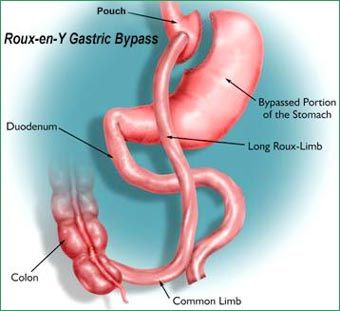
Gastric bypass
Definition
A gastric bypass is a method of surgical treatment that can cause an extremely small stomach; scrap of the stomach is taken away. The small intestine is connected to the new stomach, permitting the lower part of the stomach to become bypassed.
Purpose
Gastric bypass surgery is supposed to treat obesity, an ailment seen as a rise in bodyweight beyond the skeletal and physical needs of the person, leading to excessive putting on weight. The explanation for gastric bypass surgery is the fact that making the stomach smaller an individual struggling with obesity will consume less food and therefore gain less weight. The operation limits intake of food and cuts down the feeling of hunger while giving a sensation of satiety within the new smaller stomach.
Description
Various kinds’ mal-absorptive methods, meaning procedures which are meant to lower calorie intake, enables to perform gastric bypass surgery, which includes:
- laparoscopic RNY bypass
- gastric bypass with long gastrojejunostomy
- vertical gastric bypass
- Roux-en-Y gastric bypass
- transected Roux-en-Y bypass
- biliopancreatic diversion
- distal Roux-en-Y bypass
All procedures try to restrict intake of food and differ within the surgical approach accustomed to produce a smaller stomach. Selection of procedure depends on the patient's all around health status as well as on the surgeon's objective viewpoint and experience. Within the operating room, the individual is first placed under general anesthesia through the anesthesiologist. When the patient is asleep, an endotracheal tube is positioned with the mouth from the patient to the trachea for connecting the individual to some respirator during surgery. A urinary catheter can also be put into the bladder to empty urine during surgery but for the first couple of days after surgery. This enables the surgeon to watch the patient's hydration. A nasogastric (NG) tube can also be placed with the nose to empty secretions and it is usually taken out the morning after surgery.
In many clinics and hospitals, the operation of preference for obese people may be the RNY gastric bypass. The doctor starts by developing a small pouch in the patient's original stomach. When finished, the pouch is going to be totally separated in the remainder from the stomach and can get to be the patient's new stomach. The initial stomach is first divided into two sections. Top of the part is created right into a small pouch concerning the size an egg that may initially hold 30-60 ml, than the 1.2l-1.5 l held with a normal stomach. It's created across the more muscular side from the stomach that makes it not as likely to stretch with time. This process allows food to proceed in the mouth towards the esophagus, to the gastric pouch, after which immediately to the main small bowel known as the jejunum. Food no more would go to the bigger part of the stomach. Because none of the original stomach is taken away, its secretions can go the duodenum. Both areas of the stomach are thus totally separated and therefore are closed by stapling and sewing to get rid of the potential of leaks. Scarring ultimately forms in the stapled and sewn area so the pouch and stomach are permanently divided and sealed. Finally, the physician reconnects part one from the jejunum and also the duodenum comprising the juices in the stomach, pancreas, and liver towards the segment of small bowel which was attached to the gastric pouch.
The opening between patient’s new stomach and also the small bowel is known as stoma. It features a diameter of some 0.8 cm. All food adopts the brand new small stomach and must then go through this narrow stoma before entering the little intestine. Negligence the little intestine in the upper functioning small stomach and also the main small intestine in the initial lower stomach are joined inside a Y connection so the gastric juices can mix using the food from the small pouch. The RNY may also be carried out laparoscopically. It makes sense just like a wide open surgery RNY, with the exception that rather than opening the individual having long incision about the stomach, surgeons creates a small incision and place a pencil-thin optical device, known as a laparoscope, to project an image to one TV monitor. The laparoscopic RNY leads to smaller scars in most cases only 3 to 4 small incisions are created. The typical time necessary to complete the laparoscopic RNY gastric bypass is around 2 hours.
Who performs the process and where could it be carried out?
A gastric bypass is conducted with a board-certified general surgeon that has specialized within the surgical procedure of obese patients. An anesthesiologist accounts for administering anesthesia, and also the operation is conducted inside a hospital setting.
Demographics
The amount of overweight and obese Americans has continuously increased since 1960, and also the trend hasn't slowed up recently. Every year, obesity plays a role in a minimum of 300,000 deaths in the USA, with associated health-care costs amounting to around $100 billion.
Diagnosis/Preparation
An analysis of obesity depends on the patient's health background as well as on an appearance weight evaluation in line with the BMI as well as on waist circumference measurements. Based on the American Obesity Association (AOA), a BMI more than 25 defines overweight and marks the stage where the chance of disease raises from excess fat. A BMI more than 30 defines obesity and marks the stage where the chance of death raises from excess fat. Waist circumference exceeding 101 cm in males and 89 cm in females increases disease risk. Gastric bypass like a weight reduction treatment methods are considered just for seriously obese patients.
To organize for surgery, the individual is asked to reach in the hospital a couple of hours before surgery. Whilst in the preoperative holding room, the individual meets the anesthesiologist who explains the process and answers any queries. An intravenous (IV) lines are placed, and also the patient might be given a sedative to assist relax prior to going towards the operating room.
Important questions a patient should ask a doctor:
- What would be the alternatives?
- How is gastric bypass surgery carried out?
- What would be the advantages of the surgery?
- How long does it decide to try get over the surgery?
- How many gastric bypasses would doctor perform each year?
- When can one be prepared to go back to work and/or continue regular activities?
- What would be the risks of a gastric bypass?
Risks
Gastric bypass surgery has most of the same risks related to every other major abdominal operation. Life-threatening problems or death are uncommon, occurring in less than 1% of patients. Such significant unwanted effects as wound problems, trouble in swallowing food, infections, and extreme nausea may appear in 10-20% of patients. Thrombus after major surgery is uncommon but extremely dangerous, and when they occur may need re-hospitalization and anticoagulants.
Some risks, however, are particular to gastric bypass surgery:
- Abdominal hernias: Fundamental essentials most typical complications needing follow-up surgery. Incisional hernias exist in 10%-20% of patients and need follow-up surgery.
- Gallstones: They develop in additional than the usual third of obese patients going through gastric surgery. Gallstones are clumps of cholesterol along with other matter that build up within the gallbladder. Rapid or major weight reduction increases an individual's risk of building gallstones.
- Leakage of stomach and intestinal contents: Leakage of stomach and intestinal contents in the staple and suture lines to the abdomen may appear. This can be a rare happening and sometimes seals itself. Otherwise, another operation is needed.
- Narrowing from the stoma: The stoma, or opening between patient’s intestines and stomach, can occasionally become too small, causing vomiting. The stoma could be repaired by an outpatient procedure that utilizes a little endoscopic balloon to stretch it.
- Dumping syndrome: Generally occurs when sweet foods are eaten or when meals are eaten prematurely. Once the food enters the small intestine, it causes cramping, sweating, and nausea.
Due to the alterations in digestion after gastric bypass surgery, patients may acquire such lacking as anemia, osteoporosis, and metabolic bone disease. These deficiencies could be prevented if patient take iron, calcium, Vitamin B12 and folate supplements. It's also vital that patient maintain hydration and intake of high-quality protein and essential fat to make sure healthy weight reduction.
Normal results
Within the years following surgery, patients often regain a few of the dropped pounds. But few patients regain everything. Obviously, diet and activity level after surgery also are likely involved in just how much weight someone will swiftly lose. Is a result of long-term follow-up data of gastric bypass surgery show that more than a five-year period, patients lost 58% of the excess fat. Over ten years, losing was 55%, and after , excess fat loss was 49%. Nevertheless there is a propensity to slowly regain a few of the dropped pounds, there's still a substantial permanent weight reduction on the long time.
Morbidity and mortality rates
Obesity alone doesn't cause death. However, for all those having BMI above 20 kg/m2, morbidity for several health problems increases since the BMI increases. M2 refers back to the percent of excess fat separated by height. Higher morbidity, in collaboration with overweight and obesity, continues to be reported for hypertension, dyslipidemia, diabetes type 2, heart disease, stroke, gallbladder disease, osteoarthritis, anti-snoring and respiratory problems, plus some kinds of cancer like endometrial, breast, prostate and colon. Obesity can also be related to complications of being pregnant, menstrual problems, hirsutism, stress incontinence and psychological disorders.
Aftercare
Generally, gastric bypass is really a patient-friendly operation. Patients encounter postoperative pain and like other common difficulties of major surgery, since the NG tube along with a dry mouth. Pain is handled with medicine. A sizable dressing covers the surgical incision about the abdomen from the patient and it is generally removed through the second day within the hospital. Short showers two days after surgery are often allowed. Patients will also be fitted with Venodyne boots on the legs to massage them. By compressing the legs, these boots assist the blood flow and stop blood clot formation. In the surgeon's discretion, some patients might have a gastrostomy tube introduced during surgery to empty secretions in the larger bypassed part of the stomach. After a couple of days, it will likely be clamped and can remain closed. When introduced, the g-tube generally remains for an additional 4 to 6 weeks. It's kept in a place to avoid unlikely event how the patient may require direct feeding to the stomach. Through the evening after surgical procedures or the following day in the latest, patients are often in a position to crunches or walk around. Progressively, exercise might be increased, with normal activity resuming 3 to 4 weeks after surgery. Patients will also be taught breathing exercises and therefore are asked to cough frequently to pay off their lungs of mucus. Postoperative pain medicine is prescribed to help ease soreness and initially given by an epidural. When patients are discharged in the hospital, they'll be given medications for pain. Patients aren't allowed almost anything to eat soon after surgery and could use swabs to maintain the mouth moist. Most sufferers will routinely have a three-day hospital stay if their surgery is simple.
Postoperative day 1
The NG tube is taken away each morning after surgery. The individual is allowed sips of water during the day. The individual is assisted to get away from bed and asked to walk. It is crucial just to walk as early after surgery as patient possibly can to assist prevents pneumonia, thrombus within the legs, and constipation.
Postoperative day 2
When the patient has tolerated intake of water on day 1, she or he can start taking clear liquids. Patients are motivated or helped just to walk within the hallways a minimum of 3 times each day and therefore are asked to make use of the breathing machine. The urinary catheter is taken away in the bladder. Patients given oral pain medicines, crushed, chewed, or perhaps in liquid form.
Postoperative day 3
Patients are advanced to some more substantial diet that always includes milk-based liquids. Once the weight loss program is tolerated, pain is well managed on oral pain medicine, and patients can walk independently, they're discharged in the hospital. A dietitian generally visits the individual just before discharge to examine any queries about diet. Although most sufferers spend 3 days within the hospital, they might remain longer should they have postoperative nausea, fevers, or weakness. Additional tests are carried out in a later stage to ensure there have been no surgical difficulties. For instance, a swallow study might be performed to make certain that there isn't any leak in which the pouch and intestines happen to be joined together. Sometimes chest x-rays will also be performed to make certain that there aren't any signs and symptoms of pneumonia. Blood tests are usually necessary. These along with other postoperative tests are carried out with an individual basis as based on the surgical team.
Alternatives
Non-surgical alternatives
Dietary treatments are the essential non-surgical alternative. It calls for instruction regarding how to adjust dieting to lessen the amount of calories eaten. Decreasing calories moderately is proven to be necessary to achieve gradual and steady weight reduction also to make a difference for upkeep of weight reduction. Tricks of dietary therapy consist of teaching patients concerning the calorie content of various foods, food composition, reading nutrition labels, kinds of foods to purchase, and the way to prepare foods. Some diets suitable for weight reduction include low-calorie, very low-calorie, and low-fat regimes. Another nonsurgical alternative is exercise. Moderate exercise, progressing to half an hour or even more of all or preferably all times of the week, is suitable for weight reduction. Exercise has additionally been reported to become a major factor of maintaining weight reduction. Belly fat and, in some instances, waist circumference could be modestly reduced through exercise. Trick of exercise range from the utilization of such aerobic types of exercise as aerobic dancing, brisk walking, jogging, cycling, and swimming and selecting enjoyable activities that may be scheduled right into a regular routine.
Behavior therapy aims to enhance diet and exercise patterns and habits to new behaviors that encourage weight reduction. Behavioral therapy techniques for weight reduction and maintenance contain recording dieting and exercise patterns inside a diary; identifying such high-risk circumstances as having high-calorie foods in the home and consciously avoiding them; rewarding such particular actions as exercising a bit longer or eating a smaller amount of a particular kind of food; modifying unrealistic goals and false beliefs about weight reduction and the body image to realistic and positive ones; creating a support network in family, friends, or colleagues; or joining a support group that may encourage weight reduction in a positive and motivating manner.
Drug treatments are another nonsurgical alternative recommended like a treatment option for obesity. Three weight reduction drugs been authorized by the U.S. FDA for treating obesity: Xenical, phentermine, and sibutramine.
Surgical alternatives
The Lap-Band gastric restrictive process represents an alternative choice to gastric bypass surgery. The Lap-Band offers another method of bariatric surgery for patients who believe a gastric bypass isn't ideal for them. It causes weight reduction by lowering the capability from the stomach, thus restricting the quantity of food that may be eaten previously. The band is fastened round the upper stomach to produce a new tiny stomach pouch. Consequently, patients encounter a sensation of fullness and consume less food. While there is no cutting, stapling, or stomach rerouting involved, the process is considered minimal invasive of weight reduction surgeries. The surgeon makes numerous tiny incisions and makes use of long slender devices to implant this band. By avoiding the big incision of open surgery, patients usually experience less pain and scarring. Additionally, a healthcare facility stay is shortened to less than twenty four hours, which include overnight hospitalization. Vertical banded gastroplasty (VBG), another popular surgical technique also called stomach stapling, is today considered inferior to RNY gastric bypass in inducing weight reduction. It's also related to several unwanted problems.






