DR. BAHARAK TOLOUEI ; MD. D.MAS.
General Surgery Specialist And Laparoscopic Surgeon Member Of Iranian Association Of Surgeon Member Of Iranian Doctors Association Member Of World Association Of Laparoscopic Surgeon
Project submitted towards completion of Diploma in Minimal Access Surgery, World Laparoscopy Hospital, India 110018
ABSTRACT
Intestinal obstruction is an abdominal emergency; it is a common reason for surgical referral. There are so many studies that demonstrated the feasibility of laparoscopy in management of acute adhesive small bowel obstruction. In traditional approach, if conservative managements are unsuccessful, laparotomy will be performed.
Causes of acute intestinal obstruction are: Intussusceptions, incarcerated hernias, malrotation of bowel with midgut volvulus, post operative adhesions, annular pancreas, mesocolic hernia, necrotizing entrocolitis. The aim of this study was to compare laparoscopy and laparotomy for the treatment of adhesive small bowel obstruction. For many years previous abdominal surgery and intestinal obstruction were a contraindication to laparoscopy.
CONCLUSION
Laparoscopic adhesiolysis is an effective treatment for small bowel obstruction, morbidity is lower, hospital stay is shorter than patients with open surgery, and resumption of a normal diet is faster.
KEY WORDS
Key words: Small- bowel obstruction-Laparoscopy-Adhesiolysis
INTRODUCTION
Adhesion following abdominal and pelvic surgery is important in view of their morbidity and frequent hospital re-admission.Patients with intraperitoneal adhesions may develop chronic symptoms or present acutely with intestinal obstruction.Acute adhesive intestinal obstruction is the most common reason for emergency admission.re-admission to hospital.The obstruction is almost always in the small bowel, although the level of obstruction varies. The condition is readily diagnosed by the clinical symptoms and signs and abdominal plain film (erect and supine)(1). Laparoscopy adhesiolysis has been practiced by Semm and others for many years, but was confined and parietal peritoneal adhesions. With the rapid improvement in laparoscopic technology this approach is feasible for some patients with early or incomplete small bowel obstruction (2). All patients had well hospitalized repetitive pain triggered by either position, movement or food.
AIM
Safety and feasibility of laparoscopy in the management of adhesive small bowel obstruction are studied. This study is a comparative study between open surgery and laparoscopic surgery and outcome of these two procedures, based on postoperative hospitality. The need for re-admission and additional surgery, resumption of normal diet, morbidity and first bowel movement.
PATIENTS AND METHODS
A literature search was performed using search engine Google, Online Springer, High wire press, library facility available at World Laparoscopy Hospital. Many different pathologic processes can cause adhesions.
PATHOLOGY OF ADHESIONS
- Open abdominal or pelvic surgery
- Individual susceptibility
- Ischemic areas-anastigmatic sites, retroperitonealization of raw areas.
- Foreign bodies-talc, starch granules, gauze lint, cellulose etc.
- Peritonitis from any cause
- Inflammatory bowel disease-chron’s disease
- Radiation enteritis
- Sclerosing peritonitis-usually drug induced, e.g. certain beta-blockers (3).
The most common category is adhesion due to operation. There is definitely an individual’s susceptibility as some patients are prone to adhesions and others not, even after major operations, by the genetics and molecular biological basis for this predisposition to adhesion formation are unknown. Talc and surgical gloves are in no longer a problem. Either incorporate a hydrogel polymer or are powdered with epichlorohydrinated corn starch. Gauze lint is still important and it is responsible for 25% of cases of intraperitoneal granuloma formation caused by implanted foreign bodies. Ischaemia in the region of surgically constructed anastomoses is caused some post operative adhesions, and following attempts at reperitonealization of raw areas. It is not fully understood that what is the exact pathogenesis of intra abdominal adhesions, but trauma and exposure of the peritoneum and the subsequent biochemical and cellular response to repair this injury are involved.
The initiating step is fibrin deposition, as this is essential for mesothelial repair. There is a fine balance between resurfacing of denuded areas by mesothelial cells and fibrinolysis that removes the initial fibrin structural frame work. Disorder of this fine balance between fibrinolysis by ischaemia and mesothelial repair and other factors is thought to be responsible for adhesion formation after abdominal surgery. As the fibrinolytic activity is compromised, the fibrin matrix persists, becomes invaded by fibrinoblasts and gradually matures into fibrous bands usually within 5-7 days. Adhesions may be visceral (between bowel loops and solid organs) or parietal (between viscera and abdominal walls and diaphragms). Usually both are present in the individual cases.
Disruption of the naturally occurring surface active phospholipids barrier is another factor that is thought to be important in the development of adhesions, which normally keeps the peritoneal membrane lubricated and separates the visceral from the parietal peritoneum. The naturally surface active phospholipids barrier, which protects surfaces such as the alveolar membrane, are dipalmitoylphosphatidyl cholin (DPPC) and unsaturated phosphotidylglycerol (PG).
Surface active phospholipids (SAPL) barrier is composed of multiple layers .The lubricating and protective properties of surface active phospholipids (SAPL) barrier are compromised during surgery and may account for the development of adhesions. There is no proved classification of adhesions, they can be firmly, dense or string like, and or variable spread within the peritoneal cavity, but are usually centered on the operative site and the parietal access wound.
From the pathological view point and symptomatic, parietal adhesions (those binding the intra abdominal contents) to the parietals are more important than inter loop / visceral adhesions.
Adhesions occur after abdominal and pelvic surgery
Even with the best operative technique, emergency surgery for acute peritonitis, elective surgery on the small bowel intestine, colon and pelvis is a significant risk factor and there is an increasing argument for specific prophylaxis after these operations. Some drugs as like as anticoagulants, dextrans of various molecular sizes, antihistamines, non -steroidal anti inflammatory drugs (NSAIDS), povidone, streptokinase etc have been shown to be effective as chemo prophylactic agents against adhesion formation.
There is numerous studies that demonstrated one proven prophylactic treatment is that should be considered in these patients. This consists of a bio resorbable membrane based on sodium hyaloronate (seprafilm) which is placed on the front of the intestinal loops, greater omentum separating them from the parietal wound. This membrane is used and has been shown to be entirely safe (no detectable adverse effect) and in a prospective randomized trial of patients undergoing colectomy and ileal pouch anal anastomosis significantly reduced the incidences of adhesions (15 vs. 58 %).
A synthetic mixture of surface active phospholipids (DPPC and PG –proprietary name ALEC) has been used in experimental studies based on the role of surface active phospholipids (SAPL) barrier in peritoneal lubrication and its disruption by open surgery, and shown to reduce adhesions by 70%.
The product is available in powder form (identical to surfactant used in neonatal respiratory problems ) and is jet sprinkled into the peritoneal cavity at the end of the procedure , clinical studies are ongoing in patients undergoing emergency operations with ALEC but to date there are no published results(5,6).
The other anti adhesion agent of interest is a 4 % icodextrin solution (ADEPT) used in peritoneal dialysis extensively.Icodextrin has been studied experimentally and in one clinical trial against ringer’s solution in gynecological laparoscopic surgery as these patients do not form peritoneal adhesions. It reduced the incidence, severity and extent of adhesions in both instances.
However, its efficacy in general surgical practice is unproven, it has several advantages. These include proven non toxicity, low cost and ease of administration, i.e. one liter of the solution is instilled in the peritoneal cavity at the end of operation. This solution is contraindicated in patients with known allergy to starch based polymerase and patients with maltose or isomaltose intolerance.
Some adhesion barrier membrane like as Gore Tex and Interceede was also tried , because these absorbable membrane separate peritoneal membrane from adhered organ and thus prevent fibrous bands from binding different structure.Gore Tex is non absorbable non reactive surgical membrane, and Interceede is an absorbable fabric of oxidized regenerated cellulose. Good result after using these membranes are reported.
In laparoscopic procedure for adhesive small bowel obstruction also some fluid can be left inside after adhesiolysis to prevent recurrence. Antihistamines and steroids were tried but are used infrequent because of adverse effect high risk of dehiscence and delayed wound healing. High molecular dextran is absorbed over a period of 6-9 days, so it was tried to prevent re adhesions.
The osmotic effect of dextran draws the fluid into the peritoneal cavity and the mobile peritoneal organ floats reducing adherence between intraperitoneal organs. Although many studies in animal have demonstrated reduced postoperative adhesion, it is not fully confirm for its efficacy (5, 6).
The morbidity spectrums of intraperitoneal adhesions include:
- Chronic pain
- Acute and sub acute intestinal obstruction
- Secondary female infertility
- Increased opening time for subsequent operations
- Risk (20%) of iatrogenic bowel injuries subsequent operation (4).
Although estimates of the incidence of adhesions vary (40-49), all the reports indicate that the problem is substantial and results in both a significant morbidity and major added health care costs (5).
Complication of adhesions requiring re-admission to hospital are much more frequent after surgery on the small bowel obstruction developed in 25% of patients after total colectomy with ileo-anal pouch reconstruction in one large reported series of 1005 patient.
Approximately 70% of all hospital admission for small bowel is due to adhesion (5). Small bowel obstruction in patients was diagnosed before surgery based on clinical Symptoms, signs and radiologic studies (X-ray and CT scan).
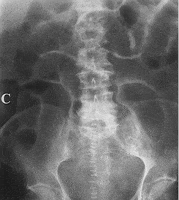
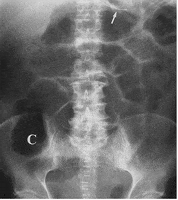
Adhesive small bowel obstruction in 52 years old woman
Supine and upright abdominal radiography reveals dilated gas-filled loops of small Scattered throughout the abdomen the obstruction site (6).Abdominal radiographs can be entirely normal in patient with complete, strangulation and closed loop obstruction (7, 8).
If the results of physical examination and the patient” clinical profile are consistent with intestinal obstruction deposit normal abdominal radiographs, abdominal ultrasonography, ct scanning or fast MRI should be performed immediately (9).CT usually enables one, to confirm the diagnosis of small bowel obstruction. The influence of CT- scan in the management of small bowel obstruction in the acute setting has been well documented (9). Preoperative broad-spectrum parentral anti biotic and external sequential pneumatic compression stockings with subcutaneous heparin were routinely used (10,11).The surgical approach was selected depending on the surgeon’s preference and the patient” condition.
Prognosis of small- bowel obstruction depends on the location and source of obstruction. With early diagnosis and treatment, the prognosis is good (12).For the first port insertion, the open Hasson technique was used, in the lateral abdomen away from any previous incisions. The most common cause of intestinal obstruction in children age and infant is Intussusception. It occurs when a part of the intestine invaginates into the lumen of another distal segment. The peak age of presentation is between 5 and 10 months, and is more common in males. Most intussusceptions are idiopathic. A lead point is identified in only 2-7 % of cases. In some patients recognizable lead points are found, such as intestinal polyp, meckel diverticulum, lymphosarcumas and rarely, foreign bodies.
At any time in life Intussusception can occur, yet the idiopathic form is primarily childhood developing especially during infancy. Usually intussusception causes a sudden onset of sever colicky abdominal pain. Children appear healthy between paroxysms of pain. The classic triad described for intussusception, which consist of colicky abdominal pain, current jelly stools and a palpable abdominal mass. Post operative intussusception occur s within 2-3 weeks after an extensive retroperitoneal approach (wilms tumor or neuroblastoma). A laparoscopic variation of the Ladd procedure has been used in some center. Good visualization of the entire bowel, expert surgeon is needed for laparoscopic approach.
Incarcerated hernia
When the contents of a hernia sac can not be reduced back into the abdominal cavity incarcerated hernia occur. Incarcerated hernia can be umbilical, inguinal or femoral. The vast majority of inguinal hernias in children are indirect hernias. Incarceration represents the most common complication associated with inguinal hernias. Umbilical hernias are common in children, often close spontaneously and rarely incarcerate. The male to female ratio for incarcerated hernias is 8.5:1. Female often have bilateral hernias. The presentation of inguinal hernia in most patients is during the first year of life. An incarcerated hernia is usually associated with signs and symptoms of bilious vomiting, abdominal distention, intestinal obstruction, constipation, obstruction. Incarcerated or non reducible hernias may contain omentum, appendix small bowel, meckle diverticulum (litter hernia).In girls, fallopian tube, the ovary, or both are usuall.The only contra indication to non operative reduction is a long standing incarceration. Incarcerated hernia is a contraindication of laparoscopy, but in many studies some patients undergoing laparoscopy with incarcerated ventral hernia and incarcerated obturator hernia.
Malrotation of bowel with midgut volvulus
Errors of midgut rotation around the superior mesenteric artery may cause intestinal malrotation. Malrotation is always present in patients with gastroschisis, omphalocele, and patients with diaphragmatic hernia. It is associated with acquired and congenital lesions of the GI tract, such as intussusception, Hirschprung disease, and atresia of jejunum, duodenum, and esophagus.
The most common form of malrotation occurs whenever rotation is incomplete and the ligament of treitz or the cecum is abnormally located or fixed.Complet volvulus of the bowels leading to complete necrosis of the involvement organ.
The hallmark of acute midgut volvulus is the sudden onset of bilious vomiting; a palpable mass may not be evident.Theories of malrotation are based on anatomical and pathologic findings, resent evidence suggested that midgut never rotate around the superior mesenteric artery and the final normal position of the midgut is probably due to differential growth of specific intestinal segments. Preserving intestinal viability requires rapid diagnosis and surgery for malformation. A Ladd procedure is the preferred treatment that is possible in laparoscopic approach.
Annular pancreas
This condition is rare and involves a lesion that consists of a thin flat ring of histologically normal pancreas surrounds the descending duodenum in an anomalous position. An annular pancreas can be asymptomatic or can cause external compression of second portion of the duodenum, which creates a partial or compete obstruction. Surgical management of annular pancreas is similar to that of duodenal atresia.A few rare cases are reported that surgical correction was completely laparoscopic with 3 mm instruments. The operation consisted of reduction of the volvulated bowel loops, division of obstructing bands, and creation of side to side duodenoduodenostomy. In compare with laparotomy it has all the potential benefits.
Mesocolic hernia
Mesocolic hernia is a malrotation abnormality. Exact incidence is still unknown. They are rather rare, non fixed colonic and duodenal mesenteries lead to potential hernia pouches, which transiently and recurrently entrap the bowel and cause partial obstruction. Surgically reduce the hernia and repair the potential hernia pouch but laparoscopy is not reported.
Necrotizing entrocolitis
Stricture from previous necrotizing enter colitis occur usually in premature infants. NEC can produce stricture that subsequently cause intestinal obstruction.Indication for surgery in necrotizing entrocolitis includes pnemoperitoneum, fixed dilated loops, children whose conditions deteriorate or show no improvement with conservative therapy. There is no evidence of benefit of laparoscopy approach.
CONTRA INDICATIONS
The absolute and relative contraindications to laparoscopy in treatment of abdominal emergencies are the same as for elective procedure (13, 14, 15, 16).
- Uncorrecte coagolopathy
- Hemodynamic instability
- Abdominal wall infection
- Sever cardiopulmonary disease
- Multiple previous upper abdominal procedures.
Patients who underwent laparoscopy and laparotomy were evaluated and compared with respect to number of previous operations and episodes of small bowel obstruction.However, the main technique for adhesiolysis with the last possibility for reformation can be described as” cold scissors dissection” with bipolar backup.
Four different laparoscope, a 10 mm 0 degree straight viewing laparoscope; a 10 mm operative laparoscope with 5 mm operating channel, a 5 mm straight viewing laparoscope for introduction through 5 mm trocar sleeves, and an oblique-angle laparoscope(30-40) for upper abdominal and pelvic procedure should be available(17).Scissors are the preferred instrument to cut adhesions, especially avascular and or congenital adhesions. Using the magnification afford by the laparoscope, most anterior abdominal wall, pelvic, and bowel adhesions can be carefully inspected. Pushing tissue with the partially open blunt scissors tip is used to develop natural planes. To facilitate direction changes, the scissors should not be too long or encumbered by an electrical cord. Sharp dissection is the primary technique used for adhesiolysis to diminish the potential for adhesion formation (18).Adhesiolysis by laparotomy and laparoscopy can be very-consuming and technically difficult.
All laparoscopic surgical procedures are done under general anesthesia, endotracheal intubation and an orogastric tube is placed routinely to diminish the possibility of a trocar injury to the stomach and to reduce small bowel distention. A Foley catheter is inserted if bladder is distended or a long operation anticipated, A catheter is inserted near the end of the operation and removed in the recovery room when the patient is aware of its presence, to prevent bladder distention. The patient” position is flat 0 degree during introducing the first trocar but after that a steep trendelenburg position 30 degrees , reverse trendelenburg position, and side to side rotation are used(19).
An open adhesiolysis is performed in the exact same as a laparoscopic adhesiolysis. First, all adhesions with the metzenbaum scissors are taken down from the abdominal wall. Second, all loops of bowel are extracted. Finally, all inter loop adhesions are lysed from ligament of treitz to the ileo-cecal valve (20).
Next, free all bowel loops in the pelvis. Small bowel attached to the vesicouterine peritoneal fold, uterus or vaginal cuff, and the rectum is liberator. Three points are that should be considered when performing bowel adhesiolysis within the pelvis: dissection with scissors without electro surgery, counter traction and blunt dissection. The bowel is gently held with an atraumatic grasper and lifted away from the structure to which it is adhered, exposing the plane of dissection (20). All data were evaluated on an intention-to treat analysis as a laparoscopic procedure.
| LAPAROCOPY GROUP | : | n = 74 |
| Hospital stay (total) | : | 7.5 days |
| First bowel movement | : | 3 days |
| Resumption of normal diet | : | 2nd day |
| Operative time | : | 80 min |
| Morbidity | : | n = 12 (16 %) |
| LAPAROTOMY GROUP | : | n = 74 |
| Hospital stay (total) | : | 14 days |
| First bowel movement | : | 6 days |
| Resumption of normal diet | : | 3rd |
| Operative time | : | 72 min |
| Morbidity | : | n = 34 (45%) |
There were a total of 148 patients in this study. Seventy four in the laparoscopy group, a mean age 52 (range 30-75) years, and 74 in the laparotomy group, a mean age 60(range 22-83) years. Differences of operative time between laparoscopy and laparotomy were noted. The diagnostic accuracy of laparoscopy group was very high, according to the rate (89_100%) (21).Identification of concomitant disease than operation in cases of unclear preoperative diagnosis, laparoscopy can shorten the period avoided the need for expensive laboratory and imaging test (22).The accuracy of radiography in these disease reaches 75%.Where as the accuracy of abdominal ultrasound is 60_89%.The ct scan more accurate 84_98%, But it is not always available in every hospital situation(23).The hospital stay after laparoscopy is shorter when compared with open controls, and patients experience a faster recovery (25, 26).
DISCUSSION
Laparoscopy allows to perform the same surgical procedure as open surgery, or even to schedule the appropriate medical therapy in the presence of concomitant disease (26, 27, and 28).
Peritoneal adhesion following open surgery account for 74% of all bowel obstruction. Morbidity associated with a long incision .prolonged post operative pain, prolonged ileus has increased inpatients who requiring surgery for adhesive small bowel obstruction. Usually, laparotomy results in incisional hernia formation and further adhesion formation, with a re-admission rate of at least 32% (29-30).
Laparoscopy surgery, with reduced surgical trauma, hospital stay, morbidity such as post operative pain, illeus, post operative complication and subsequent incidence of adhesions and incisional hernias , may offer advantages to patients undergoing surgery for adhesive small bowel obstruction.
In previous study, retrospectively compared the results of laparoscopy for adhesive small bowel obstruction, with those of laparotomy, and they found that the complication rate was significantly lower in laparotomy group.Wullstein et al. reported a 26.9% rate of bowel injury in the laparoscopy group versus 13.5% in the laparotomy group (31). In this study, there were statistically significant differences in hospital stay, time to the first bowel movement, and complication rate between the laparoscopy group, and laparotomy group.
Therefore the risk of small bowel perforation during laparoscopy for adhesive small bowel obstruction may be higher than in laparotomy. A meticulous atraumatic technique reduces the risk of small bowel perforation (32).
CONCLUSION
Adhesion formation after operative surgery is common. When compared to laparotomy, laparoscopy has been shown to result in less adhesion formation.All studies have been shown that laparoscopic management of adhesive small bowel obstruction is feasible and faster with a shorter hospital stay.Laparoscopic surgery including less postoperative analgesics and more rapid convalescence increase promptly recovery of gastrointestinal function and return to normal activation.Open adhesiolysis should be reserved for the worst possible cases where laparoscopic adhesiolysis has failed.We conclude that laparoscopy is an excellent diagnostic and traputic modality in acute small bowel obstruction.The majority of which can be simultaneously managed laparoscopically.
REFRENCES
1. Becker, J.M. Dayton, Mt, Fazio, V.M, et al (1990)Prevention of postoperative abdominal adhesions by a sodium hyalouronate-based bioresorbable membrane: a prospective randomized double-blind.JAM Coll Surg 183:297-306
2. Mouret p, Marsaud H. Laparoscopic adhesiotomy and preliminary study.Surg. Endose (in press).
3. Elis, H; Moran, B.J, Thompson, J.N. et al (1999).Adhesion related hospital readmission after abdominal and pelvic surgery: a retrospective cohort study.Lancet 353: 1476-80
4. Peritoneal adhesiolysis (1994). National patient profile 1993.Baltimore:HCIA INC. ,427:653-5
5. Van der kabben ,A.A. ,Dijkstra ,M. Nieuwenhuizen ,M. M. et al. (2000).Morbidity and mortality of inadvertent entrotomy during adhesiotomy. Br J Surg 87:476-471
6.Bender GN, Maglinte DDT.Small bowel obstruction: the need for greater radiologist involvement. Emerg radiol 1997; 4: 337-339.
7. Maglinte DDT, Balthazar EJ, Kelvin FM, Megibow AJ.The role of radiology in the diagnosis of small bowel obstruction. AJRAM J Roentgenol 1997; 1171-1180
8. Balthazar EJ, Birnbaum BA, Megibow AJ, et al. Closed loop and strangulation intestinal obstruction :ct signs .Radiology 1992; 185:769-775.
9. Balthazar EJ. Ct of small bowel obstruction.AJR AMJRoengenol 1994; 162:255-261
10. Spiro DM, Arnold DR, Barbone F: Association between antibiotic use and primaryidiopathic Med 2003 Jan; 157(1):54-9
11. M.Khaikin ,N.Schneidereit,S.Cera,D.Sands ,J.Efron ,E.G.Surg Endosc (2007) 21:742-745
12. Vijay K,Anindya C, Bhanu P,et al :Adhesive small bowel obstruction Malaysia 2005Mar ;60(1):81-4
13. Agresta F, de Simone P, Bedin N: The laparoscopic approach in abdominal emergencies.A single-center 11 years experience.JSLS 2004,8:25-30
14. Agresta F,Michelet I, Colucci G, Bedin N:Emergency laparoscopy. A community hospital experience. Surg Endosc 2000,14:484-487
15. Bailey IS, Rhodes M.O"Rourke N, Nathanson L, Filding G: Laparoscopic management of acute small bowel obstruction. Br J Surg 1998 85(1):84-87
16. Golash V, Willson PD: Eerly laparoscopy as a routine procedure in the nanagementof acute abdominal pain.Surg Endosc 2005, 19:882-885
17. Dizerega GS. Contemporary adhesion prevention. Fertil steril 1994;61:219-235
18. Odel R. Principles of electrosurgery .In Sivak M, et al.Gastroentrologic Endoscopy. New York :Saunders company, 1987: 128J
19. Mc comb PF, Paleologou A. The intussusception salpingostomy technique for the therapy of distal oviductal occlusion at laparoscopy. Obstet Gynecol1991;78:443
20. Reich H.New techniques in advanced laparoscopyic surger. In Sutton C, ed. Laparoscopyic surgery .Bailiere"s clinical obstetrics and gynecology. London: WB Saunders, 1989: 655
21. Sauerlaenad S , Agresta F, Bergamaschi R, Borezellino G , Budzynsky A, Champault G , LaJ?aroscopicfor abdominal emergencies: evidence based guidelines of the European Association for Endoscopic surgery. Surg Endosc 2006 ,20(1):14-29
22. C ueto J, Diazo, Garteiz D, Rodriguze M, Weber A: The efficacy of laparoscopic surgery in the diagnosis and treatment of peritonitis.Experience with 107 cases of Mexico City.Surg Endosc 1997,11:366-370
23. Salem TA, Molloy RG, O”Dwyer PJ: Prospective study on the role of the scan in patients with an acute abdomen.Colorectal Dis 2005 ,7(5):460-6
24. Heinzelmann M, Schob O,Gianom D, Platz A ,Simmen HP:Role of laparoscopy in the management of acute abdomen.Zetralbl Chir 1999,124 (12): 1130-6
25. Larson GM: Laparoscopy for abdominal emergencies.Scand J Gastroenterol 1995 ,208 (30 suppl):62-66
26. Faranda C, Barrat C, Catheline JM, Champault GG: Two stage laparoscopy management of generalized peritonitis due to perforated sigmoid diverticula: eighteen cases.
27. Farooq A, Ammori BJ: Laparoscopic diagnosis and management of primary bacterial peritonoitis. Surg laparosc Endosc percutan tech 2005 ,15(1):36-37.
28. Ramachandran CS, Agrawal S, Goel Dip NBD, Arora V: Laparoscopic surgical management of perforative peritonitis in enteric fever .A Preliminary study. Surg laparosc Endosc percutan tech 2004 ,14(3):122-124
29. Duepree HJ, Senagore AJ, Delaney Cp, Fazio VW (2000)Dose means of access affect the incidence of small bowel obstruction and ventral hernia after bowel resection? Laparoscopy versus laparotomy .J AM Coll Surg 197(2):177-181
30. Miller G,Boman J, Shrier I,Gordon PH (2000) Natural history of patients with adhesive small bowel obstruction.Br J Surg 87(9) 1240-1247
31. Wullstein C, Gross e (2003) laparoscopic compared with conventional treatment of acute adhesive small bowel obstruction.Br J Surg 90(9): 1147-1151
32. Suter M .Zermatten P, Halkic N, Martinet O, Bettschart V (2000) Laparoscopic management of mechanical small bowel obstruction: are there predictors of success or failure?Surg Endosc 14(5):478-483






