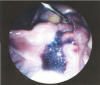
Tubal patency is often required to detect cause of infertility in female of reproductive age group.
It appears that the laparoscopic approach has several advantages:
- Cosmetically better outcome.
- Less tissue dissection and disruption of tissue planes
- Less pain postoperatively.
- Low intra-operatively and postoperative complications.
- Early return to work.
Laparoscopic tubal patency test in expert hands is now safe and effective. The public needs to be educated as to its advantages. All surgeons agree that for women of child bearing suffering with infertility, laparoscopic test for tubal patency is unquestionably the method of choice.
Patient selection:
Laparoscopic tubal patency test is a safe procedure, and can provide less postoperative morbidity in experienced hands. With better training in minimal access surgery now available, the time has arrived for it to take its place in the surgeon's repertoire.
The general anaesthesia and the pneumoperitoneum required as part of the laparoscopic procedure do increase the risk in certain groups of patients. Most surgeons would not recommend general anaesthesia in those with pre-existing disease conditions. The laparoscopy tubal patency test under local anesthesia should be performed in those cases. Patients with Cardiac diseases and COPD should not be considered a good candidate for laparoscopy. The laparoscopic tubal patency test may also be more difficult in patients who have had previous lower abdominal surgery.
Tasks:
- Preparation of the patient
- Creation of pneumoperitoneum
- Insertion of port
- Diagnostic laparoscopy.
- Cannulate the cervix with a Sprackman cannula
- Injection of methylene blue dye into the cervix
- Inspection of spillage of methylene blue dye through the fimbrial end of fallopian tube.
Preparation of patient
- Receive a general anaesthetic
- Foley urinary catheter
- Position the patient on the table
- Place the patient in supine position.
- Position the table as to tilt head 15 degree down.
- Paint thoroughly the operative area of skin
- Drape patient such as to expose 2/3 of lower abdomen.
Creation of Pneumoperitoneum:
- Check Veress needle before insertion.
- Check veress needle tip spring.
- Confirm that gas connection is functioning.
- Ensure flushing with saline does not block that needle.
- Make a small incision just above the umbilicus.
- Lift up abdominal wall and gently insert Veress needle till a feeling of giving way
- Confirm position of needle by saline drop method
- Connect CO2 tube to needle
- Switch off gas when desired pneumoperitoneum is created & Remove the Veress needle
Insertion of Port
- Extend incision on umbilicus. Insert 11mm trocar carefully
- Trocar and cannula (if using disposable check blade tip is functioning).
- Point trocar toward pelvic cavity
- Lift abdominal wall and insert trocar and cannula with sustained pressure till reduction in resistance shows thatyou are inside peritoneal cavity.
- Remove Trocar, leave the cannula.
- Insert telescope.
- Connect camera to telescope.
- Connect light source
- Do white balance.
- Connect CO2 tube to telescopic port.
First of all do diagnostic laparoscopy to exclude any other abnormality. If everything is all right then go for next step of tubal patency test.
- Cannulate the cervix with a Sprackrnan cannula, connected to a syringe containing 20 ml of saline with methylene blue dye.
- Ask the assistant to injects the methylene blue dye through the cervix. Some back spillage of dye may occur as the dye passes up the uterus, along the fallopian tube and escapes from the fimbrial end.
- The dye may sometimes cause tubal spasm, so small pressure spurts should be used.
- With gentle manipulation of pelvic structures the exterior aspects of the tube and its patency should be assessed. Mobility and fimbrial architecture should be identified.
Ending of the operation.
- Examine the abdomen for any possible bowel injury or haemorrhage.
- Remove the telescope.
- Remove telescope leaving gas valve of umbilical port open to let out all the gas.
- Close the wound with Suture. Use vicryl for rectus and un-absorbableintra-dermal or Stapler for skin.
- Apply adhesive sterile dressing over the wound.
If everything goes well the patient can be discharged on the same day. The snapshot pictures and video recording of all the procedure should be performed for future references.





