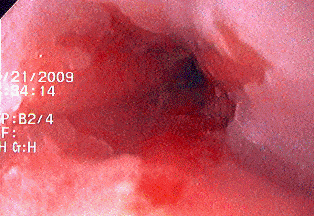
Definition
An esophagogastroduodenoscopy, also is referred to as a maximum endoscopy or upper gastrointestinal endoscopy, is really a diagnostic process that's carried out to see the esophagus, stomach, and duodenum. Within an EGD, a surgeon makes use of an endoscope, an adaptable, tube-like, telescopic device having a tiny camera mounted at its tip, to look at pictures from the upper digestive system displayed on the monitor within the evaluation room. Small devices can also be passed with the tube to deal with certain disorders in order to carry out biopsies.
Description
Upper endoscopy is recognized as to become more precise than x-ray studies for finding inflammation, ulcers, or tumors. It's accustomed to diagnose early-stage cancer and may usually help to see whether a rise is benign or malignant. A doctor can acquire biopsies of inflamed or suspected tissue for evaluation within the laboratory with a pathologist or cytologist. Cell scrapings may also be taken by introducing a little brush with the endoscope; this method is particularly useful when diagnosing cancer or contamination. Besides it works as an analyzing tool, an endoscope has channels that enable the passage of devices. This feature provides the doctor a chance to treat at that moment many conditions which may be observed in the esophagus, stomach, or duodenum. These treatments can sometimes include:
- stopping bleeding from ulcers or arteries
- removal of polyps along with other noncancerous tissue growths
- removing foreign objects which have been swallowed, for example coins, pins, buttons, small nails, and other alike items
- stretching narrowed areas within the esophagus
A few of the diseases and scenarios which are looked into identified, or treated using EGD includes:
- esophageal cancer
- gastroesophageal reflux disease, an ailment brought on by excess gastric acid
- abdominal pain
- achalasia, a problem within the muscular opening between your esophagus and also the stomach
- Crohn's disease and inflammatory disease from the small intestine
- swallowing problems
- hiatal hernia
- stomach ulcers
- Barrett's esophagus, a precancerous condition from the cells lining the esophagus
- irritable bowel syndrome
- rectal bleeding
- stomach cancer
An EGD treatment is generally carried out with a gastroenterologist, who is patient’s physician focusing on diagnosing and treating disorders from the digestive system. GI assistants, operating room nurses, or technicians might be active in the assortment of samples and proper care of the individual. Patient is going to be questioned either to gargle utilizing a local anesthetic or may have an anesthetic sprayed to their mouths onto the rear of the throat to numb the gag reflex. Then patient’s endoscopist will pass the endoscope with the mouth to the upper gastrointestinal tract as the patient is lying on his / her left side. The lens or camera at the conclusion from the device allows the endoscopist to look at each part of top of the gastrointestinal tract by observing pictures on the monitor. Photographs are often taken for reference. Throughout the procedure, air is pumped in with the device to grow the structure that's being studied and permit better viewing. Biopsy along with other method is going to be carried out when needed. The patient's breathing won't be disturbed there is going to be minimum distress. Many patients drift off during the main procedure.
Some patients shouldn't come with an EGD. This evaluation is contraindicated in patients who've:
- a suspected perforation from the esophagus or stomach
- esophageal diverticula, that are small pouches within the esophagus that may trap food or pills and be infected
- severe upper gastrointestinal bleeding
- recent surgery from the upper gastrointestinal tract the region like throat, esophagus, stomach, pyloric valve, duodenum
- a good reputation for such bleeding disorders as platelet dysfunction or hemophilia
An EGD can also be contraindicated for all those patients who're not able to cooperate fully using the process or whose total condition features are extreme underlying illness that boosts the risk of difficulties.
Purpose
An EGD is conducted to judge, and sometimes to deal with, such symptoms associated with top of the gastrointestinal tract as:
- bleeding in the upper digestive tract and related anemia’s
- difficulty swallowing
- pain within the chest or upper abdomen
- nausea or vomiting
- gastro esophageal reflux disease
Additionally, an EGD might be carried out to verify irregularities shown by such other diagnostic processes being an upper gastrointestinal x-ray series or perhaps a CT scan. It might be accustomed to treat certain conditions, for example a place of narrowing or bleeding within the upper gastrointestinal tract.
Risks
Endoscopy is recognized as a secure procedure when carried out with a gastroenterologist or other healthcare professional with special training and experience of endoscopy. The entire unwanted effect rate of EGD efficiency is under 2%; several difficulties are minor, for example inflammation from the vein by which drugs are given. Serious problems can and do occur, however, with almost half being associated with one's heart or lungs. Bleeding or perforations will also be reported, particularly when tumors or strictures happen to be treated or biopsied. Infections happen to be reported, though rarely; consideration to washing the device should prevent this problem. Perforation, that is the puncture of the organ, is extremely rare and may be surgically repaired whether it takes place during an EGD.
Diagnosis/Preparation
Certain medicines for example aspirin and also the anti-inflammatory drugs called NSAIDs ought to be stopped a minimum of 7 days before an EGD to lessen the chance of bleeding. Patient is going to be questioned to not eat or drink anything not less than six to 12 hours prior to the process to ensure top of the digestive tract is going to be empty. Prior to the process, patients might be given a sedative and/or pain medicine, generally by intravenous injection.
Normal results
The outcomes from the method or probable findings in many cases are open to the individual just before discharge in the endoscopy suite or even the recovery area. The outcomes of tissue biopsies or cell tests called cytology will require from 72-96 hours. Normal results will show how the esophagus, stomach and duodenum have the freedom of strictures, ulcers or erosions, diverticula, tumors, or bleeding. Abnormal results range from the presence associated with of those problems, in addition to esophageal infections, fissures, or tears. An ever more common finding is medication-induced esophageal injury, brought on by tablets and capsules which have lodged within the esophagus. These injuries can be related to harm to the esophageal tissue from gastrointestinal reflux disease also called GERD and also the related exposure from the esophagus to considerable amounts of gastric acid.
Aftercare
Following the process, the individual is going to be seen in the endoscopy suite or perhaps in another recovery area to have an hour, or before sedative or pain medicines has worn out. Someone ought to be open to go ahead and take patient home and turn into together for some time. Consuming meals ought to be avoided before local anesthetic has worn out within the throat and also the gag reflex has returned, which might take a couple of hours. To try when the gag reflex has returned, a spoon can be put about the back from the tongue for some seconds with light pressure to determine when the patient gags. Hoarseness along with moderate sore throat is normal following the process; the individual can drink cool fluids or gargle to alleviate the soreness. The individual may feel some bloating, belching, and flatulence after an EGD because air is introduced to the digestive system throughout the procedure. To avoid any problems for the esophagus from taking medicines orally, patients should drink a minimum of 4 or even more ounces of liquid with any pill, and remain sitting upright for half an hour after taking pills which are prone to cause injury. A doctor ought to be notified when the patient develops temperature; difficult or uncomfortable swallowing called dysphagia; breathing complications; or pain within the throat, chest, or abdomen.






