Dr. Ghassan I. Kh. Saidi
Jordanian Board (General surgery)
DIPLOMA IN MINIMAL ACCESS SURGERY
Member of World Association of Laparoscopic Surgeon
Project Submitted towards Completion Of Diploma In Minimal Access Surgery, World Laparoscopy Hospital, Gurugram, NCR Delhi, India. September 2007
Abstract:
laparoscopic roux en y gastric bypass(LRYGB) has become a standard operation for obesity patients. Obesity is the seventh cause of death in united states, although the benefits of such a surgery are diverse and the surgeons experience with this surgery has increased dramatically, but still with such major surgery complications are still recorded either due to surgical procedure it self or due to the change of alimentary tract physiology and its consequences. This surgery consist of creating a small gastric pouch creating a restrictive effect (alimentary tract) and bypassing the gastropancreaticobiliary secretion distally in food tract creating mall absorption effect (hepatobiliary tract). In this article I sum up most of the literature written complications and our current proposed management off it.
Key words: Gastric bypass, Laparoscopic bariatric surgery, Complications of bypass surgery, Laparoscopic bypass surgery
Introduction:
Roux en y gastric bypass surgery was already being done in the 1990s for super morbid obese patient as open surgical technique but with the increased laparoscopic surgical experience it started to gain popularity between bariatric surgical centre around the world specially it has a dual restrictive and mall absorption effect causing sustained late low weight t effect in comparison with gastric banding and vertical gastroplasty.. its also superior to the current available medical therapy so far.
Objective:
To sum up the complications associated with that procedure and possible management.. Complications with (LRyGb) is divided to complication due the surgical procedure early and late type A and complications due to the mall absorption effect type B.
The following parameters were discussed in this article:
- Operation technique
- Anesthesia management of (LRYGB)
- Mall absorption effect
- Metabolic syndrome
- Rare syndromes
- Rule of imaging
- Proposed management and precautions
Materials and methods:
Review of articles was done by using high wire press web, Springer Link and library facility available at laparoscopic hospital, The following search terms was used; laparoscopic roux en y gastric bypass, complications, metabolic change, Criteria for selection of papers were upon statistical way of analysis, institute if they were specialized for laparoscopy, the way of management and the technique of operations
(LRyGb)
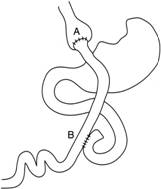
Laparoscopic LRyGb was described by wittgrove, clark,and tremblay 1994 ,,creating a small vertical gastric pouch of 5 to 30 ml using linear stapler .treitz ligament is identified and a jejunum is divided 12 cm away with a linear stapler ..a75 to 150 cm of roux limb is constructed to perform side by side jejunojejunostomy by linear endoscopic stapler (Schwartz’s). Many modification of this technique took place since then like using a linear stapler instead of circular to connect the jejunum (roux limb) with gastric pouch ,,other change from retro colic anastomosis to anticolic anastomosis
Complications Perioperative:
Anesthetic complication is warranted in such a procedure like prevention of deep vein thrombosis (DVT), slipping of patient , sciatica nerve and brachial plexus injury by extreme abduction and pressure lateral femoral cutaneus nerve and ulnar nerve injury is recorded lipophilic drugs (barbiturates , benzodiazepines) raised peak respiratory pressure ,, increase incidence of atelectasis 45% [22,30, 31,49]. Careful consideration for the sequealae of LRyGb and awareness of the consequences is mandatory. Low molecular weight heparin enoxaparin 40 mg /12h or nadroparin 5700 once daily is protective and not associated with increased incidence of bleeding using graduated compressing stockings to lower limb during after the procedure while patient in bed leg exercise (cycling , stretching) is beneficial, incentive spirometry preoperative consultation with cardiologist and pulmonologist is warranted specialty with patient with many comorbedities [30,31] Suturing of the orogastric tube is recorded during gastroijejunostomy anesthetist should withdraw the tube to adequate level [10]. Hhemorrhage during the procedure is not un common adequate laparoscopic experience would manage such a problem.
Early Postoperative Complications:

A: Leakage is on of the most reported complications in literature .leakage at the gastrojejunal pouch anastomosis is reported to be discovered at the 7 th day post operative while leakage at the jejunojejunal anastomosis is reported to be discovered at the 2nd day (4) (16) . it leads to abscess formation or peritonitis, conservative management for gastric pouch leak by aspiration was more than surgical management, for jejunojejunal leak surgical management was the rule. [7,40]. Omental wrap have been tried in two studies as a protective method and no leak was recorded. Early gastrografin study is the gold standard examination and its being done as standard check up test in 2nd day postoperative nevertheless some studies has challenged this test an its benefits but still most of the literature is advising early test and the radiologist awareness of the new anatomy. Helical ct scan is still a good diagnostic test to detect any leakage. One study is advising that during the curve of learning, cases with a lot of comobidities (hypertension ,apnea, diabetes ) should be avoided by surgeons because the percentage of leak are higher, but experience does not preclude leak. Conflicting reports the relation of the age of the patient and leak complications regarding super obesity no increase in complication rate was detected. One study insist on the utilization of drain as early detection of any leak plus radiology. Endoscopy has been also utilized to a lesser extent to detect anastomitic dehiscence and leak [4,5,6,7,11,14,16,20,29,31,39,41,45,48,57]. B- hemorrhage is an early complication of LRyGb intra luminal and extra luminal ,surgeon should realize this possibility and is usually manifested systemically by tachycardia, drop in blood pressure and recurrent hemoglobin level high level of suspicion should be there. Itraluminal hemorrhage will be discrete if nasogastric tube is inserted perioperatively it could appear in the tube till manifested by Melina. Extra luminal hemorrhage could appear in abdominal tube, jejunojejunl bleeding is difficult to recognize, conservative therapy is the rule if patient is thermodynamically stable. Blood transfusion, stopping low molecular heparin, careful endoscopy for gastric pouch bleeding is recorded in literature and is successful. Selective embolisation is also suggested , application of fibrin glue is widely used laparoscopically. Mallory-Weiss tear is recorded early after excessive retching associated with bleeding [50,47,46,5].
C- Richter hernia immediate formation D- Atelectasis is very common good pain control, awareness of nurses ,respiratory therapy ,incentive spirometry ,D- splenic injury E- Wound infection
Late Postoperative Complications:
The most common late surgical complications is intestinal obstruction or stricture of the anastomosis:
1-Stricture formation was recorded more with old transmesocolic anastomosis technique specially at the fixation suture, although it happens with ante colic technique, rare long jejunal limb stricture is recorded and thought to be due to ischemia and prolong hypotension, marginal ulcer formation happens and lead to stricture its thought to be ischemic or to undetected ulcer preoperatively (acid production could happen from parietal cell if the gastric pouch was not as small as possible) wish will encourage stomasl ulcers formation ,,stricture was repaired successfully by balloon dilatation endoscopically.
2- Obstruction is attributed to many causes recorded years after the procedure is done
A: volvulus is common in (LRyGb) reported as common as leak around 4% B: adhesions C: internal hernia
internal hernia markedly decreased with anticolic technique , it was more common transmesocolic with retro colic technique ..,,it happens around the roux jejunal limb (anticolic) ,alimentary),,,,,,,other article with large series mention the benefit of coming from left side anastomotic jejunal limb than coming from right side in decreasing number of internal hernia ,internal hernia it happens also paraduodenal ,at foramen of Winslow, pericecal ,intersigmoid. Helical CT scan is a gold standard test , it appears as mushroom shape of hernia ,mesenteric fat surrounded by small bowl loops posterior to superior mesenteric artery,jejunal anastomosis located at right side ..
D: ventral hernia The late-onset type Frequent hernia Protrusion of the intestine and/or omentum
E: Bbezoars: Rare type reported as hemorrhagic bezoars
F: Intussusceptions: Reported postoperatively as far as 4 years but rare
G: Superior mesenteric artery syndrome: rare syndrome reported as 3rd part of duodenum distension due to obstruction by superior mesenteric artery pressure its thought its due rapid weight loss..Treated by laparoscopic duodojejunostomy successfully
3- Gastro gastric fistulae are common as 6% in one series, late complication discovered incidentally some time by endoscopy thought to be due incomplete separation of the gastric pouch or leak followed by formation of an abscess and followed by fistulisation of the abscess. Its manifested by slow weight loss recurrent nonspecific abdominal pain. [1/2/3/4/9/12/14/16/18/24/28/29/34/41/42]
COPLICATIONS RELATED TO THE MALABSORPTION SYNDROME
THESE COPLICATION IS DUE OF CREATION OF THE MALLABSORPTION EFFECT ITS DIVERSE NOT FULLY UDERSTOOD.
A -Renal oxalate nephropathy post LRyGb is will recorded it may be the cause of oxalate renal stones there is conflicting reports regarding the formation of renal stones some studies denies increase incidence of renal stones ,,but all studies report about the existence of enteric hyperoxaluria ,,other than that less urinary calcium is excreted and less citrate.
B -Bone Many studies monitored calcium metabolism and bone resorption rate. Increase bone resorption rate between 3 to 6 month postoperatively. Decrease in bone mass, osteoporotic patient candidate for LRyGb should be carefully monitored. Calcium supplement are given for almost all bypass surgery as prophylactic.
C -Cholilithiasis Its will known that obese patient are stone formers. All type of bariatric surgery report the increase of gall bladder stone as high as 30% to 40%, the dilemma hear whether to perform lapcholycestectomy (lpc)on a routine base during LRyGb . Which is justified . or wait till patient is symptomatic, although doing (lpc) will increase time of operatio , time of hospitalization and possible intra operative complications on the other hand waiting could increase the complication of gallbladder stone (pancreatitis ,cholycestitis ). Selective management is applicable. Literature advice intraoperative gall bladder ultrasound to detect stones followed by (lpc), no evidence till now that expectant management will increase complications , cholycestectomy is easier to perform post weight loss ,avoid intraoperative complication of (lpc) with a major LRyGb. Some study advocate the use of ursodiol for 6 month postoperatively as protection, still need to estimate the true cost of such approach ,other study relate this practice to the level of bypass or expected weight loss.
D—Nutritional effect, vitamin, electrolyte, iron and folic acid deficiency: Malabsorption syndrome is will known in literature due to many causes other than LRyGb .. magnesium and phosphate deficiency is recorded , lipophylic vitamin deficiency (A,D,E,K) ,B1 ,B12,iron ,folat deficiency ,the consequence of such loss is sever ,,(see below) ,physiologic enlargement of the stoma and change in gut adipocyte hormone (ghrelin,leptin). Patient should be monitored periodically for loss ,,now surgeons give multivitamin , iron ,nutritional supplement routinely, no consensus on specific regime was found [15/17/19 /44/33].
E—NEUROLOGICAL MANIFESTATIUONS ; Aaround 4% developed mononeuropathy (carpal tunnel syndrome ) ,polyneuropathy ,,polyradiculopathy , optic neuropathy ,wernicke encephalopathy , myopathy ,occurred as acute syndromes(around 6 weeks post surgery) but as far back as 6 month to 8 years are recorded .. encephalopathy and peripheral neuropathy are related to vitamin B1 deficiency ,(bariatric beriberi), patient responded to thiamine supplement between 3 to 6 month ,, vitamin B12 deficiency detected almost in 70% of post LRyGb ..Patient..of vitamin B12 deficiency associated with parethesias ,loss of cutaneous sensation ,weakness , decreased reflexes , incontinence, loss of vision, spasticity , dementia, ataxia , psychosis . and. mood swings. Vitamin B1 and B12 deficiencies could lead to irreversible neurological manifestations[37/17/19/21/56]. Myelopathy (posterolateral) occurred late after a decade it was the most frequent disabling problem, folat deficiency ,niacin deficiency : cause hyperkeratosis, hyper pigmentation,desquamation.,glossitis , diarrhea ,fatigue ,hallucinations and encephalopathy. Vitamin D deficiency can cause hypocalcaemia, serum calcium level is observed to be at it lowest normal level, decrease renal calcium excretion .increase bone metabolism manifested as carp pedal spasm ,facial twitching and ophthalmoplegia years after Copper deficiency may cause myelopathy and neuromusculoskeltal symptoms described to rabid fat metabolism is reported but no consensus regarding this syndrome it still need to have hard evidence but changes in gut adipocyte hormone are recorded.
F Psychological disorder; mood swings, psychosis, dementia are described one article is describing a food phobia after one year of LRyGb.
G—Infertility; infertility clinic is reporting some referrals of secondary azoospermy for preoperative fertile men [8,13,15,17,19,21,23,25,26,32,33,37,38,44,52,53,54,55,56]
REFERENCES AND SOURCES:
Surgical Text Book of (Schwartz’s)
- AGastrogastric fistula: a possible complication of Roux-en-Y gastric bypass. AJ Filho, W Kondo, LS Nassif ,,,,, JSLS, July 1, 2006; 10(3): 326-31.
- Intussusception after Roux-en-Y gastric bypass MA Edwards, R Grinbaum,,,,Surg Obes Relat Dis, July 1, 2006; 2(4): 483-9
- Superior mesenteric artery syndrome, D Goitein, DJ Gagne, Obes Surg, August 1, 2004; 14(7): 1008-11.
- Bypass Leak Complications, J. Stephen Marshall, MD; Anil Srivastava, Arch Surg. 2003;138:520-524.
- . Complications of Laparoscopic Roux-en-Y Gastric Bypass Surgery: Clinical and Imaging Findings, Arye Blachar, MD, Michael P. University of Pittsburgh Medical Center, 1 From the Department of Radiology (A.B., M.P.F., K.M.P.) and the Center for Minimally Invasive Surgery
- complications are not increased in super-super obese, DS Tichansky, EJ DeMaria, Surg Endosc, July 1, 2005; 19(7): 939-41.
- Omental wrap: a simple technique for reinforcement, Department of Surgery, Michigan State University, Kalamazoo Center for Medical Studies,
- Orogastric tube complications, BS Sanchez, BY SafadiObes Surg, April 1, 2006; 16(4): 443-7.
- Normal Appearance and Spectrum of Complications at Imaging1 Elmar M. Merkle, MD, Peter Department of Radiology, Duke University Medical Center,
- The tethered bezoar as a delayed complication of laparoscopJS Pratt, M Van Noord,,,,J Gastrointest Surg, May 1, 2007; 11(5): 690-2.
- Metabolic Syndrome Following Roux-en-Y Gastric Bypass SurgeryDetection of Strictures on Upper Gastrointestinal Tract Radiographic Examinations After Laparoscopic Roux-En-YSaurabh Jha1, Marc S. LevineDepartment of Radiology, Hospital of the University of Pennsylvania
- Long-Term Impact of Bariatric Surgery on Body Weight, Comorbidities, and Nutritional StatuMeena Shah, Vinaya Simha Division of Nutrition and Metabolic Diseases.University of Texas Southwestern Medical Center at Dallas, Dallas, TexUsing Radiography to Reveal Chronic Jejunal Ischemia as a Complication of Gastric Bypass SurgeryRoss Silver1, Marc S. Levine1 Department of Radiology, Hospital of the University of Pennsylvania, 3400 Spruce St., Philadelphia, PA 19104.Neurologic complications of gastric bypass surgery for morbid obesityKatalin Juhasz-Pocsine, MD, Stacy A. Rudnicki, MD, Department of Neurology, University of Arkansas for Medical SciencesInternal Hernia After Gastric Bypass: Sensitivity and Specificity of Seven CT Signs with Surgical Correlation and ControlsMark E. Lockhart1, Franklin N. Tessler Department of Radiology, University of Alabama at Birmingham
- The Neurological Complications of Bariatric Surgery
- Joseph R. Berger, MD Arch Neurol. 2004;61:1185-11Obesity currently ranks as the seventh leading cause of death in the United States.89.
- Perioperative Morbidity Associated With Bariatric Surgery
- Robert W. O’Rourke, MD; Jason Andrus, Arch Surg. 2006;141:262-268.
- Acute Psychotic Disorder After Gastric Bypass
- Wei Jiang, M.D., Jane P. Gagliardi, M.D Am J Psychiatry 163:15-19, January 2006
- Anesthetic Considerations for Bariatric Surgery
- Babatunde O. Ogunnaike, MD*, Stephanie B. Jones, MD, University of Texas Southwestern Medical Center Southwestern Center for Minimally Invasive Surgery
- Trocar Site Hernia, Hitoshi Tonouchi, MD, PhD; Yukinari Ohmori, MD, Arch Surg. 2004;139:1248-1256
- Secondary male factor infertility after Roux-en-Y gastric bypass for morbid obesity
- Antonio Scotto di Frega1, Brian Dale1,II Università degli Studi di Napoli, Centre for Reproductive Biology
- True Fractional Calcium Absorption is Decreased After Roux-En-Y Gastric Bypass Surgery , Claudia S. Riedt*, Robert E. Brolin Department of Nutritional Sciences, Rutgers University, New Jersey
- Population-based Study of Trends, Costs, and Complications of Weight Loss Surgeries from 1990 to 2002, Chetna Mehrotra*, Mary SerdulaCenters for Disease Control and Prevention, Atlanta, Georgia.
- Review of Internal Hernias: Radiographic and Clinical FindingsLucie C. Martin1, Elmar M. Merkle1Department of Radiology, Duke University Medical Center, Box 3808, Durham, NC 2771029Normal Anatomy and Complications after Gastric Bypass Surgery: Helical CT Findings1Jinxing Yu, MD, Mary Ann TurnerDepartments of Radiologyand Surgery,,VCUHS/MCV Hospitals and Physicians, Richmond, Received April 7, 2003
- Cardiorespiratory Fitness and Short-term Complications After Bariatric Surgery* Peter A. McCullough, MD, MPH; Michael J. GallaghDivisions of Cardiologyer, MD; Beaumont Hospital, 4949 Coolidge Hwy, Royal Oak
- Hemodynamic Changes During Laparoscopic Gastric Bypass ProceduresDominick Artuso, MD; Michael Wayne, Arch Surg. 2005;140:289-292.
- A Rational Approach to Cholelithiasis in Bariatric Surgery Paul E. O'Brien, MD, FRACS; John B. Dixon, MBBS, FRACGP Arch Surg. 2003;138:908-912.
- Nutrition and Gastrointestinal Complications of Bariatric Surgery Scott A. Shikora, MD, FACS, Julie J. Kim, MD Obesity Consult Center, Center for Minimally Invasive Obesity Surgery, Tufts–New England Medical Center, Boston, Massachusetts
- Diagnosis of Transmesocolic Internal Hernia as a Complication of Retrocolic Gastric Bypass: CT Imaging Criteria Department of Radiology, Baylor University Medical Center, 3500 Gaston Ave., Dallas, TX 75231 Suraj A. Reddy1, Caroline Yang1
- Belsey Mark IV After Roux-en-Y Gastric Bypass
- Postoperative Nursing Care of Gastric Bypass Patients By Melissa M. Barth, RN, MS, CCRN and Carole E. Jenson Mayo Clinic College of Medicine, Mayo Clinic-Rochester, Rochester, Minn
- Biofeedback-Assisted Relaxation, Exposure, and Cognitive-Behavioral Treatment of Gastric Bypass Surgery Related Anxiety Nicholas A. Lind Jeffrey A. Cigrang Wright-PattersonMedical Center
- Gastric Bypass Surgery for Morbid Obesity Leads to an Increase in Bone Turnover and a Decrease in Bone Mass Penelope S. Coates, John D. Fernstrom Osteoporosis Prevention and Treatment Center (P.S.C., S.L.G.), University of Pittsburgh, Pittsburgh, Pennsylvania 1
- Does experience preclude leaks in laparoscopic gastric bypass? Volume 20, Number 11 / November, 2006 SpringerLink Date Friday, September 08, 2006
- Alan A. Saber1 and Ollie Jackson1 Section of Minimally Invasive Surgery and Bariatric Surgery, Michigan State University/Kalamazoo Center for Medical Studies, 1000 Oakland Dr., Kalamazoo, MI, 49008, USA omental wrap prvent leak 124 case
- Experience with over 3,400 open and laparoscopic bariatric procedures: Multivariate analysis of factors related to leak and resultant mortality Volume 18, Number 2 / February, 2004 Z. Fernandez Jr1, E. J. DeMaria1 The Orientation of the Antecolic Roux Limb Markedly Affects the Incidence of Internal Hernias after Laparoscopic Gastric Bypass Brian B Quebbemann1 and Ramsey M Dallal2 Volume 15, Number 6 / June, 2005
- Endoscopy after Roux-en-Ygastricbypass: a community hospital experience. BJ Marano Jr Obes Surg, March 1, 2005; 15(3): 342-5.
- Inpatient Pain Medication Requirements after Laparoscopic Gastric BypassDepartment of Surgery, University of Tennessee Health Science Center, Memphis, TN, USA Atul K Madan1, Craig A Ternovits2 Department of Surgery, University of Tennessee Health Science Center, Memphis, TN, USA Springer New York Volume 15, Number 6 / June, 2005,
- Effects of Weight Loss after Biliopancreatic Diversion on Metabolism and Cardiovascular ProfileRosa Palomar1, Gema Fernández-Fresnedo2 Department of Nephrology, Hospital Marqués de Valdecilla, University of Cantabria, Santander, Spain Springer New YorkVolume 15, Number 6 / June, 2005
- Endoscopy after Roux-en-Ygastricbypass: a community hospital experience. BJ Marano Jr Obes Surg, March 1, 2005; 15(3): 342-5
- Mallory-Weiss tear after laparoscopic Roux-en-Ygastricbypass. AK Madan, SJ Kuykendall 4th, CA Ternovits, and DS Tichansky Surg Obes Relat Dis, September 1, 2005; 1(5): 500-2
- Management of acute bleeding after laparoscopic Roux-en-Ygastricbypass. A Mehran, S Szomstein, N Zundel, and R Rosenthal Obes Surg, December 1, 2003; 13(6): 842-7.
- The utility of contrast studies and drains in the management of patients after Roux-en-Ygastricbypass. F Serafini, W Anderson, P Ghassemi, J Poklepovic, and MM Murr Obes Surg, February 1, 2002; 12(1): 34-8.
- An approach to venous thromboembolism prophylaxis in laparoscopic Roux-en-Ygastricbypass surgery. MT Miller and PF Rovito Obes Surg, June 1, 2004; 14(6): 731-7.
- Applications of Fibrin Sealant in SurgeryMeng-G Martin Lee, MD Department of Surgery, Beth Israel Deaconess Medical Center, Boston, MA
- Routine abdominal drains after laparoscopicRoux-en-Y gastricbypass: a retrospective review of 593 patients. E Chousleb, S Szomstein, D Podkameni, F Soto, E Lomenzo, G Higa, C Kennedy, A Villares, F Arias, P Antozzi, N Zundel, and R Rosenthal Obes Surg, October 1, 2004; 14(9): 1203-7.
- Prophylactic Cholecystectomy with Gastric Bypass Operation: Incidence of Gallbladder Disease Volume 12, Number 3 / June, 2002 SpringerLink Date Wednesday, August 29, 2007 Mal Fobi1, Hoil Lee2
- Elective Cholecystectomy During Laparoscopic Roux-En-Y Gastric Bypass: Is it Worth the Wait? Volume 13, Number 1 / February, 2003 SpringerLink Date,,,,, Tuesday, August 28, 2007 Giselle G Hamad1, Sayeed Ikramuddin25
- Is Routine Cholecystectomy Required During Laparoscopic Gastric Bypass? Leonardo Villegas1, Benjamin Schneider2 Volume 14, Number 1 / January, 2004 SpringerLink Date, Friday, August 24, 2007
- Prevention or surgical treatment of gallstones in patients undergoing gastric bypass surgery for obesityCurrent Treatment Options in Gastroenterology Current Medicine Group LLC. Volume 7, Number 2 / April, 2004 SpringerLink Date,,,,,,,,, Monday, June 04, 200756 Postgastrectomy polyneuropathy with thiamine deficiencyH Koikea, K Misua, J Neurol Neurosurg Psychiatry 2001;71:357-362 (September)
- Avoidance of Complications in Older Patients and Medicare Recipients Undergoing Gastric Bypass Peter T. Hallowell, MD; Thomas A. Stellato Arch Surg. 2007;142:506-512.






