopic surgery for endometrial cancer: long-term results of a multicentric study. Eur J Gynaecol Oncol. 2002;23(4):305-10
- Galaal K, Fisher A, Kew F, Lopes Laparoscopy versus laparotomy for the management of endometrial cancer ( Cochrane Protocol)
- Wong CK et alLaparoscopy compared with laparotomy for surgical staging of endometrial carcinoma. J.Obstet. Gynaecol. Res. 31,4 ;286-290 2005
- Obermaier A 2004 Total laparoscopicHysterectomy for endometrial cancer. Patterns of recurrence and survival. Gyn. Onc. 92 (2004):789-793
- Obermaier A 2005 et al.Total Laparoscopic hysterectomy versus total abdominal hysterectomy for obese women with endometrial cancerInt. Gynecol Cancer 2005, 15, 319-324
- Kaligiannidis I. Laparoscopy assisted vaginal Hysterectomy compared abdominal hysterectomy in clinical stage I endometrial cancer: safety, recurrence, and long-term outcome. Am J. Ostetric Gynecol. Oncology Research March 2007
- Janda M.et al . Total laparoscopic versus open surgery for stage 1 endometrial cancer : the LACE randomized controlled trial. J Contemporary Clinical Trial 27, 2006 353- 363






