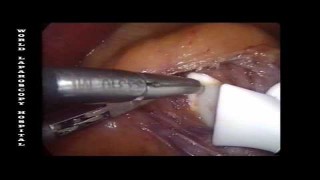
Exploring the Use of Indocyanine Green (ICG) in Colorectal Surgery - Steven D Wexner
Add to
Share
257 views
Report
4 months ago
Description
Colorectal surgery often poses significant challenges due to the complexity of the pelvic anatomy and the critical need to ensure adequate blood supply to anastomoses. Recent advancements have embraced the use of fluorescence imaging as a transformative approach to enhance surgical outcomes. Indocyanine Green (ICG), a near-infrared fluorescent dye, has emerged as a pivotal tool in this regard, particularly for assessing tissue perfusion and enhancing lymphatic mapping. This article delves into the applications, benefits, and considerations of using ICG in colorectal surgery. What is Indocyanine Green? Indocyanine Green (ICG) is a water-soluble, tricarbocyanine dye that, when injected, binds rapidly to plasma proteins and remains intravascular. It has the unique property of emitting near-infrared light when excited by specific wavelengths, allowing real-time visualization of vascular flow and lymphatic systems. The safety profile of ICG is well-established, with minimal adverse effects, primarily due to its rapid excretion by the liver into the bile. Applications in Colorectal Surgery Assessment of Anastomotic Perfusion: The primary application of ICG in colorectal surgery is to assess the perfusion of anastomoses. Inadequate perfusion is a major risk factor for anastomotic leakage, a serious complication. By injecting ICG intravenously and using a near-infrared camera system, surgeons can visually confirm the blood supply to the anastomosis during the procedure, potentially reducing the risk of leakage. Lymphatic Mapping and Sentinel Node Identification: ICG is valuable in oncologic surgery for tracing lymphatic drainage pathways and identifying sentinel lymph nodes. In colorectal cancer, this technique can help delineate the extent of necessary lymph node dissection, thereby optimizing surgical accuracy and potentially improving oncological outcomes. Identification of Ureters: The fluorescence properties of ICG can also assist in the identification of ureters during pelvic surgery. Accidental injury to ureters is a concern in lower colorectal procedures due to their close proximity to the surgical field. Benefits of Using ICG Enhanced Visual Assessment: ICG provides real-time, visual confirmation of tissue vascularization, which is crucial for successful surgical outcomes. Reduction in Postoperative Complications: By ensuring adequate perfusion, ICG use can lead to a lower incidence of anastomotic leakages and associated morbidity. Improved Oncological Precision: Accurate mapping of lymphatic drainage can influence the extent of nodal dissection, reducing the risk of residual disease. Considerations and Limitations Equipment Availability: The necessity for specialized equipment capable of detecting near-infrared fluorescence might limit the use of ICG in resource-constrained settings. Learning Curve: Effective use of ICG fluorescence imaging requires specific training and experience, which can initially extend surgical time. Cost Implications: Although the cost of ICG is relatively low, the overall expense including the imaging systems can be significant. Conclusion The integration of Indocyanine Green into colorectal surgical practice represents a significant advancement in enhancing intraoperative decision-making and improving patient outcomes. Its ability to provide real-time feedback on vascular and lymphatic integrity makes it an invaluable tool in both routine and complex cases. As technology progresses and becomes more accessible, the use of ICG in colorectal surgery is likely to expand, further solidifying its role in modern surgical practices. Contact us World Laparoscopy Hospital Cyber City, Gurugram NCR Delhi, India World Laparoscopy Training Institute Bld.No: 27, DHCC, Dubai, UAE World Laparoscopy Training Institute 5401 S Kirkman Rd Suite 340 Orlando, FL 32819, USA
Similar Videos