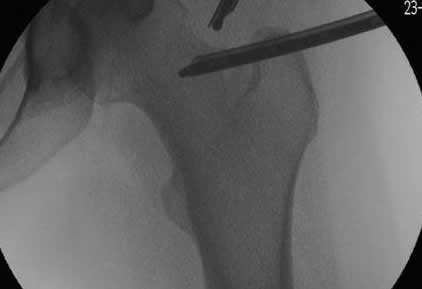
Arthroscopic surgery
Definition
Knee arthroscopic surgery is a procedure carried out through small incisions within the skin to repair injuries to tissues such as ligaments, cartilage, or bone inside the knee joint area. The surgery is conducted with the aid of an arthroscope, which an extremely small tool is guided with a lighted scope mounted on a television monitor. Other devices are placed through three incisions around the knee. Arthroscopic surgeries vary from minor procedures for example flushing or smoothing out bone surfaces or tissue fragments (lavage and debridement) related to osteoarthritis, to the realignment of the dislocated knee and ligament grafting surgeries. The range of surgeries signifies different procedures, risks, and aftercare prerequisites.While the clear advantages of arthrocopic surgery lie in surgery with fewer anesthetics, less cutting, and less recovery time, this surgery nonetheless requires a very comprehensive study of what causes knee injury or pain in front of patient’s decision for surgery.
Purpose
There are many procedures that currently fall under the overall surgical group of knee arthroscopy. They fall under roughly two groups-acute injuries that destabilize the knee, and pain management for floating or displaced cartilage and rough bone. Acute injuries are often the result of traumatic injury to the knee tissues such as ligaments and cartilage through accidents, sports movements, plus some excessive use results in. sensitive injuries include damage to the mechanical features, including ligaments and patella from the knee. These injuries can result in knee instability, severe knee dislocations, and finish lack of knee mobility. Ligament, tendon, and patella placements are key elements from the surgery. The kind of treatment for acute injuries depends in large part on a rigid grading system that rates the injury. For example, grades I and II call for rest support by crutches or leg brace, pain management, and rehabilitation. Grades III and IV indicate the need for surgery. Acute injuries to the four stabilizing ligaments from the knee joint-the anterior cruciate ligament (ACL), the posterior cruciate ligament (PCL), the medial collateral ligament (MCL), and also the lateral collateral ligament (LCL)-as well regarding the "tracking," or seating from the patella, can be highly debilitating. Treatments of those acute injuries include such common surgeries as:
- Repairs of a torn ligament or reconstruction of the ligament.
- Release of the mal-aligned kneecap. This involves tendon surgery release and fit the patella better into its groove.
- Grafts to ligaments to aid smoother tracking of the knee with the femur.
Pain management surgeries, however, are utilized to relieve extreme uneasiness from the knee because of osteoarthritis conditions. These treatments goal at relieving pain and lack of stability brought on by more chronic, "wear and tear" types of conditions and involve minor and more optional surgical procedures to deal with cartilage and bone surfaces. Included in this are arthroscopic techniques to remove detached or obtruding pieces of cartilage within the joint space like the meniscus (a fibrous cushion for the patella), to smooth aged, rough surface bone, or to get rid of parts of the liner of the joint which are inflamed.
Treatment variations between arthroscopic surgery for serious injuries and those for pain management are important and really should be kept in patient’s mind. They've implications for the necessity for surgery, risks of surgery, complications, aftercare, and anticipation for improvement. Arthroscopic surgery for acute injuries is less controversial because clear dysfunction and/or severe lack of stability are measurable signals for surgery and easily recognizable. Surgery indications for pain management are mostly for chronic damage but for the milder grades or stages of acute injuries (severity Grade I and II). They are questionable because of the information on pain management and rehabilitation alternatives.
By whom and where the procedure is performed?
Surgery is performed by an orthopedic doctor, a specialist in joint and bone surgery, trained in arthroscopic surgery. Arthroscopic surgery is usually performed in a general hospital with an outpatient operating suite.
Diagnosis/Preparation
Disease and injury can damage joints, ligaments, cartilage, and bone surfaces. Because the knee carries most of the weight from the body, this damage takes place almost inevitably as people age, because of sports injuries and through accidents. Diagnosing of knee injuries or damage includes a health background, physical examination, x-rays, and the additional, more in depth imaging techniques with MRI or CT scan. Severe or chronic pain and/or knee instability initially brings the individual to an orthopedic physician. After that, patient’s decision is perfect for surgery or for rehabilitation. Aspects that influence the decision for surgery would be the likelihood for repair and recovery of function, the patient's health insurance and age, and, most importantly, the willingness of the patient to think about alterations in lifestyle, especially because this pertains to sport activity. Arthroscopic viewing is easily the most correct tool for diagnosis, and for some repairs. The doctor may provide only a provisional diagnosis before actual surgery but will apprise the individual of the most likely course the surgery will require.
Arthroscopic surgery can be performed under local, regional, or general anesthetic. The kind used relies upon largely on the seriousness of damage, the level of pain after surgery, patient wishes, and patient health. The surgery is brief, under two hours. After closing the incisions, the leg will be wrapped tightly and also the patient is come to recovery. For many same-day surgeries, individuals are allowed to leave once the anesthetic effects normally wear off. Patients are not permitted to drive. Arrangements for get after surgery are mandated.
Unlike open surgery, arthroscopic surgery normally does not require a hospital stay. Patients generally go home exactly the same day. Any crutches or canes required prior to surgery will be needed after surgery. Follow-up visits will be scheduled within about a week, at which dressings will be removed.
Demographics
More than five and a half million people visit orthopedic surgeons each year because of knee problems. Over 600,000 arthroscopic surgeries are performed annually; 85% turn out for knee surgery. One very common knee injury is really a torn anterior cruciate ligament (ACL) that usually happens in athletic activity. The most typical source of ACL injury is skiing. The incidence of ACL injuries in females is two to eight times greater than in males. As the exact causes are not clear, differences in anatomy, strength, or conditioning are thought to experience main roles. Women also seem to be more prone to patella-femoral syndrome (PFS), which is the inability of the patella to track smoothly with the femur. PFS arrives primarily to development of tendons that influence the ways the knee tracks in movement. It is also because of misalignments to other parts of the low body like foot pronation.Other ligament surgeries can be brought on by injury or overuse.
Many of these injuries heal without treatment and go undetected. Many people with multiple traumas in accidents have knee dislocations which go undiagnosed. Knee dislocations are of special concern, particularly in traumatic injury, because their early diagnosis is required if surgery will be effective. Knee dislocations in the morbidly obese individuals often take place instinctively and may be associated with artery injury. This surgery involves difficulties related to the obesity. Finally, knee dislocations have been reported to occur in up to 6% of trampoline-associated accidents.
Description
Arthroscopic surgery for serious injuries: The knee bone sits between patient’s femur and the tibia, attached by four ligaments that keep the knee stable since the leg moves. These ligaments could be damaged or split through injuries and accidents. Once damaged, they do not offer stability to the knee and can cause buckling, or permit the knee to "give way." Ligaments may also "catch" and freeze the knee or result in the knee track in a different direction than its leg movement, causing the knee to dislocate. Traumatic injuries such as car accidents may cause several ligament injuries, necessitating several repairs to ligaments.
Four arthroscopic procedures relate to harm to each one of the four ligaments that stabilize the knee joint movement. The four procedures are:
- Anterior cruciate ligament (ACL). A front-crossing ligament connecting the femur to the tibia through the knee; this ligament maintains the knee from hyperextension or being displaced back in the femur. The ACL is really a rather large ligament that can withstand 500 lb (227 kg) of pressure. If it is split or becomes detached, it remains that way and surgery is pointed out. Within the most severe cases, a graft to the ligament is essential to reattach it towards the bone. The surgery can use tissue in the patient, called an auto graft, or from a cadaver, called an allograft. The patella tendon, which connects the patella towards the tibia, is easily the most commonly used auto graft. ACL reconstructive surgery involves drilling a tunnel into the tibia and also the femur. The graft will be pushed through the tunnels and secured by stapling or sutures.
- Posterior cruciate ligament (PCL). A back-crossing ligament that attaches the front of the femur to back of the tibia behind the knee that retains the knee from hyperextension or being displaced backward, PCL injuries are not as frequent as ACL injuries. These injuries are mostly due to fall on the knee or hitting the knee about the dashboard of a car within an accident. Both displace the tibia too far back and tear the ligament. Surgery towards the PCL is rare, because the split can usually be treated with rest with rehabilitation. If surgery is needed, it is usually to reattach the PCL towards the tibia bone.
- Medial collateral ligament (MCL). It becomes an inside lateral ligament joining the femur and tibia and backing the knee against lateral dislocation left or to the right. The injury is usually due to external pressure from within the knee. Regarding a grade I or II collateral ligament tear, doctors will probably brace the knee for four to six weeks. A grade III tear may need surgery to repair ligament tear and it is followed by 3 months of bracing. Physiotherapy may be required before resuming full activity.
- Lateral collateral ligament (LCL). Some other lateral ligament connecting the femur and tibia and backing the knee against lateral dislocation, In the case of a grade I or II collateral ligament tear, physicians are likely to brace the knee for four to six weeks. A Grade III split may require surgery to reattach the ligament to bone. Surgery will be followed by 3 months of bracing. Physiotherapy might be necessary before returning to full activity.
Patello-femoral syndrome (PFS)
The patella rests in a groove about the femur. Anything but a great fit may cause the patella to be unstable in the movement and very painful. A lot of people have chronic issues with the proper tracking from the patella with the femur. This may be related to conditions related to physical characteristics like foot pronation, in order to the types of body development in exercising or excessive use of muscles. In the case of damage, a test of the cartilage surrounding the patella can determine cartilage that increases friction as the patella moves. Smoothing the damaged cartilage can increase the ease of movement and eliminate pain. Finally, a tendon can occasionally make the patella track off center from the femur. By moving where the tendon is attached through lateral discharge surgery, the patella can be forced back into its groove. Pain management with lavage and debridement.
As well as the ligament and patella surgeries that are mostly necessary for traumatic injuries, arthroscopic surgery treats the damage and tear injuries associated with a torn meniscus, which is the crescent-shaped cartilage that cushions the knee, in addition to injuries to the surface of bone that makes joint movement painful. These are related to osteoarthritis and rheumatoid arthritis symptoms. In lavage and debridement, the doctor recognizes floating or out of place tissue pieces and only flushes those out having a solution applied with arthroscopy or smoothes the surface of bone to diminish pain. All of the above procedures are carried out through the visual images offered by the lighted arthroscope that allows the doctor to follow the surgery on a television monitor. Devices only about 0.15 in (4 mm) thick are introduced inside a triangular fashion around the knee. The arthroscope gets into one incision, and instruments to cut and/or smooth and to engage in other maneuvers are put through the other incisions. On this fashion, the doctor has magnification, perspective, and also the capability to make tiny adjustments to the tissue without open surgery. The triangular approach is highly effective and safe.
Risks
The risks of arthroscopic surgery less difficult less than open surgery, but they are not nonexistent. The chance of any surgery carries by using it danger in the utilization of anesthesia, including heart attacks, strokes, pneumonia, and thrombus. The risks are uncommon; however they increase with the chronological age of the patient. Blood clots would be the most common dangers, but they arise rarely in arthroscopic surgery. Other risks consist of infections at the surgery site or at the skin level, bleeding, and skin scars.
Risks related specifically to arthroscopic surgery are mainly ones associated with injury at the time of surgery. Arteries, veins, and nerves could be injured, resulting in discomfort in minor cases and leg weakness or decreased sensation in more serious complications. These injuries are rare. One major risk of arthropscopic surgery to the knee for problems associated with tissue tears is that the pain might not be relieved through the operation; it might even become worse.
Morbidity and mortality rates
Difficulties occur in less than 1% of arthroscopic surgeries. Different procedures have different complications. In general, morbidity results mostly from medically induced nerve and vascular damage; death or amputations almost never occur. Graft infection may take place, along with other types of infection largely due to microbes introduced with instruments. The latter cases have become progressively scarce since the science of arthroscopic surgery develops.
Normal results
Normal results of ligament surgery are pain, initial immobility and inflexibility, bracing from the leg, crutch dependence, with increasing mobility and flexibility with rehabilitation. Full recovery towards the level of prior exercise can take as much as 3 months. With ACL surgery, pain within the front of the knee happens in 10-20% of individuals. Restricted range of motion occurs in less than 5% because of inadequate keeping the graft. Another surgery might be necessary.
The pain-relieving effects for arthroscopic partial menisectomy (removal of torn areas of cartilage) and debridement (the abrasion of cartilage to make it smooth) are not very reliable.
Aftercare
Ligament- and patella-tracking surgeries: Arthroscopic surgery for serious ligament harms or knee displacement frequently involves ligament grafting. In some instances, including taking tissue from a tendon to use for that graft and drilling holes within the femur or tibia or both. Aftercare requires the use of crutches for six to eight weeks. A rehabilitation program for strengthening is generally suggested. Recovery times for resumed athletic activity are highly determined by age and health. The doctor often makes very careful tests about recovery and the requirement for rehabilitation. Patella-tracking surgeries offer in regards to a 90% chance that the patella won't dislocate. However, lots of people have continued swelling and pain after surgery. These appear to be dependent upon how carefully the rehabilitation plan's developed and/or adhered to through the patient. Lavage and debridement surgeries: Elevation from the leg after surgery is generally necessary for a brief period. A crutch or knee immobilizer adds additional stability and assurance when walking. Physical therapy is usually advised to strengthen the muscles around the knee and also to provide additional support. Special awareness ought to be paid to any changes to the leg a couple of days after surgery. Swelling and pain towards the leg often means a blood clot has been dislodged. If this takes place, problems ought to be informed immediately. Getting up soon after surgery decreases the risk of thrombus.
Alternatives
Whether or not surgical treatment is the greatest choice depends upon a number of variables and choices. Age and also the degree of injury or damage are the key factors to deciding whether to have surgical procedures or rehabilitation. Problems calibrate the severity of acute injuries and only proceeds to established treatment plan immediately or recommend surgery. Alternatives for acute ligament injuries rely on the severity of injury and whether the patient could make change in lifestyle and it is prepared to move from athletic activities. This decision becomes paramount for many people with collateral and cruciate injuries.
Conservative treatment for acute injuries involves RICE: Rest, Ice, Compression, Elevation, as well as a follow-up rehabilitation plan. The RICE protocol involves resting the knee to allow the ligament to heal, applying ice two or three times each day for 15-20 minutes, compression with a bandage or brace, and elevation from the knee whenever you can. Rehabilitation requires range-of-motion exercises to increase flexibility, braces to manage joint immobility, exercise for quadriceps to support the leading of the thigh, and upper thigh exercise having a bicycle. For arthritis-related damage and pain management, anti-inflammatory medication, weight reduction, and use can all be crucial to strengthening the knee to alleviate pain. Evidence suggests that these alternatives are well as surgery.






