Dr. SAMSON CHANDRA, SpOG. D.MAS
OBSTETRICIAN, GYNECOLOGIST AND LAPAROSCOPIC SURGEON
PLUIT HOSPITAL, JAKARTA, INDONESIA
MEMBER OF WORLD ASSOCIATION OF LAPAROSCOPIC SURGEON
ABSTRACT
Pelvic inflammatory disease (PID) is the most common cause of acute pelvic pain and infertility due to transport factor. Acute complications of pelvic inflammatory disease include tubo-ovarian complex and abscess (TOA), pyosalpinx, and peritonitis. At late sequelae of this patient can be suffer of chronic pelvic pain, infertily, ectopic pregnancy or lifethreathening peritonitis if this disease could not be identify
PID and/or TOA can be diagnosed clinically or with several modalities like ultrasound, CT scan and MR imaging. However, the gold standard of diagnosis is still laparoscopy, particularly for the questionable diagnosis although many experts do not agreed with as a routinely tool because of the invasive method and expensive for among certain people.
The recently advance of antibiotic and method of drainage of the abscess with CT scan or ultrasound guidance are other available modalities which also arise controversy
Nevertheless some specific roles of laparoscopy are irreplaceable by other modalities particularly for women in reproductive age, menopausal women, doubtful diagnosis and other special cases
AIM OF STUDY
Laparoscopy is the best single diagnostic test, but it is invasive and not routinely used in clinical practice. The management of PID especially with TOA is still debated. In this article the laparoscopic management of tubo-ovarian abscesses (TOA) was evaluated. The study sought to provide the role of laparoscopy in diagnostic and treatment, what the efficacy compared to conservative treatment and laparotomy, at what condition laparoscopy should be preferred choice, how far the conservative therapy could be applied and what is the outcome if there is a late in manage of this disease.
METHODOLOGY
This reviews of article in role of laparoscopy in the management of tubo-ovarian abscess was searched using search engine Google, Hirewire press, Springerlink, Pub Med, Yahoo and other linked references. The following search keywords were used: laparoscopy, TOA, tubo-ovarian abscess and PID
INTRODUCTION
A pocket of pus that forms during an infection of a fallopian tube and ovary is called a tubo-ovarian abscess. Tubo-ovarian abscesses can develop in women who have pelvic inflammatory disease (PID) [1].
Tubo-ovarian abscess (TOA) most commonly occurs in women of reproductive age. Upper genital tract infections and acute or chronic pelvic inflammatory disease (PID) are the primary causes in most cases. Findings show that TOA develops in up to 34% of patients hospitalized for PID. Symptomatic and subclinical infections can lead rapidly to TOA. Untreated TOA may rupture and result in lifethreatening peritonitis. Because it is one cause of chronic pelvic pain, and because it has a negative impact on fertility, TOA is a major health concern [2].
A tubo-ovarian abscess is usually diagnosed by physical exam or pelvic ultrasound. Some abscesses are found by surgical exploration of the abdomen (laparoscopy or laparotomy) [1] These abscesses are usually treated with antibiotics. Very large abscesses or abscesses that do not go away after antibiotic treatment may have to be drained. Draining may be done by using a large needle that is guided by ultrasound or by cutting into the abscess during laparoscopy or laparotomy. Sometimes the infected tube and ovary also have to be removed surgically [1].
PELVIC INFLAMATION DISEASE (PID)
PID is defined as an infection of the female upper genital tract involving any combination of the endometrium, fallopian tubes, pelvic peritoneum and contiguous structures [3, 4]. Many causes may lead to lower abdominal pain in women, including gynecologic disease or dysfunction (complications of pregnancy, acute infections, endometriosis, adnexal disorders, menstrual disorders), as well as gastrointestinal (appendicitis, gastroenteritis, inflammatory bowel disease), genitourinary (cystitis, pyelonephritis, nephrolithiasis), musculoskeletal and neurologic causes.
- The most common infectious cause of lower abdominal pain in women is pelvic
- inflammatory disease (PID).
- PID is a polymicrobial infection with multiple microbial etiologies.
- Most cases of PID are associated with more than one organism.
- Pathogens can be categorized as sexually transmitted or endogenous organisms [3].
About 10% of women with PID will suffered infertile and 30% develop chronic pain. Up to 5% of women who subsequently conceive have an ectopic pregnancy. Spontaneous resolution of symptoms probably occurs in many women, but early initiation of treatment should be needed to prevent impairment of fertility [5]. Clinical improvement should occur within 3 days of initiating therapy. Consider further diagnostic test and/or laparoscopy if symptoms do not improve or worsen [6].
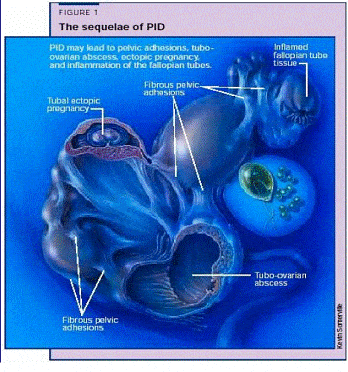
Fig. 1 . PID may causes sequlae that was caused of PID: adhesion, tuboovarian abscess, ectopic pregnancy, and inflammation of fallopian tubes [7].
��TUBO-OVARIAN ABSCESS (TOA)
A tubo-ovarian abscess is collection of pus in the adnexa which develops in about 15% of women with salpingitis. It can accompany with acute or chronic infection and is more likely if treatment is late or incomplete. Pain, fever, and peritoneal signs are usually present and may be severe. The abscess may rupture, causing progressively severe symptoms and lead to septic shock.
Pathophysiology of TOA
- Ascending bacterial infection originating in the uterus
- Extending to the fallopian tube and broad ligament
- Acute supprative salpingitis, salpingo-oophoritis, pyosalpinx
- Tuboovarian complex or tuboovarian abscess [7].
Ovarian abscess is an almost unheard entity during pregnancy. Maternal and fetal morbidity and mortality significantly increase if the tubo-ovarian abscess is not removed at an optimal time. In pregnancy, diagnosis and management are difficult than in non-pregnant state. Clinical data may not reveal the diagnosis until surgery is resorted to as an elective or emergency procedure [3].
Arora D, 2004, reported a case a women that pregnant a round 19 weeks have a laparotomy for removal the ovarian abscess. The patient discharge on 10th post operative day with ongoing pregnancy. And she delivered a healthy male baby. The author suggested that if there is a large sized ovarian cyst should be removed pre-conceptionally. If diagnosed in early pregnancy it should be removed during 2nd trimester to prevent complications of rupture, torsion or soft tissue obstruction during labor [8].
Tubo-ovarian abscess may require more prolonged IV antibiotics and hospitalization. Treatment with ultrasound- or CT-guided percutaneous or transvaginal drainage can be considered if response to antibiotics alone is incomplete. Laparoscopy or laparotomy is sometimes required for drainage. Suspicion of a ruptured tubo-ovarian abscess requires immediate laparotomy. In women of reproductive age, surgery should aim to preserve the pelvic organs (with the hope of preserving fertility).
DIAGNOSIS OF PID/ TOA WITH CONVENTIONAL MODALITIES: The exact incidence of PID is unclear because the disease cannot be diagnosed reliably from clinical symptoms and signs. Comparing with laparoscopy the positive predictive value of clinical diagnosis is 65-90% [4, 9] and from observational studies suggest that delaying treatment by 3 days can impair fertility [5, 10].
Ultrasonography is very useful aids in establishing the diagnosis of TOA, although the "gold standard" remains laparoscopy [10]. However, if the patient cannot tolerate a thorough palpation of the adnexa because of pain, pelvic ultrasonography may be needed. An ultrasonographic examination excludes the presence of a tubo-ovarian abscess (TOA). However, if a TOA is not present, ultrasonography will probably not be helpful [11].
Pelvic sonograms finding frequently appear normal in the early stages or in uncomplicated conditions. In severe or advanced conditions, sonographic findings include endometrial thickening with or without endometrial fluid and gas, ovarian enlargement with indistinct ovarian borders, uterine enlargement with indistinct uterine contours, and free intraperitoneal fluid. Ascending extrauterine disease may cause tuboovarian complexes (Fig. 2a), originating as a combination of dilated inflamed fallopian tubes and enlarged inflamed ovaries, or frank tuboovarian abscess (Fig. 2b). [12]
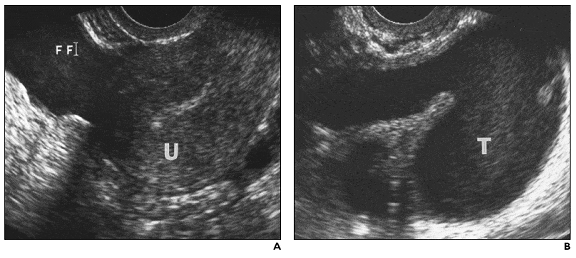
Fig. 2.— 24-year-old woman with pelvic inflammatory disease and tuboovarian complex. A, Sagittal endovaginal sonogram reveals complex free fluid (FF). U = uterus. B, Coronal image of left adnexa reveals dilated fallopian tube (T) with echogenic fluid. Findings are consistent with those of pyosalpinx [12].

Fig.3 CT scan imagine of tubo-ovarian abscess [13].
CT scan examination has been found to be superior than USG for the detection of abdominal abscess (78-100% sensitivity) as compared to ultrasound with a sensitivity of 75 - 82%[13].

Fig. 4. MR imaging of tubo-ovarian abscess with left hydrosalpinx in a 31 years old woman. Images show an about 5 x 4 cm sized thick walled cystic lesion (arrow) in the right adnexa. Also noted an elongated sausageshaped cystic lesion (arrows) in the left sided cul-de-sac. Both lesions have internal solid portions and pelvic LNs, mimicking malignancy. Note fluidfluid levels (arrows) in both adnexal lesions [7].
Timo A, et al, reported MR imaging diagnose PID with sensitivity 95% and specificity 89% and overall accuracy was 93% of the 21 patient which proved with laparoscopy. And for transvaginal US, the values were 81%, 78%, and 80% respectively [14].
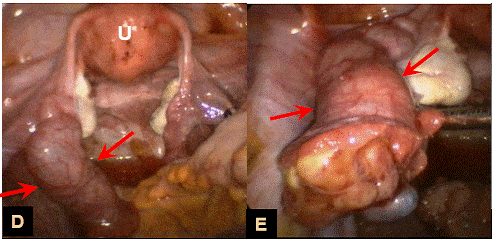
Fig. 5. Laparoscopy umage and close-up image of same patient shoe sausage-shape dilated right fallopian tube (arrow) [7].
Differential diagnosis:
Always consider specifically ectopic pregnancy and appendicitis in the differential diagnosis
- Ectopic pregnancy
- Acute appendicitis
- Complications of an ovarian cyst
- Endometriosis
- Urinary tract infection
- Constipation and surgical causes of acute abdomen
- Functional pain
- Irritable bowel syndrome
Investigations
- Urine pregnancy Test to exclude ectopic
- Full STD screen
- Consider laparoscopy to confirm diagnosis (this is the gold standard for diagnosis)
- Consider blood tests, ESR may be raised as may WCC and CRP
- Negative microbiological tests do not exclude a diagnosis of PID [15].
THE ROLE OF LAPAROSCOPY IN THE MANAGEMENT OF PID/TOA
In some cases, a laparoscopy may be necessary to confirm the diagnosis [16]. Laparoscopy was systematically used in Sweden to ensure the accuracy of the diagnosis of salpingitis in the 1960s – 1970s and during this period the poor accuracy of the clinical diagnosis became apparent (Jacobson and Weström 1969). Microbiologic sampling also enabled laparoscopically and it became the gold standard for the diagnosis. In the 1980s, videolaparoscopy introduced a completely new surgical vision, and laparoscopy could serve not only for diagnosis but also for therapeutic procedures. Both conservative and radical laparoscopic procedures were now possible also in the management of PID patients [17].
DIAGNOSIS WITH LAPAROSCOPY
When the diagnosis is remain unclear after other tests are done or when antibiotic treatment is not working; diagnostic is the definitive test [10,18]. Failure to identify pelvic inflammatory disease (PID) at an early stage may lead to tubo-ovarian abscess (TOA) and added morbidity. Observational studies suggest that delaying treatment by 3 days can impair fertility. Missing a TOA when present or mistakenly treating one on an outpatient basis can lead to a ruptured TOA and the requirement for major abdominal surgery. Diagnostic laparoscopy is usually used [5,10].
In reproductive ages, early diagnosis is essential to prevent future sequelae causing infertility [19]
Azzizet al, 2003, in his study investigated 92 patient cases over an eight-year period concluded that laparoscopy continues to be a useful tool in the workup of an infertile couple. Using together with a set of predictors for intrapelvic disease may help many couples avoid months of needless therapies [19].
Laparoscopy also allows the gynecologist to look for signs of ectopic pregnancy or infection and scar tissue, and make repairs if necessary [18].
TREATMENT WITH LAPAROSCOPY
Surgery is not usually done to treat pelvic inflammatory disease (PID). Ninety percent of patients with PID respond to medical therapy if no TOA is present. Most patients respond to IV antibiotics alone if a TOA is smaller than 7 cm.
Some indications for surgery are:
- Failure to respond within 48 to 72 hours of medical management
- Need to drain or remove an abscess, such as a tubo-ovarian abscess.
- Cut scar tissue (adhesions) that is causing pain [10,13].
Surgical therapy is necessary in a round 25% of patients treated for TOA. TOA diameter larger than 8 cm were less likely to respond to antimicrobial treatment than smaller abscesses [20]. Akyol et al, 1998, reported that they performed surgical therapy of their patients for TOA in 28,5% [20].
Arda et al, 2004, in their study about TOA in a sexually inactive adolescent patient concluded that laparoscopic surgery which minimises postoperative complications should be the first option in the treatment of TOA. Because early diagnosis and treatment are needed to prevent future sequelae causing infertility [21].
Protopapas AG et al, 2004, in their study reviewing the incidence of gynecological malignancy in menopausal women who develop tubo-ovarian abscesses. They concluded that postmenopausal women presenting with TOAs, should be thoroughly investigated. Conservative treatment of TOAs has no place during the menopause because of a significant concomitant gynecological malignancy was found including a variety of cancers [22].
Intra abdominal ruptured of tubo-ovarian abscess remains controversial and generally is decided on the basis of the patient’s age, parity and clinical circumstances[23] . Rupture of TOA is a surgical emergency with a very high mortality rate. Aggressive surveillance for the presence of a TOA and prompt inpatient medical management is required. Diagnosis of a ruptured TOA must be consider if the patient has increased peritoneal signs and a rigid abdomen [16].
Michael W et al, reported a rare case of fatal S pneumoniae infection from a tuboovarian abscess. At autopsy, a 6-cm tuboovarian abscess (TOA) was documented, with pathologic evidence of severe suppurative oophoritis of the right ovary [24].
Laparoscopy Prosedure:
- Laparoscopy was performed under general anesthesia by the conventional three-puncture technique.
- In all but one case with clinically suspected acute PID; the laparoscopic PID diagnosis was based on commonly accepted visual findings
- Acute salpingitis was diagnosed when a hyperemic edematous fallopian tube was visible, with no sign of intraluminal pus. A pyosalpinx was diagnosed as an enlarged, edematous tube with partial or total destruction of the fimbriated end.
- A TOA was diagnosed when the ovary and the Fallopian tube could not be distinguished from each other, forming an adnexal complex with abscess formation.
- Salpingitis was considered mild PID, whereas pyosalpinx and TOA were considered severe PID.
In patients with laparoscopically proven PID, one or more of the following procedures were performed:
- Lysis of pelvic adhesions, drainage and irrigation of pyosalpinges and TOAs, and extirpation of a unilateral infectious complex.
- Irrigation of the pelvic cavity with 2 liters of physiologic saline was performed in all cases.
- Patients with disease other than PID were treated laparoscopically when possible . But in certain cases, appendectomy was performed by laparotomy for severe infection
- All laparoscopies were documented by videotape.
- Unnecessary antimicrobial therapy was ended in patients with no sign of infectious disease in laparoscopy [17].
Although in the past, tubo-ovarian abscess occurred primarily in an older women age group; over the past several decades, a progressively younger patients group have been encountered. The young patient with a tubo-ovarian abscess who desires to maintain reproductive function presents a significant dilemma to the gynaecologist today [23]. However, in Buchweitz’s study, 2002, he concluded that if laparoscopic treatment of TOA is performed, organ-preserving treatment ( incision of the abscess cavity and lavage) should be preferred in order to reduce the risk of complications compare with laparoscopic salpingectomy or salpingo-oophorectomy (ablative treatment). This choice should be made irrespective of the patient's age or desire to remain fertile [25].
Yang et al, 2002, in their study with 69 women demonstrated that laparoscopy surgery had significant advantage over conventional laparotomy. It decreases hospital stay, had a lower percentage of wound infection, and had a shorter time for fever to subside. Advantages of open laparoscopic surgery over exploratory laparotomy in patients with tubo-ovarian abscess. They also concluded that although management of TOA consists of conservative medical treatment with antibiotics, it is now widely accepted that surgical intervention should be pursued early after the diagnosis [26].
DISCUSSION
Despite the development of new diagnostic aids, pelvic inflammatory disease (PID) is still poorly recognized and managed. Misdiagnosed of PID will consequence with potentially serious sequelae, particularly in fertile age women could become infertile.
Patients of fertile age represent an especially difficult patient group because of a variety differential diagnose of gynecologic and non-gynecologic.
Various imaging methods have been proposed for the diagnosis of PID. Transvaginal sonography (TVS) is routinely used in the diagnosis of acute gynecologic disorders. An overall concern is the poor performance of TVS in mild PID. CT scan has been found than be superior to USG for the detection of tubo-ovarian abscess (78-100% sensitivity) as compared to ultrasound with a sensitivity of 75 - 82%. In the diagnosis of intra-abdominal conditions, magnetic resonance imaging (MRI) has been widely accepted, although MRI has been used rarely in the imaging of adnexal masses and gynecologic infections. In a scenario of questionable diagnosis or if there is evidence of rupture of tuboovarian abscess immediate surgical intervention is recommended.
Drainage and appropriate use of broad-spectrum antibiotics are indispensable in treatment. In patients who failed to respond, laparoscopy or laparotomy was performed. For 21 Years, laparoscopy has been the gold standard for the diagnosis and treatment of TOA. The operative procedure involves blunt lysis and hydrodissection of adhesions, drainage of the abscess cavity, aspiration of purulent fluid from the pelvis, removal of necrosis, and irrigation of the peritoneal cavity. And compared to laparotomi, if there is no rupture of TOA or peritonitis, usually laparoscopy should be prefered Effective management laparoscopically will prevents complications associated with delayed treatment and often preserves the patient’s fertility. Some studies indicate that operative laparoscopy may improve the primary recovery of acute PID patients. Laparoscopic surgery which minimises postoperative complications should be the first option in the treatment of TOA.
CONCLUSION
Treatment of PID and TOA primarily should be with antibiotic,however if there is no respond in 3 days or clinical diagnosis remain unclear further measurement both for diagnostic and therapeutic have to be considered.
Laparoscopy offers the possibility to diagnose and manage PID more early, safely and probably cost-effectively. Effective management prevents complications associated with delayed treatment and often preserves the patient’s fertility or even catastrophic. Laparoscopy also improve the primary recovery of acute PID patients
Reference:
- Kathe Gallagher, MSW, Tubo-ovarian abscess and pelvic, inflammatory disease, Family Medicine, January 30, 2007
- O. Buchweitz, E. Malik, P. Kressin, A. Meyhoefer-Malik, K. Diedrich, Laparoscopic management of tubo-ovarian abscesses, Retrospective analysis of 60 cases, University of Luebeck, Ratzeburger Allee 160, 23538 Luebeck, GermanReceived, 2000
- Canadian Guidelines on Sexually Transmitted Infections 2006 Edition- Updated October 2007 )
- STD Treatment Guidelines. //www.cdc.gov/std/
- Jonathan Ross, Pelvic inflammatory disease, BMJ Clin Evid 2006;09:1606
- Pelvic Inflammatory Disease, www.ohiorepromed.com/ illustrations.htm
- Mi Young Kim, Sung Eun Rha, Soon Nam Oh, Young Joon Lee, Seung Eun Jung, Jae Young Byun, MR Imaging Findings of Hydrosallpiinx due to Various Causes: Comprehensive Review and Histopathologic Correlation Department of Radiology. The Catholic University of Korea, 2005
- Arora D, Pregnancy with ovarian abscess, Case report The Journal of Obstetrics and gynecology of India, J Obstet Gynecol India Vol. 55, No. 2 : March/April 2005 Pg 181-182
- CJ Tseng, Clinical Guideline Pelvic inflammatory disease, Chang Gung Memorial Hospital at ChiaYi, 2005
- Jason A. Dominitz, M.D. , MHS, John H. Sekijima, M.D., and Mary Watts, M.D, Abdominal Pain
- Ollendoff AT, Oophoritis, emedicine, 2007
- Y. Kaakaji, H. V. Nghiem, C. Nodell, T. C. Winter, AJR, Sonography of Obstetric and Gynecologic Emergencies: Part II, Gynecologic Emergencies, 2000;174:651–656 0361–803X/00/1743–651
- Gupta, Nupur Arora, Manju; Singh, Neeta; Dadhwal, Vatsla; Et al, A Clinical Experience of Ruptured Tuboovarian Abscesses, Red orbit, 2007
- Timo A. Tukeva, Hannu J. Aronen, Pertti T. Karjalainen, Pontus Molander, Timo Paavonen and Jorma Paavonen, MR Imaging in Pelvic Inflammatory Disease: Comparison with Laparoscopy and US, Radiology;210:209-216, 1999.
- Drs. Ros Sanders Hewett & Richard Lau, Pelvic Inflammatory Disease.Illustration, Department of Genitourinary Medicine, St. George's Hospital,28 September 2001, courtesy of: www.ohiorepromed.com/ illustrations.htm
- Westrom L and Eschenbach D. In: K. Holmes, P. Sparling, P. Mardh et al (eds), Pelvic Inflammatory Disease. ACOG Patient Education Pamphlet, 1999. Sexually Transmitted Diseases, 3rd Edition. New York: McGraw-Hill, 1999, 783-809.
- Pontus Molander, Diagnosis and management of patients with clinically suspected acute pelvic inflammatory disease, Helsinki, 2003
- Pelvic inflammatory disease Surgery ,WebMD Medical Reference from Healthwise November 28, 2006 ) Azziz, Can laparoscopy help you avoid unnecessary treatments?, 2003, sheknows.co






