Advancing Surgical Expertise: Laparoscopic Repair of Common Bile Duct (CBD) Injury
Add to
Share
2,001 views
Report
2 years ago
Description
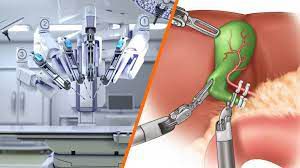
Introduction: Common bile duct (CBD) injuries are complex and challenging complications that can occur during certain surgical procedures, particularly those involving the hepatobiliary system. Traditionally, the management of CBD injuries required open surgical techniques with extensive incisions and prolonged recovery times. However, the advent of laparoscopic repair for CBD injuries has revolutionized the field of surgical expertise. This essay explores the significant advancements and benefits of laparoscopic repair in addressing CBD injuries, offering improved outcomes, reduced morbidity, and enhanced patient recovery. Body: Understanding Common Bile Duct (CBD) Injuries: CBD injuries can occur during various surgical procedures, such as cholecystectomy or liver resection. These injuries may lead to bile duct leakage, strictures, or obstruction, which can result in severe complications, including infection, biliary peritonitis, or liver dysfunction. Historically, open surgery was the primary approach for CBD injury repair, which involved larger incisions, increased trauma, and longer hospital stays. The emergence of laparoscopic repair techniques has transformed the management of CBD injuries. Advantages of Laparoscopic Repair: Laparoscopic repair offers several advantages over traditional open surgical techniques. Firstly, the minimally invasive nature of laparoscopy involves smaller incisions, resulting in reduced tissue trauma, decreased post-operative pain, and improved cosmetic outcomes. Additionally, laparoscopic repair provides surgeons with enhanced visualization through high-definition imaging and magnification, enabling precise identification and repair of CBD injuries. This precision reduces the risk of complications and allows for better preservation of healthy bile duct tissue. Enhanced Patient Outcomes: Laparoscopic repair of CBD injuries has shown promising results in terms of improved patient outcomes. The minimally invasive approach leads to reduced post-operative pain, decreased blood loss, and shorter hospital stays compared to open surgery. Patients undergoing laparoscopic repair experience quicker recovery times and can resume their daily activities sooner, leading to an enhanced overall quality of life. The reduced morbidity and faster recovery associated with laparoscopic repair contribute to improved patient satisfaction and a more efficient healthcare system. Technical Expertise and Training: Performing laparoscopic repair for CBD injuries requires a high level of surgical expertise and specialized training. Surgeons must possess advanced skills in laparoscopic techniques, including suturing, tissue manipulation, and precise dissection. Continuous training and experience in laparoscopic surgery are essential for mastering this intricate procedure. With advancements in technology and surgical education, more surgeons are acquiring the necessary skills to offer laparoscopic repair options to patients with CBD injuries. Future Directions and Innovation: As laparoscopic techniques continue to evolve, the field of CBD injury repair is witnessing further innovation. Novel tools, such as robotic-assisted surgery, are being explored to enhance surgical precision and overcome technical challenges. Continued research and advancements in imaging modalities and intraoperative navigation systems offer opportunities for real-time guidance and improved decision-making during laparoscopic repair. These advancements hold the potential to refine surgical outcomes and expand the applicability of laparoscopic CBD injury repair in complex cases. Laparoscopic repair of common bile duct (CBD) injuries represents a significant advancement in surgical techniques for managing complex hepatobiliary complications. This minimally invasive approach, compared to traditional open surgeries, offers numerous advantages such as smaller incisions, reduced trauma, improved visualization, and faster recovery times. By utilizing high-definition imaging and precise instrumentation, laparoscopic repair enables surgeons to address CBD injuries with enhanced precision, leading to improved patient outcomes and a shorter hospital stay. This description highlights the benefits of laparoscopic repair and its transformative impact on the management of CBD injuries, providing patients with a less invasive and more efficient surgical solution. Conclusion: Laparoscopic repair of CBD injuries represents a significant advancement in surgical expertise. This minimally invasive approach offers numerous benefits, including improved patient outcomes, reduced morbidity, and faster recovery times. The precise visualization and manipulation provided by laparoscopy enable surgeons to repair CBD injuries with greater accuracy and preserve healthy tissue. With ongoing advancements and evolving techniques, laparoscopic repair continues to expand its role in the management of CBD injuries, demonstrating the potential to revolutionize surgical practice and enhance patient care.
Similar Videos