Successfully addressing both sides of recurrent inguinal hernias through laparoscopic repair
Add to
Share
2,014 views
Report
2 years ago
Description
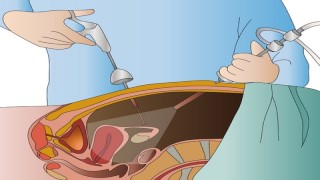
Introduction: Inguinal hernias are a common condition that affects millions of people worldwide. These hernias occur when a part of the intestine or abdominal tissue protrudes through a weak spot in the abdominal wall, resulting in a visible bulge in the groin area. While surgical repair is the primary treatment for inguinal hernias, the recurrence of hernias can pose a significant challenge. However, advancements in medical technology have introduced an effective and less invasive approach to tackle this problem: laparoscopic repair. Body: Understanding recurrent inguinal hernias: Recurrence of inguinal hernias can be attributed to various factors, including inadequate tissue healing, increased abdominal pressure, or the presence of additional weak spots in the abdominal wall. It is estimated that approximately 10% to 20% of patients experience recurrent inguinal hernias following traditional open repair surgery. Such recurrences not only cause physical discomfort but also raise concerns regarding the efficacy of the initial procedure. The emergence of laparoscopic repair: Laparoscopic repair has revolutionized the field of hernia surgery by offering a minimally invasive alternative to open repair. This technique involves the use of small incisions and the insertion of a laparoscope, which is a thin, flexible tube equipped with a camera and specialized surgical instruments. The camera provides a high-definition view of the internal structures, enabling surgeons to navigate and repair hernias with precision. Advantages of laparoscopic repair for recurrent inguinal hernias: a) Bilateral approach: One of the significant advantages of laparoscopic repair is its ability to address both sides of a recurrent inguinal hernia simultaneously. By gaining access to the abdominal cavity, surgeons can visualize and repair hernias on both the left and right sides. This bilateral approach reduces the risk of recurrence on either side and improves overall patient outcomes. b) Minimally invasive nature: Laparoscopic repair minimizes trauma to the abdominal wall compared to traditional open repair. The smaller incisions result in reduced post-operative pain, decreased blood loss, and faster recovery times. Patients undergoing laparoscopic repair experience fewer complications, allowing them to return to their normal activities sooner. c) Enhanced visualization and precision: The laparoscope provides surgeons with a magnified, three-dimensional view of the operative site. This enhanced visualization enables precise identification of the hernia defect and accurate placement of mesh or sutures for repair. Surgeons can also assess the surrounding tissues for additional weak spots and address them during the procedure, further reducing the risk of future hernias. Patient outcomes and satisfaction: Studies have consistently demonstrated favorable outcomes and high patient satisfaction rates with laparoscopic repair for recurrent inguinal hernias. The reduced risk of recurrence, minimal scarring, and faster recovery contribute to improved quality of life for patients. Furthermore, the laparoscopic approach offers a cosmetic advantage, with smaller incisions resulting in less noticeable scars. The laparoscopic repair of bilateral recurrent inguinal hernia is a cutting-edge surgical technique that addresses the challenge of hernia recurrence through a minimally invasive approach. Inguinal hernias, characterized by the protrusion of abdominal tissue or intestines through weakened areas in the abdominal wall, can cause discomfort and require surgical intervention. However, in some cases, hernias may recur even after traditional open repair surgery. The laparoscopic repair method utilizes advanced medical technology to effectively tackle bilateral recurrent inguinal hernias. By employing small incisions and inserting a laparoscope—a thin tube equipped with a camera and specialized surgical instruments—surgeons can visualize and repair hernias with precision. The camera provides a high-definition view of the internal structures, enabling surgeons to navigate the affected area and perform the necessary repairs. One of the notable advantages of laparoscopic repair is its ability to address both sides of the recurrent inguinal hernias simultaneously. Surgeons gain access to the abdominal cavity, allowing them to visualize and repair hernias on both the left and right sides. This bilateral approach significantly reduces the risk of recurrence on either side, improving the overall success rate of the procedure. Furthermore, laparoscopic repair offers several benefits compared to traditional open repair surgery. It is a minimally invasive procedure that minimizes trauma to the abdominal wall. The smaller incisions result in reduced post-operative pain, less blood loss, and faster recovery times. Patients who undergo laparoscopic repair experience fewer complications, allowing them to return to their normal activities more quickly. The laparoscopic approach also provides enhanced visualization and precision. Surgeons can accurately identify the hernia defect and place mesh or sutures for repair with utmost accuracy. Additionally, the laparoscope allows surgeons to assess the surrounding tissues for additional weak spots, which can be addressed during the procedure, further reducing the risk of future hernias. Patients who undergo laparoscopic repair for bilateral recurrent inguinal hernias generally report favorable outcomes and high satisfaction rates. The reduced risk of recurrence, minimal scarring, and faster recovery contribute to an improved quality of life for patients. Moreover, the cosmetic advantage of smaller incisions results in less noticeable scars. Overall, laparoscopic repair of bilateral recurrent inguinal hernias represents a significant advancement in hernia surgery. This technique offers a minimally invasive, precise, and effective approach to address hernia recurrences on both sides simultaneously. With its numerous benefits and positive patient outcomes, laparoscopic repair is transforming the field of hernia surgery and providing hope for individuals seeking long-lasting relief from recurrent inguinal hernias. Conclusion: Laparoscopic repair has emerged as a highly effective approach to address both sides of recurrent inguinal hernias. Its minimally invasive nature, combined with enhanced visualization and precision, offers numerous advantages over traditional open repair techniques. Surgeons can simultaneously repair bilateral hernias, resulting in reduced recurrence rates and improved patient outcomes. As this technique continues to evolve, it holds great promise in revolutionizing hernia surgery and enhancing the lives of individuals suffering from recurrent inguinal hernias.
Similar Videos